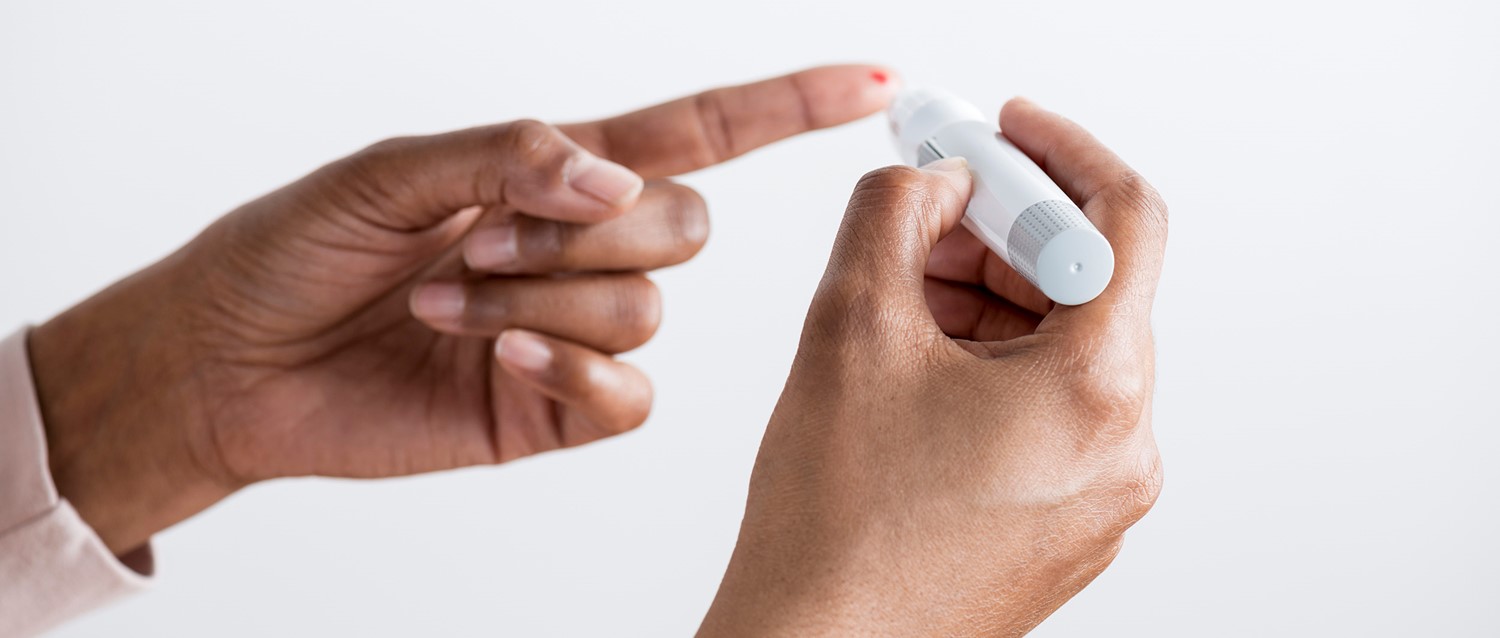
The future of diabetes treatment
Peer reviewed by Dr Joshua AldermanLast updated by Danny ChadburnLast updated 28 Sept 2017
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
How might the landscape of diabetes have changed by 2050? We asked leading diabetes physician Dr David Cavan, author of Reverse Your Diabetes and Reverse Your Diabetes Diet, for his predictions.
Sign up for our free 10-week Diabetes course!
Each week, we'll explore a different topic to help you better understand and manage your diabetes, including everyday living and medicines, to mental wellbeing, the latest in diabetes tech, and nutrition.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
In this article:
Continue reading below
Will rates of diabetes continue to rise?
Unfortunately, yes. In the UK, numbers rose from 1.4 million to almost 3.5 million between 1996 and 2016. Globally, diabetes is predicted to affect 642 million by 2040 – that’s one in 10 people.
Type 2 diabetes is driving the increase. It affects over 90% of those diagnosed and is directly linked to modern day diet and lifestyles; 50 years ago, it was relatively uncommon. We’ve seen a significant increase in cases over the past decade, so a significant change in the way we live our lives is needed to slow its growth.
Type 1 diabetes, which affects less than 10% of sufferers, is also on the rise but more slowly - and we’re not sure why. It’s an autoimmune condition, not linked to diet or lifestyle, but autoimmune conditions in general seem to be on the increase.
What does this mean for the NHS?
Back to contentsVast expense – the total cost associated with diabetes in the UK stands at £23.7 billion and is predicted to rise to £39.8 billion by 2035/6. It’s not just treatment costs but also wider economic implications, such as time off work. Treating the complications of diabetes, such as cardiovascular problems or damage to the nerves, kidneys, eyes or feet, is the biggest expense.
The solution? Prevention, reversal, and better management of symptoms, so people don’t get to the stage where they have complications. It needs a huge public health drive to raise awareness, change habits and prevent type 2 developing in the first place.
Continue reading below
Is there a cure on the horizon?
Back to contentsCurrently, type 2 diabetes is mainly treated with medication, such as metformin, to improve insulin sensitivity and normalise blood sugar. If these stop working effectively, insulin may be needed.
However, the exciting news is we now know that weight-loss surgery, also known as bariatric surgery, can lead to remission in type 2. The effects have also been replicated in studies using a very low-calorie diet for rapid and significant weight loss.
Although this works in the short term, there also needs to be a long-term lifestyle change, so I have been developing a low-carbohydrate eating plan to promote weight loss and reduce blood glucose levels. Following a low-fat, low-calorie diet - which is often high-carb - traditionally recommended by doctors doesn’t make sense if you can’t tolerate carbohydrates.
Dr David Unwin, a GP in Southport, has already saved his surgery tens of thousands of pounds in drug costs by advising those with type 2 diabetes to follow a low-carb diet, and has published papers on his findings. Of course, it’s not a cure if people revert to poor habits - it needs to be a complete and lasting change.
What about a cure for type 1 diabetes?
Back to contentsThere’s certainly potential for a cure by 2050. One theory is that type 1 is an autoimmune condition process triggered by an infection of some sort, along with a genetic predisposition. If scientists could identify the infection or trigger, they could potentially vaccinate against it.
The other major discovery could be stem cell technology – using the body’s own stem cells to prevent or treat certain conditions. If we could use stem cells to get the body to start producing insulin again, this would effectively be a cure.
Continue reading below
How might treatment for type 1 develop?
Back to contentsThe latest advance is continuous glucose monitoring, via a sensor implanted just under the skin, which gives minute-by-minute feedback on blood glucose levels rather than insulin users having to do regular pinprick tests. At the moment these are expensive and not widely available on the NHS, but I think their use will become more widespread.
The recent introduction of insulin pumps, rather than injections, has been a life-changing development for many with type 1 diabetes. These are worn continuously and deliver fast-acting insulin throughout the day and night, removing the need for injections and giving the user very fine control over how much they receive and when. The pump is made up of a small, battery-operated pack, attached to a thin, flexible tube (cannula) that inserts just beneath the skin, usually on the abdomen.
We’ll see insulin pumps further refined, to the point where artificial intelligence, or AI, is delivering treatment via sensors. If a sensor can interpret information and make intelligent decisions to instruct the pump, it’s acting as an artificial pancreas. This is already in research stages and looking highly possible.
The European Conference on Artificial Intelligence (ECAI) in 2016 even included a workshop on AI for diabetes. This makes sense because the core of type 1 diabetes management is pattern recognition - machine-learning algorithms could make light work of analysing all the variables, such as weight, food intake and activity levels, that are needed to tailor a patient’s insulin dose.
Other areas of research are looking at delaying the onset of treatment by targeting the immune system, and slowing the destruction of insulin-producing cells.
So is there hope on the horizon?
Back to contentsThe future is looking brighter for those with type 1, or a predisposition to diabetes, but when it comes to type 2 we all need to act. There’s no medical vaccination yet, but a healthy diet and lifestyle is a vaccine.
Patient picks for Diabetes mellitus
Diabetes
The link between diabetes and mental health conditions
The physical symptoms of diabetes need managing 24 hours a day, 7 days a week. According to Diabetes UK, 2 in 5 people feel mentally overwhelmed by the demands of living with the condition.
by Lawrence Higgins

Diabetes
What you should know about diabetes burnout
Managing diabetes is a full-time job. It involves a continuous cycle of blood sugar monitoring, medicine management, and proactive planning. Like many challenges in life, the constant need to monitor this health condition can lead to burnout if you don't take steps to recognise, address, and prevent it. This World Diabetes Day, we highlight the importance of self-care, support, and finding the right resources if you’re living with diabetes.
by Victoria Raw
Sign up for our free 10-week Diabetes course!
Each week, we'll explore a different topic to help you better understand and manage your diabetes, including everyday living and medicines, to mental wellbeing, the latest in diabetes tech, and nutrition.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
About the author

Danny Chadburn
Head of Content
Danny was the previous Head of Content at Patient.
About the reviewerView full bio

Dr Joshua Alderman
Clinical Consultant
MA (Cantab), BM, BCh (Oxon), DRCOG, FRCGP, MBE
After training in medicine at Cambridge and Oxford, Dr Sarah Jarvis MBE became a GP.
Article history
The information on this page is peer reviewed by qualified clinicians.
28 Sept 2017 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.