Epidermoid and pilar cysts
Sebaceous cysts
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 12 Jun 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Epidermoid and pilar cysts are commonly referred to as 'sebaceous cysts' (pronounced 'seb-ay-shuss'). They are overgrowths of skin cells (called keratin) held together in a little capsule, or sac.
They are harmless smooth lumps just under the surface of the skin. They are not cancerous and do not require removal unless they are bothering you by the look or the feel of them.
They can occur almost anywhere in the body, but are commonly found on the back or scalp.
In this article:
Video picks for Skin rashes
Continue reading below
What are cysts?
A cyst is a sac that is filled with a fluid or semi-fluid material. Cysts develop in various places in the body and arise from different tissues in the body. Two of the most common types of cyst that occur under the skin surface are epidermoid and pilar cysts.
These cysts are often called sebaceous cysts but this term is no longer correct, as the origin of these cysts is not from the sebaceous glands in the skin, as was once thought.
Many doctors still call them sebaceous cysts, though.
What is an epidermoid cyst?
An epidermoid cyst is a cyst where the cyst sac forms from epidermal cells that normally occur on the top layer of the skin (the epidermis).
There are lots of other names for epidermoid cysts, such as epidermal cysts, inclusion cysts, and keratin cysts.
What is a pilar cyst?
A pilar cyst is a cyst where the cyst sac forms from cells similar to those that are in the bottom of hair follicles (where hairs grow from).
A pilar cyst is also known as a trichilemmal cyst.
In both cases, the semi-fluid content of the cyst looks a bit like cottage cheese. This substance is soggy keratin. Keratin is made by skin cells and is the substance that hairs are made from and the substance that covers the top layer of the skin.
Who gets them?
Back to contentsEpidermoid cysts can affect anyone but are most common in young and middle-aged adults. They can appear anywhere on the skin but develop most commonly on the face, neck, chest, upper back and sometimes on the scrotum.
Pilar cysts can affect anyone but are most common in middle-aged women. They can appear anywhere on the skin but develop most commonly on the scalp. It is common for several to develop at the same time on the scalp.
Continue reading below
Epidermoid and pilar cysts symptoms
Back to contentsEpidermoid and pilar cysts are smooth round lumps which you can see and feel just beneath the skin surface. They are very common.
They range in size but often they are small, like a pea. Sometimes, they can grow slowly over many months to become a few centimetres in diameter. They look very similar to each other but can be distinguished from each other if the cells that form the cyst sac are looked at under the microscope.
Epidermoid and pilar cysts usually cause no symptoms. Occasionally:
Cysts can become infected, when they may become red, inflamed and painful. A course of antibiotics will usually clear an infection if it occurs. Sometimes they settle down even without antibiotics.
The cyst may leak the cheese-like material on to the skin if the cyst is punctured or damaged.
A little horn may grow on the skin over the cyst.
A cyst may form in an uncomfortable place such as in the genital skin or beside a nail.
This photo shows the typical appearance of an epidermoid cyst on someone's neck:
Epidermoid cyst on the neck
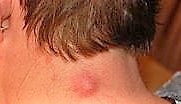
© Steven Fruitsmaak (Own work) - close-up view, CC BY-SA 3.0, via Wikimedia Commons
What causes epidermoid and pilar cysts?
Back to contentsIt seems that some cells that are normally near to the surface of the skin (cells of the epidermis or cells in hair follicles) get into deeper parts of the skin and continue to multiply. The cells that multiply form into a sac and produce the keratin that they would normally make on the top layer of the skin. The keratin becomes soggy and forms into a cheese-like substance and a cyst can occur.
Usually epidermoid cysts pop up for no particular reason: there is nothing you can do to prevent them. They are not related to cleanliness, nor will exfoliating stop them occurring.
Pilar cysts on the scalp can be hereditary and run in families, although this is rare.
Rarely, epidermoid cysts can occur due to genetic disorders. A genetic condition might be present if someone has a lot of epidermoid cysts in unusual locations (like on the fingers and toes).
Are epidermoid and pilar cysts painful?
Not usually. If they do not bother you then it is best just to leave them alone. If one has grown recently it's worth asking your doctor to check that it is a harmless cyst. Sometimes a person with an epidermoid or pilar cyst requests that it be removed. This is usually for one of three reasons:
Cosmetic reasons. For example, the cyst is in an obvious site on the skin and looks unsightly.
They are sometimes easy to catch and traumatise. This typically occurs on the scalp when combing hair.
If the cyst often becomes infected or irritating.
Epidermoid and pilar cysts are non-cancerous (benign). They do not spread to other parts of the body or cause any serious problems.
Continue reading below
Removal of epidermoid and pilar cysts
Back to contentsIf required, the cyst can usually be easily removed by a simple operation under local anaesthetic. The surrounding skin is numbed by injecting some local anaesthetic. A small cut is made over the cyst. It can then be gradually teased out by the doctor. The wound is then stitched up. A small scar will result. Sometimes, after the removal of a cyst, it gradually regrows in the same site under the scar.
Bear in mind you then exchange a small cyst for a scar: some people would rather have been left with the cyst, once they see the results of the surgery.
Patient picks for Skin rashes

Skin, nail and hair health
Pemphigus vulgaris
Pemphigus vulgaris is a very serious skin disease that causes blisters. It is rare. Pemphigus vulgaris is more serious than most other blistering skin conditions. Before treatment became available, most people with the condition used to die soon after the disease started. These days most cases can be controlled with treatment. Treatment is usually with steroid medicines and other medicines to suppress the immune system. A skin specialist should supervise treatment.
by Dr Oliver Starr, MRCGP

Skin, nail and hair health
Actinic keratosis
An actinic keratosis (also known as a solar keratosis) is the most common skin condition caused by sun damage. It is the result of skin being damaged by the sun over many years. Actinic keratoses are usually rough, scaly patches on sun-exposed areas such as the head and face. Actinic keratoses are common, especially in older people, many of whom have more than one. Usually they are harmless but there is a small risk that they may eventually turn into skin cancer and therefore treatment may be advised.
by Dr Doug McKechnie, MRCGP
Further reading and references
- Cysts; DermNet NZ
- Jawa DS, Sircar K, Somani R, et al; Gorlin-Goltz syndrome. J Oral Maxillofac Pathol. 2009 Jul;13(2):89-92. doi: 10.4103/0973-029X.57677.
- Ali SY, Prabhat S, Ramanamurty ChV, et al; Coexistence of porokeratosis of Mibelli with Gardner's syndrome: A rare case report. Indian Dermatol Online J. 2011 Jul;2(2):94-6. doi: 10.4103/2229-5178.86001.
- Verma S, Kushwaha JK, Sonkar AA, et al; Giant sublingual epidermoid cyst resembling plunging ranula. Natl J Maxillofac Surg. 2012 Jul;3(2):211-3. doi: 10.4103/0975-5950.111386.
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
12 Jun 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.