Epidural pain relief after surgery
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 20 Nov 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
The content of this leaflet is used with the permission of the Royal College of Anaesthetists, the professional body responsible for the speciality throughout the UK, ensuring the quality of patient care through the maintenance of standards in anaesthesia, critical care and pain medicine.
In this article:
Video picks for Anaesthesia
Continue reading below
What is an epidural?
An epidural is used for giving pain relief. It is often used in childbirth but it can also be used during surgery to supplement a general anaesthetic, and it is continued after the operation for pain control.
How does an epidural work?
Back to contentsDuring an epidural, an anaesthetist uses a needle to place a fine plastic tube (an epidural catheter) into somewhere called the epidural space. The epidural space is the area the spinal nerves pass through to the lower back close to the spine.
Local anaesthetic, and sometimes other pain relief drugs, are put through the epidural catheter. This lies close to the nerves in the back. As a result, the nerve messages are blocked. This gives the pain relief, which varies in extent according to the amount and type of drug given. The local anaesthetic may cause some numbness as well as pain relief.
An epidural pump is used to give pain relief drugs continuously through the epidural catheter. The pain relief lasts as long as the pump is running. When it is stopped, full feeling will return within a few hours.
Continue reading below
How is an epidural done?
Back to contentsEpidurals can be put in:
When you are fully awake.
With sedation (drugs that make feel you sleepy and relaxed).
During a general anaesthetic.
The anaesthetist will talk to you about which might be best for you.
The steps for having an epidural are:
A cannula (drip) is placed in a vein in your arm for giving fluid.
You will be asked to sit up or lie on your side. You will be helped to bend forwards, curving your back as much as you can.
A small injection of local anaesthetic is given to numb the skin.
A needle is used to place a thin plastic catheter (tube) into the epidural space in your back. The needle is removed, leaving only the catheter in your back.
Does an epidural hurt?
Back to contentsThe local anaesthetic injection in the skin will hurt briefly. There will then be the feeling of pushing, but usually no more than discomfort as the needle and catheter is inserted.
Occasionally, a sharp feeling, like an electric shock, is felt. If this happens, it will be obvious to your anaesthetist. They may ask you where you felt it.
A sensation of warmth and numbness gradually develops. For some types of epidural, your legs may feel heavy and become difficult to move.
Overall, most people do not find these sensations to be unpleasant, just a bit strange. Feeling and movement will return to normal when the epidural is stopped.
Continue reading below
What are the benefits of an epidural?
Back to contentsIf the epidural is working properly, the pain relief will be better than with other methods, particularly when you take a deep breath, cough or move about in the bed.
There should be less need for alternative strong pain relief medicine. This means your breathing will be better, there should be less nausea and vomiting, and you are likely to be more alert.
There is also some evidence that other complications of surgery may be reduced, including blood clots in the legs or lung and chest infection. There is some evidence that you may lose less blood with an epidural, which will reduce your chance of needing a blood transfusion.
Do you have to have an epidural?
Back to contentsIt is your choice. The anaesthetist will tell you if they particularly recommend an epidural, and what alternatives there may be.
Other pain relief methods use morphine or similar drugs. These are strong pain relief medicines. These drugs have side effects that include nausea and constipation. Some people become confused when taking morphine.
Morphine, or other similar drugs, can be given by mouth, by injection or using a pump that you control yourself (patient-controlled analgesia, commonly known as PCA).
Alternatively, there are other ways that local anaesthetic can be given - for example, a nerve block.
Every effort will be made to keep you as comfortable as possible.
Can anyone have an epidural?
Back to contentsNo. An epidural is not possible for some people. It might not be possible if:
Blood thinning drugs, such as warfarin are being taken.
There is a blood clotting problem.
There is an allergy to local anaesthetic.
There is a significant deformity of the spine.
There is an infection in your back.
There has been previous surgery on the spine with metalwork in the back.
There have been problems with a spinal or epidural in the past.
What are the side-effects of an epidural?
Back to contentsRisks explained
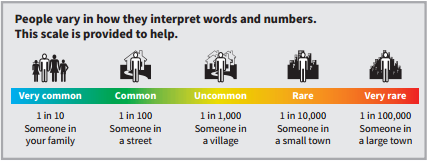
Very common side-effects
Back to contentsLow blood pressure
It is normal for the blood pressure to fall a little when you have an epidural. Your anaesthetist will use fluids and drugs to correct it.
Inability to pass urine
The nerves to the bladder are affected by the epidural. A catheter (tube) is inserted into the bladder to drain away the urine. This is often needed after major surgery with or without an epidural.
Itch
This is a side-effect of the pain relief drugs that may be used in your epidural. Anti-histamine drugs help, or the drug in the epidural can be changed.
Feeling sick
This is less common with an epidural than with other pain relief methods. It is treated with anti-sickness medicines.
Inadequate pain relief
The epidural may not relieve all your pain. Your anaesthetist or the pain relief nurses looking after you will decide if it can be improved or if you need to switch to another pain relief method.
Common side-effects
Back to contentsHeadache
Headaches happen quite often after surgery. It is possible to get a severe headache after having an epidural. This is because the needle used to place the epidural inadvertently punctured the bag of fluid that bathes the spinal cord. A small amount of fluid leaks out, causing a headache.
Epidural headache is a severe headache that is worse if you sit up and relieved by lying flat. The staff looking after you should alert the anaesthetic team immediately. You may need specific treatment for the headache. For more information, please see Headache after an Epidural or Spinal Anaesthetic.
Uncommon complications
Back to contentsSlow breathing
Some drugs used in the epidural can cause slow breathing or drowsiness, which requires treatment.
Nerve damage: temporary
Uncommonly, the needle or epidural catheter can damage nerves. This can give loss of feeling or movement in a large or small area of the lower body. In most people this gets better after a few days, weeks or months.
Rare or very rare complications
Back to contentsNerve damage: permanent
Permanent nerve damage by the needle or the catheter is rare. A study has shown it happens in between 1 in 6,000 and 1 in 12,000 epidurals used for surgery. Also rarely, this can happen for other reasons during surgery, related to the surgery itself or for other medical reasons unrelated to the epidural.
You can find more information about this from the leaflet Nerve Damage Associated with a Spinal or Epidural Injection.
Catheter infection
An infection can occasionally develop around the epidural catheter. If this happens, it will be removed. It is rare for the infection to spread deeper than the skin. Antibiotics may be necessary or, rarely, emergency back surgery. Disabling nerve damage due to an epidural abscess is very rare.
Other complications
Convulsions (fits), severe breathing difficulty, permanent paraplegia (loss of use of one or more limbs) or death are very rare.
The risk of complications should be balanced against the benefits and compared with alternative methods of pain relief. Your anaesthetist can give you more information and help you understand the relative risks.
Questions you may like to ask your anaesthetist
Back to contentsWhy are you recommending an epidural for me?
What are the advantages and disadvantages of an epidural for me?
What about the alternatives?
Who will do my epidural?
Have you often used this type of pain relief?
Do I have any special risks?
How will I feel afterwards?
How will I feel afterwards if I don’t have an epidural?
Content used with permission from the Royal College of Anaesthetists website: Epidural anaesthesia during and after surgery (6th Edition, June 2023) - see Further Reading below Copyright for this leaflet is with the Royal College of Anaesthetists.
Patient picks for Anaesthesia
Surgery and procedures
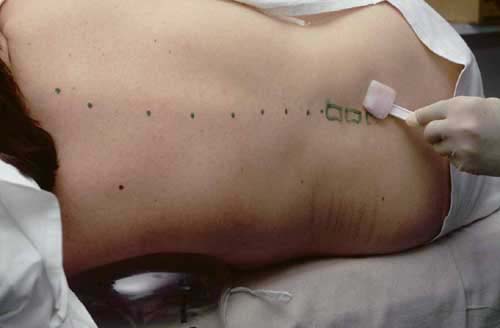
Spinal anaesthetic
A spinal anaesthetic is an alternative to a general anaesthetic for some operations. It allows the patient to stay awake during the operation without feeling any pain.
by Dr Doug McKechnie, MRCGP

Surgery and procedures
Anaesthetic for hip or knee replacement
This leaflet is adapted from the leaflet: Anaesthetic for Hip or Knee Replacement, provided by the Royal College of Anaesthetists, the professional body responsible for the speciality throughout the UK, ensuring the quality of patient care through the maintenance of standards in anaesthesia, critical care and pain medicine. Hip replacement and knee replacement are relatively common operations. They are often carried out for people with severe osteoarthritis, and so the number of people having these operations has increased as more people are living longer. See the leaflets on Hip Replacement and Knee Replacement for further information.
by Dr Colin Tidy, MRCGP
Further reading and references
- Ashouri M, Karvandian K, Ataie-Ashtiani Z, et al; Continuous epidural catheter for anaesthesia management and post-op pain relief in colorectal surgery, complicated by epidural haematoma and bilateral paraplegia: A case report. Int J Surg Case Rep. 2021 Jun;83:106039. doi: 10.1016/j.ijscr.2021.106039. Epub 2021 May 26.
Continue reading below
About the author

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 4 Oct 2028
20 Nov 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.