Pancoast's syndrome
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 21 Apr 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Synonyms: Tobias syndrome, Ciuffini-Pancoast-Tobias syndrome
Continue reading below
What is Pancoast's syndrome?1
Pancoast's syndrome is usually caused by a malignant neoplasm of the superior sulcus of the lung which produces destructive lesions of thoracic inlet along with involvement of brachial plexus and stellate ganglion. These cancers are rare, accounting for fewer than 5% of all lung cancers. The neoplasm is usually bronchogenic in origin (about half are squamous cell carcinomas, half adenocarcinomas).2
Pancoast's syndrome symptoms (presentation)2
Back to contentsThis syndrome results from the invasion of a number of structures and tissues around the thoracic inlet and may be characterised by:
Ipsilateral invasion of the cervical sympathetic plexus, leading to Horner's syndrome (miosis, enophthalmos, ptosis) in 14-50% of patients.3
Ipsilateral reflex sympathetic dystrophy in the arm, with enhanced sensitivity to touch, and skin changes.
Shoulder and arm pain (from the brachial plexus invasion C8-T1) with wasting of the intrinsic hand muscles and paraesthesiae in the medial side of the arm.
Less commonly, unilateral recurrent laryngeal nerve palsy producing unilateral vocal cord paralysis (hoarse voice ± bovine cough), and/or phrenic nerve involvement.
Arm oedema secondary to the compression of blood vessels.
Superior vena cava obstruction, with facial swelling, difficulty breathing and a flushed appearance.
The main presenting features of shoulder and arm pain, in the absence of respiratory symptoms, can result in a delay in diagnosis while the patient is inappropriately investigated for cervical arthritis, shoulder bursitis and rotator cuff injuries.4
X-ray image of Pancoast tumour
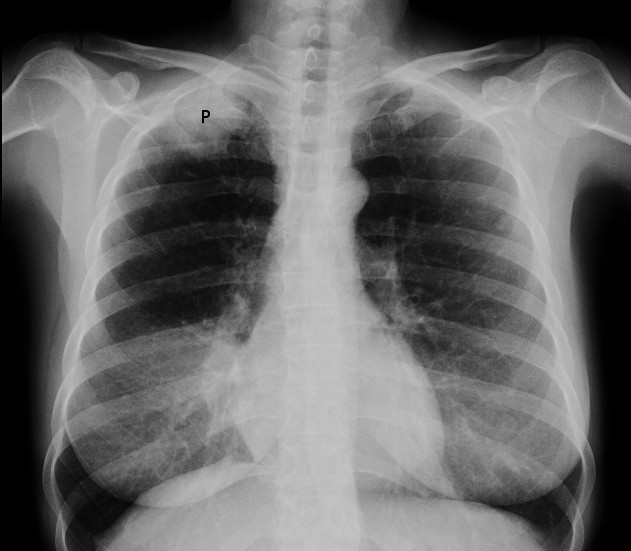
© Jmarchn (Own work), CC BY-SA 3.0, via Wikimedia Commons
Continue reading below
Other causes
Back to contentsMalignancies other than lung cancer can result in Pancoast's syndrome. Primary cancers have been reported, such as breast, mesothelioma, plasmacytoma or lymphoma;5 or metastatic carcinoma from the larynx, cervix, bladder, thyroid or colon.6
Non-neoplastic causes of Pancoast's syndrome are rare. However, there have been reported cases due to bacterial pneumonia (staphylococcal or pseudomonas), tuberculosis, hydatid disease,7 8 mycotic aneurysm, disseminated nocardiosis (a rare Gram-positive bacterial infection), plasma-cell granulomas, a cervical rib and pulmonary amyloidosis.
Staging
Back to contentsThis is as for other bronchogenic carcinomas, ie the tumour, node and metastasis (TNM) classification. Most Pancoast tumours are T3 at presentation, as there is invasion of pleura and the brachial plexus.3
Continue reading below
Investigations1
Back to contentsThis is similar to other lung cancers with an emphasis on imaging, including CXR and CT scan of the lungs and abdomen, and also possibly positron emission tomography (PET). MRI is the imaging of choice to assess structures at the thoracic inlet prior to surgery.3 9 Brain CT or MRI are usually performed, as it is the most common site of metastases. Good biopsy results are usually achieved by percutaneous methods.10
Pancoast's syndrome treatment and management1 11
Back to contentsThe National Institute for Health and Care Excellence (NICE) recommends that Pancoast tumours should be treated in the same way as other types of non-small cell lung cancer (NSCLC), with multimodality therapy according to resectability, stage of the tumour and performance status of the person.12
However, management may differ from other types of non-small cell lung cancer (NSCLC). Its position and close proximity to vital structures may make surgery difficult. Therefore, depending on the stage of the cancer, treatment may involve radiation and chemotherapy given prior to surgery.
Surgery may consist of the removal of the upper lobe of a lung together with its associated structures as well as mediastinal lymphadenectomy.
There are a number of surgical approaches, each with their advantages and disadvantages.13 The three most common procedures are the high postero-lateral approach, the anterior transcervical thoracic approach and the anterior trans-sternal approach.
Resection may involve a wedge resection or a lobectomy.3 10 14 Historically the involved brachial plexus has also been resected, leading to paralysis and neuropathic pain; however, this has largely been shown to be unnecessary.15
Prognosis
Back to contentsUntil the 1990s bimodal treatment (pre-operative radiotherapy followed by surgery) resulted in a five-year survival at best of only 30%, and a recurrence rate of 70%.13 However, the advent of trimodal therapy (induction chemoradiotherapy followed by resection) has decreased recurrence rates to 30%; five-year survival remains modest at between 40% and 70%.3 13
Further reading and references
- Villgran VD, Chakraborty RK, Cherian SV; Pancoast Syndrome. StatPearls, Jan 2023.
- Gundepalli SG, Tadi P; Lung Pancoast Tumor. StatPearls, Jan 2023.
- Palumbo VD, Fazzotta S, Fatica F, et al; Pancoast tumour: current therapeutic options. Clin Ter. 2019 Jul-Aug;170(4):e291-e294. doi: 10.7417/CT.2019.2150.
- Panagopoulos N, Leivaditis V, Koletsis E, et al; Pancoast tumors: characteristics and preoperative assessment. J Thorac Dis. 2014 Mar;6 Suppl 1:S108-15. doi: 10.3978/j.issn.2072-1439.2013.12.29.
- Foroulis CN, Zarogoulidis P, Darwiche K, et al; Superior sulcus (Pancoast) tumors: current evidence on diagnosis and radical treatment. J Thorac Dis. 2013 Sep;5(Suppl 4):S342-S358.
- Singh D, Wijeyekoon B; Case report of Pancoast tumour mimicking temporal arteritis; BMJ Case Reports 2012; doi:10.1136/bcr-2012-006285.
- Sarkar A, Das A, Basuthakur S, et al; Pancoast syndrome: A rare presentation of non-Hodgkin's lymphoma. Lung India. 2013 Jul;30(3):209-11. doi: 10.4103/0970-2113.116266.
- Lu CC, Lin HF, Lee HS, et al; Metastatic colon cancer presenting as Pancoast's disease. Am J Surg. 2009 May;197(5):e51-2. Epub 2009 Feb 13.
- Ozpolat B, Ozeren M, Soyal T, et al; Unusually located intrathoracic extrapulmonary mediastinal hydatid cyst manifesting as Pancoast syndrome. J Thorac Cardiovasc Surg. 2005 Mar;129(3):688-9.
- Dao I, El Mostarchid B, Onen J, et al; Pancaost syndrome related to hydatid cyst. Pan Afr Med J. 2013 Mar 27;14:118. doi: 10.11604/pamj.2013.14.118.1754. Print 2013.
- Manenti G, Raguso M, D'Onofrio S, et al; Pancoast tumor: the role of magnetic resonance imaging. Case Rep Radiol. 2013;2013:479120. doi: 10.1155/2013/479120. Epub 2013 Mar 31.
- Rusch VW; Management of Pancoast tumours. Lancet Oncol. 2006 Dec;7(12):997-1005.
- Nikolaos P, Vasilios L, Efstratios K, et al; Therapeutic modalities for Pancoast tumors. J Thorac Dis. 2014 Mar;6 Suppl 1(Suppl 1):S180-93. doi: 10.3978/j.issn.2072-1439.2013.12.31.
- Lung cancer: diagnosis and management; NICE guideline (2019 - updated March 2024)
- Marulli G, Battistella L, Mammana M, et al; Superior sulcus tumors (Pancoast tumors). Ann Transl Med. 2016 Jun;4(12):239. doi: 10.21037/atm.2016.06.16.
- Deslauriers J, Tronc F, Fortin D; Management of tumors involving the chest wall including pancoast tumors and tumors invading the spine. Thorac Surg Clin. 2013 Aug;23(3):313-25. doi: 10.1016/j.thorsurg.2013.05.001. Epub 2013 Jul 16.
- Davis GA, Knight SR; Pancoast tumors. Neurosurg Clin N Am. 2008 Oct;19(4):545-57, v-vi.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 19 Apr 2028
21 Apr 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free