Cushing's syndrome
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Rachel Hudson, MRCGPLast updated 20 Jun 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Cushing's syndrome is caused by too high a level of glucocorticoid in the body. This can be caused by taking steroid medication long-term (the common cause) or by the body making too much cortisol (the main glucocorticoid made by the body).
Symptoms usually develop gradually and so the diagnosis (other than that caused by steroid medication) may not be clear for some time.
In this article:
Video picks for Adrenal problems
There are various reasons why the body may produce too much cortisol, and complex tests may be needed to find the root cause of the excess cortisol. The most common cause of excess cortisol is a small, non-cancerous tumour in the pituitary gland which makes too much of a hormone called ACTH which stimulates the adrenal glands to make too much cortisol. This tumour can usually be removed by surgery.
Continue reading below
What is Cushing's syndrome?
Cushing's syndrome develops when the level of a glucocorticoid in your body is too high over a long period of time. Glucocorticoids are a class of steroid hormones. Too much glucocorticoid can occur from an exogenous or endogenous source.
Exogenous glucocorticoids
This means you take a glucocorticoid medicine regularly. These medicines are commonly called steroid (corticosteroid) medicines. Prednisolone is the most commonly prescribed steroid medicine.
Steroid medicines are sometimes used to treat various conditions such as some types of arthritis and some cancers. It is long-term treatment with a steroid medicine that can cause Cushing's syndrome.
Long-term steroid medication is the most common reason for Cushing's syndrome to develop.
Endogenous glucocorticoids
This means glucocorticoids made by your body. Cushing's syndrome can develop when your body makes too much of a hormone called cortisol (a main glucocorticoid). This condition was first described by a Dr Cushing who first wrote about it in the early 20th century.
How rare is Cushing's syndrome?
Back to contentsCushing's syndrome, caused by the body making too much cortisol, is rare. About 5 in 1 million people develop this type of Cushing's syndrome each year. Most cases are in people aged between 20 and 50. Women are five times more commonly affected than men.
The rest of this leaflet is about Cushing's syndrome due to the body making too much cortisol. See the separate leaflet called Oral Steroids for a discussion on the possible problems associated with taking steroid medication.
Continue reading below
Cushing's syndrome symptoms
Back to contentsThe symptoms that are said to be the most indicative of Cushing's syndrome are:
Easy bruising.
Facial redness (plethora).
Proximal muscle weakness.
Stretch marks (striae) - especially if reddish purple and more than 1 cm wide.
In children, weight gain but being short for their age
Symptoms of Cushing's syndrome occur because you have too much cortisol in your body over a long period of time. In most cases, several of the symptoms listed below develop, although you are unlikely to have them all:
Fat deposits build up on the side of the skull in the facial area, causing the appearance of a round, full, and puffy face. This used to be likened to a moon face.
Fat may accumulate at the upper back and behind the neck. This used to be inappropriately likened to a buffalo hump.
Facial puffiness and the face often looking redder than usual.
Facial hair in women.
Muscle weakness. In particular a proximal muscle weakness. The proximal muscles are the ones in your arms and legs nearest to the body. So, the muscles around the thighs, pelvis, shoulders and upper arms are the proximal muscles.
Thin skin which bruises easily.
Purple/pink stretch marks (striae) may appear - similar to those seen on some pregnant women.
Tiredness.
Aches and pains - particularly backache.
Mood swings - such as being more irritable, depressed or anxious than usual.
Lack of sex drive (loss of libido).
Periods may become irregular, or stop, in women.
'Thinning' of the bones (osteoporosis). You may fracture a bone more easily than usual.
'Water retention' (oedema) around the ankles.
Excess thirst.
Increased susceptibility to infections.
Affected children tend to be obese but grow slowly so are short for their age.
How does Cushing's syndrome progress?
Back to contentsIn most cases (apart from when steroid medication is the cause), the symptoms develop gradually. The diagnosis is often not clear for quite some time, sometimes years, after symptoms first begin.
This is because most of the symptoms can also be caused by other common problems. For example, although most people with Cushing's syndrome have obesity, most people with obesity do not have Cushing's syndrome. Likewise, high blood pressure is common but Cushing's syndrome is a rare cause of it.
Also, the symptoms can be fairly nonspecific at first. For example, you may put on some weight, have mood swings and just not feel right. However, it is difficult to say why. You may even be treated for depression or obesity before the cause of your symptoms becomes clear.
Cushing's syndrome in children
This is rare.
Weight gain.
Slowed/stopped vertical growth.
Raised blood pressure.
Cushing's syndrome in males
Reduced libido (sex drive).
Fertility problems.
Erection difficulty.
Cushing's syndrome in females
Thick dark hair growth on the face/body.
Periods become irregular or stop.
Continue reading below
What causes Cushing's syndrome?
Back to contentsThere are a number of causes of Cushing's syndrome. These include the following:
Pituitary adenoma - Cushing's disease
A pituitary adenoma is a small, non-cancerous (benign) tumour in the pituitary gland. It is usually less than 1 cm in size and is made of abnormal cells which make lots of ACTH. The ACTH stimulates the adrenal glands which then make too much cortisol. The abnormal cells in the adenoma are not 'turned down' by feedback from the high levels of cortisol.
If you exclude cases caused by medication (as mentioned earlier), about 4 in 5 cases of Cushing's syndrome are caused by a pituitary adenoma. Cushing's syndrome caused by a pituitary adenoma is called Cushing's disease.
Adrenal problems
There are various rare disorders of the adrenal glands which can cause high levels of cortisol. These include:
Adrenal hyperplasia - which means there is increased number and growth of the cells in the adrenal glands. These cells then make too much cortisol. There are various different types of adrenal hyperplasia.
Adrenal tumours:
A non-cancerous tumour of an adrenal gland.
A cancerous (malignant) tumour of an adrenal gland (very rare).
Other causes of too much ACTH ('ectopic ACTH')
Some rare tumours in other parts of the body sometimes make ACTH - for example, some types of lung cancer. The ectopic ACTH (ie ACTH not made in the pituitary gland) then stimulates the adrenal glands to make too much cortisol.
A variety of tumours can make ACTH, some cancerous and some non-cancerous. Some non-cancerous tumours are so small that it is very difficult to find where in the body the excess ACTH is being made.
Can steroids cause Cushing's syndrome?
Some people take steroid medicines which are similar to cortisol - for example, prednisolone. This is sometimes used to treat various conditions such as some types of arthritis and some cancers. The side-effects of long-term treatment with steroids can cause symptoms and problems similar to Cushing's syndrome.
Other causes
Some people who drink a lot of alcohol make too much cortisol. The cortisol level goes back to normal if drinking alcohol stops.
Some people with severe depression make too much cortisol.
How to diagnose Cushing's syndrome
Back to contentsTests to confirm the high level of cortisol
The level of cortisol normally varies throughout the day. So, a simple blood test is not good enough to diagnose Cushing's syndrome. One or more of the following tests may be advised:
A test to measure the amount of cortisol that you pass in your urine. You need to collect all the urine that you pass over 24 hours into a plastic container. This is sent to the laboratory to measure the cortisol.
In addition, or as an alternative, a blood test may be arranged after you take a medicine called dexamethasone. This medicine normally suppresses the amount of cortisol that you make. A blood cortisol level which is high after taking this medicine helps to confirm Cushing's syndrome.
A night-time blood test or saliva test to measure the level of cortisol. The level of cortisol should be low after you go to sleep and a high level is abnormal.
Tests to find the cause of the high cortisol
Once it is confirmed that you are making too much cortisol, you will need further tests to find out what is causing the high level. For example, is it due to a pituitary tumour (adenoma), an ectopic cause of ACTH, or to an adrenal cause?
Blood tests which measure cortisol and other hormones may help to locate the cause. This may involve taking blood from unusual sites of the body. You may also need a CT scan of the pituitary gland, adrenal glands or other parts of the body. The tests are often quite complex.
Petrosal sinus sampling
The petrosal sinuses are the veins at the base of the skull that drain the pituitary gland. Petrosal sinus sampling is an extremely sensitive, specific and accurate test for diagnosing Cushing's disease and distinguishing between a pituitary cause and ectopic ACTH.
A catheter is placed into a vein in each leg and threaded up into the jugular vein on either side of the neck. A tiny catheter is then threaded through each of these catheters into the petrosal sinus on both sides of the pituitary gland. Blood samples are taken from both catheters, as well as from the blood circulating through the body to measure the hormone levels.
How to treat Cushing's syndrome
Back to contentsThe treatment options depend on what is causing the high level of cortisol.
Surgical treatment for a pituitary adenoma
If you have a pituitary adenoma, the most common treatment is to have it removed by surgery. This is done using very fine instruments. The surgeon can get to the pituitary gland through a small cut behind the upper lip, just above the front teeth (or sometimes from inside a nostril).
The instruments are passed through the base of the skull - the sphenoid bone. So, this operation is called 'trans-sphenoidal surgery' and is done under general anaesthetic. The aim is to remove the adenoma but to leave the rest of the pituitary gland intact.
Removing the adenoma causes the level of cortisol in your body to go from high to almost zero. So, following surgery you need to take a medicine called hydrocortisone (similar to cortisol) for several months before your pituitary gland returns to normal.
It also takes several months for your body to readjust and for symptoms gradually to improve. The operation is successful in about 8 in 10 cases. Your surgeon will advise on the possible complications which sometimes occur - for example:
Sometimes the operation may damage some other parts of the pituitary gland. This may cause a reduced production of some other hormones. If this occurs, you can take replacement hormone therapy.
Sometimes it is not possible to remove all the cells which make the excess ACTH. If this occurs and the ACTH remains high following surgery, options include a second operation or other treatments listed below.
Other treatments for a pituitary adenoma
Where pituitary surgery is not possible, is declined, or has failed, other treatments may be considered:
Radiotherapy
Radiotherapy can destroy the pituitary adenoma. This has a good chance of success but may take months or years to take effect.
Medication
This may be needed until the radiation treatment takes effect. Also, the radiotherapy may damage the normal pituitary cells and may cause low levels of other hormones made by the pituitary gland. However, replacement hormone therapy can usually be taken if this occurs.
Surgery
A surgical procedure to remove both adrenal glands is an option. This stops your body making any cortisol (and other hormones) from your adrenal glands. You will need lifelong replacement therapy of certain hormones.
However, the adenoma will remain in the pituitary gland and continue to produce high levels of ACTH which can cause problems in some cases. Medication to block the production or effects of cortisol may work. There are several medicines which can be tried with various levels of success.
Treatments for other causes of Cushing's syndrome
The treatment options depend on the cause. For example:
If a tumour in an adrenal gland is the cause, an operation to remove it will cure the condition.
For adrenal hyperplasia (see above), both adrenal glands may need to be removed. You will then need to take lifelong replacement therapy of certain adrenal hormones.
Other tumours in the body which make ectopic ACTH may be able to be removed, depending on the type of tumour, where it is, etc.
Medication to block the production or effects of cortisol may be an option.
What is cortisol and what does it do?
Back to contentsCortisol is classed as a glucocorticoid hormone which is made by the adrenal glands. (A hormone is a chemical which is made in one part of the body but passes into the bloodstream and has effects on other parts of the body.) You have two small adrenal glands which lie just above each kidney.
Cortisol is vital for life. It has several functions including:
Helping to regulate blood pressure.
Helping to regulate the immune system.
Helping to balance the effect of insulin to keep the blood sugar level normal.
Helping the body to respond to stress.
How is the level of cortisol normally controlled?
Back to contentsPituitary and adrenal glands
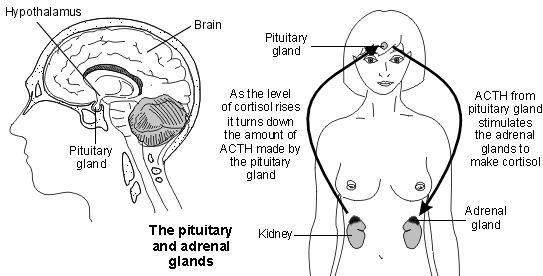
The level of cortisol needs to be just right. Too much or too little can cause problems. The amount of cortisol which is made in the adrenal glands is controlled by another hormone called adrenocorticotropic hormone (ACTH) - and sometimes just called corticotropin. ACTH is made in the pituitary gland.
The pituitary gland lies just below the brain. It makes several hormones, including ACTH. The amount of ACTH made by the pituitary gland is largely controlled by another hormone called corticotropin-releasing hormone (CRH).
CRH is made in a small part of the brain called the hypothalamus, which is just above the pituitary gland. CRH stimulates certain cells in the pituitary gland to make ACTH.
ACTH passes into the bloodstream, is carried to the adrenal glands and stimulates the adrenal gland to make cortisol. If the level of ACTH increases in the bloodstream, the adrenal glands make more cortisol.
However, cortisol has what is known as a negative feedback effect on the pituitary gland. That is, as the level of cortisol in the bloodstream rises above a certain level, it turns down the amount of ACTH made by the pituitary gland.
This means that the adrenal gland is then stimulated less and therefore less cortisol is made. So, the level of cortisol is kept within a certain range - just enough as is needed by the body.
Patient picks for Adrenal problems

Hormones
Addison's disease
Addison's disease is a condition in which your adrenal glands are not working as well as they should. In Addison's disease the adrenal glands do not produce as much of the steroid hormones (such as cortisol) as they normally do. These hormones are vital for your body and if you do not have enough of them, you can become very unwell. If the level of these hormones becomes very low, it can be life-threatening. Treatment is with replacement hormone tablets which you need to take every day.
by Dr Doug McKechnie, MRCGP

Hormones
Adrenal fatigue
Adrenal fatigue is a theory that the adrenal glands can become 'overworked' from chronic stress, leading to symptoms such as fatigue and low energy. However, there is no scientific evidence to support this claim. Adrenal fatigue is not recognised as a medical condition by professional medical societies, and the consensus amongst mainstream doctors is that it does not exist as a disease.
by Dr Doug McKechnie, MRCGP
Further reading and references
- The Pituitary Foundation
- Biller BM, Grossman AB, Stewart PM, et al; Treatment of ACTH-dependent Cushing's syndrome: a consensus statement. J Clin Endocrinol Metab. 2008 Apr 15;.
- Boscaro M, Arnaldi G; Approach to the patient with possible Cushing's syndrome. J Clin Endocrinol Metab. 2009 Sep;94(9):3121-31.
- Tritos NA, Biller BM; Advances in medical therapies for Cushing's syndrome. Discov Med. 2012 Feb;13(69):171-9.
- Gadelha MR, Vieira Neto L; Efficacy of medical treatment in Cushing's disease: a systematic review. Clin Endocrinol (Oxf). 2014 Jan;80(1):1-12. doi: 10.1111/cen.12345. Epub 2013 Nov 12.
- Fleseriu M; Recent advances in the medical treatment of Cushing's disease. F1000Prime Rep. 2014 Mar 3;6:18. doi: 10.12703/P6-18. eCollection 2014.
- Guignat L, Bertherat J; The diagnosis of Cushing's syndrome: an Endocrine Society Clinical Practice Guideline: commentary from a European perspective. Eur J Endocrinol. 2010 Jul;163(1):9-13. doi: 10.1530/EJE-09-0627. Epub 2010 Apr 7.
- Nieman LK; Cushing's syndrome: update on signs, symptoms and biochemical screening. Eur J Endocrinol. 2015 Oct;173(4):M33-8. doi: 10.1530/EJE-15-0464. Epub 2015 Jul 8.
- Zografos GN, Perysinakis I, Vassilatou E; Subclinical Cushing's syndrome: current concepts and trends. Hormones (Athens). 2014 Jul-Sep;13(3):323-37.
- Chaudhry HS, Singh G; Cushing Syndrome
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
20 Jun 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.