Lactose intolerance
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Doug McKechnie, MRCGPLast updated 23 Aug 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Food allergy and intoleranceNut allergyCow's milk protein allergyOral allergy syndrome
Lactose intolerance is a condition in which the body has difficulty digesting lactose. Lactose is a sugar found in milk and other dairy foods. People with lactose intolerance may get diarrhoea, stomach pains and bloating if they drink milk or eat dairy foods. Some people are born with a tendency to develop lactose intolerance; others get it as a result of gastroenteritis or chemotherapy. The treatment is mainly to avoid lactose.
In this article:
Video picks for Food allergy and intolerance
Continue reading below
What is lactose intolerance?
Diagram naming the parts of the gut
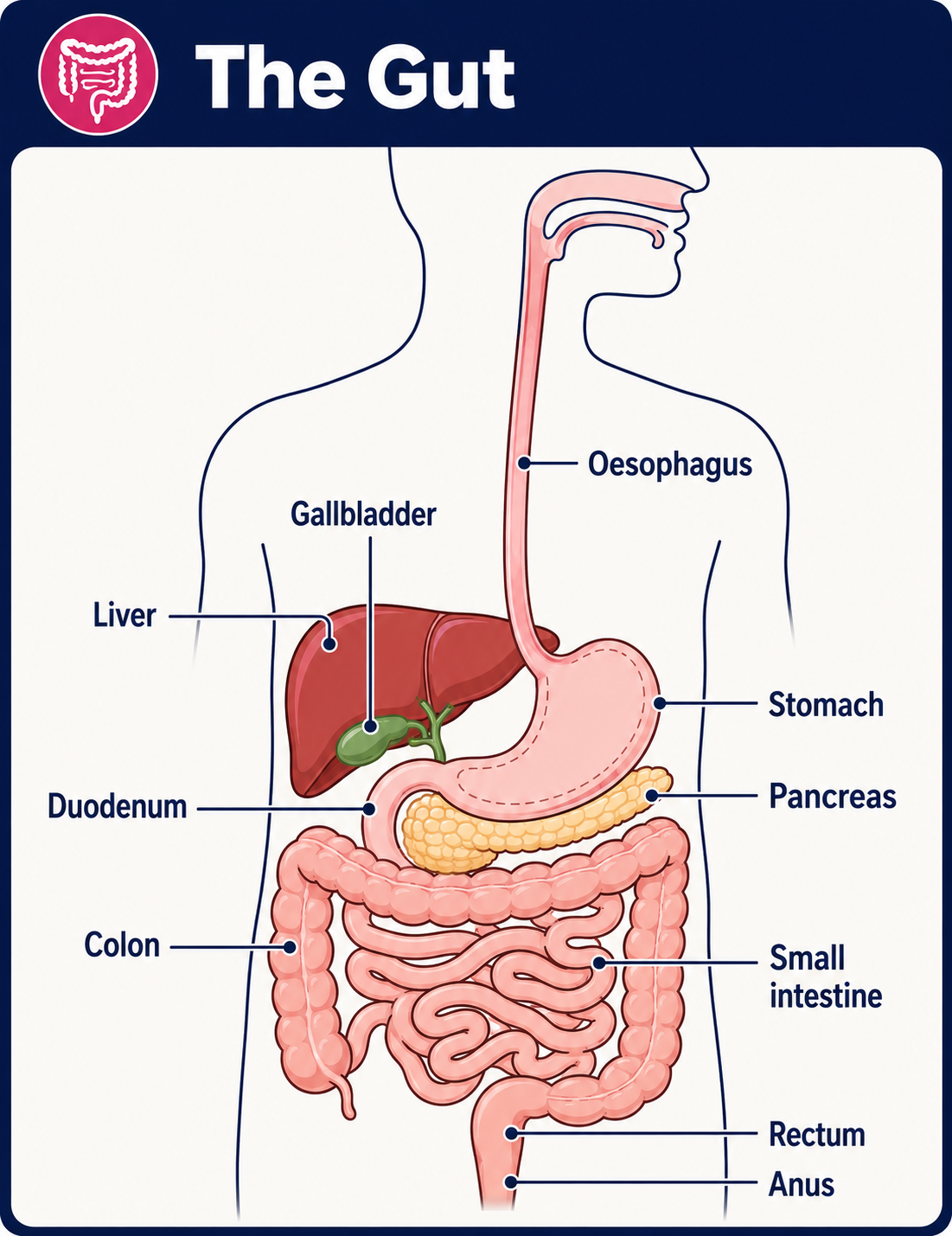
Lactose is a type of sugar found in milk. It cannot become absorbed by the body unless is gets changed into more simple sugars called glucose and galactose. This change happens when lactose passes through the stomach into the upper part of the gut (small intestine) and comes into contact with a protein (enzyme) called lactase.
Lactase is made by cells that line the upper part of the small intestine.
If there is not enough lactase in the small intestine, lactose cannot be broken down and cannot get absorbed. This leads to lactose intolerance.
Humans and other mammals are born with high levels of lactase, to allow them to digest breastmilk as babies and infants. Lactase levels reduce after birth.
In most non-human mammals, as they get older, lactase levels drop so low that they are no longer able to digest lactose by the time they reach adulthood. This also happens in human beings from many parts of the world; for example, people of African, Southeast Asian and South American descent often lose the ability to digest lactose as they grow older. This is the most common cause of lactose intolerance (see below).
Humans with ancestry from other areas (particularly northern Europe and northwest India), by contrast, often have higher levels of lactase in adulthood, and so are able to continue eating and drinking dairy products.
Some people confuse lactose intolerance with allergy to cow's milk. With milk allergy, the immune system reacts to proteins found in milk products, causing inflammation, which can cause symptoms.
Lactose intolerance is not an allergy. Symptoms are caused by the undigested lactose in the gut.
Lactose intolerance symptoms
Back to contentsLactose intolerance may lead to:
Bloating.
Stomach pains.
Excessive burping or passing a lot of wind.
Watery diarrhoea or itching around the bottom (anus).
These symptoms tend to develop from one to several hours after consuming milk, dairy products or any food containing lactose.
How bad the symptoms are depends on how much lactose your body can absorb, and this varies a lot between different people. A lot of people with lactose intolerance can eat some lactose without developing symptoms.
In general, the more lactose you eat, the more likely that symptoms will develop. The inherited condition (primary lactase deficiency) tends to cause less severe symptoms than the intolerance which develops after gastroenteritis or chemotherapy.
Babies and toddlers may have signs of malnutrition and poor growth (failure to thrive) but this is unusual unless they have the rare congenital form.
Continue reading below
What causes lactose intolerance?
Back to contentsThere can be a number of causes of lactose intolerance.
Is lactose intolerance genetic?
There are inherited forms of lactose intolerance. These are passed on through families:
Primary lactase deficiency: this causes decreasing levels of lactase with age after a child stops breast or bottle feeding. Symptoms can develop at any age but rarely before the age of 6 years. This is closely linked to ancestry; primary lactase deficiency is less common in people with northern European or northwestern Indian heritage, and, when it does develop, tends to develop later in life than in people of different heritage.
It's thought that, tens of thousands of years ago, all humans had primary lactase deficiency. At some point, groups of people started to develop and pass on genetic mutations that stopped lactase levels from dropping in adulthood. Other groups of people didn't, and remained unable to digest lactose in adulthood.
One possible explanation is that this was due to evolution: some people lived in societies and cultures that moved to diets containing lots of dairy products. People in those societies who were able to tolerate dairy products got more nutrition, and were more likely to survive and pass on their genes to their children. In cultures where dairy was not a major part of the diet, there was no evolutionary benefit from being able to digest lactose in adulthood, and so no reason for the lactose persistence gene to spread.
Congenital lactase deficiency: this causes a complete lack of lactase from birth. Symptoms develop as soon as the baby is given milk or lactose formula. This is extremely rare. Babies will require a special lactose-free milk if they have this condition.
Secondary lactase deficiency
This happens when something damages the cells in the lining of the upper gut (small intestine) where lactase production takes place. It is common in children and often occurs after a stomach infection (such as viral or bacterial gastroenteritis).
It can also be a complication of other bowel diseases, prolonged antibiotics, or chemotherapy. This is a temporary condition which improves when the lining of the gut heals.
Developmental lactase deficiency
When a baby is born, it takes time for a reasonable amount of lactase to build up in the digestive system. Babies more than six weeks premature may be born with very low levels of lactase, leading to temporary lactose intolerance. The condition disappears as the baby gets older.
How many people are lactose intolerant?
Back to contentsThis varies according to heritage and how much dairy produce is eaten within the country. In communities where a lot of dairy food is eaten, lactose intolerance is less common. Between 4 and 17 in 100 people in Northern Europe have the inherited form, whereas this figure can be up to 80 to 90 in 100 people in Hispanic, Asian or African communities.
Lactose intolerance is very common in adults worldwide - about 65% of all people have it. Many people may have a lack of lactase but not have much in the way of symptoms.
Continue reading below
How to test for lactose intolerance
Back to contentsIf you get symptoms after eating or drinking dairy or other lactose-containing products, it is fairly clear that you have lactose intolerance. Tests are not usually needed, but might be offered to look for other causes of the symptoms, such as coeliac disease.
If it's not clear whether lactose intolerance is causing the symptoms, other tests may be performed. Some of these are not routinely available on the NHS.
A hydrogen breath test. This measures hydrogen levels in breath after drinking a lactose-containing fluid. High levels of hydrogen suggest that someone is lactase deficient.
A stool acidity test. Unabsorbed lactose is converted into lactic acid by bacteria in the colon, which makes stools (poo) more acidic.
A milk tolerance test. Milk is drunk and a blood glucose (blood sugar) measurement is taken; the milk should cause blood glucose levels to rise, and, if it doesn't, it suggests lactose intolerance. A similar test can be done with lactose instead of milk.
A genetic test. These have been used in some countries, but are not widely available and not funded on the NHS.
A biopsy (sample) of the lining of the small bowel. This is rarely done, and often only to look for another condition, such as coeliac disease or inflammatory bowel disease.
Are there any complications from lactose intolerance?
Back to contentsMost people do not have any long-term problems. Babies with severe deficiency of lactase may develop lack of fluid in the body (dehydration) and malnutrition if the condition is not diagnosed early enough.
Avoiding all dairy products can mean you don't get enough calcium. Calcium is a mineral needed for bones to grow normally and be strong. Lack of it could mean children don't grow as well as they should, or adults could have weak bones that break easily.
What is the treatment for lactose intolerance?
Back to contentsPrimary lactose intolerance
People with primary lactose intolerance (the common inherited form) should find out how much lactose they can handle, by gradually building up the amount they eat. People do have varying levels of intolerance. Sometimes the amount they can tolerate can be increased by giving milk or dairy products little and often.
Having milk with meals may help. Full-fat or chocolate milk may be better than skimmed milk. Thicker foods such as yoghurts and curds are likely to be better tolerated because they move through the bowel at a slower rate. Live yoghurts and hard cheese (such as Cheddar, Edam, Emmental or Parmesan) may not cause problems.
Lactose-free milks are available but may be less nutritious than cow's milk. Check they are calcium-enriched. It is possible to buy lactase supplements at health food shops, to be taken with dairy products. However, these may be expensive and cannot be prescribed.
Secondary lactose intolerance
Secondary lactose intolerance, due to damage to the lining of the gut (small intestine), is usually treated by stopping dairy products for a short time, depending on the age of the child.
In babies and children with gastroenteritis, if the diarrhoea persists beyond two weeks and the baby is breastfed, most doctors advise parents to carry on with breast milk. If the baby is formula fed, or in very young babies, some doctors recommend withdrawing lactose, switching to a lactose-free formula milk, then going back to lactose again after around eight weeks. If the diarrhoea is very severe, occasionally treatment by fluid through a drip may be needed.
The chance of premature babies getting lactose intolerance due to developmental lactase deficiency can be reduced by feeding them half-strength lactose formula or breast milk.
What can I do to help with symptoms?
If you have lactose intolerance you should read the labels of food and drink very carefully. Not all foods with milk in them will cause problems. For example, lactose is broken down by fermentation and is not found in hard cheese such as Cheddar or Emmental. Foods that may cause problems include milk, cream, cottage cheese, yoghurts, ice cream and milk chocolate. Lactose is not present in dark chocolate.
Foods containing 'hidden' lactose may include some types of the following:
Bread.
Cakes.
Cereals.
Margarine.
Dressings.
Sweets.
Snacks.
Ready meals.
Also remember that many medicines contain lactose, so you should check the leaflet that comes with any medication you are taking.
Patient picks for Food allergy and intolerance

Allergies, blood and immune system
Food allergy and intolerance
Food allergy and food intolerance are not the same thing. The following leaflet explores the difference between them, their causes, and how they are diagnosed and managed.
by Dr Hayley Willacy, FRCGP

Allergies, blood and immune system
Cow's milk protein allergy
Cow's milk protein allergy is one of the most common food allergies seen in children. It is most commonly seen during the first year of life. Many children who have been allergic to cow's milk protein become tolerant to it by the time they are 5 years old.
by Dr Hayley Willacy, FRCGP
Further reading and references
- Shaukat A, Levitt MD, Taylor BC, et al; Systematic Review: Effective Management Strategies for Lactose Intolerance. Ann Intern Med. 2010 Apr 19.
- Heyman MB; Lactose intolerance in infants, children, and adolescents. Pediatrics. 2006 Sep;118(3):1279-86.
- Mattar R, de Campos Mazo DF, Carrilho FJ; Lactose intolerance: diagnosis, genetic, and clinical factors. Clin Exp Gastroenterol. 2012;5:113-21. doi: 10.2147/CEG.S32368. Epub 2012 Jul 5.
- Di Rienzo T, D'Angelo G, D'Aversa F, et al; Lactose intolerance: from diagnosis to correct management. Eur Rev Med Pharmacol Sci. 2013;17 Suppl 2:18-25.
- Lactose Intolerance; Nottinghamshire Area Prescribing Committee
- Lactose Intolerance; Allergy UK
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 21 Aug 2028
23 Aug 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.