Neck pain
Peer reviewed by Dr Surangi Mendis, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 10 Aug 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Cervical spondylosisWhiplash neck sprainTorticollis
A sudden-onset (acute) bout of neck pain is common. Two out of three people will have neck pain at some time in their lives. In most cases it is not due to a serious condition or neck problem and often the exact cause for the pain is not clear.
The usual advice is to keep the neck active. Painkillers can be helpful until the pain eases. Persistent (chronic) pain develops in some cases and further treatment may then be needed.
At a glance
Neck pain is common, affecting about 1 in 2 people at some point.
Most neck pain is 'nonspecific' and can be caused by minor strains or poor posture.
Conditions like whiplash, torticollis, or wear and tear can also cause neck pain.
Keep your neck moving gently and take painkillers to help manage the pain.
See a doctor if pain worsens, lasts over 4-6 weeks, or if you develop arm weakness or numbness.
In this article:
Video picks for Other signs and symptoms
Continue reading below
What are the types and causes of neck pain?
Neck pain is common. About 1 in 2 people develop a bout of neck pain at some time in their lives. It is most common in those aged 35-50 years, and it is more common in women than in men.
Types and causes of neck pain include:
Nonspecific neck pain
This is the most common type. This is sometimes called 'simple' or 'mechanical' neck pain. Often the exact cause or origin of the pain is not known. It may include minor strains and sprains to muscles or ligaments in the neck.
Bad posture may also be a contributing factor in some cases. For example, neck pain is more common in people who spend much of their working day at a desk, with a 'bent-forward' posture.
Whiplash
This is most commonly due to an accident involving a vehicle, such as a car crash. It can cause neck pain. See the separate leaflet called Whiplash Neck Sprain for more details.
Sudden-onset (acute) torticollis
This is sometimes called 'wry neck'. A torticollis is a condition in which the head becomes twisted to one side and it is very painful to move the head into a straight position. The cause of acute primary torticollis is often not known although it may be due to a minor strain or sprain to a muscle or ligament in the neck.
It is common for people to go to bed feeling fine and to wake up the next morning with an acute torticollis. The pain usually eases and clears away, without any treatment, over a few days.
Occasionally, torticollis is due to more serious causes. See the separate leaflet called Torticollis for more details.
Wear and tear
Wear and tear of the vertebrae and the discs between the vertebrae is a common cause or recurring or persistent neck pain in older people. This is sometimes called cervical spondylosis.
However, most people over the age of 50 have some degree of degeneration (spondylosis) without getting neck pain. See the separate leaflet called Cervical Spondylosis for more details.
Cervical radiculopathy
When the root of a nerve is pressed on or damaged as it comes out from the spinal cord in the neck (cervical) region, the condition is known as cervical radiculopathy.
As well as neck pain, there are symptoms such as numbness, pins and needles, and pain and weakness in parts of an arm supplied by the nerve. These other symptoms may actually be the main symptoms rather than neck pain.
The common causes of a radiculopathy are cervical spondylosis and a prolapsed disc. (A prolapsed disc is sometimes called a 'slipped disc' but the disc does not actually slip. What happens is that part of the inner softer area of the disc bulges out (prolapses) through the outer harder part of the disc, pressing on the nerve as it passes out of the vertebra.)
Various less common disorders can also cause cervical radiculopathy. These are discussed in more detail in the cervical spondylosis leaflet.
Rarer and more serious causes
These include rheumatoid arthritis, bone disorders, infections, cancers and serious injuries that damage the vertebrae, spinal cord or nerves in the neck.
The rest of this article deals only with the common 'nonspecific neck pain'.
What causes neck pain?
Neck pain symptoms
Back to contentsPain develops in the neck and may spread to the shoulder, upper back or base of the skull. Movement of the neck feels restricted and moving the neck may make the pain worse. The pain sometimes spreads down an arm, sometimes as far as the fingers.
Sometimes, 'pins and needles' develop in part of the arm or hand. This is due to irritation of a nerve going to the arm from the spinal cord in the neck.
Continue reading below
What is the outlook for neck pain?
Back to contentsThe outlook is usually good in most cases of sudden-onset (acute) neck pain. Symptoms commonly begin to improve after a few days, and are usually gone within a few weeks. However, the time taken for symptoms to settle varies from person to person.
Some people develop persistent (chronic) neck pain. In chronic neck pain, the tendency is for the pain to come and go with 'flare-ups' from time to time.
Do I need any tests?
Back to contentsUsually not. Nonspecific neck pain can be identified from the description of the pain and by an examination. Therefore, usually no tests are needed. There is no test that can prove or confirm nonspecific neck pain.
As previously mentioned, many people over the age of 50 will show some degree of 'wear and tear' (degeneration) on an X-ray, without this necessarily being the cause of the pain.
Current UK guidelines are clear that routine tests such as X-rays and scans should not be done if the diagnosis of nonspecific neck pain is made. Tests such as X-rays or scans may be advised in certain situations. This is mainly if there are symptoms, or signs during a doctor's examination, to suggest that there may be a more serious underlying cause for the neck pain.
Continue reading below
Can neck pain indicate a more serious problem?
Back to contentsA clinician's assessment and examination can usually determine that a bout of neck pain is nonspecific and not due to a more serious cause. The following are the sort of symptoms that may indicate a more serious problem:
If neck pain develops when ill with other problems such as rheumatoid arthritis, AIDS, or cancer.
If the pain becomes progressively worse.
If some function of an arm is affected. For example, weakness or clumsiness of a hand or arm, or persistent loss of feeling (numbness). (As mentioned, some pins and needles may occur with nonspecific neck pain. However, this is mild and usually goes within four weeks.)
If feeling generally unwell with other symptoms such as weight loss or a high temperature (fever).
If the neck bones (vertebrae) are very tender (which may indicate a bone problem).
If any problems develop with walking or with passing urine. This may indicate problems with pressure on the spinal cord.
What are the treatments for neck pain?
Back to contentsExercise your neck and keep active
The aim is to keep the neck moving as normally as possible. At first, the pain may be quite bad and it may be necessary to rest for a day or so. However, it is important to exercise the neck gently as soon as possible. It should not be allowed to 'stiffen up'.
The range of the neck movements should be increased gradually. Every few hours the neck should be gently moved in each direction. This should be done several times a day and, as far as possible, normal activities should be continued. Damage will not be caused to the neck by moving it.
Medicines
Painkillers are often helpful.
Paracetamol at full strength is often sufficient. For an adult this is two 500 mg tablets, four times a day.
Anti-inflammatory painkillers. Some people find that these work better than paracetamol. They can be used alone or combined with paracetamol. They include ibuprofen which can be bought at pharmacies or obtained on prescription. Other types such as naproxen need a prescription. Some people with stomach ulcers, asthma, high blood pressure, renal impairment, or heart failure may not be able to take anti-inflammatory painkillers.
A stronger painkiller such as codeine is an option if anti-inflammatories do not suit or do not work well. Codeine is often taken in addition to paracetamol. Constipation is a common side-effect from codeine. To prevent constipation, have lots to drink and eat foods with plenty of fibre.
Other treatments
Some other treatments which may be advised:
A good posture may help. Check that the sitting position at work or at the computer is not poor. It is important to make sure that the head is not flexed forward and also that the back is straight upright when sitting and working. Yoga, Pilates and the Alexander Technique all improve neck posture but their value in treating neck pain is uncertain.
A firm supporting pillow seems to help some people when sleeping. Try not to use more than one pillow.
Physiotherapy:
Various treatments may be advised by a physiotherapist. These include traction, heat, cold, manipulation, etc. The value of each of these treatments is uncertain, as the results of research studies looking at which treatments work best can be conflicting.
However, what is often most helpful is the advice a physiotherapist can give on neck exercises to do at home.
Low-level laser therapy (LLLT) is a relatively uncommon, non-invasive treatment for neck pain, in which non-thermal laser irradiation is applied to sites of pain. It can be effective in some people.
Treatment may vary and medical advice should be sought:
If the pain becomes worse.
If the pain persists beyond 4-6 weeks.
If other symptoms develop such as loss of feeling (numbness), weakness, or persistent pins and needles in part of an arm or hand, as described previously.
Other pain-relieving techniques may be tried if the pain becomes persistent (chronic). A pain management programme may be offered to help control and live with your pain. Chronic neck pain is also sometimes associated with anxiety and depression which may also need to be treated.
Understanding the neck
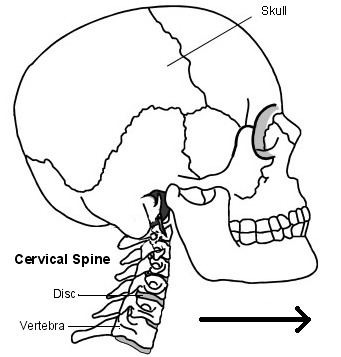
Back to contentsThe back of the neck includes the cervical spine and the muscles and ligaments that surround and support it. The cervical spine is made up of seven bones called vertebrae.
The first two are slightly different to the rest, as they attach the spine to the skull and allow the head to turn from side to side.
The lower five cervical vertebrae are roughly cylindrical in shape with bony projections.
The sides of the vertebrae are linked by small facet joints.
Between each of the vertebrae is a disc. The discs are made of a tough fibrous outer layer and a softer gel-like inner part. The discs act like shock absorbers and allow the spine to be flexible.
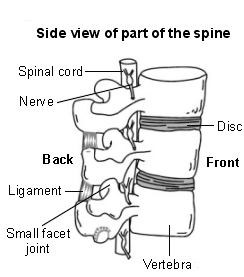
Strong ligaments attach to adjacent vertebrae to give extra support and strength. Various muscles attached to the spine enable the spine to bend and move in various ways. (The muscles and most ligaments are not shown in the diagram, for clarity.)
The spinal cord, which contains nervous tissue carrying messages to and from the brain, is protected by the spine. Nerves from the spinal cord come out from between the vertebrae in the neck to take and receive messages to the neck and arms. A major blood vessel called the vertebral artery also runs alongside the vertebrae to carry blood to the rear (posterior) part of the brain.
Cervical spine
Side view of part of the spine
Patient picks for Other signs and symptoms

Signs and symptoms
Hiccups
A hiccup is an involuntary contraction of your diaphragm that is followed by the closing of your glottis - the top of your windpipe - which makes the 'hic' sound. Hiccups are common and nothing to worry about.
by Dr Hayley Willacy, FRCGP

Signs and symptoms
Watering eyes
Watering eyes are common and can affect anyone. A blocked tear duct is the most common cause, especially in babies and older people, but there are a number of other causes. They usually get better on their own.
by Dr Hayley Willacy, FRCGP
Frequently asked questions
What is 'nonspecific' neck pain and what causes it?
Nonspecific neck pain is the most common type and is sometimes called 'simple' or 'mechanical' neck pain. Often, the exact origin of the pain isn't known, but it can be due to minor strains or sprains of muscles or ligaments in the neck. Bad posture, especially for people who work at a desk with a 'bent-forward' posture, can also be a contributing factor.
How long does acute neck pain typically last?
For sudden-onset (acute) neck pain, the outlook is usually good. Symptoms commonly start to improve after just a few days and generally disappear within a few weeks. However, the time it takes for symptoms to fully settle can vary from person to person.
Can I continue with my normal activities if I have neck pain?
Yes, it is important to keep your neck moving as normally as possible. While you might need to rest for a day or so if the pain is severe, you should gently exercise your neck as soon as you can. Gradually increase the range of movements, moving your neck in each direction several times a day. You should continue with your normal activities as much as possible, as moving your neck won't cause damage.
What kind of pillow is recommended for sleeping with neck pain?
Some people find that using a firm supporting pillow helps when they sleep. It's also recommended to try not to use more than one pillow.
When should I consider seeking further medical advice for my neck pain?
You should seek medical advice if your pain gets worse, if it continues beyond 4-6 weeks, or if you develop new symptoms. These include loss of feeling (numbness), weakness, or persistent pins and needles in any part of your arm or hand.
Can 'wear and tear' always cause neck pain, even in older people?
Wear and tear of the vertebrae and the discs in the neck, also known as cervical spondylosis, is a common cause of recurring or persistent neck pain in older individuals. However, it's important to note that most people over the age of 50 will show some degree of this degeneration without experiencing any neck pain.
Further reading and references
- Gross A, Langevin P, Burnie SJ, et al; Manipulation and mobilisation for neck pain contrasted against an inactive control or another active treatment. Cochrane Database Syst Rev. 2015 Sep 23;(9):CD004249. doi: 10.1002/14651858.CD004249.pub4.
- Gross AR, Paquin JP, Dupont G, et al; Exercises for mechanical neck disorders: A Cochrane review update. Man Ther. 2016 Aug;24:25-45. doi: 10.1016/j.math.2016.04.005. Epub 2016 Apr 20.
- Barreto TW, Svec JH; Chronic Neck Pain: Nonpharmacologic Treatment. Am Fam Physician. 2019 Aug 1;100(3):180-182.
- Neck pain - non-specific; NICE CKS, April 2023 (UK access only)
- Neck pain - cervical radiculopathy, NICE CKS, November 2023 (UK access only)
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Surangi Mendis, MRCGP
Consultant and Medical Author
MBBS, BSc (1st), MRCGP (2014), DFSRH, PGcert otology and audiology
Surangi Mendis is a consultant in Audiovestibular Medicine and Neuro-otology at The Royal National ENT and Eastman Dental Hospitals, UCLH.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 8 Aug 2028
10 Aug 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.