Cholecystitis
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 19 Sept 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:GallstonesAcute pancreatitisERCP
Cholecystitis is a painful condition caused by an inflamed gallbladder. The most common cause is gallstones.
In this article:
Video picks for Liver and gallbladder
Continue reading below
What is cholecystitis?
Cholecystitis means inflammation of the gallbladder. Most cases are caused by gallstones. Women are affected more often than men.
People with acute cholecystitis are normally admitted to hospital for treatment with painkillers, antibiotics, and fluids given through a drip into a vein.
The inflammation may settle down with treatment. Surgery to remove the gallbladder is usually advised to prevent further bouts of cholecystitis. For some people, a procedure to drain bile from the gallbladder is needed, particularly if they can't have surgery.
You can find out more about the gallbladder and gallstones in our separate leaflet called Gallstones and Bile.
How do gallstones cause cholecystitis?
Most people with gallstones do not have any symptoms or problems and do not know they have them. Commonly, the stones simply stay in the gallbladder and cause no harm. However, in some people, gallstones can cause problems. See the separate leaflet called Gallstones and Bile for more details.
Gallstones causing cholecystitis
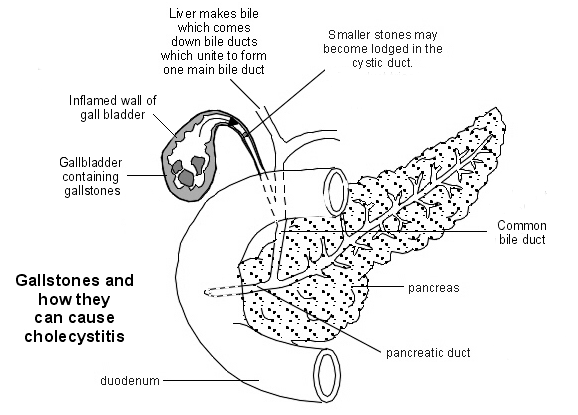
Cholecystitis is one problem that can occur with gallstones. About 19 in 20 cases of cholecystitis are thought to be caused by gallstones.
What seems to happen is that a gallstone becomes stuck in the cystic duct (this is the tube that drains bile out from the gallbladder into the bile duct).
Bile then builds up in the gallbladder, which becomes stretched (distended). Because of this, the walls of the gallbladder become inflamed. In some cases the inflamed gallbladder becomes infected. An infected gallbladder is more likely to lead to complications.
Cholecystitis symptoms
Back to contentsThe symptoms of acute cholecystitis tend to be quite characteristic. They usually come on rather quickly and people with it often feel very unwell. They are:
Pain in the upper tummy (abdomen) - the main symptom. It is usually worse on the right side, under the ribs. The pain may travel (radiate) to the back or to the right shoulder and tends to last several hours. The pain tends to be worse on breathing in deeply.
Feeling of sick (nausea).
Vomiting.
When examining the tummy (abdomen) of someone with cholecystitis, healthcare professionals might find something called 'Murphy's sign', meaning an increase in pain when the doctor places their hand under the ribs on the right hand side, and then asks the person to take a deep breath.
Continue reading below
What does an ultrasound scan do?
Back to contentsAn ultrasound scan is a generally painless test which uses sound waves to scan the tummy (abdomen). It takes around 30 minutes to complete the scan. An ultrasound scan can usually detect gallstones and also whether the wall of the gallbladder is thickened (as occurs with cholecystitis). If the diagnosis is in doubt then other more detailed scans may be done.
Are there any other tests I might need?
Back to contentsOther tests that might be done in hospital include:
Blood tests, to look for signs of infection and inflammation, as well as to check the liver.
A computerised tomography (CT) scan of the tummy (abdomen).
Continue reading below
What else could cause cholecystitis symptoms?
Back to contentsThe symptoms of cholecystitis are quite characteristic but other conditions can sometimes appear similar. These include appendicitis, a stomach ulcer, and pancreatitis. Pneumoniaof the bottom part of the right lung can cause similar symptoms.
All of these can make you seriously unwell so it's important to get the diagnosis right. The tests performed in hospital will help to check the diagnosis.
Cholecystitis treatment
Back to contentsThe main treatments for cholecystitis are:
Pain relief.
Intravenous fluids (through a drip).
Antibiotics; usually intravenously at first, and later switched to tablets.
Surgery to remove the gallbladder. This is called a cholecystectomy.
Sometimes, a plastic tube is inserted through the skin to drain infected bile from the gallbladder. This is called a percutaneous cholecystostomy.
This is often done when people are too unwell to have surgery.
Surgery for cholecystitis
For many people, surgery to remove the gallbladder (cholecystectomy) is recommended, because there is a high risk of cholecystitis occurring again, and it may cause serious problems. Removing the gallbladder stops cholecystitis from happening again.
Surgeons used to recommend waiting for 6-8 weeks, or longer, for the inflammation to settle down, before performing a cholecystectomy.
We now know that it's usually better to operate much sooner.
In the UK, the National Institute for Health and Care Excellence (NICE) recommends that people with cholecystitis are offered an operation to remove the gallbladder within a week of diagnosis. However, not all hospitals offer this. Surgeons might also recommend waiting longer if someone is too sick to have an operation.
Different techniques to remove the gallbladder may be used depending on various factors.
Keyhole surgery is now the most common way to remove a gallbladder. The medical term for this operation is laparoscopic cholecystectomy. It is called keyhole surgery as only small cuts are needed in the tummy (abdomen) with small scars remaining afterwards. The operation is done with the aid of a special telescope that is pushed into the abdomen through one small cut. This allows the surgeon to see the gallbladder. Instruments pushed through another small cut are used to cut out and remove the gallbladder. Keyhole surgery is not suitable for all people.
Some people need a traditional operation to remove the gallbladder. This is called an open cholecystectomy. In this operation a larger cut is needed to get at the gallbladder.
A newer approach called natural orifice transluminal endoscopic surgery (NOTES) is still in the development stage. An operating telescope is inserted into one of the natural openings of the body such as the mouth, anus or vagina to perform the surgery. As yet, there isn't enough evidence to recommend it over other approaches.
Do I have to have surgery?
Back to contentsSurgery is usually recommended for people with cholecystitis. Treatment with antibiotics, fluids, and pain relief can settle down the inflammation from cholecystitis, but there's a high chance of it coming back without surgery. In one study, about 1 in 3 people who had cholecystitis and didn't have surgery developed further problems from gallstones later on.
However, people can choose not to have surgery.
For some people, surgeons may also feel that surgery is too risky (for example, if they have serious medical conditions that mean they won't survive an operation).
Speak to your clinical team to find out what the options are. They should be able to tell you the risks and benefits of having surgery, as well as the risks and benefits of other options, such as not having an operation, to help you decide what's right for you.
What you can expect after surgery, including possible complications, is covered in our separate leaflet called Gallstones and Bile.
Patient picks for Liver and gallbladder

Digestive health
Non-alcoholic fatty liver disease
Non-alcoholic fatty liver disease (NAFLD) describes a range of conditions caused by a build-up of fat within liver cells.
by Dr Doug McKechnie, MRCGP

Digestive health
Gallstones
Gallstones are common but cause no symptoms in two out of three people who have them. They sometimes cause pain, yellowing of your skin or the whites of the eyes (jaundice), inflammation of the pancreas (pancreatitis) and gallbladder inflammation. Surgery is the usual treatment for gallstones that cause symptoms.
by Dr Colin Tidy, MRCGP
Further reading and references
- Gallstone disease; NICE Clinical Guideline (October 2014)
- Gallstone disease; NICE Quality standard, December 2015
- Gallstones; NICE CKS, June 2024 (UK access only)
- Cholecystitis - acute; NICE CKS, July 2021 (UK access only)
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 31 Aug 2028
19 Sept 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.