Rosacea and rhinophyma
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Rosalyn Adleman, MRCGPLast updated 6 Aug 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Rosacea article more useful, or one of our other health articles.
In this article:
Continue reading below
What is rosacea?
Rosacea is a chronic relapsing inflammatory skin disease with a high prevalence among adults of Northern European heritage with fair skin. Symptoms present in various combinations and severity, often fluctuating between periods of exacerbation and remission.1
Rosacea is characterised by recurrent episodes of facial flushing with persistent erythema, telangiectasia, papules and pustules. Ocular rosacea is usually bilateral and causes a foreign-body sensation.
What is rhinophyma?
Rhinophyma is an enlarged nose associated with rosacea which occurs almost exclusively in men. See the section on rhinophyma at the end of the leaflet for more information.
Causes of rosacea (aetiology)2
Back to contentsThe exact cause of rosacea is unclear. It is likely to be multifactorial involving genetic and environmental factors.
A systematic review found that compared with controls, people with rosacea were more likely to be infested with Demodex mites and had significantly higher skin density of Demodex mites than controls. (Demodex mites are microscopic parasites that live in the hair follicles of mammals.) However variability between studies was high and a causal relationship could not be confirmed.
Additional factors that may trigger or worsen rosacea include:
Increasing age.
Photosensitive skin types.
Ultraviolet radiation exposure.
Smoking.
Heat or cold ambient temperature.
Spicy foods and hot drinks.
Alcohol.
Emotional stress and exercise.
Drugs such as calcium-channel blockers (may worsen vasodilatation and flushing) and topical corticosteroids.
Continue reading below
How common is rosacea? (Epidemiology)
Back to contentsIn Europe, there is an increasing prevalence from South to North: in Germany prevalence is 2.2%, in Sweden 10% and in Estonia 22%.3
Rosacea is primarily a condition of the white population; it is three times more common in women than in men and has a peak age of onset between 30 and 60 years.
For a diagnosis to be confirmed the erythema should have been present for at least three months.
Signs and symptoms of rosacea (presentation)
Back to contentsSymptoms
Patients usually complain of the skin condition over the age of 30, but direct enquiry may often reveal a long history of flushing back to early teens or before.
The symptoms are initially intermittent but progress to a constant flushing with obvious telangiectasia.
A few complain of gritty eyes and facial oedema.
Signs
The disease tends to be progressive but that does not mean that everyone will develop all features.
The skin is not greasy as in acne and may be rather dry.
Erythema and telangiectasias over the forehead and cheeks are variable.
Although the usual areas affected are the nose, cheeks and forehead, other areas, such as the neck, chest and ears, can become involved.
Sebaceous glands are prominent.
The nose may be enlarged and distorted by rhinophyma.
There may be periorbital oedema.
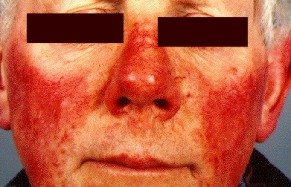
Rosacea with telangiectasia
Adult male rosacea side view
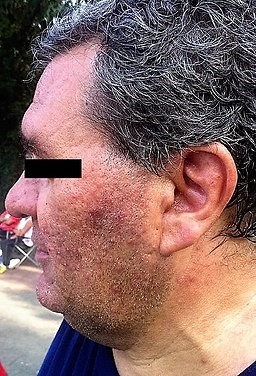
© Srecan, CC BY-SA 4.0, via Wikimedia Commons
Nose and cheeks displaying rosacea
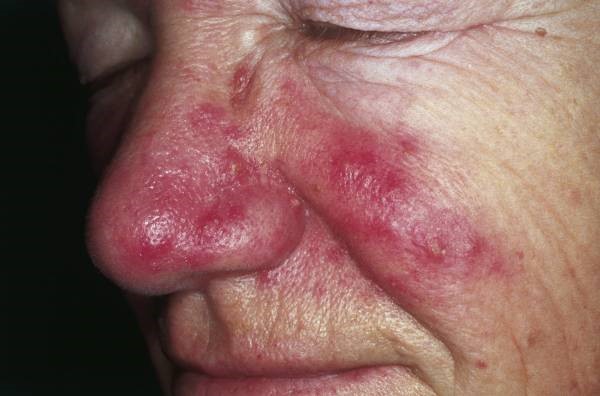
© Michael Sand, Daniel Sand, Christina Thrandorf, Volker Paech, Peter Altmeyer, Falk G Bechara, CC BY 2.5, via Wikimedia Commons
Continue reading below
Types of rosacea (classification)4
Back to contentsThere are a number of systems of rosacea classification. The mostly widely used classification recognises rosacea as a syndrome that is comprehensively depicted by four distinct clinical subtypes defined as erythematotelangiectatic, papulopustular, phymatous, and ocular rosacea:
Papulopustular rosacea (PPR) is the classical presentation. Patients are typically middle-aged women with a red central portion of their face that contains small erythematous papules surmounted by pinpoint pustules. They may have flushing. Telangiectasias are often present but may be difficult to distinguish from the erythematous background in which they exist.
Phymatous rosacea shows marked skin thickenings and irregular surface nodularities of the nose, chin, forehead, one or both ears and/or the eyelids. There are four histological types of rhinophyma that include glandular, fibrous, fibroangiomatous and actinic.
Ocular rosacea may precede the cutaneous form by years but often they develop together. The ocular signs include blepharitis, conjunctivitis, inflammation of the lids and meibomian glands, interpalpebral conjunctival hyperaemia and conjunctival telangiectasia. There may be stinging or burning of the eyes, dryness, irritation with light, or foreign body sensation. This may sometimes be confused with blepharitis.
Erythematotelangiectatic rosacea shows central facial flushing, often with burning, stinging or itching. The redness usually spares around the eyes. They usually have skin with a fine texture that lacks a sebaceous quality typical of other types. The erythematous areas of the face at times appear rough with scale likely due to chronic, low-grade dermatitis. The burning or stinging is exacerbated when topical treatments are applied. The flushing often progresses to a permanent erythema and telangiectasias over the affected areas.
Differential diagnosis2
Back to contentsAcne vulgaris, especially if it presents early in life. However, there are usually no comedones in people with rosacea. In addition, rosacea also tends to worsen with ultraviolet light, whereas acne tends to improve.
Seborrhoeic dermatitis which is more likely to cause flaking and dryness of the skin. It can co-exist with rosacea though.
Contact dermatitis
Perioral dermatitis from use of potent steroids on the face.
Corticosteroid-induced dermatitis.
Systemic lupus erythematosus or discoid lupus erythematosus.
Folliculitis.
Erysipelas.
Keratosis pilaris
Photosensitive eruptions or photodamage.
Rhinophyma may resemble lupus pernio from sarcoidosis.
Mastocytosis..
Especially when flushes start in a woman aged around 50, hot flushes may suggest the menopause.
Ophthalmic symptoms may not be recognised as part of the disease although they occur to some extent in over 50%.
Flushing
Causes of flushing are many and include:
Heat or changes in temperature.
Alcohol.
Caffeine.
Spicy foods.
Stress or embarrassment.
Sun or wind.
Medication that causes vasodilatation.
Diagnosing rosacea (investigations)
Back to contentsIn all types of rosacea the diagnosis is usually made clinically after taking a history and examining the patient. Many patients only have mild symptoms and do not actually consult their doctor. A history of flushing preceding onset of the erythema and an association with triggers can be helpful.
Where the diagnosis is in doubt a skin biopsy can be helpful; however, this is unnecessary in most cases.
Management of rosacea2
Back to contentsTreatment of rosacea depends on the severity and type of rosacea present. Although rosacea's impact on physical health is limited, it has profound effects on a person's psychological well-being.5 Therefore, treating rosacea can greatly affect a person's quality of life. Although there are numerous treatments available, none of these is completely curative.
The latest advances in rosacea treatment include skin care and cosmetic treatments, topical therapies, oral therapies, laser- and light-based therapies, injection therapies, treatments for specific types of rosacea, treatments for systemic comorbidities, and combination therapies.6
Non-drug treatment
Reassure patients of the benign nature of the condition and the relative rarity of any complications (including development of rhinophyma).
Avoid precipitating or aggravating factors for their trigger factors of flushing.
Facial massage may reduce oedema.
High factor sunscreens should be applied daily. Ultraviolet protection sunglasses may be helpful for people with features of ocular rosacea.
Avoid astringents, toners, menthols, camphor, waterproof cosmetics requiring solvents to be removed, or products containing sodium lauryl sulfate.
Judicious use of cosmetics may improve appearance significantly and, in doing so, greatly reduce distress. Yellow or green-tinted cosmetics help camouflage erythema.
If the skin is dry use emollients (hypoallergenic and non-comedogenic emollient creams).
Avoid topical steroids.
Drug treatment
Drug treatment varies according to the phenotype.
1st line treatment
Persistent erythema - topical brimonidine 0.5% gel (a topical alpha-adrenergic agonist) once daily on an 'as needed' basis, for temporary relief of symptoms.
Mild-to-moderate papules and/or pustules - topical ivermectin (an anthelmintic and insecticidal preparation) once daily for 8–12 weeks.
Alternative topical preparations are metronidazole 0.75% applied twice daily or azelaic acid 15% applied twice daily, if ivermectin is not available or inappropriate, for example for pregnant or breastfeeding women.
Moderate-to-severe papules and/or pustules, prescribe a combination of topical ivermectin, depending on local prescribing guidelines, together with oral doxycycline 40 mg once daily as a modified-release preparation for 8–12 weeks.
Alternative topical preparations are metronidazole 0.75% applied twice daily or azelaic acid 15% applied twice daily. Alternative oral preparations are oxytetracycline 500 mg twice daily or tetracycline 500 mg twice daily, or erythromycin 500 mg twice daily for pregnant or breastfeeding women.
Inflamed phymatous disease, consider prescribing oral doxycycline 40 mg once daily as a modified-release preparation (off-label indication) for 6 weeks.
2nd line treatment
Mild-to-moderate papules and/or pustules, if there is little or no improvement, consider prescribing a combination of topical preparation together with oral doxycycline 40 mg once daily as a modified-release preparation for 8–12 weeks. Electrodessication, intense pulsed light (IPL) therapy, or pulsed dye/Nd:YAG laser therapy for persistent erythema and/or telangiectasia.
Ocular rosacea treatment 2
Patients with ocular rosacea should undertake regular lid hygiene (as in the treatment of blepharitis) using diluted baby shampoo (diluted 1:10 in warm water) and a cotton bud with warm compress.
Artificial tears should be used at frequent intervals.
Referral2
Back to contentsConsider arranging referral to a dermatologist if:
Persistent or severe erythema, inflammatory papules and/or pustules have not responded to optimal management in primary care.
Severe telangiectasia has not responded to self-management advice.
An uncertain diagnosis.
Specialist management options include:
Oral isotretinoin for severe inflammatory papules and/or pustules, or clinically inflamed phymatous disease.
Electrodessication, intense pulsed light (IPL) therapy, or pulsed dye/Nd:YAG laser therapy for persistent erythema and/or telangiectasia.
Laser therapy or non-laser physical modalities, such as electrosurgery, microdermabrasion, excision, loop cautery, or scissor sculpting, for clinically non-inflamed severe phymatous disease.
Consider arranging referral to a local skin camouflage service (may be available through the local dermatology service). Patients may self-refer to the charity Changing Faces, which provides education from skin camouflage practitioners on the use and application of cosmetic camouflage creams and powders.7
Consider arranging referral to a plastic surgeon if there is prominent non-inflamed phymatous disease.
Arrange referral to an ophthalmologist if:
A serious eye complication, such as keratitis or anterior uveitis, is suspected.
Other associated ocular symptoms are severe or do not respond to optimal management in primary care.
Prognosis2 8
Back to contentsThe long-term prognosis of rosacea is variable:
People with mild forms of rosacea may be able to control their symptoms simply by avoiding irritants and vasodilating triggers.
Many people with rosacea have mild symptoms and are quite satisfied with their response to treatment and will not require any regular medicines.
Rosacea may progress in severity and also transform to include additional clinical phenotypes. It is often characterised by repeated remissions and exacerbations.
Progressive disease may include severe complications, such as rosacea fulminans
The risk of relapse is high.
A retrospective study of 234 people with different presentations of rosacea in dermatology clinics, with a median follow up of 17.5 months, found:
Partial remission in 61.5% of all participants.
Complete remission in 20.9% of all participants (median time to complete remission was 56 months).
People with inflammatory papules and pustules alone had a more favourable prognosis than other or mixed clinical presentations.
Rhinophyma9 10
Back to contentsRhinophyma is an advanced stage of rosacea affecting the nasal soft tissues and resulting in disruption of the nasal architecture, airway obstruction, and disfigurement of the nose. Rhinophyma presents with hypertrophy of the nasal soft tissues, erythema, telangiectasias, nodules, and lobules with a bulbous appearance. Significant psychosocial morbidity is associated with rhinophyma.
Treatment options vary, and include laser therapy, scalpel excision, electrocautery and the subunit method (uses six nasal flaps to provide exposure for removal of rhinophymatous tissue and enhance structure).
A review found that the subunit method had the highest complication and revision rates, followed by carbon dioxide laser therapy. Outcomes between carbon dioxide laser and scalpel therapy and electrocautery were equivalent. Patient satisfaction was common post-therapy regardless of the treatment method. The review found that over 89% of patients would recommend undergoing treatment for rhinophyma irrespective of treatment type.
Further reading and references
- Rainer BM, Kang S, Chien AL; Rosacea: Epidemiology, pathogenesis, and treatment. Dermatoendocrinol. 2017 Oct 4;9(1):e1361574. doi: 10.1080/19381980.2017.1361574. eCollection 2017.
- Rosacea; NICE CKS, January 2021 (UK access only).
- Wollina U; Recent advances in the understanding and management of rosacea. F1000Prime Rep. 2014 Jul 8;6:50. doi: 10.12703/P6-50. eCollection 2014.
- Buddenkotte J, Steinhoff M; Recent advances in understanding and managing rosacea. F1000Res. 2018 Dec 3;7. doi: 10.12688/f1000research.16537.1. eCollection 2018.
- Two AM, Wu W, Gallo RL, et al; Rosacea: Part II. Topical and systemic therapies in the treatment of rosacea. J Am Acad Dermatol. 2015 May;72(5):761-770. doi: 10.1016/j.jaad.2014.08.027.
- Zhang H, Tang K, Wang Y, et al; Rosacea Treatment: Review and Update. Dermatol Ther (Heidelb). 2021 Feb;11(1):13-24. doi: 10.1007/s13555-020-00461-0. Epub 2020 Nov 10.
- Changing Faces
- Rosacea; BMJ Best Practice, 2025
- Hassanein AH, Vyas RM, Erdmann-Sager J, et al; Management of Rhinophyma: Outcomes Study of the Subunit Method. J Craniofac Surg. 2017 May;28(3):e247-e250. doi: 10.1097/SCS.0000000000003467.
- Ferneini EM, Banki M, Paletta F, et al; Surgical management of rhinophyma: a case report and review of literature. Conn Med. 2014 Mar;78(3):159-60.
Continue reading below
About the author

Dr Rosalyn Adleman, MRCGP
MRCGP
Dr Rosalyn Adleman, is an NHS GP working in north London.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 5 Aug 2028
6 Aug 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free