Arsenic poisoning
Peer reviewed by Dr Laurence KnottLast updated by Dr Colin Tidy, MRCGPLast updated 20 Nov 2021
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Continue reading below
What is arsenic poisoning?
Arsenic poisoning is a condition that is caused by elevated levels of arsenic in the body. Arsenic is widely used in the modern industry, especially in the production of pesticides, herbicides, wood preservatives, and semiconductors. The sources of arsenic, such as contaminated water, air, soil, and food, can cause serious human diseases.1
Arsenic is a heavy metal which is a natural component of the earth's crust. It exists in compounds that may be organic or inorganic. It is highly toxic in its inorganic form. Arsenic poisoning can occur by ingestion, inhalation and dermal absorption. Elemental arsenic is the least toxic. Trivalent arsenic is well absorbed through the skin and is 60 times more toxic than pentavalent arsenic, which is well absorbed by the gut.2 Arsine gas is highly toxic.
Toxicity is due to arsenic's effect on many cell enzymes, which affect metabolism and DNA repair. Arsenic is excreted in urine but can also accumulate in many body tissues.3
Arsenic has been used in many medicines and was widely used to treat syphilis until the mid 20th century. It is currently used to treat acute promyelocytic leukaemia and other myeloproliferative disorders.4 It has also been used as a pigment, a pesticide and a poison. Arsenic shares many toxic features with the other heavy metals like mercury and lead. It is used in the production of glass and semiconductors. A source of arsenic can be natural water supplies and, in its least toxic form, it can be found in fish and seafood.5 It is also used in various industries.
How common is arsenic poisoning? (Epidemiology)
Back to contentsIn Victorian times arsenic was famous as a homicidal or suicidal poison; it is now thankfully much harder to obtain. Health and safety at work have also improved so that, in the UK, both acute and chronic arsenic poisoning are rare. However arsenic contamination affects hundreds of millions of people globally.6
Geological contamination of underground water supplies occurs in parts of:5 7
Bangladesh (79.9 million people) and West Bengal, India (42.7 million); described by the World Health Organization (WHO) as "the largest mass poisoning of a population in history".
Chile (the Antofagasta region), Argentina, Mexico and the USA (13 million people).
China, Taiwan, Thailand.
Continue reading below
Arsenic poisoning causes (aetiology)3
Back to contentsThese include:
Arsenic contaminated drinking water (as above).
Some ayurvedic medicines. Some Chinese herbal medicines. Both as intended ingredient and as contaminant.
Pesticides,8 herbicides and fungicides - no longer licensed in the UK.
Wood preservatives.
Ceramic enamels.
Paints.
Tobacco (there may be as much as 6 micrograms (mcg) per pack).
Burning of fossil fuels - arsenic is a contaminant.
In the USA, illicit whiskey ('moonshine').9
Occupational exposure10
This can occur in:
The smelting and plating industries: arsenic is a byproduct of ores containing lead, gold, zinc, cobalt and nickel.11
The microelectronics industry: gallium arsenide is used in some semi-conductor computer chips.
Coal power plants.
Manufacture of glass and fireworks.
Use of pesticides.
Contact with wood treated with arsenic as a preservative.
Note that organic arsenics found in fish and seafood are non-toxic and not a cause of arsenic poisoning. Similarly, the long-term exposure with the cutting and burning of wood preserved with copper chrome arsenate leads to elevated blood levels but no signs or symptoms of arsenic toxicity.
Arsenic poisoning symptoms
Back to contentsAcute arsenic poisoning symptoms2 3
Arsenic poisoning symptoms usually start within 30 minutes to two hours. Ingestion of high amounts of arsenic is typically followed by a severe gastroenteritis, garlic odour and hypersalivation. There is a characteristic sequence of multi-organ failure, with neurological symptoms (within hours) and cardiac features, succeeded by adult respiratory distress syndrome and renal/liver dysfunction. Marrow suppression develops after a few days to weeks in survivors, as does alopecia and an ascending motor neuropathy.
Details of acute arsenic poisoning features
Garlic odour - often present in breath and body tissues.
Gastrointestinal (GI):
Hypersalivation, abdominal pain, vomiting, diarrhoea leading to hypovolaemic shock.
Trivalent arsenic is corrosive - may cause oral burns, dysphagia and GI bleeding.
Cardiovascular:
Myocardial depression.
Dehydration, hypovolaemia or shock.
ECG changes including ST-segment changes, prolonged QT interval, ventricular tachycardia, torsades de pointes and ventricular fibrillation.
Gangrene of extremities.
Respiratory:
Pulmonary oedema, adult respiratory distress syndrome and acute respiratory failure.
Inhaled arsenic causes irritation, bronchospasm and pulmonary oedema.
Renal and hepatic:
Haematuria or haemoglobinuria (from acute haemolysis), proteinuria, acute tubular necrosis with acute kidney injury.
Jaundice, hepatomegaly, pancreatitis.
Neurological:
CNS depression, encephalopathy and coma.
Seizures.
Haematological:
Acute haemolysis.
Bone marrow suppression.
Basophilic stippling and rouleaux formation may be seen on a blood film.
Skin: rashes.
Chronic arsenic poisoning symptoms2 3 5 10
Chronic arsenic exposure through drinking water leads to an increase in mortality which is directly related to the dose of arsenic exposure.7
Main clinical features and possible complications
Skin lesions:
Skin lesions are the most common effect of chronic exposure.
They typically start about ten years after first exposure.
Keratoses on the palms and soles are characteristic.
Mees' lines (transverse white lines on nails).
Mees' lines post-chemotherapy treatment
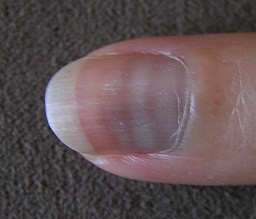
© Yannick Trottier, CC BY-SA 3.0, via Wikimedia Commons
By Yannick Trottier (Own work), CC BY-SA 3.0 , via Wikimedia Commons
Hyperpigmentation (especially on the arms and upper chest) - diffuse dark areas or 'raindrop' pigmentation.
Also, exfoliative dermatitis, alopecia, conjunctivitis, corneal ulceration.
GI:
Anorexia, weight loss, abdominal pain, diarrhoea.
Jaundice, hepatomegaly; development of portal fibrosis and cirrhosis.
Coronary heart disease, increased further in those who also smoke.
Myocarditis, pericarditis.
Hypertension.
Peripheral arterial disease.
Restrictive or obstructive lung disease.
Effects in children are seen after an average of seven years of exposure.
Haematological:
Pancytopenia,
Aplastic anaemia.
Neurological:
Peripheral neuropathy (sensory and motor at 1-3 weeks).
Muscle fasciculation and wasting.
Ataxia.
Diabetes - increased risk.
Cancer - increased risk of cancers:
Basal cell carcinoma and squamous cell carcinoma of the skin.14
Lung.
Bladder and kidney.
Possibly also lymphoid, laryngeal and liver.
History
Arsenic exposure is usually occupational or environmental but can result from deliberate poisoning.15
Exposure to arsine gas is usually the result of an industrial accident.
Take a work and travel history when a patient presents with painful peripheral neuropathy.
Other history: hobbies, unusual forms of alcohol or diet supplements, herbal medicines.
Many organ systems are involved.
Continue reading below
Differential diagnosis
Back to contentsOther forms of heavy metal poisoning - for example, lead. Botulism, gastroenteritis and haemolytic uraemic syndrome. The skin lesions may look like other forms of dermatitis.
Diagnosing arsenic poisoning (investigations)
Back to contentsAcute arsenic poisoning diagnosis2
Monitoring - for least four hours after suspected ingestion: pulse, blood pressure, respiratory rate, oxygen saturation and ECG, urine output.
Haematology, biochemistry and arterial blood gases - as for any acutely ill patient.
Urinalysis.
ECG.
Arsenic levels in blood and urine (see box below for normal levels).
CXR and plain abdominal X-ray (inorganic arsenic compounds are radio-opaque).
Important information |
|---|
Arsenic levels - normal values Normal whole blood concentration is <10 mcg/L (<130 nmol/L). Note: blood levels are of limited use, as the half-life of inorganic arsenic in the blood is short (approximately two hours). Normal 24-hour urinary excretion is <10 mcg (<130 nmol) arsenic/24 hours . Normal spot urinary arsenic concentration is <10 mcg/g creatinine (<15 nmol/mmol creatinine): Note: organic arsenical compounds found in the urine are usually from food sources such as shellfish, rather than arsenic toxicity. Ask if shellfish have been eaten in the previous few days and check whether the laboratory differentiates organic from inorganic arsenic compounds. Hair samples become positive 30 hours after exposure but may give falsely high results. They do not differentiate between ingestion and external exposure.2 |
Chronic arsenic poisoning diagnosis
Urinary concentrations are useful in chronic exposure.2
Hair samples (as above).
Arsenic levels in drinking water (high levels of arsenic in water in conjunction with relevant clinical features are useful for diagnosis in some settings).
Investigation and screening for complications may be appropriate (for example, look for diabetes, hypertension).
Arsenic levels - normal values
Arsenic poisoning treatment and management
Back to contentsManagement of acute arsenic poisoning2
In the UK, contact Toxbase® for detailed advice. The following is a summary:
Remove the patient from the source of arsenic; if there is skin contamination, wash with copious water; seal contaminated clothing.
Resuscitate ('ABC' principles).
Gastric lavage: consider if a significant amount has been ingested <1 hour previously and the patient has not vomited, or if plain X-ray indicates arsenic present in the stomach. Arsenic is absorbed primarily from the small and large intestine and rarely from the stomach. (Activated charcoal is unlikely to be of benefit - it does not absorb arsenic.)
Whole bowel irrigation with polyethylene glycol may be used to prevent arsenic absorption.
Surgical and endoscopic removal of arsenic has been used successfully.15
Supportive treatment:
Oxygen; bronchodilators if there is bronchospasm; positive end-expiratory pressure (PEEP) for pulmonary oedema.
Intravenous fluids for hypovolaemia; blood transfusion for GI haemorrhage.
Inotropes for myocardial depression.
Torsades de pointes may be treated with magnesium sulfate, or with pacing or isoprenaline (if bradycardia-dependent).
Treat seizures (diazepam, lorazepam +/- phenytoin).
Analgesia.
Renal impairment:
Maintain an alkaline urine using sodium bicarbonate over two hours and repeat as necessary.
Haemodialysis does not reduce arsenic concentrations but may be needed for acute kidney injury.
Bone marrow suppression: red cell and/or platelet transfusions.
Burns (from skin contamination) are treated conventionally.
Eye contact: treat as for a chemical eye burn.
Chelation:
Consider chelation therapy in patients who are symptomatic and/or have urine concentration >200 mcg/L.
DMPS is the chelation agent of choice. DMSA is an alternative (oral preparation only, so unsuitable if the patient is vomiting).
Dimercaprolor penicillamine have also been used (see 'History and politics', below) but are superseded by DMPS and DMSA.
Management of chronic arsenic poisoning16
Provide arsenic-free drinking water, to reduce the risk of further disease developing. Anecdotal evidence suggests that mild-moderate keratoses may improve with cessation of exposure.
Chelation therapy may have a role but its effectiveness is uncertain.17 18 19 Also, it is of no use if exposure to arsenic continues.
Micronutrients and antioxidants may be beneficial, especially in undernourished populations.17 It is recommended that all patients with skin lesions be given multivitamins.
Certain plant compounds may help to remove arsenic from tissues.17 20
Skin care for keratoses and any associated bacterial or fungal infections.
Screen and treat for complications - for example, diabetes, hypertension.
Other household members:
Check other members of the family, as they may also have been exposed.
Pregnancy and breastfeeding: arsenic is probably transferred to the baby via the placenta and breast milk.3
Prognosis3
Back to contentsThe prognosis of arsenic poisoning varies with the amount and rate of arsenic ingestion.
Effects and complications can occur at different times after exposure - from days to years later.
Arsenic poisoning prevention
Back to contentsTest all groundwater sources of drinking water for arsenic.
Provision of uncontaminated water for all is essential.
WHO guidelines advise that a value of <10 mcg/L of arsenic in drinking water is a realistic target but with the proviso to keep concentrations as low as possible. Techniques do exist to remove arsenic to levels of <5 mcg/L but this is not thought currently to be a reasonable expectation.5
Phytoremediation: some plants, notably the Chinese brake fern (Pteris vittata), have the ability to remove arsenic from the environment.21
Rainwater harvesting is an alternative in Bangladesh, which has high annual rainfall; however, it is not without risks of bacterial contamination.22
Further reading and references
- Kuivenhoven M, Mason K; Arsenic Toxicity. StatPearls, July 2021.
- Bjorklund G, Oliinyk P, Lysiuk R, et al; Arsenic intoxication: general aspects and chelating agents. Arch Toxicol. 2020 Jun;94(6):1879-1897. doi: 10.1007/s00204-020-02739-w. Epub 2020 May 9.
- TOXBASE®
- Ratnaike RN; Acute and chronic arsenic toxicity. Postgrad Med J. 2003 Jul;79(933):391-6. doi: 10.1136/pmj.79.933.391.
- Emadi A, Gore SD; Arsenic trioxide - An old drug rediscovered. Blood Rev. 2010 Jul-Sep;24(4-5):191-9. doi: 10.1016/j.blre.2010.04.001. Epub 2010 May 15.
- Guidelines for drinking-water quality, 4th edition; World Health Organization, 2017.
- Mochizuki H; Arsenic Neurotoxicity in Humans. Int J Mol Sci. 2019 Jul 11;20(14). pii: ijms20143418. doi: 10.3390/ijms20143418.
- Argos M, Kalra T, Rathouz PJ, et al; Arsenic exposure from drinking water, and all-cause and chronic-disease mortalities in Bangladesh (HEALS): a prospective cohort study. Lancet. 2010 Jul 24;376(9737):252-8. doi: 10.1016/S0140-6736(10)60481-3. Epub 2010 Jun 18.
- Lai MW, Boyer EW, Kleinman ME, et al; Acute arsenic poisoning in two siblings. Pediatrics. 2005 Jul;116(1):249-57.
- Gerhardt RE, Crecelius EA, Hudson JB; Moonshine-related arsenic poisoning. Arch Intern Med. 1980 Feb;140(2):211-3.
- Chronic arsenic poisoning - information and pictures on symptoms of chronic poisoning; DermNet NZ
- Correia N, Carvalho C, Frioes F, et al; Haemolytic anaemia secondary to arsenic poisoning: a case report. Cases J. 2009 Aug 11;2:7768. doi: 10.4076/1757-1626-2-7768.
- Chen Y, Graziano JH, Parvez F, et al; Arsenic exposure from drinking water and mortality from cardiovascular disease in Bangladesh: prospective cohort study. BMJ. 2011 May 5;342:d2431. doi: 10.1136/bmj.d2431.
- James KA, Byers T, Hokanson JE, et al; Association between lifetime exposure to inorganic arsenic in drinking water and coronary heart disease in Colorado residents. Environ Health Perspect. 2015 Feb;123(2):128-34. doi: 10.1289/ehp.1307839. Epub 2014 Oct 28.
- Karagas MR, Gossai A, Pierce B, et al; Drinking Water Arsenic Contamination, Skin Lesions, and Malignancies: A Systematic Review of the Global Evidence. Curr Environ Health Rep. 2015 Mar;2(1):52-68. doi: 10.1007/s40572-014-0040-x.
- Duenas-Laita A, Perez-Miranda M, Gonzalez-Lopez MA, et al; Acute arsenic poisoning. Lancet. 2005 Jun 4-10;365(9475):1982.
- Rahman MM, Chowdhury UK, Mukherjee SC, et al; Chronic arsenic toxicity in Bangladesh and West Bengal, India--a review and commentary. J Toxicol Clin Toxicol. 2001;39(7):683-700.
- Kalia K, Flora SJ; Strategies for safe and effective therapeutic measures for chronic arsenic and lead poisoning. J Occup Health. 2005 Jan;47(1):1-21.
- Guha Mazumder DN, De BK, Santra A, et al; Randomized placebo-controlled trial of 2,3-dimercapto-1-propanesulfonate (DMPS) in therapy of chronic arsenicosis due to drinking arsenic-contaminated water. J Toxicol Clin Toxicol. 2001;39(7):665-74.
- Kosnett MJ; The role of chelation in the treatment of arsenic and mercury poisoning. J Med Toxicol. 2013 Dec;9(4):347-54. doi: 10.1007/s13181-013-0344-5.
- Misbahuddin M, Islam AZ, Khandker S, et al; Efficacy of spirulina extract plus zinc in patients of chronic arsenic poisoning: a randomized placebo-controlled study. Clin Toxicol (Phila). 2006;44(2):135-41.
- Alkorta I, Hernandez-Allica J, Garbisu C; Plants against the global epidemic of arsenic poisoning. Environ Int. 2004 Sep;30(7):949-51.
- Karim MR; Microbial contamination and associated health burden of rainwater harvesting in Bangladesh. Water Sci Technol. 2010;61(8):2129-35. doi: 10.2166/wst.2010.031.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 19 Nov 2026
20 Nov 2021 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free