Dupuytren's contracture
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 18 Feb 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Dupuytren's contracture article more useful, or one of our other health articles.
In this article:
Continue reading below
What is Dupuytren's contracture?
Dupuytren's contracture is a benign, progressive fibroproliferative disorder of the fascia of the hands and fingers that can lead to disabling contractures.1
Excessive myofibroblast proliferation and altered collagen matrix composition lead to a thickened and contracted palmar fascia. The resultant digital flexion contractures may severely limit function.
How common is Dupuytren's contracture? (Epidemiology)1
Back to contentsDupuytren's contracture is common. The overall prevalence in the UK is about 4%, increasing to about 20% in those aged over 65 years. The incidence is highest in men older than 50 years and in women older than 60 years.
Dupuytren's contracture is most often seen in people of northern European descent.
It is up to six times more common in men than in women.
Continue reading below
Causes of Dupuytren's contracture (aetiology)
Back to contentsThe cause is unknown but genetic predisposition, trauma, inflammatory response, ischaemia, environmental factors and variable expression of proteins and growth factors within the local tissue have been implicated in the disease process.2 There is increasing evidence of a strong genetic component.3
Risk factors145
Back to contentsIncreasing age.
North European descent.
Positive family history.
Smoking. (Reported to be three times more common in smokers.)
Alcohol excess (but most affected people do not have alcohol dependence).
Diabetes mellitus. One in five people with diabetes are reported to develop Dupuytren's contracture, albeit a less severe form. It is equally common in types 1 and 2 but develops at a younger age in people with type 1 diabetes.
Occupational exposure to hand-transmitted vibration. (A report of the evidence by the Industrial Injuries Advisory Council in 2014 concluded that significant exposure to hand-held vibrating tools can more than double the risk.)6 Heavy manual work without vibration exposure may also increase the risk.78
Raised lipid levels.
Epilepsy/anticonvulsant drugs/epilepsy. It is not clear whether the association is with epilepsy or the medication used to control it.
Liver cirrhosis (whether or not it is related to alcohol).
Continue reading below
Clinical picture1
Back to contentsDupuytren’s contracture causes skin thickening, tethering, puckering, pitting, or dimpling on the palm, with firm nodules fixed to the skin and deep fascia of the palm or fingers. The nodules can occur anywhere in the palm or fingers, but the most common site is the distal palmar crease, in line with the ring or little finger. Often both hands are affected, with one hand usually more severely affected than the other. The fourth and fifth fingers are most commonly affected. The thumb and index are least likely to be affected.
It starts with pitting and thickening of the palmar skin and underlying subcutaneous tissue, with loss of mobility of the overlying skin.
Next a nodule forms which is firm and painless and fixed to the skin and deeper fascia. The nodule is palpable and later becomes visible.
A cord (a linear thickening that can resemble a tendon) then develops which begins to contract over months to years.
The contraction of the cord pulls on the metacarpophalangeal (MCP) and proximal interphalangeal (PIP) joints and leads to a progressive flexion deformity in the fingers.
Deformity can affect activities of daily living and occupation. The stage at which the patient presents will depend upon tolerance of this and is likely to depend upon the degree to which work or hobbies may be affected.
A more aggressive form can occur in which there is early age of onset, a strong family history, bilateral hand involvement and associated ectopic disease (see below).
Other areas of the body may be affected - eg, the knuckles (thickened knuckle pads over the dorsal surface of the PIP joints), soles of the feet (plantar fibromatosis) and the penis (penile fibromatosis, or Peyronie's disease).
Dupuytren's contracture on a woman's hand
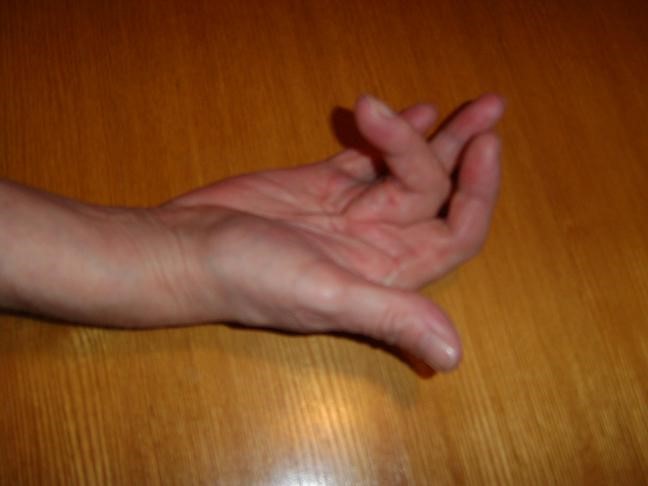
© Smartie77, CC BY-SA 3.0, via Wikimedia Commons
Examination
Back to contentsLook for:
Early skin changes: skin thickening, dimpling, pitting.
Firm nodules (the most common site is on the distal palmar crease in line with the ring finger).
Cords - longitudinal thickenings.
Contractures causing flexion deformity.
MCP joint contracture should be measured whilst applying passive extension to the PIP joint.
PIP joint contracture is measured while the MCP joint is held in flexion.
When there is 30° of flexion deformity at the MCP joint, the patient is unable to place their palm and fingers flat against a hard surface - for example, a table. This is known as Hueston's tabletop test.
If there are knuckle pads on the dorsal PIP surfaces, there is more aggressive disease.
Swan-neck deformities and boutonnière deformities may (rarely) occur.
Differential diagnosis1
Back to contentsCallus.
Ganglion.
Trigger finger.
Epithelioid sarcoma (rare).
Giant cell tumour of the tendon sheath.
Ulnar nerve palsy.
Diagnosing Dupuytren's contracture (investigations)
Back to contentsUsually a clinical diagnosis.
Due to the association with excess alcohol intake it may be judicious to take a drinking history and check LFTs.
If there is any suggestion of undiagnosed diabetes then fasting blood glucose/HbA1c should be checked.
Management of Dupuytren's contracture1
Back to contentsFor a person with contracture (who is unable to place their hand flat on a table top) or whose hand function is significantly compromised, refer them to the local hand surgery service, or to a specialist in plastic surgery or orthopaedic surgery. If there is no contracture or loss of function, there may be no need to refer, but in some cases referral may be indicated if there are painful nodules, despite no contracture or loss of function.
Treatment is usually considered when (or ideally before) functional disability occurs. It aims to restore hand function and prevent progression. Once contracture develops, early referral is recommended. This is because contracture and disability can become irreversible due to ligament remodelling; early referral means surgeons are then best placed to decide on the timing of any interventions. Surgical treatment is usually considered when the MCP joint is bent forwards by 30-45° and cannot be straightened; or the proximal interphalangeal joint is bent permanently by 10-20°.
NHS England has produced a decision tool which may be helpful for patients who are trying to decide what treatment to have for their Dupuytren's contracture (or whether to have treatment at all).9
Non-surgical treatments
Although surgical procedures such as fasciectomy or fasciotomy are often used for advanced disease, recent advances in the management of Dupuytren's disease have shown benefit of less invasive treatments, such as radiotherapy, particularly for early disease.2
Corticosteroid injections may be beneficial for some people with painful nodules (without contracture or loss of function).1
A review by the Royal College of Radiologists (RCR) states radiotherapy is effective before contracture develops and in early stages but should not be used in more advanced disease; outcomes are worse when treatment is started more than two years after the appearance of symptoms, compared to within one year. The current NICE guidance states that the evidence on the safety and efficacy of radiation therapy for early Dupuytren's disease is limited in quantity and there is uncertainty about the natural history of early Dupuytren's disease, and therefore that the procedure should only be used with special arrangements for clinical governance, consent and audit or research. It is currently available at some NHS hospitals. Radiotherapy is associated with a very small excess risk of skin cancer, with an increased risk of around 0.02% (for one hand treated) of dying from cancer compared to those who haven't had this radiotherapy.1011
Collagenase injections have been used in the past, with some studies showing similar results to needle fasciotomy, and others showing that the benefits from collagenase are less long-lasting, but collagenase is currently long-term unavailable in Europe. 1213
Surgical treatment
There is not yet evidence that one treatment is superior to others.14
Closed fasciotomy (also called percutaneous needle fasciotomy, or needle aponeurotomy)15 16
The procedure can be performed in an outpatient setting, using local anaesthesia.
With closed fasciotomy, there may be short-term benefit but by three to five years the recurrence rate can be up to 85%.
Nerve injury, tendon injury and infection are the main complications of the procedure, with a complication rate of 1% or less.
Fasciectomy
This can be a segmental fasciectomy (short segments of the cord are removed), a regional fasciectomy (the entire cord is removed) or a dermofasciectomy (the cord and overlying skin are removed followed by skin grafting). Regional fasciectomy is the most common procedure undertaken for Dupuytren's contracture.
Dermofasciectomy may be considered when there is skin involvement, aggressive or rapid recurrence, or extensive disease in younger people.
The procedure is usually done under regional block or general anaesthetic as a day case.
Splinting and hand physiotherapy are needed after surgery. A night splint is normally worn for three months. There is possibly evidence that this practice may adversely affect outcome - further trials are needed.14
Finger amputation
This is rarely done. It is used in severe cases (usually because presentation has been much delayed).
Complications of Dupuytren's contracture1
Back to contentsDupuytren's contracture can be disabling and have a detrimental effect on work and home life, particularly on hobbies that require full stretch of the fingers, such as playing certain musical instruments.
A review found a complication rate of 19% after needle fasciotomy, 17% after fasciectomy, and 12% after dermofasciectomy. The possible complications of surgery include:
Tendon rupture, digital nerve injury, and artery injury.
Infection, ischaemia, and haematoma.
Finger stiffness, swelling and pain.
Skin loss and wound healing problems.
Flare reaction: inflammatory reaction that occurs 2–3 weeks after surgery. It presents as stiffness with pain and oedema and is more common in women.
Complex regional pain syndrome (more common in women).
There are concerns about potential long-term complications of radiotherapy, such as skin cancer and sarcoma, although as yet no cases have been documented .
Prognosis1
Back to contentsDupuytren's contracture is usually a progressive and incurable condition. However about 10% will regress. 75% of people develop features of more advanced stages of the disease. The rate of progression varies with men progressing more rapidly than women and people aged under 50 years progressing more rapidly than older people.
Early-onset (before age 40 years), bilateral involvement, radial digit involvement, and involvement in other sites (such as the feet or penis) are associated with aggressive disease (Dupuytren’s diathesis).
Surgery can improve hand functionality but will not eradicate the disease. There is a risk of recurrence at the same site or elsewhere in the hand. The 10-year risk of re-operation on the same hand varies depending on the surgical technique used. It is about 20% following either limited fasciectomy or dermofasciectomy. The recurrence rate following needle fasciotomy is about 50% at 3-5 years and seems to depend on the severity of the disease.
Further reading and references
- Baron Guillaume Dupuytren; Whonamedit?
- Ledderhose disease: plantar fibromatosis; Wheeless' Textbook of Orthopaedics
- Dupuytren's Contracture; Wheeless' Textbook of Orthopaedics
- Dupuytren's disease; NICE CKS, August 2022 (UK access only)
- Black EM, Blazar PE; Dupuytren disease: an evolving understanding of an age-old disease. J Am Acad Orthop Surg. 2011 Dec;19(12):746-57.
- Ten Dam EJ, van Beuge MM, Bank RA, et al; Further evidence of the involvement of the Wnt signaling pathway in Dupuytren's disease. J Cell Commun Signal. 2016 Mar;10(1):33-40. doi: 10.1007/s12079-015-0312-8. Epub 2015 Dec 3.
- Wang Z, Wang Z, Yan Z, et al; Smoking, alcohol consumption and risk of Dupuytren's disease: a Mendelian randomization study. BMC Med Genomics. 2023 Sep 7;16(1):212. doi: 10.1186/s12920-023-01650-4.
- Descatha A, Carton M, Mediouni Z, et al; Association among work exposure, alcohol intake, smoking and Dupuytren's disease in a large cohort study (GAZEL). BMJ Open. 2014 Jan 29;4(1):e004214. doi: 10.1136/bmjopen-2013-004214.
- Dupuytren’s contracture due to hand-transmitted vibration; Report by the Industrial Injuries Advisory Council (IIAC) in accordance with Section 171 of the Social Security Administration Act 1992 considering prescription for Dupuytren’s contracture in workers exposed to hand-transmitted vibration, GOV.UK, May 2014
- Mathieu S, Naughton G, Descatha A, et al; Dupuytren's Disease and exposure to vibration: Systematic review and Meta-analysis. Joint Bone Spine. 2020 May;87(3):203-207. doi: 10.1016/j.jbspin.2020.02.001. Epub 2020 Feb 12.
- Descatha A, Bodin J, Ha C, et al; Heavy manual work, exposure to vibration and Dupuytren's disease? Results of a surveillance program for musculoskeletal disorders. Occup Environ Med. 2012 Apr;69(4):296-9. doi: 10.1136/oemed-2011-100319. Epub 2012 Jan 2.
- Decision support tools: making a decision about Dupuytren’s contracture
- Radiation therapy for early Dupuytren's disease; NICE Interventional Procedure Guidance, December 2016
- Recommendations for using radiotherapy for benign disease in the UK
- Sandler AB, Scanaliato JP, Dennis T, et al; Treatment of Dupuytren's Contracture With Collagenase: A Systematic Review. Hand (N Y). 2022 Sep;17(5):815-824. doi: 10.1177/1558944720974119. Epub 2021 Jan 21.
- Bystrom M, Ibsen Sorensen A, Samuelsson K, et al; Five-Year Results of a Randomized, Controlled Trial of Collagenase Treatment Compared With Needle Fasciotomy for Dupuytren Contracture. J Hand Surg Am. 2022 Mar;47(3):211-217. doi: 10.1016/j.jhsa.2021.11.019. Epub 2022 Jan 21.
- Rodrigues JN, Becker GW, Ball C, et al; Surgery for Dupuytren's contracture of the fingers. Cochrane Database Syst Rev. 2015 Dec 9;(12):CD010143. doi: 10.1002/14651858.CD010143.pub2.
- Diaz R, Curtin C; Needle aponeurotomy for the treatment of Dupuytren's disease. Hand Clin. 2014 Feb;30(1):33-8. doi: 10.1016/j.hcl.2013.09.005.
- Needle fasciotomy for Dupuytren's contracture; NICE Interventional Procedure Guidance, February 2004
Continue reading below
About the authorView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 17 Feb 2028
18 Feb 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free