Forearm injuries and fractures
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 6 Mar 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Forearm injuries and fractures article more useful, or one of our other health articles.
In this article:
Injury to the forearm usually results from trauma secondary to, for example, a fall, a road traffic accident or a sporting injury. It can also result from overuse. Injuries include muscle strain and contusion, crush injuries, fractures and tendon and nerve injuries.
Continue reading below
Anatomy of the forearm
The radius and ulna have an important role in positioning the hand. The ulna has a stabilising role, while the radius is articulated in a way which allows it to roll over the ulna, moving the hand from supination (external rotation) to pronation (internal rotation).
The two bones of the forearm are the radius, laterally, and the ulna, medially. Other components of the forearm include skin, blood vessels, and soft tissue.
At its upper end, the radius articulates with the capitulum of the humerus at the elbow, and with the ulna (superior radioulnar joint). At its lower end it articulates with the scaphoid and lunate bones and also with the ulna (inferior radioulnar joint).
At its upper end, the ulna articulates with the trochlea of the humerus, and with the head of the radius (superior radioulnar joint). At its lower end it articulates with the radius (inferior radioulnar joint).
The olecranon process at the upper end of the ulna forms the prominence of the elbow. The styloid processes of the radius and the ulna form prominences at the wrist.
Forearm fractures
Back to contentsForearm fractures account for most limb fractures. Wrist fractures are the most common forearm fracture.1 Fracture risk factors include osteoporosis (more common in women than in men) and malignancy (pathological fractures).
Fractures of the radius and ulna may occur in isolation - usually due to a direct blow - but these are usually associated with fracture or displacement of the other bone in that forearm.2 An epidemiological study in Denmark found that 4 out of 5 forearm fractures were treated conservatively.3
Classification
Forearm fractures can be classified as either proximal, middle or distal.
They can affect one or both forearm bones.
They are either open or closed.
Proximal forearm fractures may involve the elbow joint (see the separate Elbow injuries and fractures article; see the section below for Monteggia fractures).
Distal forearm fractures may involve the wrist (see the separate Wrist fractures article).
General assessment and initial treatment of forearm fractures
Some general principles should be followed for all forearm fractures. Specific points related to the different fracture types are discussed below. Forearm fractures in children can generally be treated differently from adult fractures because of continuing bone growth in the radius and the ulna after the fracture has healed.4
Assess Airway, Breathing and Circulation and manage as necessary.
Assess upper limb neurovascular function:
Sensory function: the median nerve supplies the thumb, index, middle and radial half of the ring finger on the palmar side of the hand and the tip of the thumb, index, middle and ring finger on the dorsum of the hand; the radial nerve supplies the dorsolateral aspect of the hand and the dorsal aspect of the thumb, index, middle and lateral half of the ring fingers; the ulnar nerve supplies the dorsal and palmar aspects of the medial half of the ring finger and the whole of the little finger.
Motor function: test the anterior interosseous branch of the median nerve by asking the patient to make the 'OK' sign (touching the tips of the first and second fingers with the thumb); test the radial nerve by asking the patient to extend their fingers or wrist against resistance; test the ulnar nerve by asking the patient to separate their fingers against resistance.
Vascular function: examine the radial (and ulnar) pulse. Assess capillary refill.
Examine the wrist, elbow and forearm for tenderness and range of motion.
Perform a complete examination for other injuries.
Immobilise the forearm and upper arm whilst waiting for X-ray or ultrasound.5
Provide analgesia.
Immediate fracture reduction is required if there is neurovascular compromise, severe displacement or skin tenting.
Orthopaedic surgeons should consider outcomes associated with nonoperative management such as lower infection rates, the possibility of rapid functional improvements and lower healthcare costs.6 Nonoperative methods for closed fractures can sometimes be more safely delivered even with more difficult fractures. This may be of particular benefit to patients with higher surgical risk.
Adult both-bone forearm fractures
Mechanism of injury: usually a significant force injury. These most commonly occur in motor vehicle accidents, and also occur from a direct blow, a fall from a height or during sport.
Presentation: pain and swelling at the site with obvious deformity.
Assessment: may be nerve involvement with paraesthesiae, paresis or loss of function. Do not elicit crepitus, as this may cause further soft tissue injury. Do not probe open fractures as this may cause deeper contamination.
Investigation: X-ray the entire length of the forearm, wrist and elbow, with AP and lateral views. Consider compartment syndrome.
Management: displaced fractures are the usual situation in adults. Operative treatment with internal fixation or intramedullary nailing will be needed in nearly all cases, so refer urgently. Closed reduction may be attempted (with sufficient sedation/analgesia ± muscle relaxants) if there is acute neurovascular compromise. Notable complications of surgery include non-union, malunion, and re-fracture after the removal of the fixation device.7
Paediatric both-bone forearm fractures
Fractures may be of greenstick type (incomplete) or complete. A greenstick fracture can occur in one bone with a complete fracture in the other. Complete fractures may be undisplaced, minimally displaced or overriding. Fractures of the proximal third are relatively rare. Middle third fractures account for about 18% of both-bone fractures and distal third fractures for about 75%.8 Late compartment syndrome may occur, unlike adults.
Mechanism of injury: usually an indirect injury following a fall on to an outstretched hand. Occasionally caused by a direct trauma.
Presentation: pain, swelling and deformity at the fracture site.
Investigation: X-rays of the wrist, elbow and whole forearm should be taken.
Management: unlike the management of these fractures in adults, conservative management is still the first line of treatment for paediatric forearm fractures, especially in children less than 10 years old. Due to a child’s physeal growth potential, varying degrees of fracture angulation can be accepted - depending on the age of the child and his or her ability to remodel.9 After reduction, forearm pronation and supination should be checked and the arm placed in a long-arm cast or splint. Surgical treatment is by open reduction and plating/intramedullary nails, depending on the degree of overriding/angulation.8
Radial shaft fractures (Galeazzi fractures)
Definition: solitary fractures of the distal one third of the radius with accompanying subluxation or dislocation of the distal radioulnar joint (DRUJ). The synonym is reverse Monteggia's fracture.10
Mechanism of injury: commonly caused by a fall on to an extended, pronated wrist.
Presentation: pain, swelling and deformity of the wrist and forearm. Tenderness and swelling at the distal radius and tenderness at the DRUJ.
Investigation: X-ray the entire length of the forearm including wrist and elbow joints; AP and lateral views are usually sufficient.
Management: in adults, this requires surgical open reduction of the distal radius and DRUJ with internal fixation. In children, the fracture can often be treated by closed reduction with longitudinal traction and correction of radial angulation. General anaesthesia (GA) may be required in difficult cases. If closed reduction under GA fails, K-wire insertion may be needed to lever the fracture into position. Open reduction may be needed in some cases.10
Ulnar shaft fractures
Definition: isolated mid-shaft ulnar fractures have the synonym 'nightstick fracture'.
Mechanism of injury: usually caused by a direct blow to the ulnar border, classically if someone receives a blow from an object whilst raising their arm in defence.11
Presentation: point tenderness over the ulnar shaft, and forearm swelling.
Investigation: need to X-ray the ulna from the wrist to the elbow.
Management: this requires orthopaedic referral. Non-displaced or minimally displaced fractures can be treated with a posterior splint from the mid-upper arm to the dorsum of the metacarpal joints with the wrist in slight extension, the forearm in a neutral position and the elbow at 90°. After 7-10 days, when swelling has subsided, use a plaster sleeve or functional brace for the following 4-6 weeks. Monitor weekly for the first three weeks for any displacement. Fractures with marked displacement or angulation should be treated with open reduction and internal fixation.
Monteggia's fractures
Definition: these are fractures of the proximal third (usually) of the ulna with associated dislocation of the radial head. Classified as:
Type I - fracture with anterior radial head dislocation. This is the most common (60%).12
Type II - fracture of the proximal ulna with posterior or posterolateral dislocation of the radial head (15%).12
Type III - fracture of the ulnar metaphysis with lateral or anterolateral dislocation of the radial head (20%).12
Type IV - fracture of both the radius and ulna at their proximal third with anterior dislocation of the radial head (5%).12
Mechanism of injury: usually caused by a fall on to an outstretched, extended and pronated elbow, or by a direct blow.
Presentation: acute, severe pain and swelling in the forearm and elbow. Damage may occur to the posterior interosseous nerve.
Monteggia fracture
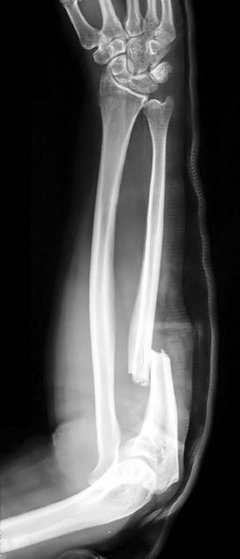
© Jane Agnes (own work), via Wikimedia Commons
Investigation: X-ray the entire length of the radius and ulna, including the wrist and elbow - AP and lateral views are usually sufficient but there may be a need for radiocapitellar views.
Management: in adults, immobilise the joint in a splint and refer for open reduction and internal fixation. Most paediatric Monteggia's fractures are treated closed.13
Isolated proximal ulnar fractures are rare. Always examine for a Monteggia's fracture/dislocation.
Complications of forearm fractures
See the general separate Complications from fractures article.
Non-union and malunion (uncommon).
Compromise of the brachial/radial artery blood supply.
Median, ulnar or radial nerve injury.
Infection (more likely if the fracture is secondary to a crush injury).
Compartment syndrome (more common in both-bone forearm fractures).
Radioulnar fusion (synostosis).
Re-fracture.
Prevention of forearm fractures
Prevention of osteoporosis.
Adequate treatment of existing osteoporosis.
The use of wrist and elbow guards whilst taking part in certain sporting activities, such as mountain biking and skating.
Continue reading below
Forearm overuse injuries
Back to contentsApart from tennis and golfer's elbow (lateral and medial epicondylitis), forearm overuse injuries are not that common outside the realms of sports medicine.
Commonly, they affect athletes who take part in racquet or throwing sports. If an activity involves repetitive flexion-extension of the elbow or pronation-supination of the wrist, it can lead to an overuse injury.
Ulnar nerve injury and olecranon stress fractures can also occur if there is increased stress on the elbow joint.
Three major nerves cross the elbow joint: the median nerve, the ulnar nerve and the radial nerve. Overuse injuries or direct trauma to the elbow can affect these nerves.
Pronator syndrome and radial tunnel syndrome can occur in sports where there is excessive wrist flexion-extension or pronation-supination.
History taking is an essential part of the examination.
Pronator syndrome14
This is due to entrapment of the median nerve.
There is pain or paraesthesia over the median nerve distribution in the anterior proximal forearm. It is aggravated by throwing/swinging a racquet.
It can be distinguished from carpal tunnel syndrome because in carpal tunnel syndrome, sensation over the thenar eminence is preserved (the sensory branch of the median nerve that innervates the thenar eminence does not pass through the carpal tunnel).
There are negative Tinel's and Phalen's tests at the wrist in pronator syndrome and difficulty making the 'OK' sign.
Treatment is rest/modification of activity, ice, analgesia, physiotherapy and occupational therapy.
Radial tunnel syndrome15
This is due to entrapment of the radial nerve.
Pain is experienced distal to the lateral epicondyle of the humerus and radiates down the dorsum of the forearm.
It is often misdiagnosed as lateral epicondylitis.
A Tinel's test approximately 6 cm distal to the lateral epicondyle over the radial nerve can reproduce pain. There is also pain on resisted supination with the forearm extended.
Treatment is rest/modification of activity, ice, analgesia, physiotherapy and occupational therapy.
Further reading and references
- Patel DS, Statuta SM, Ahmed N; Common Fractures of the Radius and Ulna. Am Fam Physician. 2021 Mar 15;103(6):345-354.
- Kyriakides J, Peeters W, Ahluwalia AK, et al; Paediatric forearm fractures: assessment and initial management. Br J Hosp Med (Lond). 2022 Sep 2;83(9):1-9. doi: 10.12968/hmed.2021.0564. Epub 2022 Sep 22.
- Ochen Y, Peek J, van der Velde D, et al; Operative vs Nonoperative Treatment of Distal Radius Fractures in Adults: A Systematic Review and Meta-analysis. JAMA Netw Open. 2020 Apr 1;3(4):e203497. doi: 10.1001/jamanetworkopen.2020.3497.
- Black WS, Becker JA; Common forearm fractures in adults. Am Fam Physician. 2009 Nov 15;80(10):1096-102.
- Sonin A; Fractures of the elbow and forearm. Semin Musculoskelet Radiol. 2000;4(2):171-91.
- Abrahamsen B, Jorgensen NR, Schwarz P; Epidemiology of forearm fractures in adults in Denmark: national age- and gender-specific incidence rates, ratio of forearm to hip fractures, and extent of surgical fracture repair in inpatients and outpatients. Osteoporos Int. 2014 Aug 20.
- Rodriguez-Merchan EC; Pediatric fractures of the forearm. Clin Orthop Relat Res. 2005 Mar;(432):65-72.
- Hassankhani A, Amoukhteh M, Jannatdoust P, et al; A meta-analysis on the diagnostic utility of ultrasound in pediatric distal forearm fractures. Emerg Radiol. 2024 Apr;31(2):213-228. doi: 10.1007/s10140-024-02208-2. Epub 2024 Feb 5.
- Coon M, Denisiuk M, Woodbury D, et al; Closed Fracture Treatment in Adults, When is it Still Relevant? Spartan Med Res J. 2022 Feb 24;7(1):28060. doi: 10.51894/001c.28060. eCollection 2022.
- Schulte LM, Meals CG, Neviaser RJ; Management of adult diaphyseal both-bone forearm fractures. J Am Acad Orthop Surg. 2014 Jul;22(7):437-46. doi: 10.5435/JAAOS-22-07-437.
- Wheeless' Textbook of Orthopaedics; Pediatric Both Bone Forearm Fractures. Duke Orthopaedics. Cited from textbook online October 2024
- Vopat ML, Kane PM, Christino MA, et al; Treatment of diaphyseal forearm fractures in children. Orthop Rev (Pavia). 2014 Jun 24;6(2):5325. doi: 10.4081/or.2014.5325. eCollection 2014 Apr 22.
- Galeazzi's Fracture (Adults); Wheeless' Textbook of Orthopaedics
- Ulna/Ulnar Shaft Fracture; Wheeless' Textbook of Orthopaedics
- Monteggia's Fracture; Wheeless' Textbook of Orthopaedics
- Monteggia Fractures in Children; Wheeless' Textbook of Orthopaedics
- Dididze M, Tafti D, Sherman AL; Pronator Teres Syndrome.
- Levina Y, Dantuluri PK; Radial Tunnel Syndrome. Curr Rev Musculoskelet Med. 2021 Jun;14(3):205-213. doi: 10.1007/s12178-021-09703-w. Epub 2021 Apr 23.
Continue reading below
About the author

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 5 Mar 2028
6 Mar 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free