Infant seborrhoeic dermatitis
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 15 Dec 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Seborrhoeic dermatitis in babies article more useful, or one of our other health articles.
In this article:
Synonym: cradle cap
Continue reading below
What is seborrhoeic dermatitis?1
Seborrhoeic dermatitis is a common skin condition in infants, adolescents, and adults. The characteristic symptoms-scaling, erythema, and itching-occur most often on the scalp, face, chest, back, axilla, and groin.
In infants, seborrhoeic dermatitis typically causes yellow crusty greasy scaling. This is most frequently found on the scalp and, when confined to the scalp, is known as 'cradle cap'.
In adults, seborrhoeic dermatitis usually starts around puberty.
See the separate Seborrhoeic Dermatitis article.
Pathogenesis1
Back to contentsSeborrhoeic dermatitis is a papulosquamous disorder affecting the areas with most sebum, such as the scalp, face, and trunk. There is known to be an association with skin yeasts of Malassezia spp. This is thought to be due to a reaction to the yeast, rather than a simple infection. Overactivity of the sebaceous glands in the newborn may be a factor.
Continue reading below
How common is seborrhoeic dermatitis in infants? (Epidemiology)2
Back to contentsSeborrhoeic dermatitis is extremely common in infants. Many children with the condition are not brought to the attention of the medical services and so the precise incidence is unknown. It most commonly presents in the first six weeks, and the majority resolve over the next few weeks. Less commonly, it persists for 6-9 months or more.
Seborrhoeic dermatitis symptoms3
Back to contentsSeborrhoeic dermatitis presenting in infancy is a very common condition which may be brought to the attention of the health visitor or GP.
In the majority of cases it is a benign self-limiting condition which usually clears spontaneously during the first 6-12 months of life but, in a small number, it can be particularly troublesome and require treatment.
Infant seborrhoeic dermatitis occurs most commonly in the lipid-rich areas of skin and, in infants, occurs predominantly on the scalp and upper face, producing an appearance which may give rise to some concern from parents. It may also occur behind the ears and in the creases of the neck, axillae and groins.
Cradle cap
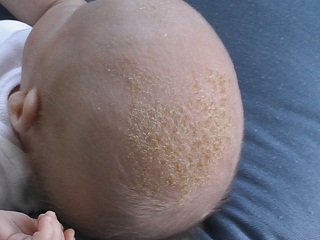
© Image via Wikimedia Commons
Cradle cap is very common and usually appears in the first few weeks of life. There are greasy, yellow scaling patches that may eventually coalesce to a thick, scaly layer. The condition is not usually itchy and the child is not distressed by it. There may be loss of small amounts of hair in the area of scalp affected. There may be some areas of redness around the plaques. It tends to be very scaly on the scalp, whereas in the flexural areas it may be more erythematous in nature4 .
Continue reading below
Differential diagnosis3 4
Back to contentsAreas of reddened skin with scales may be mistaken for atopic eczema.
If the plaques become infected, they may resemble impetigo.
Nappy rash or candidiasis in the groin and perianal areas (the rash of seborrhoeic dermatitis is usually sharply demarcated and brightly erythematous).
Psoriasis may cause confusion and can look extremely similar in babies.5 . Indeed there are some who are of the opinion that seborrhoeic dermatitis in the nappy area is in fact psoriasis.6 .
Fungal infections - eg, tinea.
Irritant or contact dermatitis.
Investigations
Back to contentsUsually no investigation is required and the diagnosis is made on clinical appearance alone.
Infant seborrhoeic dermatitis is uncommon in pre-adolescent children and tinea capitis is uncommon after adolescence. Dandruff in a child is more likely to represent a fungal infection. A fungal culture may aid the diagnosis but the disease may occur with a negative culture and a positive culture is not diagnostic.
Infant seborrhoeic dermatitis treatment3
Back to contentsReassurance - typically resolves spontaneously within a few months.
Scalp is affected ( most common presentation):
Advise massage a topical emollient onto the scalp to loosen scales, brush gently with a soft brush and wash off with shampoo.
If not effective, consider topical imidazole cream (clotrimazole 1% or miconazole 2% cream) daily for up to 4 weeks.
If symptoms persist longer than 4 weeks with treatment, seek specialist advice.
Areas other than the scalp (including the nappy area):
Advise bathing the infant every day using an emollient as a soap substitute. Avoid soaps/detergents and vigorous cleansing.
Encourage frequent nappy changes and use of barrier emollients such as Zinc and Castor Oil ointment BP, or white soft paraffin BP ointment.
Consider a topical imidazole (clotrimazole 1% or miconazole 2%) for up to 4 weeks until symptoms resolve.
If symptoms persist longer than 4 weeks with treatment, seek specialist advice.
Low potency topical corticosteroids (such as 1% hydrocortisone) may be helpful for some infants with nappy rash.
Referral3
Back to contentsConsider referral to a dermatologist/paediatrician if there is:
Severe or widespread seborrhoeic dermatitis: consider possible underlying conditions such as immunodeficiency.
Diagnostic uncertainty.
Failure to respond to routine treatment.
Complications3 7
Back to contentsSecondary infection can occur occasionally.
Leiner's disease (severe generalised seborrhoeic dermatitis - lesions become confluent and there is widespread redness and scaling). The child becomes unwell with diarrhoea, vomiting and anaemia.
Prognosis
Back to contentsThis condition usually resolves spontaneously within three to four months.8 In some it takes 6-9 months or longer. The majority of children with infant seborrhoeic dermatitis will have complete resolution and have no further skin disease. It is not known whether they have an increased risk of seborrhoeic dermatitis later in life.4
Further reading and references
- Clark GW, Pope SM, Jaboori KA; Diagnosis and treatment of seborrheic dermatitis. Am Fam Physician. 2015 Feb 1;91(3):185-90.
- Cradle cap (infantile seborrhoeic dermatitis); DermNet NZ
- Seborrhoeic dermatitis; NICE CKS, November 2024 (UK access only)
- O'Connor NR, McLaughlin MR, Ham P; Newborn skin: Part I. Common rashes. Am Fam Physician. 2008 Jan 1;77(1):47-52.
- Sampaio AL, Mameri AC, Vargas TJ, et al; Seborrheic dermatitis. An Bras Dermatol. 2011 Nov-Dec;86(6):1061-71; quiz 1072-4.
- Seborrhoeic eczema; Primary Care Dermatology Society (PCDS)
- Leiner disease; DermNet NZ
- Gary G; Optimizing treatment approaches in seborrheic dermatitis. J Clin Aesthet Dermatol. 2013 Feb;6(2):44-9.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Dec 2027
15 Dec 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free