Atopic eczema
Peer reviewed by Dr Rachel Hudson, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 26 Apr 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Eczema triggers and irritantsEmollients and eczema creamsTopical steroids for eczemaDiscoid eczemaPompholyxEczema herpeticum
Eczema is sometimes called dermatitis which means inflammation of the skin. There are different types of eczema, but most are chronic conditions. The most common type is atopic eczema.
In this type of eczema there is a typical pattern of skin inflammation which causes the symptoms. Moisturisers (emollients) and steroid creams or ointments are the common treatments. About 2 in 3 children with atopic eczema grow out of it by their mid-teens.
At a glance
Atopic eczema is a common inflammatory skin condition, often starting in early childhood.
Symptoms include dry, red, inflamed, and itchy skin, which can sometimes blister or weep.
There is no cure, but treatments can help control symptoms.
Regular use of moisturisers (emollients) is important for daily treatment.
Steroid creams and ointments are used when inflammation flares up.
See a doctor if flare-ups worsen, or if usual treatments are not working.
In this article:
Video picks for Eczema
Continue reading below
What is atopic eczema?
Atopic eczema is an inflammation of the skin, which tends to flare up from time to time. It usually starts in early childhood. The severity can range from mild to severe. There is no cure but treatment can usually control or ease symptoms.
The word atopic describes people with certain allergic tendencies. However, atopic eczema is not just a simple allergic condition. People with eczema have an increased chance of developing other atopic conditions, such as asthma and hay fever.
Are atopic dermatitis and eczema the same thing?
Generally, yes. When people say 'eczema' on its own, they usually mean 'atopic dermatitis', and vice versa.
'Eczema' can also mean chronic inflammation of the skin generally, so sometimes the term eczema is used alongside another word to describe a different condition. For example, there is discoid eczema, and venous eczema, and the condition seborrhoeic dermatitis is sometimes called 'seborrhoeic eczema'.
What is eczema?
What does atopic eczema look like?
Atopic eczema behind knees
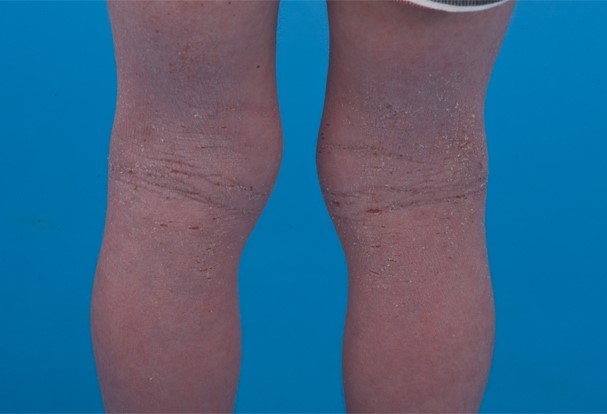
© NIAID, CC BY 2.0, via Wikimedia Commons
Atopic eczema symptoms
Back to contentsSymptoms of atopic eczema include:
Dry skin.
Red and inflamed skin. (The most commonly affected areas are next to skin creases, such as the front of the elbows and wrists, backs of knees, face and scalp and around the neck. However, any areas of skin may be affected. The face is commonly affected in babies with atopic eczema.)
Scaly patches of skin and thickened skin, caused by scratching a lot.
Blistered and weepy skin.
Typically, inflamed areas of dry skin tend to flare up from time to time and then tend to settle down. However, sometimes inflamed areas of itchy skin do become infected.
Continue reading below
How long does a flare-up last?
Back to contentsThe severity and duration of eczema flare-ups varies from person to person and from time to time in the same person.
In mild cases, a flare-up may cause just one or two small, mild patches of inflammation. Often these are behind the knees, or in front of elbows or wrists. Eczema flare-ups may occur only now and then.
In severe cases, the flare-ups can last several weeks or more and cover many areas of skin. This can cause great distress.
Many people with atopic eczema are somewhere in between these extremes.
Who gets atopic eczema?
Back to contentsMost cases first develop in young children under the age of five years. Current figures suggest about 1 in 3 children have some degree of atopic eczema. However, statistics show that it is becoming more common year on year.
By the mid-teenage years the flare-ups of eczema have either gone completely, or are much less of a problem for 2 out of 3 young people. However, there is no way of predicting who will still be affected as adults.
It is unusual to develop atopic eczema for the first time after the age of 20. About one in ten adults have eczema.
See the separate article called What causes sudden eczema in adults for more details.
Continue reading below
What causes atopic eczema?
Back to contentsWhat is the main cause of eczema?
There is no proven single cause for atopic eczema but factors which may play a part include:
Changes in climate.
Pollution.
Allergies to house dust mite or pollens.
Diet.
Infections.
Other early-life factors.
The cause is not fully understood. The oily (lipid) skin barrier tends to be reduced in people with atopic eczema. This leads to an increase in water loss and a tendency towards dry, itchy skin. Also, some cells of the immune system release chemicals under the skin surface, which can cause some inflammation.
Genetic factors
Inherited (genetic) factors play a part. Atopic eczema occurs in about 8 in 10 children where both parents have the condition and in about 6 in 10 children where one parent has the condition.
For many people, the exact genetic cause is not clear. In severe eczema, though, about half of all people have mutations in the filaggrin gene, which is important for maintaining the defensive barrier of the skin.
House dust mite allergies
Many people with atopic eczema are allergic to house dust mite.
If you have moderate or severe atopic eczema which is difficult to control with the usual treatments, you may wish to consider reducing the number of house dust mites in your home. See the separate leaflet called House Dust Mite and Pet Allergy, which gives more details on how to reduce house dust mites.
Multiple eczema triggers
There may be a combination of factors in someone who is genetically prone to eczema, which causes the drying effect of the skin and the immune system to react and cause inflammation in the skin.
Other atopic eczema triggers
Other possible factors which may trigger symptoms, or make symptoms worse, include:
Stress and habit scratching.
Pollens, moulds, and dander from pets.
Pregnancy and hormonal changes before a period in women.
However, some of these may not be avoidable.
See the separate leaflet in this series, called Eczema Triggers and Irritants, for more details.
Atopic eczema treatment
Back to contentsWhen do I need to see a doctor about eczema?
The usual treatment consists of three parts:
Avoiding irritants to the skin and other causes (triggers) wherever possible.
Moisturisers (emollients) - used every day to help prevent inflammation developing.
Steroid creams and ointments (topical steroids) - mainly used when inflammation flares up.
Avoid triggers and irritants
Many people with atopic eczema have flare-ups from time to time for no apparent reason. However, some eczema flare-ups may be triggered or made worse by irritants to the skin, or by other factors. It is commonly advised to:
Avoid soaps, bubble baths, etc, when you wash. They can dry out the skin and make it more prone to irritation. Instead, use a soap substitute plus a bath/shower moisturiser.
Biological washing powders and fabric conditioners can also sometimes cause problems.
Try as much as possible not to scratch. To help with this, keep nails short and use anti-scratch mittens in babies. If you need to relieve an itch, rub with fingers rather than scratch with nails.
Wear cotton clothes next to skin rather than irritating fabrics such as wool. However, it is probably the smoothness of the material rather than the type of the material which helps. Some smooth man-made fabrics are probably just as good as cotton.
Avoid getting too hot or too cold as extremes of temperature can irritate the skin.
After you wash clothes with detergent, rinse them well. Some biological detergents are said by some people to be irritating. But there is little proof that commonly used detergents that are used in the normal way make atopic eczema worse.
See the separate article called How to wash your hands if you have eczema or dry skin.
Avoid food allergies
About 1 in 2 children with atopic eczema have a food allergy which can make symptoms worse. In general, it is young children with severe eczema who may have a food sensitivity as a trigger factor. The most common food allergies which trigger symptoms in some people include cow's milk, eggs, soya, wheat, fish and nuts.
If you suspect a food is making your child's symptoms worse then see a doctor. You may be asked to keep a diary over 4-6 weeks. The diary aims to record any symptoms and all foods and drink taken. It may help to identify one or more suspect foods.
If food allergies are suspected, it should be confirmed by a specialist. They may recommend a diet without this food if the eczema is severe and difficult to control by other means.
Use moisturisers (emollients)
Emollients are lotions, creams, ointments and bath/shower additives which prevent the skin from becoming dry.
They oil the skin, keep it supple and moist and help to protect the skin from irritants. This helps to prevent itch and helps to prevent or to reduce the number of eczema flare-ups.
Warning: some types of moisturiser contain paraffin or other oils, which are flammable. Oils from moisturisers can sink into clothes and bedding and create a fire risk.
Be careful around naked flames (including cigarettes) when using emollients. Avoid smoking in bed.
The regular use of moisturisers is the most important part of the day-to-day treatment for atopic eczema. Your doctor, nurse or pharmacist can advise on the various types and brands available and the ones which may suit you best.
Some points about emollients include:
Thicker, greasy ointments work better and for longer than thinner creams but they are messier to use.
Apply liberally to all areas of skin. You cannot overdose or overuse emollients. They are not active medicines and do not get absorbed through the skin.
Apply emollients in the general direction of hair growth. If applied in the opposite direction the base of the hair shafts can get blocked, leading to possible infection.
Use emollients every day. A common mistake is to stop using emollients when the skin appears good. Patches of inflammation may quickly flare up again.
Various emollient preparations come as bath additives and shower gels. These may be considered in people with extensive areas of dry skin. However, there is some debate as to how well these work. If you do use them, they should be used in addition to, not instead of, creams, ointments or lotions that you rub on to the skin.
Pump dispensers are better than pots because they are less likely to harbour germs. If you need to use a pot, use a clean spoon or spatula to get the contents out, rather than your fingers.
Many people with atopic eczema use a range of different moisturisers. For example, a typical routine for a person with moderately severe atopic eczema might be:
Consider adding an emollient oil to bath water or as you shower. This will give your skin a general background oiling.
Use a thick emollient ointment as a soap substitute for cleaning. You can also rub this into particularly dry areas of skin.
After a bath or shower it is best to dry by patting with a towel rather than by rubbing. Then apply an emollient cream or ointment to any remaining dry areas of skin.
Between baths or showers, use an emollient cream, ointment or lotion as often as necessary.
A dry dressing may be helpful if your eczema is more severe, as this helps to keep the emollient from being rubbed off the skin and stops scratching. However, you should not use a dressing if a skin infection is present.
Use an emollient ointment at bedtime.
Note: emollients used for eczema tend to be bland and non-perfumed. Occasionally, some people become allergic (sensitised) to an ingredient in an emollient. This can make the skin worse rather than better.
If you suspect this, see your doctor for advice. There are many different types of emollients with various ingredients. A switch to a different type will usually sort out this uncommon problem.
Warning: bath additive emollients will coat the bath and make it greasy and slippery. It is best to use a mat and/or grab rails to reduce the risk of slipping. Warn anybody else who may use the bath that it will be slippery.
See the separate leaflet called Moisturisers for Eczema (Emollients) for more details.
Steroid creams and ointments (topical steroids)
Topical steroids work by reducing inflammation in the skin. They are grouped into four categories depending on their strength - mild, moderately potent, potent and very potent. There are various brands and types in each category.
For example, hydrocortisone cream 1% is a commonly used steroid cream and is classed as a mild topical steroid. The greater the strength (potency), the more effect it has on reducing inflammation but the greater the risk of side-effects with continued use.
Creams are usually best to treat moist or weeping areas of skin. Ointments are usually best to treat areas of skin which are dry or thickened. Lotions may be useful to treat hairy areas such as the scalp.
As a rule, a course of topical steroid is used when one or more patches of eczema flare up. You should use topical steroids until the flare-up has completely gone and then stop them. In many cases, a course of treatment for 7-14 days is enough to clear a flare-up of eczema.
In some cases, a longer course is needed. Many people with atopic eczema require a course of topical steroids every now and then to clear a flare-up. The frequency of eczema flare-ups and the number of times a course of topical steroids is needed can vary greatly from person to person.
It is common practice to use the lowest-strength topical steroid which clears the flare-up. If there is no improvement after 3-7 days, a stronger topical steroid is usually then prescribed. For severe eczema flare-ups a stronger topical steroid may be prescribed from the outset.
Sometimes two or more preparations of different strengths are used at the same time. For example, a mild steroid for the face and a stronger steroid for patches of eczema on the thicker skin of the arms or legs.
High-strength steroids
Back to contentsShort bursts of high-strength steroid as an alternative
For adults, a short course, usually three days, of a strong topical steroid may be an option to treat a mild-to-moderate flare-up of eczema. A strong topical steroid often works quicker than a mild one.
(This is in contrast to the traditional method of using the lowest strength wherever possible. However, studies have shown that using a high strength for a short period can be more convenient and is thought to be safe.)
Side-effects of topical steroids
Short courses of topical steroids (fewer than four weeks) are usually safe and normally cause no problems. Problems may develop if topical steroids are used for long periods, or if short courses of strong topical steroids are repeated often. The concern is mainly if strong topical steroids are used in the long term. Side-effects from mild topical steroids are uncommon.
Thinning of the skin has always been considered a common problem. However, recent research suggests that this mainly occurs when high-strength steroids are used under airtight dressings. In normal regular use skin thinning is unlikely and, if it does occur, it often reverses when the topical steroid is stopped.
With long-term use of topical steroid the skin may develop permanent stretch marks (striae), bruising, discolouration, or thin spidery blood vessels (telangiectasias).
Topical steroids may trigger or worsen other skin disorders such as acne, rosacea and perioral dermatitis.
Some topical steroid gets through the skin and into the bloodstream. The amount is usually small and normally causes no problems unless strong topical steroids are used regularly on large areas of the skin. The main concern is with young children who need frequent courses of strong topical steroids. The steroid can have an effect on growth. Therefore, children who need repeated courses of strong topical steroids should have their growth monitored.
Recently, there has been more awareness in the media about topical steroid withdrawal (TSW). TSW is still being studied and is poorly defined. Some people find that their skin gets worse after stopping topical steroids, or that their skin seems 'addicted' to topical steroids. There are a few possible reasons:
Some people have severe eczema which rebounds when topical steroids are reduced or stopped. If so, the problem is the eczema, not the steroids - and further, stronger, eczema treatments may be needed.
Occasionally people can develop an allergic reaction to ingredients in a particular steroid cream - meaning they have to use more and more of the steroids, as if they were 'addicted'. If this is suspected, allergy tests can look for the allergy, and different brands of steroids can be used.
Some people have reported red, painful, flaking and peeling skin that appears shortly after stopping topical steroids. This is probably 'true' TSW. It's not clear how often this happens but is probably rare. When it has happened, it's usually occurred after using strong topical steroids on thin areas of skin (eg, the face) for a long time (over a year). TSW is probably much less likely if you avoid using topical steroids for long uninterrupted courses, and avoid using strong steroids on delicate areas of skin.
For more details about side-effects see the separate leaflet called Topical Steroids for Eczema.
Short-duration treatment to prevent flare-ups (weekend therapy)
Some people have frequent flare-ups of eczema. For example, a flare-up may subside well with topical steroid therapy. But then, within a few weeks, a flare-up returns. In this situation, one option that might help is to apply steroid cream on the usual sites of flare-ups for two days every week.
This is often called weekend therapy. This aims to prevent a eczema flare-up from occurring. In the long run, it can mean that the total amount of topical steroid used is less than if each flare-up were treated as and when it occurred. You may wish to discuss this option with your doctor.
Note: don't forget you can use emollients as well when you are using a course of topical steroids. See the separate leaflet called Fingertip Units for Topical Steroids for more details.
Using moisturisers and topical steroids together
Back to contentsMost people with eczema will be prescribed emollients to use every day and a topical steroid to use when flare-ups develop. When using the two treatments, apply the emollient first. Wait 10-15 minutes after applying an emollient before applying a topical steroid.
That is, the emollient should be allowed to sink in (be absorbed) before a topical steroid is applied. The skin should be moist or slightly tacky but not slippery, when applying the steroid.
Infected eczema patches
Sometimes, one or more patches of eczema become infected during a flare-up. Characteristics of infected eczema include:
Weeping blisters.
Infected skin lumps (pustules).
Crusts.
Failure to respond to normal treatment.
Rapidly worsening eczema.
If the skin infection becomes more severe, you may also develop a high temperature (fever) and generally feel unwell. If infected eczema develops and you are unwell in yourself or feverish, then a course of an antibiotic tablet or liquid medicine will usually clear the infection.
This is used in addition to usual eczema topical treatments.
The UK's National Institute for Health and Clinical Excellence (NICE) updated its guidance on treating infected eczema in 2021. It noted that:
Weeping blisters and crusted eczema do not always mean that eczema has become infected.
There is not much evidence to suggest that treating eczema flare-ups with antibiotics makes a big difference to the outcome (most people get better without them).
Giving antibiotics, especially repeated courses, increases the risk of developing resistant bacteria (meaning that future courses of antibiotics might not work when needed).
They therefore recommend that antibiotics should be only be given if someone with an eczema flare-up is also generally unwell (eg, they have a fever). For people with an infected eczema flare who are otherwise well, they recommend avoiding antibiotics and instead using the usual eczema treatment. In some cases, doctors might recommend antibiotics anyway, if someone is at high risk of a serious complication from infected eczema.
Skin swabs usually aren't helpful in most eczema flares. They can't tell between bacteria that are causing infection, and bacteria that are simply sitting on the skin (which is normal).
There is a rare condition where eczema becomes infected with a virus called herpes simplex. This requires antiviral medication rather than antibiotics. See the separate leaflet called Eczema Herpeticum for more details.
Once the infection is cleared, it is best to throw away all your usual creams, ointments and lotions and obtain fresh new supplies. This is to reduce the risk of applying creams, etc, that may have become contaminated with germs (bacteria).
Also, if you seem to have repeated bouts of infected eczema, you may be advised to use a topical antiseptic such as chlorhexidine on a regular basis. This is in addition to your usual treatments. The aim is to keep the number of bacteria on your skin to a minimum.
What if the eczema treatment doesn't work?
Back to contentsIs eczema forever?
See your doctor if a flare-up of atopic eczema is getting worse or not clearing despite the usual treatments with moisturisers (emollients) and topical steroids. Things which may be considered include:
Whether the strength of the topical steroid should be increased.
Whether emollients are being used often enough to keep the skin supple and moist.
The need for an antibiotic if the inflamed skin has become infected.
Allergy. Occasionally, some people become allergic (sensitised) to an ingredient in a cream (such as a preservative which is included with the steroid or emollient). This can make the skin inflammation worse rather than better.
You may be referred to a skin specialist if a flare-up does not improve with the usual treatments.
Other treatments for atopic eczema
Back to contentsTacrolimus ointment and pimecrolimus cream
They work by suppressing some cells involved in causing inflammation. (They are called topical immunomodulators.) Tacrolimus ointment and pimecrolimus cream are not steroids.
They seem to work well to reduce the skin inflammation of atopic eczema. They are licensed for use in people aged 2 years and over who have atopic eczema which is not controlled very well with usual treatments. They should not be used on infected skin.
Steroid tablets
In some cases, steroid tablets are prescribed for a short time if the eczema becomes severe and topical treatments are not helping much.
Eczema soaks
Eczema with blisters may need special soaks to dry up the weepy blisters.
Hospital treatment
This is sometimes needed for severe cases. Treatments which are sometimes used include wet wraps, tar and/or steroid occlusion bandages, light therapy and immunosuppressive/immune-modifying medication.
Tar shampoos
These types of shampoo are useful to lift scale from affected scalps.
Antihistamine tablets
Antihistamine tablets do not have a great effect on reducing itch but some types of antihistamines can make you drowsy. A dose at bedtime may help young children who are troubled with itch to get to sleep.
Dilute bleach baths
Bathing with diluted bleach has been used to good effect in some children with long-term difficult-to-control eczema. The logic is that it helps to clear the skin of germs (bacteria).
Note: this should only be done under the direct supervision and advice of a doctor. Bleach can seriously harm and using the wrong dilution can be very damaging. Do not try this on your own without individual professional advice.
Alternative remedies for atopic eczema
Back to contentsAlternative remedies for eczema, such as herbal medicines, are sometimes tried by some people. However, you should be cautious about using them, especially if their labels are not in your usual language and you are not sure what they contain. Some herbal treatments are mixed with steroids and some (particularly Chinese remedies) have been linked to liver damage.
How to prevent atopic eczema in newborns
Back to contentsIt may be worth breastfeeding a newborn baby for three months or more if several members of the family suffer from allergies such as eczema, hay fever or asthma. There is, however, no evidence to suggest that the mother should avoid any particular foods during pregnancy or breastfeeding.
Complications of atopic eczema
Back to contentsEczema can lead to other problems, such as:
Infected eczema, as discussed above.
Mental health difficulties. Eczema can cause a lot of distress to people, and affect their daily lives. In both adults and children, mental health can suffer as a result of eczema symptoms, potentially leading to poor self-image, poor self-confidence, and depression. In children, eczema can lead to problems such as missing school, and being teased or bullied.
Sleep problems. Itchy eczema can stop children and adults from being able to sleep.
Allergy. People with eczema are more likely to get hay fever and asthma - two other atopic conditions. Eczema in infants seems to be linked with a higher risk of developing allergy, particularly food allergy, later on. One theory is that food particles get onto the skin, and can sink into the leaky skin of children with eczema, where the immune system learns to recognise them as allergens.
Changes in skin colour. After a patch of inflamed eczema has healed, the skin can look lighter or darker than the surrounding areas. This is called post-inflammatory hypopigmentation (if the skin is lighter) or hyperpigmentation (if it's darker). It's more common in people with black or brown skin. It can take several months to heal.
Sleep problems. Itchy eczema can stop children and adults from being able to sleep.
Allergy. People with eczema are more likely to get hay fever and asthma - two other atopic conditions. Eczema in infants seems to be linked with a higher risk of developing allergy, particularly food allergy, later on. One theory is that food particles get onto the skin, and can sink into the leaky skin of children with eczema, where the immune system learns to recognise them as allergens.
Changes in skin colour. After a patch of inflamed eczema has healed, the skin can look lighter or darker than the surrounding areas. This is called post-inflammatory hypopigmentation (if the skin is lighter) or hyperpigmentation (if it's darker). It's more common in people with black or brown skin. It can take several months to heal.
Patient picks for Eczema

Skin, nail and hair health
Eczema triggers and irritants
In atopic eczema, avoiding certain causes (triggers) and irritants may help to prevent flare-ups of symptoms.
by Dr Philippa Vincent, MRCGP

Skin, nail and hair health
Discoid eczema
Eczema (dermatitis) is a term used to describe conditions where there is inflammation of skin. There are several types of eczema. Discoid eczema is one type which causes round or oval red patches of inflamed skin. The cause is uncertain. Treatment includes regular use of emollients to moisturise your skin, steroid creams to reduce inflammation and treatment of any infection of the affected skin.
by Dr Philippa Vincent, MRCGP
Frequently asked questions
If I have atopic eczema, am I more likely to develop other conditions?
Yes, people with atopic eczema have an increased chance of developing other atopic conditions such as asthma and hay fever. In infants, eczema also seems to be linked with a higher risk of developing allergies, especially food allergies, later on.
Can food allergies worsen atopic eczema symptoms?
About 1 in 2 children with atopic eczema have a food allergy that can make their symptoms worse. This is generally seen in young children with severe eczema where food sensitivity acts as a trigger. Common food allergies include cow's milk, eggs, soya, wheat, fish, and nuts. If you suspect a food is making symptoms worse, it's advised to consult a doctor, who may suggest keeping a food diary. A specialist can confirm food allergies and recommend avoiding that food if eczema is severe and hard to control.
What is 'weekend therapy' for frequent eczema flare-ups?
Weekend therapy involves applying steroid cream to typical flare-up sites for two days every week, even when the skin appears clear. This aims to prevent flare-ups from occurring frequently. It can lead to less overall topical steroid use compared to treating each flare-up as it happens. This approach should be discussed with your doctor.
Is it true that atopic eczema can affect mental health and sleep?
Yes, eczema can cause significant distress, impacting daily life and mental well-being in both adults and children. This can lead to poor self-image, low self-confidence, and depression. In children, it might result in missed school days or bullying. Additionally, the itchiness of eczema can disrupt sleep for both children and adults.
What should I do if my eczema treatments don't seem to be working?
If an eczema flare-up is worsening or not clearing with your usual moisturisers and topical steroids, consult your doctor. They may consider increasing the strength of your topical steroid, checking if emollients are being used frequently enough, or prescribing antibiotics if the skin is infected. Occasionally, an allergy to an ingredient in a cream can worsen the inflammation, in which case a change in product may be needed. You might be referred to a skin specialist if the flare-up persists.
Are there any alternative treatments for severe eczema?
For severe cases, non-steroid treatments like tacrolimus ointment and pimecrolimus cream, which suppress inflammation, may be prescribed. Short courses of steroid tablets can be used for very severe eczema not responding to topical treatments. Severe cases might also require hospital treatment such as wet wraps, tar/steroid occlusion bandages, light therapy, or immunosuppressive medication. Dilute bleach baths are also used in some children with difficult-to-control eczema, but only under strict medical supervision.
Can my skin colour change after an eczema flare-up?
Yes, after a patch of inflamed eczema has healed, the affected skin can appear lighter or darker than the surrounding areas. This is known as post-inflammatory hypopigmentation (lighter skin) or hyperpigmentation (darker skin). It is more common in individuals with black or brown skin and can take several months for the skin colour to return to normal.
Further reading and references
- Tacrolimus and pimecrolimus for atopic eczema; NICE Technology appraisal guidance, August 2004
- Atopic eczema in children; NICE Clinical Guideline (December 2007, last updated June 2023)
- Huang JT, Abrams M, Tlougan B, et al; Treatment of Staphylococcus aureus colonization in atopic dermatitis decreases disease severity. Pediatrics. 2009 May;123(5):e808-14.
- Secondary bacterial infection of eczema and other common skin conditions: antimicrobial prescribing; NICE Guideline (March 2021)
- Abrocitinib, tralokinumab or upadacitinib for treating moderate to severe atopic dermatitis; NICE Technology appraisal guidance, August 2022
- Eczema - atopic; NICE CKS, April 2022 (UK access only)
Continue reading below
About the authorView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Rachel Hudson, MRCGP
General Practitioner and Medical Author
MBChB, MRCGP (2008), BSc (Medical Science), DFSRH, DRCOG, DCH
Dr Rachel Hudson, is an NHS GP working in the North West of England.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 24 Apr 2028
26 Apr 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.