Lichen planus
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 18 Jun 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Lichen planus article more useful, or one of our other health articles.
In this article:
Continue reading below
What is lichen planus?
Lichen planus (LP) is a pruritic, papular eruption characterised by its violaceous colour and polygonal shape, sometimes with a fine scale. It is most often found on the flexor surfaces of the upper extremities, genitalia and on the mucous membranes. The cause of lichen planus is unknown but it is most likely a T-cell-mediated immunological disease. The antigen involved remains unidentified.1
How common is lichen planus? (Epidemiology)
Back to contentsCutaneous LP has a prevalence of approximately 0.2% to 1% of adults worldwide, but oral LP is more common and reported in 1% to 4% of the population.2
It can occur at any age but is more common in middle age.
Most studies report a male:female ratio of 1:1.5.
It can be precipitated by trauma (Köbner's phenomenon).
Immunologically mediated (perhaps triggered by a virus) and can occur in families.
Associated with primary biliary cirrhosis.3and both hepatitis B and hepatitis C (these patients are twice as likely to have LP).4
Continue reading below
Symptoms of lichen planus (presentation)
Back to contentsOnset is usually acute, affecting the flexor surfaces of the wrists, forearms and legs.
The typical lesion is an intensely itchy 2-5 mm red or violet shiny flat-topped papule with white streaks ('Wickham's striae').
Lichen planus
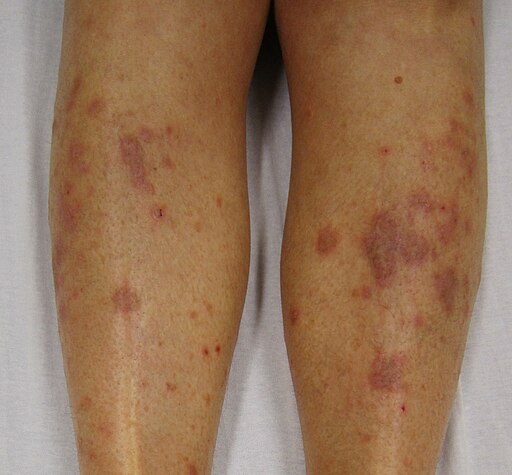
© James Heilman, MD, CC BY-SA 3.0, via Wikimedia Commons
Blisters occasionally occur.
As the papules clear they may be replaced by brown discolouration (especially in the dark-skinned). Lesions may occur on any part of the body surface but most commonly on the front of the wrists, flexor aspects of the forearms, genitals, lumbar region and ankles and shins (where lesions are most commonly hypertrophic, frequently very itchy and may ulcerate).
On the palms and soles the papules are firm and yellow.
Mucous membranes are commonly affected:
Classically, white slightly raised lesions with a trabecular, lacy appearance on the inside of the cheeks.
Oral lichen planus
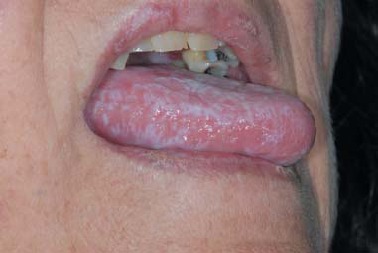
© Department of Dermatology, Mayo clinic, Rochester, Minnesota, CC BY 3.0, via Wikimedia Commons
The mucous membrane lesions are often asymptomatic but can be very painful and difficult to treat. Oral lichen planus may cause sensitivity to heat. There is also an association with mercury fillings.5
Lesions may also be found on the genitalia, anus, larynx and, very rarely, on the tympanic membrane or oesophagus (where it can present as dysphagia and cause benign strictures).
Nails are involved in up to 10% of patients: longitudinal lines and linear depressions of the nail plate, severe dystrophy and complete destruction of the nail bed may occur.
The scalp is usually spared but lichen planus affecting the scalp may cause permanent scarring alopecia.
Variations of lichen planus
As well as the classical form, the following can occur:
Hypertrophic lichen planus - this causes very itchy lesions, usually found on the extensor surfaces of the extremities, especially the ankles. They can last for a long time and leave residual scarring and pigmentation.
Atrophic lichen planus - a few lesions are present which are often resolving annular or hypertrophic lesions.
Erosive/ulcerative lichen planus - found on mucosal surfaces and develop from sites where lichen planus previously developed.
Follicular lichen planus - this is also known as lichen planopilaris. Keratotic papules are present that may merge into plaques. The condition is more common in women than in men and often involves mucous membranes and nails. A scarring alopecia sometimes develops.
Annular lichen planus - purely annular lesions are rare. Papules with an atrophic centre may develop on the male genitalia or the buccal mucosa.
Vesicular and bullous lichen planus - usually these develop from existing areas of lichen planus. The lower limbs and the mouth are the most common areas. Rarely, a combination of lichen planus and bullous pemphigoid can develop, called lichen planus pemphigoides.
Actinic lichen planus - this is seen in subtropical regions such as Africa, the Middle East and India. The typical appearance is of nummular patches with a hyperpigmented centre surrounded by a hypopigmented area. The condition is mildly itchy and often spares the nails, scalp, mucous membranes and covered areas.
Lichen planus pigmentosus - more commonly affects darker skin - eg, people from Latin America or Asia are commonly affected. It resembles another condition called erythema dyschromicum perstans (ashy dermatosis) and some authorities maintain that it is indeed the same condition. It is relatively rare.
Diagnosing lichen planus
Back to contentsLichen planus can usually be diagnosed clinically and histology is not often required. Skin biopsy is characteristic:
There is a 'saw-tooth' pattern of epidermal hyperplasia and vacuolar alteration of the basal layer of the epidermis along with an intense upper dermal band-like lymphohistiocytic infiltrate (mainly T cells).
This initially develops around blood vessels at the dermal/epidermal junction and disrupts the basal epidermal layer.
There is a reduced number of melanocytes in this region and focal areas with a thicker granular layer and infiltrate (the 'Wickham's striae').
Direct immunofluorescence shows globular deposits of IgM (occasionally IgG and IgA).
Continue reading below
Differential diagnosis
Back to contentsDrug eruption (lichenoid) - eg, thiazides, antimalarials, gold.
Cutaneous graft-versus-host-reaction.
Lichen amyloidosis.
Pleomorphic (small-cell) T-cell lymphoma.
Management of lichen planus67
Back to contentsTreatment is not always needed. Skin lichen planus may resolve spontaneously within a year, although mucous membrane lichen planus may be more persistent and resistant to treatment.
If drugs are suspected as the cause, they should be stopped.
Symptomatic treatment for itching - eg, moderately potent topical steroids (intralesional steroid injections may be beneficial for patients with severe and persistent itch) and sedating antihistamines.
Local treatments for the symptomatic cutaneous or mucosal disease include:
Potent topical corticosteroids (including steroid impregnated tape).
Topical calcineurin inhibitors, tacrolimus ointment, and pimecrolimus cream.
Topical retinoids.
Intralesional steroid injections.
Systemic treatment for widespread lichen planus or severe local disease often includes a 1- to 3-month course of systemic steroids (eg, prednisolone), along with another therapy, which may be one of the following:
Acitretin.
Hydroxychloroquine.
Methotrexate.
Azathioprine.
Mycophenolate mofetil.
Phototherapy. In actinic lichen planus, phototherapy should be avoided because lesions are typically triggered by sun exposure. Sun protection, including use of sunscreen, is an essential component of treatment.
Anecdotal success is reported from long courses of antibiotics eg, metronidazole, sulfasalazine, antifungals (such as griseofulvin), and JAK inhibitors.
Psoralen combined with ultraviolet A (PUVA) radiation treatment has been used to reduce pruritus and help to clear the lichen planus.89
Complications of lichen planus
Back to contentsPeople with oral lichen planus have a 1.1% risk of developing oral squamous cell carcinoma (OSCC); therefore, regular follow-up for these patients is recommended.10 A higher rate of transformation is found among smokers, people with alcohol dependency, and HCV-infected patients.
Rarely, carcinoma may develop in association with vulval lesions in women.11
Hypertrophic lesions may leave residual hyperpigmentation.
Prognosis
Back to contentsSpontaneous resolution of cutaneous lesions usually occurs over 12-24 months but hypertrophic lesions can last longer.2
Oral lesions usually have a chronic and progressive course and may never completely resolve.
The degree of pruritus tends to decrease with time.
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Sanatkhani M, Mosannen Mozafari P, Amirchaghmaghi M, et al; Effect of cedar honey in the treatment of oral lichen planus. Iran J Otorhinolaryngol. 2014 Jul;26(76):151-61.
- Arora SK, Chhabra S, Saikia UN, et al; Lichen planus: a clinical and immuno-histological analysis. Indian J Dermatol. 2014 May;59(3):257-61. doi: 10.4103/0019-5154.131389.
- Gorouhi F, Davari P, Fazel N; Cutaneous and mucosal lichen planus: a comprehensive review of clinical subtypes, risk factors, diagnosis, and prognosis. ScientificWorldJournal. 2014 Jan 30;2014:742826. doi: 10.1155/2014/742826. eCollection 2014.
- Arnold DL, Krishnamurthy K; Lichen Planus. StatPearls Publishing; Jan 2024.
- Nagao Y, Sata M; Disappearance of Oral Lichen Planus After Liver Transplantation for Primary Biliary Cirrhosis and Immunosuppressive Therapy in a 63-year-Old Japanese Woman. Hepat Mon. 2014 Mar 11;14(3):e16310. doi: 10.5812/hepatmon.16310. eCollection 2014 Mar.
- Nosratzehi T; Oral Lichen Planus: an Overview of Potential Risk Factors, Biomarkers and Treatments Asian Pac J Cancer Prev. 2018 May 26;19(5):1161-1167. doi: 10.22034/APJCP.2018.19.5.1161.
- McParland H, Warnakulasuriya S; Oral lichenoid contact lesions to mercury and dental amalgam--a review. J Biomed Biotechnol. 2012;2012:589569. doi: 10.1155/2012/589569. Epub 2012 Jul 24.
- Lichen Planus; Primary Care Dermatology Society (PCDS)
- Lichen Planus; DermNet.
- Alsenaid A, Alamri A, Prinz JC, et al; Lichen planus of the lower limbs: successful treatment with psoralen cream plus ultraviolet A photochemotherapy. Dermatol Ther. 2016 Mar-Apr;29(2):109-13. doi: 10.1111/dth.12321. Epub 2015 Dec 2.
- Atzmony L, Reiter O, Hodak E, et al; Treatments for Cutaneous Lichen Planus: A Systematic Review and Meta-Analysis. Am J Clin Dermatol. 2016 Feb;17(1):11-22. doi: 10.1007/s40257-015-0160-6.
- Aghbari SMH, Abushouk AI, Attia A, et al; Malignant transformation of oral lichen planus and oral lichenoid lesions: A meta-analysis of 20095 patient data. Oral Oncol. 2017 May;68:92-102. doi: 10.1016/j.oraloncology.2017.03.012. Epub 2017 Apr 5.
- Tjalma WA, Siozopoulou V, Huizing MT; A clitoral verrucous carcinoma in an area of lichen planus has aggressive features. World J Surg Oncol. 2017 Jan 6;15(1):7. doi: 10.1186/s12957-016-1069-0.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 17 Jun 2027
18 Jun 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free