Nail disorders and abnormalities
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 17 Aug 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Nail disorders and abnormalities are common. Appearances may be difficult to diagnose with certainty. Care must be taken to ensure correct diagnosis and therefore treatment.
Continue reading below
Abnormal-looking nails1 2
The following are common nail abnormalities, with possible causes.
Beau's lines
Transverse ridges are usually transient and due to a temporary disturbance of nail growth - eg, severe illness, trauma or infection. Beau's lines occur in ALL nails, due a general cause preventing nail growth.
Other causes of transverse ridges include:
Psoriasis.
Paronychia.
Eczema.
Longitudinal ridging
Causes include lichen planus, rheumatoid arthritis, myxoid cysts and peripheral arterial disease.
Pitted nails
Causes include alopecia areata, psoriasis and eczema.
Clubbing
An increase in the soft tissue of the distal part of the fingers or toes; common causes of finger clubbing include:
Cyanotic congenital heart disease, infective endocarditis.
Lung cancer, pulmonary fibrosis, cystic fibrosis, bronchiectasis, empyema, lung abscess.
Finger clubbing
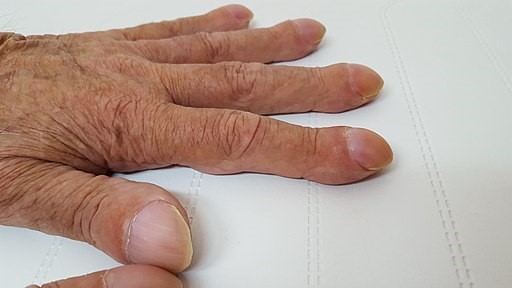
© Wesalius, CC BY-SA 4.0, via Wikimedia Commons
Koilonychia
Dystrophy of the fingernails in which they are thinned and concave with raised edges (spoon-shaped nails).
May be due to iron deficiency or to trauma.
Koilonychia - iron deficiency
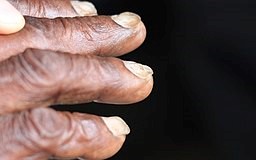
© CHeitz, CC BY 2.0, via Wikimedia Commons
Nail-patella syndrome
A congenital nail disorder, autosomal dominant inheritance.
The patellae and some of the nails are rudimentary or absent.
Green nails
These may be caused by pseudomonal infection, which results in green-blue or black discolouration.
Blue nails
May occur as a side-effect of certain medications, such as minocycline, hydroxyurea or mepacrine.
Black nails
These may be a feature of Peutz-Jeghers syndrome, vitamin B12 deficiency, pseudomonas infection and post-irradiation.
Black streaks may indicate a junctional melanocytic naevus or malignant melanoma.
Purple/black discolouration occurs with a subungual haematoma. This should gradually grow distally and there is often (although not always) a history of trauma.
Leukonychia (white nail)
This may be congenital or due to minor trauma, hypoalbuminaemia in chronic liver disease, chronic kidney disease, Beau's lines (which may be white), fungal infection or lymphoma.
Yellow nail syndrome
Yellow nail syndrome is characterised by slow-growing, excessively curved and thickened yellow nails which are associated with peripheral lymphoedema and exudative pleural effusions.
Yellow or yellow/white nails without thickening or onycholysis
Causes include:
Nicotine staining from smoking (brown/yellow).
Trauma, particularly from poorly fitting footwear in active individuals, and particularly affecting the big toenail.
Dermatophyte or fungal infection.
Psoriasis.
Paronychia.
Medication including tetracyclines, captopril, trimethoprim, indometacin and isoniazid.
Ingrowing toenail3
Back to contentsIngrown toenail
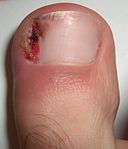
© ExistentialExplosion at English Wikipedia, CC0, via Wikimedia Commons
A common problem resulting from various causes - eg, improperly trimmed nails, trauma, poorly fitting shoes, abnormally shaped nails or pressure from other digits.
Also called onychocryptosis.
It often presents with pain but may progress to infection and difficulty with walking.
Treatment options include cutting nails square, hot water soaks, cotton wool inserts at the nail edges, antibiotics or excision and wedge excision or total excision of nail. A Cochrane review found that surgical treatments were more effective than non-surgical treatments.4
Continue reading below
Onycholysis5 6 7
Back to contentsThe nail becomes detached from its bed at the base and side, creating a space under the nail that accumulates dirt. Air under the nail may cause a grey-white colour but can vary from yellow to brown.
In psoriasis there may be a yellowish-brown margin between the margin between the normal nail (pink) and the detached parts (white).
If Pseudomonas aeruginosa grows underneath the nail then there may be a green colour.
When nail bed separation begins in the middle of the nail then appearance resembles an 'oil spot' or 'salmon patch'.
Causes of onycholysis include:
Idiopathic or inherited.
Systemic disease - eg, thyrotoxicosis.
Skin disease - eg, psoriasis.
Infection - eg, candida, dermatophytes, pseudomonas, herpes simplex.
Local causes - eg, trauma or chemicals.
Treatment involves treating or eliminating the cause. Once this is done, nails should gradually grow back normally. Meanwhile nails should be kept short and dry, and irritants and trauma avoided.
Onychogryphosis8
Back to contentsThickening and hardening of the nail plate, which becomes curved
Also called ram's horn nails
Mainly seen on big toes of the elderly, associated with injury to the foot, badly fitting shoes or poor blood supply.
Continue reading below
Median nail dystrophy1 9
Back to contentsAlso called median canaliform dystrophy of Heller.
Small cracks in the centre of the nail extend laterally in the shape of the branches of a fir tree.
Also, the cuticle is pushed back and inflamed.
It usually affects one nail, and improves over time. The thumb is commonly involved.
Most commonly it results from the compulsive habit of a patient picking at a proximal nail fold thumb with an index fingernail.
It disappears if the patient stops the habit.
Splinter haemorrhages1
Back to contentsSplinter haemorrhages are linear haemorrhages lying parallel to the long axis of fingernails or toenails.
They are red or brown/black.
Splinter haemorrhage
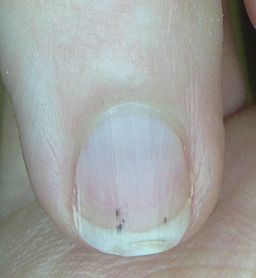
© Splarka, Public domain, via Wikimedia Commons
Causes include:
Trauma (the most common cause).
Infective endocarditis.
Vasculitis - eg, rheumatoid arthritis, systemic lupus erythematosus, polyarteritis nodosa.
Haematological malignancy.
Severe anaemia.
Psoriasis.
Psoriasis
Back to contentsSee also the separate Psoriatic Nail Disease article.
Virtually all patients with psoriasis have nail involvement at some time and it occurs in 50% of cases at any given time.10
Abnormalities include nail pits, transverse furrows, crumbling nail plate, roughened nails.
Nail psoriasis
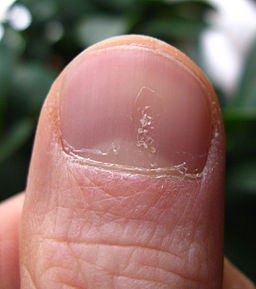
© Seenms, CC BY-SA 3.0, via Wikimedia Commons
Nail pitting is associated with alopecia areata as well as with psoriasis. It can sometimes be seen in nail bed 'oil spot', distal onycholysis, distal subungual hyperkeratosis, splinter haemorrhages and false nail following spontaneous separation of nail plate.
Lichen planus11
Back to contentsSee also separate Lichen Planus article.
Nails are involved in approximately 10% of cases of disseminated lichen planus. However, it may be the only presentation of this disease.
Within the matrix it causes thinning, brittleness, and crumbling of the nail with accentuated surface longitudinal ridging and colour change to black or white.
Typically the lunula is raised more than the distal part of the nail.
Severe chronic inflammation causes either partial or complete loss of nail plate and formation of pterygium with partial loss of central nail plate seen as distal notch or completely split nail. Involvement of the nail bed causes onycholysis, distal subungual hyperkeratosis, formation of bulla or permanent anonychia.
Lichen planus can affect any number of nails.
Refer early, as timely treatment can prevent destructive permanent nail damage.1
Treatment:
Nail tumours
Back to contentsSquamous cell carcinoma (SCC)14 15 16
The most common malignant tumour of the nail unit.
An association with human papillomavirus (mainly types 16 and 18) has been reported.
Skin-coloured or hyperpigmented lesions appearing as keratotic or hyperkeratotic or warty papules and plaques found on the proximal and lateral nail folds and hyponychium.
Subungual lesions may be missed and the diagnosis delayed due to similar presentations to other, benign nail disorders.
SCC in situ (SCCIS) can extend into the nail bed, producing onycholysis.
Invasive SCC arising within SCCIS can cause pain if it invades bone.
Occurs much more commonly on fingers than toes, usually the thumb and index finger, usually as a solitary lesion.
Can involve multiple fingers in immunocompromised patients.
Refer urgently to secondary care where SCC is suspected.
Treat with CO2 laser ablation, Mohs' surgery or amputation of the digit if necessary.
Successful use of electronic brachytherapy has been reported.17
Melanoma1 18
Melanoma of the nail unit accounts for around 1% of melanoma in white-skinned people. It is not thought to be due to sun exposure. It is most common between the ages of 40 and 70 years.
Types include:
Acral lentiginous melanoma
Nodular melanoma
Desmoplastic melanoma
Presentation:
Often presents as a longitudinal line the length of the nail. This may be brown, black or red, then becomes wider and more irregular. It may then extend and start to disrupt the nail. (There are other benign causes of longitudinal lines.)
In some cases there is no pigmentation.
In some cases a nodule forms, lifting the nail (onycholysis).
Hutchinson's sign is pigment involving the nail fold (skin to the side of the nail) and is suspicious of melanoma.
Thumb melanoma
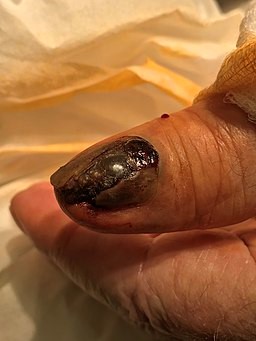
© Wawjak, CC BY 4.0, via Wikimedia Commons
Diagnosis is by biopsy and treatment is by surgical removal. Amputation may be required.
Benign tumours
Pyogenic granuloma - a rapidly growing papule which bleeds easily.
Myxoid cyst - found around the proximal nail fold. There is a smooth shiny surface. Pressure from the cyst may cause a lateral groove in the nail.
Glomus tumour - benign vascular tumour.
Fungal nail infections - onychomycosis
Back to contentsSee the separate Fungal Nail Infections article.
Paronychia19
Back to contentsParonychia (also known as whitlow) describes localised inflammation of the tissue around a nail. There may be accumulation of pus between the skin and the nail matrix. The area may become swollen, red and tender. If it lasts longer than six weeks, it is termed chronic paronychia.
Toenail paronychia green discolouration
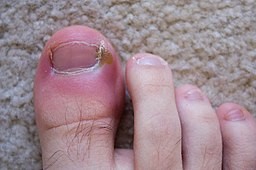
© X-Fi6, CC0, via Wikimedia Commons
Acute paronychia
Erythema, swelling and throbbing pain in the nail fold caused by bacterial infection, most commonly Staphylococcus aureus.
Common causes include excessive manicuring, finger biting, trauma, splinters, skin conditions such as eczema or contact dermatitis, ingrowing nails.
Treatment options include antibiotics or incision and drainage.
Chronic paronychia20
Chronic paronychia commonly occurs in patients with skin conditions affecting the hands, or whose hands are constantly in water with repeated minor trauma damaging the cuticle so that irritants can further damage the nail fold. People whose occupations predispose to chronic paronychia include fishermen, cleaners, housewives, dairy farmers, and bartenders.
Proximal and lateral nail folds show erythema and oedema with loss of cuticle and part of the proximal nail fold separating from the nail plate.
Commonly it becomes infected, especially with Candida albicans or pseudomonas. Eventually the nail fold retracts and becomes thickened and rounded.
There are episodes of painful acute inflammation often due to infection between the proximal nail fold and nail plate from which pus may drain.
Over time, lateral edges of the nail plate become irregular and discoloured and eventually the entire nail plate becomes involved showing numerous transverse grooves.
Removing the source of the irritation is the most important aspect of treatment. Hands should be kept dry and warm.
Topical steroids appear to be better than topical or oral antifungals. A number of surgical options are used where medical management fails. There is a newer surgical treatment called the Swiss roll technique (the nail fold is elevated and reflected proximally over a non-adherent dressing).
Further reading and references
- Becker C, Bershow A; Lasers and photodynamic therapy in the treatment of onychomycosis: a review of the literature. Dermatol Online J. 2013 Sep 14;19(9):19611.
- Dias MF, Bernardes-Filho F, Quaresma-Santos MV, et al; Treatment of superficial mycoses: review. Part II. An Bras Dermatol. 2013 Nov-Dec;88(6):937-44. doi: 10.1590/abd1806-4841.20132018.
- Nail disorders; Primary Care Dermatology Society (PCDS)
- Nail Disorders; Skin Dermatologists
- Bryant A, Knox A; Ingrown toenails: the role of the GP. Aust Fam Physician. 2015 Mar;44(3):102-5.
- Eekhof JA, Van Wijk B, Knuistingh Neven A, et al; Interventions for ingrowing toenails. Cochrane Database Syst Rev. 2012 Apr 18;(4):CD001541. doi: 10.1002/14651858.CD001541.pub3.
- Jadhav VM, Mahajan PM, Mhaske CB; Nail pitting and onycholysis. Indian J Dermatol Venereol Leprol. 2009 Nov-Dec;75(6):631-3. doi: 10.4103/0378-6323.57740.
- Onchyolysis; DermNet NZ
- Zaias N, Escovar SX, Zaiac MN; Finger and toenail onycholysis. J Eur Acad Dermatol Venereol. 2015 May;29(5):848-53. doi: 10.1111/jdv.12862. Epub 2014 Dec 16.
- McDermott R et al; Case Report, International Journal of Case Reports and Images, Vol. 3 No. 1, January 2012
- Kota R, Pilani A, Nair PA; Median Nail Dystrophy Involving the Thumb Nail. Indian J Dermatol. 2016 Jan-Feb;61(1):120. doi: 10.4103/0019-5154.174092.
- Psoriasis: The assessment and management of psoriasis; NICE Clinical Guideline (October 2012 - last updated September 2017)
- Nakamura R, Broce AA, Palencia DP, et al; Dermatoscopy of nail lichen planus. Int J Dermatol. 2013 Jun;52(6):684-7. doi: 10.1111/j.1365-4632.2011.05283.x. Epub 2013 Feb 22.
- Irla N, Schneiter T, Haneke E, et al; Nail Lichen Planus: Successful Treatment with Etanercept. Case Rep Dermatol. 2010 Oct 21;2(3):173-176.
- Gomez Vazquez M, Navarra Amayuelas R; Marked improvement in nail psoriasis during treatment with etanercept. Dermatol Ther. 2011 Sep-Oct;24(5):498-500. doi: 10.1111/j.1529-8019.2012.01472.x.
- Dika E, Fanti PA, Patrizi A, et al; Mohs Surgery for Squamous Cell Carcinoma of the Nail Unit: 10 Years of Experience. Dermatol Surg. 2015 Sep;41(9):1015-9. doi: 10.1097/DSS.0000000000000452.
- Patel PP, Hoppe IC, Bell WR, et al; Perils of diagnosis and detection of subungual squamous cell carcinoma. Ann Dermatol. 2011 Dec;23(Suppl 3):S285-7. doi: 10.5021/ad.2011.23.S3.S285. Epub 2011 Dec 27.
- Nicholls A, Jacoby J, Hartley R, et al; Squamous cell carcinoma of the nail bed. BMJ. 2015 Sep 2;351:h4640. doi: 10.1136/bmj.h4640.
- Arterbery VE, Watson AC; An electronic brachytherapy technique for treating squamous cell carcinoma in situ of the digit: a case report. BMC Res Notes. 2013 Apr 15;6(1):147.
- Melanoma of the nail unit; DermNet NZ
- Paronychia - acute; NICE CKS, December 2023 (UK access only)
- Relhan V, Goel K, Bansal S, et al; Management of Chronic Paronychia. Indian J Dermatol. 2014 Jan;59(1):15-20.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 16 Aug 2027
17 Aug 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free