Fungal nail infections
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 26 Nov 2021
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Fungal nail infection article more useful, or one of our other health articles.
In this article:
Synonyms: onychomycosis, tinea unguium
Continue reading below
What are fungal nail infections?
Different fungal organisms may infect the nails, with different patterns of presentation, affecting any part of the nail from the nail bed to the nail matrix and plate. The most common result is a poor cosmetic appearance of the affected nail(s); however, the condition may also cause pain, disfigurement and functional impairment.
Whilst not life-threatening, quality of life may be impaired through psychological distress caused by the appearance of the nails and localised pain. 1
How common are fungal nail infections? (Epidemiology)
Back to contentsThis is one of the most frequently diagnosed dermatological conditions. Global prevalence is around 5.5%. 2 UK prevalence studies report a range of 3-8% in the UK which is similar to that in the United States. 3
The incidence of new cases of onychomycosis (OM) appears to be rising due to the increasing prevalence of diabetes in the population, more frequent incidence of immunosuppression and an ageing population.4
Risk factors for fungal nail infections321
Age - adults are ~30 times more likely than children to suffer the condition and it increases in incidence with age.2
Immunosuppression - illness or medications that suppress immune responses greatly increase the likelihood of developing fungal nail infections.
Diabetes mellitus - one study found that clinical onychomycosis was found in 162 of 321 patients with type 2 diabetes mellitus.5
Cutaneous fungal infection (tinea pedis).
Living in a warm, humid climate.
Obesity.
Prior trauma to the nail.
Family history of fungal nail infections.
Continue reading below
Infecting organisms6 7
Back to contentsDermatophytes
Trichophyton rubrum or Trichophyton mentagrophytes causes between 50 and 70% of fungal nail infections.38
Other organisms in this group include Epidermophyton spp. and Microsporum spp.
Yeasts
Yeasts are increasingly found in nail samples where onychomycosis is suspected. This could be due to Candida onychomycosis but it is also thought possible that the yeasts are secondary colonisers and do not cause disease. Candida cultured from toenails is often found in asymptomatic nails whereas onychomycosis is more likely if yeasts are found on fingernail material.8
Non-dermatophyte moulds
These cause about 10% of total infections globally and are increasing in incidence. They are much more common in tropical and subtropical regions, with over 50% of fungal nail infections in Iran being found to be due to non-dermatophyte moulds.8
Clinical appearance does not correlate with the causative organism; thus, differentiation should be based entirely on microbiological evidence.
Fungal nail infection symptoms
Back to contentsThe toenails are affected much more frequently than fingernails.39
Toe onychomycosis
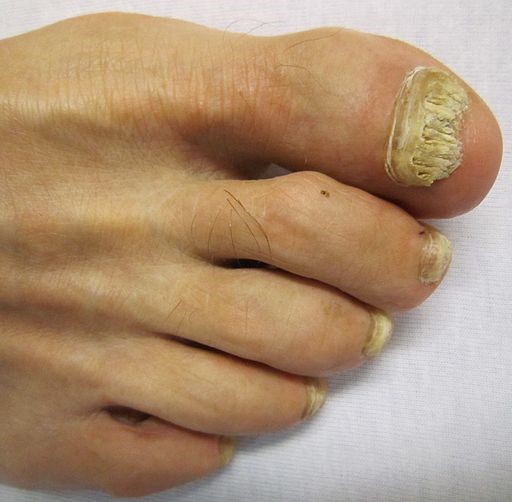
© James Heilman, MD, CC BY-SA 3.0, via Wikimedia Commons
Distal lateral subungual onychomycosis (DLSO) 3
DLSO form the vast majority of cases of fungal nail infections.
Nearly always caused by dermatophytes.
Can either affect a healthy nail or one already diseased - eg, by psoriasis.
Affects the hyponychium (epithelium of nail bed), often at the lateral edges initially.
Spreads proximally along the nail bed, causing creamy/buff discolouration, subungual hyperkeratosis and onycholysis.
The nail plate is not affected initially but may become so in time.
May be confined to one side of the nail or spread sideways to involve the whole nail bed.
Relentless progression until it reaches the posterior nail fold. Progression can occur within weeks or more slowly over months or years with the nail becoming opaque, thickened and cracked, friable and raised from the nail bed.
The nail plate becomes friable and may disintegrate, particularly after trauma.
Surrounding skin is nearly always affected by tinea pedis.
Approximately 80% of cases occur on the feet, especially on big toes, often affecting both toenails and fingernails. Fingernail DLSO has a similar appearance although nail thickening is less common; toenail infection usually precedes it.
Superficial white onychomycosis (SWO)3
SWO is less common than DLSO.
It is usually due to dermatophyte infection with T. mentagrophytes.
It presents as white chalky plaque on the proximal nail plate, almost exclusively on the toenails.
The surface of the nail plate is affected rather than the nail bed. The nail plate may become eroded and even lost.
There is white rather than creamy discolouration.
There is a notably flaky surface on the nail plate.
Onycholysis is not usually a feature.
Concurrent tinea pedis is less common than in DLSO.
Proximal subungual onychomycosis (PSO)3
PSO is uncommon but is more common in patients with AIDS.
Causes chronic paronychia with secondary nail dystrophy.
May affect the distal nail alone without paronychial involvement (usually in cases of Raynaud's phenomenon or peripheral arterial disease).
Usually affects fingernails without toenail involvement in those whose occupations cause them constantly to have wet or allergen-irritated hands.
Cuticular detachment and signs of infection and inflammation in the nail matrix may be observed.
May complicate CMC or as a secondary infection due to other causes of nail disease - eg, psoriasis.
Total dystrophic onychomycosis (TDO)3
Represents a long-standing, severe, end-stage disease progressing from any fungal nail infection.
It can take 10-15 years to develop.
Complete destruction of the nail plate is observed.
Microbiological confirmation of the diagnosis is necessary before starting antifungal therapy, as it is relatively toxic and needs to be administered for long periods.
Continue reading below
Differential diagnosis3
Back to contentsOnly about 50% of discoloured or dystrophic-appearing nails have a fungal infection confirmed with dermatophyte on culture. Other causes include:
Onychogryphosis (thickening and distortion of the nail, typically of the big toe, thought to be due to previous nail bed trauma).
Trauma (tight shoes, nail biting).
Poor foot care.
Eczema (irritant or allergic contact dermatitis).
Subungual melanoma.
Bacterial paronychia - eg, Pseudomonas spp. infection.
Systemic disease - eg, thyroid disease, diabetes, peripheral arterial disease.
Rare systemic disorders - eg, keratosis follicularis (Darier's disease), yellow nail syndrome, nail-patella syndrome, pachyonychia congenita.
Idiosyncratic drug reaction (especially tetracyclines, quinolones and psoralens).
Yellow nail syndrome.
Diagnosing fungal nail infections (investigations)10
Back to contentsTesting for fungal infection is not needed if treatment would not be given. However tests should always be done if treatment is requested. Treating without confirmed fungal nail infection is not advised.
Nail material should be sent for microscopy. There is a high false negative rate (30-40%) and even positive results should be interpreted with caution, as fungal organisms may exist as saprophytes, rather than as an invasive infection.
Culture of nail material should also be undertaken, as this increases sensitivity and will determine species but may take a few weeks.
Nail histology is not usually necessary unless there is reason to suspect another cause of nail pathology, such as psoriasis.6
Polymerase chain reaction is an effective method of detecting dermatophytes but is not used in routine practice.
Interpretation of results11
Microscopy results take a few days but culture results may take 4-6 weeks. The results are regarded as positive:
For dermatophytes, if either microscopy or culture is positive.
For Candida spp., if both microscopy and culture are positive.
For non-dermatophytes, if both microscopy and culture are positive on at least two samples taken at different times. Non-dermatophyte moulds are less common causes of nail infection (usually secondary infection following trauma or an underlying dermatophyte infection).
Increasing microbiological yield
Subungual material from the most proximal part of the infection will give the highest yield, as this is where the maximal concentration of hyphae is found.
In DLSO, encourage the patient to use a scraper to obtain a specimen from below the nail plate.
In onycholytic nails, the nails should be cut as short as possible and samples taken from below the nail.
Encourage the patient to send as much material to the lab as possible.
Associated diseases118
Back to contentsAny cause of immunocompromise.
Tinea pedis that has often been present for years.
Psoriasis.
Nail trauma.
Hereditary predisposition.
Fungal nail infection treatment and management1210
Back to contentsTo treat or not to treat?
There is no need to treat if the person is not worried about the appearance, or there are no symptoms and no comorbidities which could increase the risk of complications.
Patients should be given the information to make an informed decision based on:
Even after successful treatment of the fungal infection, the nail may not look completely normal.3
Cure is not achieved in 20-40% of patients.
Even in those in whom it is successful, nails may appear abnormal for over 12 months due to their slow growth.
Relapse occurs in about 20-25% of people.8
Oral medication is taken for six weeks for fingernail infections and for three months for toenail infections.
Topical treatments may need to be applied for up to 12 months.
All medication has potential side-effects.
If the condition progresses, it can cause significant morbidity and functional disturbance, particularly in the elderly.
Cosmetic treatment
Referral to a chiropodist may be helpful.
Nail filing and nail polish can lessen cosmetic effects.
It is helpful to trim dystrophic nails.
Medical treatment
Self-care management1113
Nails should be trimmed short.
Looser footwear should be worn, without high heels or narrow toes. Old footwear, which could be contaminated, should be considered for replacement.
Shoes should not be shared and it is best to avoid sandals or going barefoot in public places.
Cotton, absorbent socks should be worn.
Good foot hygiene is important.
Protective footwear should be worn in communal areas - eg, changing rooms, and gyms - to avoid re-exposure.
Prolonged or frequent exposure to warm, damp conditions should be avoided if possible.
Trauma to the nails should be avoided if possible.
Topical therapy11
Topical therapy can be bought over the counter.
More recent topical therapies have significantly better efficacy than in the past. Topical terbinafine has a 76% cure rate whilst itraconazole pulse dosing has a 63% cure rate, and fluconazole 48%.3However, guidelines advise that topical treatment should only be used where there is very minor disease or where oral treatments are contra-indicated.
Treatment should be given daily for 6 months for fingernails and 9-12 months for toenails .
Systemic therapy1011
Systemic treatment is recommended if topical treatment fails or is contra-indicated. The slow growth of nails means that they do not appear normal even after effective treatment so it remains important to confirm ongoing fungal nail infection.
If dermatophyte nail infection is confirmed
Terbinafine:
Currently first-line with evidence of greater efficacy compared to itraconazole.
Prescribe 250 mg once a day for between six weeks for fingernails, and for three to six months for toenails.
Advise the person that visible improvement may be seen after the end of two months of fingernail treatment and three months of toenail treatment.
It is not licensed for use in children.
There have been cases of severe idiosyncratic skin and hepatotoxic reactions.
Terbinafine should not be prescribed to anyone with hepatic impairment. LFTs should be checked before treating and some guidelines advise repeating LFTs after 4-6 weeks.
Terbinafine should not be prescribed to anyone with severe renal impairment. Caution should be used with more moderate renal impairment, as well as with psoriasis or auto-immune disease.
It interacts with rifampicin and cimetidine.
Itraconazole:
Should be offered if an alternative to terbinafine is indicated.
Highly active against Candida spp. but much less so against dermatophytes.
It can be given in a pulsed rather than continuous regimen. 200 mg twice a day for one week, with subsequent courses repeated after a further 21 days.
Prescribe two pulses for fingernails and three pulses for toenails.
It can cause hepatotoxicity and LFTs should be checked for treatment lasting longer than a month.
It is contra-indicated in pregnancy and not licensed for use in children.
It interacts with a wide variety of commonly used pharmaceutical agents, including warfarin, antihistamines, antipsychotics, digoxin, H2-receptor antagonists, some statins, and phenytoin.
Griseofulvin is no longer recommended as a treatment for fungal nail infections.
Side-effects
Side-effects of systemic antifungals include headache, itching, loss of sensation of taste, gastrointestinal symptoms, rash, fatigue, abnormal liver function, urticaria, and Stevens-Johnson syndrome along with others. 1415
There are very few recent studies looking at the safety of antifungal treatments. A meta-analysis in 2007 suggested that the risk of having asymptomatic serum transaminase elevation which did not require treatment discontinuation was less than 2.0% for all treatment regimens. The risk of an adverse liver reaction requiring treatment to be stopped ranged from 0.1% (continuous itraconazole) to 1.2% (continuous fluconazole). 16
Recent studies also confirm that the risks are low but not zero. 17
If candidal or non-dermatophyte nail infection is confirmed
Use itraconazole first-line and terbinafine second-line.
Treatment failure
Manage any comorbidities which may be hampering the effectiveness of treatment.
Consider re-investigating the cause.
Consider referral to a podiatrist if available in your area or to a dermatologist.
Refer to a paediatric dermatologist in a child as fungal nail infections are significantly less common in children.
Surgery
Keratolysis with 40% urea preparations under occlusion has become the accepted method of atraumatic nail removal. However, even surgical treatment is ineffective without anti-fungal treatment. It is unlikely that surgical management will be available on the NHS.
Refer where:
Diagnostic uncertainty remains.
There is no response to medical treatment.
Children are concerned - it is a rarer condition in children compared to adults and there are more limited treatment options.
There is suspected immune deficiency - eg, mucocutaneous candidiasis.
There is extensive disease.
There are recurring candidal nail infections.
Complications of fungal nail infections
Back to contentsPoor cosmetic appearance of hands/feet.
Disfigurement and total destruction of the nail plate.
Paronychia.
Damage to diabetic feet.
Cellulitis, osteomyelitis, sepsis, and necrosis in elderly patients and people with diabetes.
Psychosocial problems due to embarrassment at cosmetic appearance.
Pain and limitation of function, particularly in older patients.
Prognosis
Back to contentsThe prognosis is variable and depends on the type of infection as well as host factors such as comorbidities and age. Meta-analyses report mycotic cure rates of 76% for terbinafine, 63% for itraconazole with pulse dosing, 59% for itraconazole with continuous dosing and 48% for fluconazole.18
Important information |
|---|
There is often a discrepancy in clinical and microbiological cure rates in clinical trials.19 Cure, as defined by successful eradication of fungus on microscopy and culture, will not always result in a normal appearance of the affected nail due to: - Delay of 6-12 months as the damaged nail grows out. - The nail possibly having been dystrophic to begin with, predisposing it to fungal infection. |
Fingernail infections usually have much higher cure rates, in the region of 70%.
Untreated, fungal nail disease is usually progressive, leading to gradual destruction of the nail plate.
Fungal nail infection prevention
Back to contentsSecondary prevention with topical terbinafine cream after cure with systemic terbinafine appears to be effective in reducing relapse rates,20 but it is not recommended as standard management.
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Diagnosis of Onychomycosis: From Conventional Techniques and Dermoscopy to Artificial Intelligence; S S Lim et al; Frontiers in Medicine
- Onychomycosis: Clinical overview and diagnosis; S R Lipner and R K Scher; Journal of the American Academy of Dermatology
- Bodman MA, Syed HA, Krishnamurthy K; Onychomycosis.
- Rosen T, Friedlander SF, Kircik L, et al; Onychomycosis: epidemiology, diagnosis, and treatment in a changing landscape. J Drugs Dermatol. 2015 Mar;14(3):223-33.
- Gulcan A et al; Prevalence of toenail onychomycosis in patients with type 2 diabetes mellitus and evaluation of risk factors. J Am Podiatr Med Assoc. 2011 Jan-Feb;101(1):49-54.
- Grover C, Khurana A; Onychomycosis: newer insights in pathogenesis and diagnosis. Indian J Dermatol Venereol Leprol. 2012 May-Jun;78(3):263-70.
- Ataides FS, Chaul MH, El Essal FE, et al; Antifungal susceptibility patterns of yeasts and filamentous fungi isolated from nail infection. J Eur Acad Dermatol Venereol. 2012 Dec;26(12):1479-85. doi: 10.1111/j.1468-3083.2011.04315.x. Epub 2011 Nov 3.
- S1 Guideline onychomycosis; P Nenoff et al; Journal of the German Society of Dermatology
- Overview: Nail fungus; Institute for Quality and Efficiency in Health Care
- Fungal Skin and Nail Infections: Diagnosis and Laboratory Investigation - Quick Reference Guide for Primary Care; GOV.UK, 2017
- Fungal nail infection; NICE CKS, August 2023 (UK access only)
- Leelavathi M, Noorlaily M; Onychomycosis nailed. Malays Fam Physician. 2014 Apr 30;9(1):2-7. eCollection 2014.
- Elewski BE; Onychomycosis: pathogenesis, diagnosis, and management. Clin Microbiol Rev. 1998 Jul;11(3):415-29. doi: 10.1128/CMR.11.3.415.
- https://bnf.nice.org.uk/drugs/itraconazole/
- BNF Terbinafine
- Chang CH, Young-Xu Y, Kurth T, et al; The safety of oral antifungal treatments for superficial dermatophytosis and onychomycosis: a meta-analysis. Am J Med. 2007 Sep;120(9):791-8.
- Risk/benefit ratio of modern antifungal therapy: Focus on hepatic reactions; R J Hay; Journal of the American Academy of Dermatology
- Westerberg DP, Voyack MJ; Onychomycosis: Current trends in diagnosis and treatment. Am Fam Physician. 2013 Dec 1;88(11):762-70.
- Scher RK, Tavakkol A, Sigurgeirsson B, et al; Onychomycosis: diagnosis and definition of cure. J Am Acad Dermatol. 2007 Jun;56(6):939-44. Epub 2007 Feb 16.
- Arroll B, Oakley A; Preventing long term relapsing tinea unguium with topical anti-fungal cream: a case report. Cases J. 2009 Jan 21;2(1):70. doi: 10.1186/1757-1626-2-70.
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 25 Nov 2026
26 Nov 2021 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free