Necrobiosis lipoidica
Peer reviewed by Dr Rachel Hudson, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 15 Jun 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Continue reading below
What is necrobiosis lipoidica?1
Necrobiosis lipoidica is a rare inflammatory granulomatous skin disorder occurring as a result of collagen degeneration. It is characterised by irregularly shaped, callous lesions with reddish-brown pigmentation and central atrophy.
It was originally described in conjunction with diabetes. As it occurs in the absence of diabetes as well, it is now known as necrobiosis lipoidica, a term applied to all cases, whether occurring in those with diabetes or not.
The pathology is collagen degeneration with granulomatous response, associated with thickened blood vessels and fat deposition. The underlying cause is unknown but is believed to involve microangiopathy.2
For people with diabetes, prevention includes optimising glucose control. Improved glycaemic control can even lead to abatement in further progression to microvascular complications and improved long-term outcomes.3
How common is necrobiosis lipoidica? (Epidemiology)4
Back to contentsIt is a rare skin condition. Whilst there is a high prevalence of diabetes mellitus in patients with necrobiosis lipoidica (one third of cases have diabetes, and two thirds have glucose tolerance abnormalities), the reported prevalence of necrobiosis lipoidica in patients with diabetes is 1-2%.
It most commonly presents in the 30s but can present at any age, including infancy. It tends to appear earlier in those with diabetes than in others: in one study, approximately 2% of young people with diabetes (aged up to 22 years) had a necrobiosis lipoidica lesion compared with none of the control subjects.5
It is three times as common in women as it is in men. Non-diabetic familial clustering of necrobiosis lipoidica does occur but extremely rarely.
Smoking is more prevalent in patients with diabetes with necrobiosis lipoidica than in those without it, as are diabetic complications (retinopathy and nephropathy), although the presence of necrobiosis lipoidica does not correlate with diabetic control.
Continue reading below
Symptoms of necrobiosis lipoidica (presentation)
Back to contentsNecrobiosis lipoidica
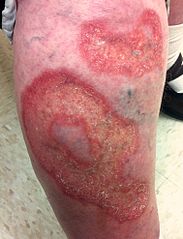
© Warfieldian, CC BY-SA 3.0, via Wikimedia Commons
Shiny patches slowly enlarge over months or years. They are initially a reddish brown and 1-3 mm in diameter but progress to yellow and become depressed and atrophic plaques.
The most common site is the pretibial area but they can occur on the face, scalp, trunk and upper arms where they are less likely to be correctly diagnosed.
There is often no pain (due to associated neuropathy) but it can be very painful.
Trauma produces ulceration.
Köbner's phenomenon may be demonstrated, in which lesions occur in areas of trauma. (This phenomenon is more typically associated with psoriasis and lichen planus.)
Differential diagnosis
Back to contentsUsually the appearance is fairly typical but variations can be difficult to diagnose. Consider as a cause of atypical leg ulcers in diabetic patients.6
Superficial annular lesions may look like granuloma annulare. However, granuloma annulare do not exhibit the typical yellow fatty appearance of necrobiosis lipoidica plaques.
Yellow, fatty lesions may resemble xanthoma.
Sarcoidosis can appear very similar, even on histology.
Erythema nodosum. These lesions do not ulcerate.
Rheumatoid nodules are similar histologically but tend to be raised rather than atrophic. Ulcerated necrobiotic areas have been described in rheumatoid arthritis.
Varicose eczema produces a scaly rash and is usually near the malleoli.
Continue reading below
Investigations
Back to contentsIf the patient is not known to have diabetes this must be checked. Biopsy of the lesion may be helpful but be aware of poor wound healing.
Management of necrobiosis lipoidica4 7
Back to contentsManagement is impaired by lack of understanding of the aetiology of the condition. No treatment to date is completely effective and, whilst numerous treatments have been tried, none has proven effectiveness based on controlled trials.1
Trauma should be avoided, and strategies for prevention of ulcers employed. Wound care for established ulcers is as for other diabetic ulcers.
Potent topical steroids are usually considered first-line treatment. This may reduce inflammation but it does not benefit burned-out lesions and may aggravate atrophy, so careful monitoring for this is required.
Intralesional injections of steroids are also sometimes helpful, but increase the risk of ulceration.
Immunomodulating drugs have also been used, including:
Studies demonstrate spontaneous healing of necrobiosis lipoidica following pancreas and kidney transplantation and the immunosuppressive regime is thought to have played a significant role in this.11 12Antiplatelet treatment seems logical but controlled trials have had different results. Aspirin and dipyridamole have been used. Pentoxifylline decreases blood viscosity and increases fibrinolysis and erythrocyte deformity and it may be helpful. Ticlopidine and perilesional injections of heparin have been used in uncontrolled trials.
Excision and grafting are occasionally used but poor healing and recurrence are common.
Phototherapy. Photodynamic therapy has been used, as have topical retinoids and topical psoralens with ultraviolet A (PUVA).
Laser treatment has been used to stabilise lesions and reduce erythema and telangiectasias.
Prognosis3
Back to contentsThe lesions often do not heal well and it becomes a chronic, relapsing condition. However, lesions are known to remit spontaneously and even resolve. The most common complication is ulceration, but occasionally squamous cell carcinoma can arise in areas of long-standing necrobiosis lipoidica.2 13
Further reading and references
- Related conditions - Necrobiosis lipoidica; Diabetes UK
- Dissemond J; Images in clinical medicine. Necrobiosis lipoidica diabeticorum. N Engl J Med. 2012 Jun 28;366(26):2502. doi: 10.1056/NEJMicm1109700.
- Necrobiosis lipoidica; DermNet NZ
- Lause M, Kamboj A, Fernandez Faith E; Dermatologic manifestations of endocrine disorders. Transl Pediatr. 2017 Oct;6(4):300-312. doi: 10.21037/tp.2017.09.08.
- Necrobiosis lipoidica; Primary Care Dermatology Society (PCDS).
- Feily A, Mehraban S; Treatment Modalities of Necrobiosis Lipoidica: A Concise Systematic Review. Dermatol Reports. 2015 Jun 8;7(2):5749. doi: 10.4081/dr.2015.5749. eCollection 2015 May 21.
- Reid SD, Ladizinski B, Lee K, et al; Update on necrobiosis lipoidica: a review of etiology, diagnosis, and treatment options. J Am Acad Dermatol. 2013 Nov;69(5):783-91. doi: 10.1016/j.jaad.2013.05.034. Epub 2013 Aug 19.
- Naik PP, Farrukh SN; Clinical Significance of Diabetic Dermatopathy. Diabetes Metab Syndr Obes. 2020 Dec 8;13:4823-4827. doi: 10.2147/DMSO.S286887. eCollection 2020.
- Grillo E, Rodriguez-Munoz D, Gonzalez-Garcia A, et al; Necrobiosis lipoidica. Aust Fam Physician. 2014 Mar;43(3):129-30.
- Pavlovic MD, Milenkovic T, Dinic M, et al; The prevalence of cutaneous manifestations in young patients with type 1 diabetes. Diabetes Care. 2007 Aug;30(8):1964-7. Epub 2007 May 22.
- Gottrup F, Karlsmark T; Leg ulcers: uncommon presentations. Clin Dermatol. 2005 Nov-Dec;23(6):601-11.
- Erfurt-Berge C, Seitz AT, Rehse C, et al; Update on clinical and laboratory features in necrobiosis lipoidica: a retrospective multicentre study of 52 patients. Eur J Dermatol. 2012 Nov-Dec;22(6):770-5. doi: 10.1684/ejd.2012.1839.
- Stanway A, Rademaker M, Newman P; Healing of severe ulcerative necrobiosis lipoidica with cyclosporin. Australas J Dermatol. 2004 May;45(2):119-22.
- Rallis E, Korfitis C, Gregoriou S, et al; Assigning new roles to topical tacrolimus. Expert Opin Investig Drugs. 2007 Aug;16(8):1267-76.
- Suarez-Amor O, Perez-Bustillo A, Ruiz-Gonzalez I, et al; Necrobiosis lipoidica therapy with biologicals: an ulcerated case responding to etanercept and a review of the literature. Dermatology. 2010;221(2):117-21. doi: 10.1159/000314694. Epub 2010 Jun 25.
- Gullo D, Latina A, Tomaselli L, et al; Healing of chronic necrobiosis lipoidica lesions in a type 1 diabetic patient after pancreas-kidney transplantation: a case report. J Endocrinol Invest. 2007 Mar;30(3):259-62.
- Souza AD, El-Azhary RA, Gibson LE; Does pancreas transplant in diabetic patients affect the evolution of necrobiosis Int J Dermatol. 2009 Sep;48(9):964-70.
- Lim C, Tschuchnigg M, Lim J; Squamous cell carcinoma arising in an area of long-standing necrobiosis lipoidica. J Cutan Pathol. 2006 Aug;33(8):581-3.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
15 Jun 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free