Neuropathic joints
Charcot joints
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 29 Dec 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
hropathia neurotica, neuropathic arthritis/arthropathy, tabetic osteoarthropathy
Continue reading below
What are neuropathic joints?
Neuropathic joints, often called Charcot joints, are caused by loss of sensation in the joint so that it is severely damaged and disrupted.1
The Charcot foot is triggered by a combination of mechanical, vascular and biological factors which can lead to late diagnosis and incorrect treatment and eventually to destruction of the foot.2
The damage and disruption becomes so gross that the diagnosis of a neuropathic joint is easily made as the destruction progresses, both on clinical examination and X-rays, because no one who had sensation would tolerate such destruction of the joint.
Causes of neuropathic joints (aetiology)
Any pathology that leads to loss of sensation in a joint may lead to a Charcot joint:
Classically, Charcot joints in the lower limb were most often the result of tabes dorsalis but that is much rarer these days.
The most common cause is diabetic neuropathy and diabetes is increasing in prevalence.
In the upper limb the classical cause is syringomyelia.
Diabetic neuropathy is common in developed countries where diabetes is common but in developing countries, tabes dorsalis and leprosy account for a significant amount of neuropathic joints.
Continue reading below
Neuropathic joint symptoms (presentation)
Suspect acute Charcot arthropathy if there is redness, warmth, swelling or deformity (in particular, when the skin is intact), especially in the presence of peripheral neuropathy or chronic kidney disease. Consider acute Charcot arthropathy even when deformity is not present or pain is not reported.3
Presentation is variable, depending upon the stage of the disease.4
There may be swelling.
There may be distortion.
There may be loss of function.
Pain is present in 75% but (considering the state of the joint) the clinician will be surprised that there is not considerably more pain.
The presence of pain does not exclude a Charcot joint.
Examination will often show that:
The skin over the joint is hot and red with an effusion of the joint.
There may also be osteomyelitis, complicating the picture.
There may be instability.
Examination of such a grossly affected joint will cause surprisingly little distress. As there is neuropathy, it is quite common to find that the skin is also ulcerated and this will cause further concern about infection and osteomyelitis.
Neurological examination should be performed to identify the extent of sensory loss and whether there is any motor loss too.
Charcot presentation
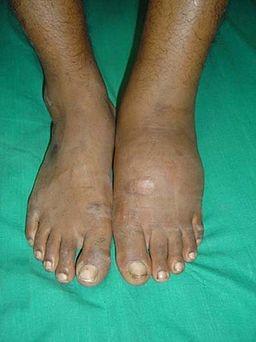
By J. Terrence Jose Jerome, CC BY 3.0, via Wikimedia Commons
The picture shows a Charcot foot due to diabetic neuropathy. There is a diffuse swelling in the left foot effusion. This may have been noted at a routine diabetes clinic whilst the patient complained of nothing.
There are a number of classifications of Charcot joints but these are mostly of interest to orthopaedic surgeons.
Differential diagnosis4
Severe trauma.
Osteomyelitis may well co-exist with a Charcot joint.
Continue reading below
Investigations5
A plain X-ray may show considerable disruption of the joint but, in early disease, the picture will resemble osteoarthritis.
MRI scanning or radionucleotide imaging may be valuable to differentiate soft tissue infection from osteomyelitis.
Investigation may also be required to ascertain the cause of the neuropathy, or HbA1C testing to assess the control of the diabetes.
Associated diseases
Diabetes, tabes dorsalis, syringomyelia and leprosy have been mentioned.
The differential diagnosis of peripheral neuropathy includes alcoholism, beriberi (vitamin B1 deficiency) and vitamin B12 deficiency.
Neuropathic joint treatment and management
Important information |
|---|
To confirm the diagnosis of acute diabetic Charcot arthropathy of the ankle/foot, refer the person within one working day to the multidisciplinary foot care service for triage within one further working day. Offer non-weight-bearing treatment until definitive treatment can be started by the multidisciplinary foot care service.3 |
General measures
The patient must be educated about the risk of damaging a joint that is devoid of pain.
An underlying disease may need to be treated. However, treatment of tertiary syphilis will not reverse tissue damage, although it will prevent further progression of that disease.
Alcoholism or deficiency diseases may require attention.
Good control of diabetes is essential to prevent progression of the neuropathy.
The affected joint is initially immobilised in a cast. It may still permit ambulation but this should be limited for best results. If there is ulceration, the cast must be changed weekly for ulcer evaluation and debridement. Plain X-rays every month help evaluate progress. The cast is usually on for three to six months.
Podiatry
After removing the cast, protection of the joint for the rest of the patient's life is essential. This requires patient education and foot care by a podiatrist. Various types of braces may protect the foot.
Various types of protective shoes may be required. If ulcers are present, a rocker bottom sole can be used. Plastic inserts can also be used for anaesthetic feet. A less intense regime may be permitted after 6-24 months, depending upon clinical progress; however, special footwear is required for life.
The total process of healing usually takes 1-2 years. Preventing further injury, noting temperature changes, checking feet every day, reporting trauma, and receiving professional foot care are important aspects of treatment.
Pharmacological
Bisphosphonates may be of value to help heal the bones, particularly if caught in the acute phase.6
Surgical
Surgery is indicated for patients with severe or unstable deformities that, if untreated, will result in major amputations.1
Current surgical options include fusion and Achilles tendon lengthening. There is little strong evidence and consensus concerning the timing of treatment and use of different fixation methods.7
Complications
Fractures can occur without pain and the absence of treatment leads to deformity.
Neuropathic ulcer may occur and introduce infection.
Soft tissue infection or osteomyelitis may occur.
Severe damage may require amputation.
Prognosis8
Charcot neuroarthropathy is a progressive, destructive condition that is characterised by acute fracture, dislocation and joint destruction. In its acute phase, it is often misdiagnosed and can lead to deformities, ulcerations and also amputation for soft tissue or bone infection. Early diagnosis and management are imperative to avoid rapid progression.9
A good prognosis therefore depends upon early recognition of the problem and effective management, which includes patient education.10
Charcot arthropathy is associated with higher mortality risk than diabetes alone but with lower risk than foot ulcer. A 2022 meta-analysis reported 5- to 7-year mortality rates between 15-24.5% depending on variable.11
Prevention
In Western societies the most important form of prevention would be the prevention of type 2 diabetes and the control of existing diabetes. Diabetes clinics facilitate early detection of problems.
In the developing world, prevention of syphilis and leprosy is still important.
History
Jean-Martin Charcot was a French neurologist who was born in Paris in 1825 and died in 1893. He is regarded as the father of neurology and has 15 medical eponyms, not all of them related to neurology. He described neuropathic joints due to syphilis in 1868 but the earliest recorded description would appear to be from William Musgrave in 1703.
Further reading and references
- Charcot Changes in the Diabetic Foot and Ankle; Wheeless' Textbook of Orthopaedics
- Jean-Martin Charcot; Whonamedit.com
- Varma AK; Charcot neuroarthropathy of the foot and ankle: a review. J Foot Ankle Surg. 2013 Nov-Dec;52(6):740-9. doi: 10.1053/j.jfas.2013.07.001. Epub 2013 Aug 18.
- Trieb K; The Charcot foot: pathophysiology, diagnosis and classification. Bone Joint J. 2016 Sep;98-B(9):1155-9. doi: 10.1302/0301-620X.98B9.37038.
- Diabetic foot problems: prevention and management; NICE Guidelines (August 2015 - last updated October 2019)
- Harris A, Violand M; Charcot Neuropathic Osteoarthropathy.
- Chan RLS, Chan CH, Chan HF, et al; The many facets of neuropathic arthropathy. BJR Open. 2019 Jul 29;1(1):20180039. doi: 10.1259/bjro.20180039. eCollection 2019.
- Durgia H, Sahoo J, Kamalanathan S, et al; Role of bisphosphonates in the management of acute Charcot foot. World J Diabetes. 2018 Jul 15;9(7):115-126. doi: 10.4239/wjd.v9.i7.115.
- Galhoum AE, Trivedi V, Askar M, et al; Management of Ankle Charcot Neuroarthropathy: A Systematic Review. J Clin Med. 2021 Dec 17;10(24):5923. doi: 10.3390/jcm10245923.
- Perrin BM, Gardner MJ, Suhaimi A, et al; Charcot osteoarthropathy of the foot. Aust Fam Physician. 2010 Mar;39(3):117-9.
- Idusuyi OB; Surgical management of Charcot neuroarthropathy. Prosthet Orthot Int. 2015 Feb;39(1):61-72. doi: 10.1177/0309364614560939.
- Diacogiorgis D, Perrin BM, Kingsley MIC; Factors impacting the evidence-based assessment, diagnosis and management of Acute Charcot Neuroarthropathy: a systematic review. J Foot Ankle Res. 2021 Apr 7;14(1):26. doi: 10.1186/s13047-021-00469-5.
- Yammine K, Boulos K, Assi C, et al; Amputation and mortality frequencies associated with diabetic Charcot foot arthropathy: a meta-analysis. Foot Ankle Surg. 2022 Dec;28(8):1170-1176. doi: 10.1016/j.fas.2022.08.004. Epub 2022 Aug 13.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 16 Dec 2027
29 Dec 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free