Pneumonia
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Mohammad Sharif Razai, MRCGPLast updated 24 Jun 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Pneumonia article more useful, or one of our other health articles.
In this article:
There are separate articles on Aspiration pneumonia, Pneumocystis jirovecii pneumonia and Lower respiratory tract infection in children.
Continue reading below
What is pneumonia?
Pneumonia is characterised by acute inflammation, with an intense infiltration of neutrophils in and around the alveoli and terminal bronchioles. Due to the resulting inflammation and oedema, the affected bronchopulmonary segment or entire lobe may be consolidated.
Pneumonia is typically classified based on the causative organism. Symptoms of pneumonia include cough, fever, dyspnoea, chest pain, and fatigue. The risk factors, signs, and symptoms of each type of pneumonia may vary according to its aetiology and pathogenic mechanism.
Risk factors1
Back to contentsAge: especially infants, young children and the elderly.
Lifestyle: smoking and alcohol.
Preceding viral infections: for example, influenza can predispose individuals to Streptococcus pneumoniae infection.
Respiratory: asthma, chronic obstructive pulmonary disease (COPD), malignancy, bronchiectasis and cystic fibrosis.
Immunosuppression: AIDS and cytotoxic therapy increase the risk of infection with Staphylococcus species, tuberculosis, Gram-negative bacilli, and Pneumocystis jirovecii.
Intravenous drug abuse: often associated with Staphylococcus aureus infection.
Hospitalisation: often involves Gram-negative organisms.
Aspiration pneumonia: patients with impaired consciousness, neurological diseases such as cerebrovascular or Parkinson's disease, or oesophageal obstruction are at risk. Aspiration pneumonia typically affects the right lung and is caused by anaerobes from the oropharynx.
Underlying predisposing diseases, such as diabetes mellitus and cardiovascular disease.
Proton pump inhibitors are associated with a 1.5-fold increased risk of community-acquired pneumonia due to reduced gastric acid secretion, which facilitates pathogen colonisation of the upper respiratory tract.23
Continue reading below
Community-acquired pneumonia
Back to contentsThis is pneumonia acquired outside hospitals or healthcare facilities. It involves the presence of symptoms and signs consistent with acute lower respiratory tract infection, accompanied by new radiographic shadowing for which there is no alternative explanation.
Pathogenesis
The most likely organisms are: S. pneumoniae, S. aureus, Mycoplasma pneumoniae, Haemophilus influenzae, Chlamydophila pneumoniae and respiratory viruses.5 Mixed pathogens occur up to 25% of the time.
How common is pneumonia? (Epidemiology) 6
0.5-1% of people in the UK develop community-acquired pneumonia (CAP) every year.
Among adults who present to GPs with symptoms of lower respiratory tract infection, 5-10% are diagnosed with CAP, and 22-42% of these cases are admitted to hospital.
The mortality rate for CAP is between 5% and 14%, and more than 50% of pneumonia-related deaths occur in people over the age of 84.
1.2-10% of adults admitted to hospital with CAP require admission to intensive care units, and for these patients, the risk of dying is more than 30%.
CAP results in about 100,000 hospital admissions each year in England.
Most episodes of CAP occur during the autumn or winter.7
Symptoms and signs of pneumonia (presentation)
Symptoms: cough, purulent sputum (may be blood-stained or rust-coloured), dyspnoea, fever, pleuritic chest pain, rigors and night sweats.
The elderly may present with mainly systemic symptoms such as confusion, malaise, fatigue, anorexia, myalgia, and worsening pre-existing health conditions.
Children and young adults may present with nausea, abdominal pain, diarrhoea, sore throat, and headache.
Signs: tachypnoea, bronchial breathing, crepitations, pleural rub, dullness with percussion.
Diagnosis is unlikely if there are no focal chest signs, and heart rate, respiratory rate and temperature are normal.
Assessing whether patients with CAP need hospital admission6
The decision to admit is based on a variety of factors, including the severity of illness, age, underlying health problems and social circumstances.
The National Institute for Health and Care Excellence (NICE) recommends using the CRB-65 score in conjunction with clinical judgement.
A 4-point score system is used, with one point for each of the following:
Confusion: abbreviated mental test score of 8 or less, or new disorientation in person, place or time.
Respiratory rate: 30 breaths/minute or more.
Blood pressure: systolic blood pressure below 90 mm Hg or diastolic below 60 mm Hg.
Age: 65 years or older.
Patients who have a CRB-65 score of 0 are at low risk of mortality and should be considered for home care. Consider hospital admission for all other patients, particularly those with a CRB-65 score of 2 or higher. For patients with a score of 3 or more (high-severity), immediate hospital admission is required.
Management of community-acquired pneumonia
When managing pneumonia, use a systematic approach to patient assessment and management.
Oxygen: administer oxygen for hypoxia and consider ventilation if there is severe hypoxia.
Fluids: provide intravenous fluids to patients with volume depletion.
Analgesics: use non-steroidal anti-inflammatory drugs (NSAIDs) and paracetamol for mild pleuritic pain. More severe pain may require opiate analgesia, but caution is needed to avoid aggravating CO2 retention.
Nebulised saline may help with expectoration.
Chest physiotherapy has doubtful benefit for pneumonia. Physiotherapy may be more important in helping to mobilise the patient, but a Cochrane review found no effect on reducing mortality.9
Advise patients with CAP to avoid smoking, rest, and drink plenty of fluids.
Safety netting advice
Those who fail to improve after 72 hours of treatment should be advised to seek further medical advice. All cases that cause concern should be considered for hospital admission. Community patients should be advised to return if their symptoms do not resolve after three weeks.
Antibacterials are recommended in all suspected cases of pneumonia, starting as soon as possible.
Antimicrobial therapy should be based on the patient's characteristics, the setting, the severity of pneumonia, and available information regarding local pathogens and resistance patterns.
Low-severity CAP:
Offer a five-day course of amoxicillin, reserving clarithromycin, erythromycin (in pregnancy) or doxycycline for patients allergic to penicillin or if an atypical pathogen is suspected.
Stop antibiotics after five days unless microbiology results suggest a longer course or the patient is not clinically stable.
Moderate-to-severe CAP:
Patients with moderate-to-severe CAP are normally treated in hospital. However, there may be occasions (eg, when a patient refuses admission) when the GP is required to provide treatment.
For moderate-severity CAP, treatment should be as per low-severity CAP pending microbiology results.
For high-severity CAP, a five-day course of co-amoxiclav with clarithromycin or erythromycin (in pregnancy) should be offered. The oral or intravenous route can be used, though the latter may prove challenging in the community.
Levofloxacin orally or intravenously is an option for patients allergic to penicillin.
Pneumonia due to atypical pathogens1011
Back to contentsPathogenesis
The most common organisms are:
Mycoplasma pneumoniae.
Chlamydophila pneumoniae.
Legionella pneumophila.
Other micro-organisms that cause similar patterns of presentation via pulmonary infection include:
Chlamydophila psittaci: exposure to birds, particularly ill ones, is a useful clue in history.
Coxiella burnetii: presenting as Q fever.
Viral pneumonias: including influenza A, severe acute respiratory syndrome (SARS), respiratory syncytial virus (RSV), adenoviridae and pneumonitis due to varicella (chickenpox pneumonitis).
Epidemiology
Atypical organisms might be implicated in about 22% of CAP globally. 1213
Risk factors
Mycoplasma and Chlamydophila spread by person-to-person contact, with transmission most common in closed populations such as schools and offices.
Legionellae are typically found in infested water and man-made water systems.
Coxiella burnetii is transmitted by inhalation or by ingestion of contaminated animal products.
Symptoms of atypical pneumonia
M. pneumoniae:14
Vague and slow-onset history over a few days or weeks of constitutional upset, fever, headache, dry cough with tracheitic ± pleuritic pain, myalgia, malaise and sore throat.
This is like many of the common viral illnesses but the persistence and progression of symptoms is what helps to mark it out.
In otherwise healthy individuals, it usually resolves spontaneously over a few weeks.
The hacking, dry cough can be very persistent.
Extra-respiratory features include rashes such as erythema multiforme, erythema nodosum and urticaria; neurological complications like Guillain-Barré syndrome, transverse myelitis, cerebellar ataxia and aseptic meningitis; haematological complications such as cold agglutinin disease and haemolytic anaemia; joint symptoms like arthralgia and arthritis; cardiac complications such as pericarditis and myocarditis; rarely, may cause pancreatitis.
C. pneumoniae:15
Gradual onset, which may show improvement before worsening again; incubation period is 3-4 weeks.
Initial nonspecific upper respiratory tract infection symptoms lead on to bronchitic or pneumonic features.
Most of those infected remain well or are asymptomatic.
Cough with scanty sputum is a prominent feature.
Hoarseness is a common feature.
Headache affects the majority of symptomatic sufferers.
Fever is relatively unusual.
Symptoms may drag on for weeks or months, despite a course of appropriate antibiotics.
Where it causes significant problems, this may be due to secondary infection or co-existing illness, such as diabetes.
L. pneumophila:16
This tends to be the most severe of the pneumonias due to atypical pathogens. See the separate Legionnaires' disease article.
Focal outbreaks centred around poorly maintained air-conditioning or humidification systems, often noted retrospectively by public health physicians.
It has 2-10 days' incubation period.
Initial mild headache and myalgia leading to high fever, chills and repeated rigors; non-chest symptoms often predominate early on.
Cough is nearly always present, initially unproductive but may lead to expectoration later.
Dyspnoea, pleuritic pain and haemoptysis are not uncommon.
Gastrointestinal upset, such as diarrhoea, nausea and vomiting or loss of appetite/anorexia, may occur.
There may be neurological complications such as confusion, disorientation and focal neurological deficit.
Arthralgia and myalgia are often reported.
Severe complications include pancreatitis, peritonitis, pericarditis, myocarditis, endocarditis and glomerulonephritis.
Signs of atypical pneumonia
Look for evidence of extra-thoracic involvement if an atypical pathogen is suspected, and check vital signs.
Chest signs are generally not helpful. Indeed, the discordance between the chest signs and the patient's illness or the floridity of initial CXR appearance often raises suspicion of an atypical pathogen.
Nonspecific chest signs and evidence of consolidation may be found but this is much less common than in the 'standard' pneumonias.
There may be signs in other systems, due to complications of the infection.
Management of atypical pneumonia
Pneumonias due to atypical pathogens are usually treated as for other CAP, at least initially. Serological testing is of little value for most patients with CAP.11
Doxycycline, clarithromycin, and erythromycin (the preferred option in pregnancy) have been shown to be effective in treating all three most common infective organisms. They should be considered in all cases of pneumonia (including community-acquired) where atypical pathogens are suspected.10
Resistance to macrolides is a growing concern.17
Severe legionella infections may require rifampicin as well as a macrolide.16 .
Fluoroquinolones are also effective against all three of the common infective organisms.10
Continue reading below
Hospital-acquired pneumonia6 18
Back to contentsThis is defined as a new infection of lung parenchyma appearing more than 48 hours after admission to the hospital.
It occurs mostly in patients who are severely debilitated, immunocompromised or mechanically ventilated.
Infection occurring less than five days after hospital admission is usually caused by S. pneumoniae.
Infection occurring after this time is usually caused by H. influenzae , methicillin-resistant Staphylococcus aureus (MRSA), Pseudomonas aeruginosa and other non-pseudomonal Gram-negative bacteria.
Hospital-acquired pneumonia is often caused by multiple organisms.
Differential diagnoses
Back to contentsPulmonary oedema.
Pleural effusion.
Pneumothorax.
Pulmonary embolus.
Asthma.
COPD.
Bronchiectasis.
Fibrosing alveolitis.
Neoplasm.
Sarcoidosis.
Pneumonia complication - eg, empyema and lung abscess.
Diagnosing pneumonia (investigations)6
Back to contentsInvestigations are usually not necessary for the majority of patients managed in the community. Simple methods such as pulse oximetry can be used to assess oxygenation and clinical status.
If a patient is admitted to the hospital, the following investigations could help with the diagnosis:
Chest X-ray
A definitive diagnosis of CAP requires evidence of consolidation on a chest x-ray (CXR). Therefore, it is recommended to perform a CXR for all patients admitted to hospital as soon as possible, ideally within 4 hours of admission.
Blood tests
Full blood count with differential white cell count.
C-reactive protein (CRP) to aid diagnosis and as a baseline measure.
Urea and electrolytes.
Liver function tests.
Blood cultures.
Arterial Blood Gas (ABG)
Other tests
Sputum examination and culture.
Aspiration of pleural fluid (for biochemistry and culture).
Pneumococcal and legionella urinary antigen tests.
Radiographic image of pneumonia before (left) and after (right) antibiotic therapy
Acute pneumonia
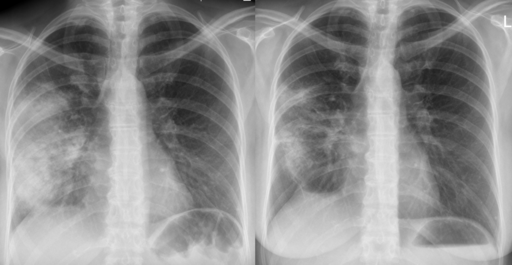
© Hellerhoff, CC BY-SA 3.0, via Wikimedia Commons
Complications of pneumonia
Back to contentsPleural effusion that is usually sterile.
Empyema: a reactive effusion can occur but is trivial. Empyema is potentially more serious and presents as the persistence of fever and leukocytosis after 4-5 days of appropriate antibiotic therapy.
Lung abscess: can be caused by S. pneumoniae and is classically seen in patients with klebsiella or staphylococcal pneumonia.
Acute Respiratory Distress Syndrome (ARDS)
Pneumatocele.
Pneumothorax.
Pyopneumothorax, eg, following rupture of a staphylococcal lung abscess in the pleural cavity.
Deep vein thrombosis (DVT).
Septicaemia, pericarditis, endocarditis, osteomyelitis, septic arthritis, cerebral abscess, and meningitis (particularly in pneumococcal pneumonia).
Postinfective bronchiectasis.
Acute kidney injury.
Prognosis
Back to contentsMortality from CAP is less than 1% in those well enough to be managed in the community.19 The mortality rate in patients admitted to hospital is 5-10% for those not requiring intensive care unit admission, as high as 25% in intubated patients and nearly 50% in intensive care unit patients requiring administration of vasopressors.20
Legionella has the most severe course and may cause significant morbidity if not treated early. A meta-analysis of patients on two different treatment regimes reported that those taking quinolones had a mortality rate of 4%, while those taking macrolides had a mortality rate of 10.9%.21
Prevention
Back to contentsThe main methods of prevention are managing risk factors, primarily through vaccination and smoking cessation.
Vaccination
According to the UK Health Security Agency, adults aged 65 or over and at-risk groups (eg, those with diabetes, chronic respiratory disease, chronic kidney disease, or who are immunosuppressed) should be offered a single dose of the 23-valent pneumococcal polysaccharide vaccine (PPV23).
Adults aged 65 or over and at-risk groups should also receive an annual influenza vaccine if there are no contraindications.
Smoking cessation
Cigarette smoking, including passive smoking, is an independent risk factor for CAP.22 Therefore, it is crucial to encourage smoking cessation, particularly for those at risk of pneumonia.
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Pneumonia in adults; NICE Quality standard, January 2016
- Heo JY, Song JY; Disease Burden and Etiologic Distribution of Community-Acquired Pneumonia in Adults: Evolving Epidemiology in the Era of Pneumococcal Conjugate Vaccines. Infect Chemother. 2018 Dec;50(4):287-300. doi: 10.3947/ic.2018.50.4.287.
- Torres A, Peetermans WE, Viegi G, et al; Risk factors for community-acquired pneumonia in adults in Europe: a literature review. Thorax. 2013 Nov;68(11):1057-65. doi: 10.1136/thoraxjnl-2013-204282.
- Abramowitz J, Thakkar P, Isa A, et al; Adverse Event Reporting for Proton Pump Inhibitor Therapy: An Overview of Systematic Reviews. Otolaryngol Head Neck Surg. 2016 Oct;155(4):547-54. doi: 10.1177/0194599816648298. Epub 2016 May 17.
- Eom CS, Jeon CY, Lim JW, et al; Use of acid-suppressive drugs and risk of pneumonia: a systematic review and meta-analysis. CMAJ. 2011 Feb 22;183(3):310-9. doi: 10.1503/cmaj.092129. Epub 2010 Dec 20.
- Durrington HJ, Summers C; Recent changes in the management of community acquired pneumonia in adults. BMJ. 2008 Jun 21;336(7658):1429-33.
- Woodhead M, Blasi F, Ewig S, et al; Guidelines for the management of adult lower respiratory tract infections--summary. Clin Microbiol Infect. 2011 Nov;17 Suppl 6:1-24. doi: 10.1111/j.1469-0691.2011.03602.x.
- Pneumonia: Diagnosis and management of community- and hospital-acquired pneumonia in adults; NICE Clinical Guideline (December 2014 - last updated October 2023)
- Oosterheert JJ, Bonten MJ, Schneider MM, et al; Effectiveness of early switch from intravenous to oral antibiotics in severe community acquired pneumonia: multicentre randomised trial. BMJ. 2006 Dec 9;333(7580):1193. doi: 10.1136/bmj.38993.560984.BE. Epub 2006 Nov 7.
- Annotated BTS Guideline for the management of CAP in adults; British Thoracic Society (2009 - Summary of recommendations updated 2015)
- Yang M, Yan Y, Yin X, et al; Chest physiotherapy for pneumonia in adults. Cochrane Database Syst Rev. 2013 Feb 28;(2):CD006338. doi: 10.1002/14651858.CD006338.pub3.
- Pneumonia (community-acquired): antimicrobial prescribing; NICE Guidance (September 2019)
- Guidelines for the management of adult lower respiratory tract infections; European Respiratory Society and European Society of Clinical Microbiology and Infectious Diseases (September 2011)
- Arnold FW, Summersgill JT, Ramirez JA; Role of Atypical Pathogens in the Etiology of Community-Acquired Pneumonia. Semin Respir Crit Care Med. 2016 Dec;37(6):819-828. doi: 10.1055/s-0036-1592121. Epub 2016 Dec 13.
- Bjarnason A, Westin J, Lindh M, et al; Incidence, Etiology, and Outcomes of Community-Acquired Pneumonia: A Population-Based Study. Open Forum Infect Dis. 2018 Feb 8;5(2):ofy010. doi: 10.1093/ofid/ofy010. eCollection 2018 Feb.
- Waites KB, Xiao L, Liu Y, et al; Mycoplasma pneumoniae from the Respiratory Tract and Beyond. Clin Microbiol Rev. 2017 Jul;30(3):747-809. doi: 10.1128/CMR.00114-16.
- Choroszy-Krol I, Frej-Madrzak M, Hober M, et al; Infections caused by Chlamydophila pneumoniae. Adv Clin Exp Med. 2014 Jan-Feb;23(1):123-6.
- Brady M et al; Legionnaires' Disease (Legionella Infection), 2019
- Sharaby Y, Nitzan O, Brettar I, et al; Antimicrobial agent susceptibilities of Legionella pneumophila MLVA-8 genotypes. Sci Rep. 2019 Apr 16;9(1):6138. doi: 10.1038/s41598-019-42425-1.
- Pneumonia (hospital-acquired): antimicrobial prescribing; NICE Guidance (September 2019)
- Guidelines for the management of community acquired pneumonia in adults; British Thoracic Society (2009), Thorax Vol 64 Sup III
- Restrepo MI, Faverio P, Anzueto A; Long-term prognosis in community-acquired pneumonia. Curr Opin Infect Dis. 2013 Apr;26(2):151-8. doi: 10.1097/QCO.0b013e32835ebc6d.
- Burdet C, Lepeule R, Duval X, et al; Quinolones versus macrolides in the treatment of legionellosis: a systematic review and meta-analysis. J Antimicrob Chemother. 2014 Sep;69(9):2354-60. doi: 10.1093/jac/dku159. Epub 2014 May 14.
- Lim WS, Baudouin SV, George RC, et al; BTS guidelines for the management of community acquired pneumonia in adults: update 2009. Thorax. 2009 Oct;64 Suppl 3:iii1-55. doi: 10.1136/thx.2009.121434.
Continue reading below
About the authorView full bio

Dr Mohammad Sharif Razai, MRCGP
General Practitioner. Medical Author
BSc, BA, MBBChir, MA (Cantab), MRCGP (2021), FHEA, MA (Distn)
Dr Mohammad Sharif Razai is an award-winning interdisciplinary scientist, clinician and educator. He holds an MA and a Bachelor of Medicine and Surgery from the University of Cambridge, a BSc from University College London and an MA from Birkbeck University of London.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 23 Jun 2027
24 Jun 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free