Rheumatic fever
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 30 Sept 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Rheumatic fever article more useful, or one of our other health articles.
In this article:
Continue reading below
What is rheumatic fever?
Rheumatic fever (RF) used to be a fairly common disease among children in developed countries until about the middle of the 20th century. It was a major cause of death in children until 1960 and a common cause of chronic structural heart disease in developed countries. In developing countries it still remains a major cause of death and heart disease.
Pathogenesis1
Back to contentsThe pathogenesis and immune mechanisms are not fully understood.
It is caused by Lancefield group A beta-haemolytic streptococci (GpA BHS) of which those with the M antigen are most likely to cause the disease (M types 3, 5, 18, 19, 24). However, RF and rheumatic heart disease have been discovered in communities where other responsible serotypes have been found.2
It is thought that host susceptibility, virulence of the organism and the environment combine to determine the clinical manifestation and the severity in a particular individual.
The decline in RF is not just due to penicillin but also to improved social conditions and a reduction in virulence of the GpA BHS. It remains prevalent in other parts of the world, particularly developing countries.3
The disease affects joints, skin, heart and nervous system.
Twin studies have shown a 44% monozygotic concordance but only a 12% dizygotic concordance, strongly supporting the idea of a genetic susceptibility to developing rheumatic fever after exposure to the bacterium, rather than a simple throat infection.4
The features of the disease are thought to be the result of a hypersensitivity reaction caused in the main by cross-reacting antibodies. It is thought there is a combined humoral and cell-mediated immune response to the bacterium (pharyngitis or skin streptococcal infection) which may lead to infiltration of the heart valve endothelium by T cells cross-reactive with streptococcal M protein and cardiac myosin.1
Pathological evaluation of the valves of patients dying from acute rheumatic fever (ARF) indicates microscopic disease in each of the four cardiac valves. Clinically, the mitral valve is involved in 90-95% of this group, in whom 20-25% also have aortic valve involvement. Isolated aortic valve, tricuspid valve or pulmonary valve involvement is much less common.5
Continue reading below
How common is rheumatic fever? (Epidemiology)
Back to contentsDifferent methods of collecting data can make comparisons of statistics very difficult. The incidence remains high where there is overcrowding and poor access to healthcare. In these populations with the highest incidence it is often most difficult to obtain reliable epidemiological data.
The incidence is highest in children aged 2-8 and 89% of all cases in England are found in children aged under 10.
The incidence of RF is 8-51 per 100,000 people worldwide, with incidence of ARF having fallen in high-income countries to less than 1 per 100,000 population. However, it is much less common in developed countries than in developing countries.6
Even in developed countries, prevalence is a function of socio-economic status. The incidence is higher particularly when there is overcrowding and in the winter and spring months.
The incidence in developing countries remains high. The indigenous populations of Australia and New Zealand have some of the highest incidences recorded in recent years with 374 per 100,000 per year in those aged 5-14 years. Around 60% of these patients develop rheumatic heart disease. Sub-Saharan Africa has been identified as a high-burden area, although accurate data are hard to collect.7
At least 233,000 deaths are attributable to rheumatic fever or rheumatic heart disease each year.8
Risk factors
Overcrowding, poor hygiene and lack of access to medical services are all important. In hot countries, skin infection is a more important source of streptococci than pharyngitis. Those at the extremes of age (young or old) are particularly at risk, as are those who are immunocompromised, have comorbidities such as diabetes, or have concurrent chickenpox or influenza, and who are dependent on drugs or alcohol.9 10
Rheumatic fever symptoms and presentation3
Back to contentsSymptoms appear between one and five weeks after a sore throat, with an average of three weeks.
In recurrent cases this incubation period is shorter, in keeping with a faster immune response.
The diagnosis is based on major and minor criteria. In the acute disease the arthritis and toxicity are obvious but it can be more insidious with mild carditis. This probably accounts for only about half of those with typical rheumatic heart disease giving a history of RF.
Diagnosis is based on Jones Criteria that were devised in 1944, revised in 1992 and updated in 2015.11 The update included the role of echocardiography to detect subclinical valvular lesions.3 They can be used to identify patients with a high likelihood of having RF.
Jones Criteria
A method of identifying patients with a high likelihood of having RF:
Evidence of recent streptococcal infection (eg, history of scarlet fever, positive throat swab or rising or increased antistreptolysin O titre (ASOT) >200 U/mL or DNase B titre).
Plus two major criteria; or
One major and two minor criteria.
Definitions of these criteria are set out below.
Major criteria
Polyarthritis:
The most obvious presenting feature is a flitting or migratory arthritis affecting large joints like the knees, ankles, wrists and elbows.
The joints are hot and red with decreased range of movement. Typically, one joint is exquisitely painful and inflamed while another is improving.
Usually one or two joints are affected at any time with each being only involved for between a few hours and a few days.
Aspirin has been the traditional treatment but nowadays other non-steroidal anti-inflammatory drugs (NSAIDs) might be considered in view of Reye's syndrome. If it fails to respond, consider an alternative diagnosis.Carditis (occurs in 40% of patients):
There is a pancarditis affecting the pericardium, myocardium and the endocardium.
Endocarditis leads to valvular heart disease which, along with myocarditis, is fatal in about 1%.
Examination of the pulse will show tachycardia beyond that expected for the temperature.
A murmur of aortic regurgitation is common in older children or young adults.
Auscultation of the heart may reveal a pericardial rub. It is present in 40-60% without chorea and 20-30% with chorea.
Carditis has characteristic findings on Doppler echocardiography. The mitral valve is the most common to be involved at 65-70%, with the aortic valve second at 25%. Aortic valve disease, unlike most other manifestations of this disease, is more common in males. The tricuspid valve is affected in barely 10% and involvement of the pulmonary valve is very rare.
Nearly all acquired mitral valve disease is rheumatic in origin. Certain characteristic murmurs have acquired eponymous names:
Carey Coombs' murmur is a soft, short diastolic filling murmur due to vegetations on the mitral valve.
Austin Flint's murmur is from aortic regurgitation as the vibration of the anterior leaflet of the mitral valve is buffeted simultaneously by the blood jets from the left atrium and the aorta.
Chorea (also known as Sydenham's chorea and 'St Vitus' Dance'):
Occurs in 10-30% of patients.
It usually presents in children between 7-12 years, with a female preponderance.
There are both psychological and physical features. It causes rapid and purposeless movements, particularly of the face and upper extremities.
Paediatric autoimmune neuropsychiatric disorder associated with streptococcal infection (PANDAS) and Tourette's syndrome are other varieties of movement and neurological disorders described.
It may stop when the patient sleeps.
Subcutaneous nodules:
Occur in 10% of patients.
They are infrequent and appear over the extensor surfaces of the elbows, knees, ankles, knuckles, scalp and spinous processes of the lumbar and thoracic vertebrae.
They are firm, painless lumps from a few millimetres to 2 cm in size.
They are normally in crops of three or four, appearing 2-3 weeks after onset of fever.
The histology resembles Aschoff bodies found in the heart and they are indicative of severe carditis.
Erythema marginatum (also known as erythema annulare):
It occurs in about 5-15% of patients.
The rash comprises pale-red macules or papules between 1 cm and 3 cm in diameter on the trunk and proximal limbs but never on the face.
The rash occurs early in the disease and remains long past the resolution of other symptoms.
It is exacerbated by heat and fades when the patient is cool.
Rash (non-itchy) of erythema marginatum
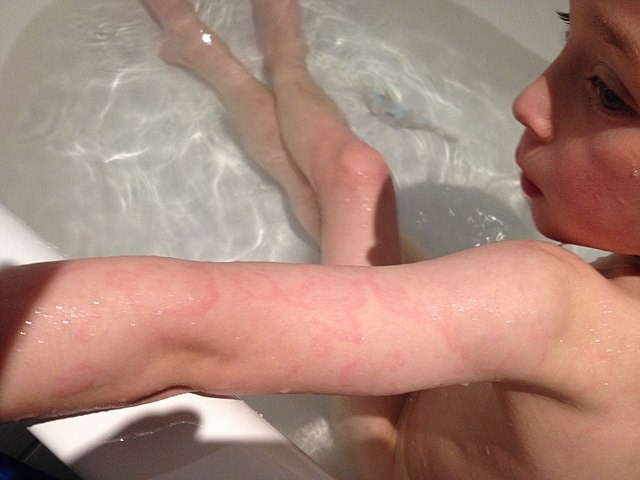
© Adsie, CC BY-SA 4.0, via Wikimedia Commons
Minor criteria
Fever:
This is present in 90% of cases. It is usually over 39°C, stays high for a week and is lower for the following two weeks.
In pure chorea the patient may be apyrexial.
ESR or serum CRP are raised (greater than 60 mm/h or 3.0 mg/dl respectively).
Arthralgia (but not if arthritis is one of the major criteria).
Prolonged PR interval (but not if carditis is the major criterion).
Those working in countries where there is a higher risk of rheumatic fever should note that there are slightly different Jones criteria for those whose patients are at a medium or high risk of rheumatic fever. See our Jones Criteria reference which includes Table II Diagnostic criteria for rheumatic fever, modified 2015.11
Other clinical scenarios
There are three other clinical scenarios that are not part of the Jones criteria but merit attention:
Chorea may occur late and be the only feature of the disease.
Low-grade carditis may present too late for diagnosis of the RF.
Newly ill patients with a history of RF, especially with heart disease, who have supporting evidence of a recent streptococcal infection and who have either a single major or several minor criteria.
The paper looking at the revision of the Jones Criteria also addresses the question of excessive diagnosis.12
Continue reading below
Differential diagnosis13
Back to contentsArthritis - consider:
Rheumatoid arthritis (including Still's disease in children).
Heart disease - consider:
Rash (erythema marginatum) - consider:
Chorea - consider:
Drug reactions (especially in young people) to: metoclopramide, oral contraceptives, phenytoin, haloperidol or amitriptyline.
Huntington's disease. This does not usually present until at least the age of 30 years (peak age 35-45).
Chorea gravidarum may occur in pregnancy.
Investigations5 13
Back to contentsThroat swabs are usually performed but may fail to grow streptococci by the time symptoms of RF appear.
Clinical features begin when antibodies are at a peak. Antistreptococcal antibodies are especially useful in patients with only chorea. Sensitivity can be improved by testing for several antibodies:
Check antibody titres two weeks apart for a rise.14
The most common antibodies tested include ASO and anti-DNase B, antihyaluronidase, antistreptokinase, antistreptococcal esterase and anti-nicotinamide adenine dinucleotide (anti-NAD).
Generally, the antibodies rise during the first month after infection and then plateau for 3-6 before returning to normal levels at 6-12 months. ASOT peaks 2-3 weeks after the onset of clinical disease and there is a sensitivity of 80-85%. Anti-DNase B has a slightly higher sensitivity at 90%.
ECG may show a prolonged PR interval and possibly other features too. Tachycardia is usual, although some children develop bradycardia. ST elevation suggests pericarditis.
CXR may show features of heart failure.
Doppler echocardiography is more sensitive than clinical assessment in the detection of carditis in acute RF and can contribute to earlier diagnosis. The use of handheld echocardiography is being explored in low resource settings.15
RF should still be considered as a likely diagnosis, even if criteria are not fully satisfied, when there is chorea or carditis without apparent cause and recent streptococcal infection, or when the patient has had previous RF and has symptoms of a recurrence.
Rheumatic fever treatment and management5 13
Back to contentsThe main aims of management are to:
Eradicate the streptococcal infection if infection is still present (usually a pharyngitis).
Suppress inflammation arising from the autoimmune response.
Provide supportive treatment, particularly for cardiac complications such as congestive cardiac failure.
General
This is one of the very few conditions in which bed rest is enforced even if the patient feels well enough to be up and about. Full activity should not be resumed until markers for inflammation and infection (acute-phase reactants) have returned to normal.
Drugs
The initial infection should be treated with appropriate antibiotics - IM benzathine penicillin is usually recommended. Azithromycin is recommended in cases of true penicillin allergy and it may also be worth discussing with your local microbiology team.16
IM penicillin is a painful injection - reconstituting it with 1% lidocaine is recommended to reduce the pain.17
Aspirin usually relieves arthritis within a few days. High doses are required and other NSAIDs like naproxen may be safer.18
Heart failure will require usual management. If this fails, consider cardiac surgery - even in acute failure. Mitral valve repair or replacement may be life-saving.17
Chorea is often self-limiting but is likely to need suppression with diazepam. Chorea may be treated with haloperidol, although this drug can cause extrapyramidal effects. Other possible treatments include steroids, intravenous immunoglobulin and plasma exchange.19
Complications
Back to contentsThe most important complications and sequelae derive from:
Carditis.
Mitral stenosis.
Congestive cardiac failure.
Prognosis
Back to contentsIt is difficult to give exact numbers of how likely acute RF is to lead to chronic RF, because in many cases of chronic RF there is no reported history of acute RF, suggesting that the acute infection was not diagnosed or treated. One study of children with acute RF, found that 72% of the 258 children developed chronic valvular disease, 16% severely. Progression is highest in the first year after acute RF. Patients need long-term follow-up of cardiac status and myocarditis leaves the myocardium weak for life. Most recurrences occur within five years of the original episode.17
Clinical features of RF resolve inside 12 weeks in 80%.13
Chorea can occasionally continue in remitting fashion for years. Mortality is rare in industrialised countries but is about 1.5% per year globally.5 Penicillin is said to have significantly reduced the rate of valvular heart disease.20
Rheumatic fever prevention
Back to contentsSecondary prophylaxis requires that every patient should start a long-term programme of regular antibiotics to prevent further GpA BHS infection.2 The duration of prophylaxis is the subject of some controversy; a recent American Heart Association summary gives a list of the different recommendations made by different groups, which include for 10 years after the last episode of acute RF, until the age of 40, and for life if there has been valve surgery or severe valve damage.17
A vaccine against RF is possible in theory but has not yet been developed.21 Prophylactic antibiotics before dental or surgical treatment (to prevent infective endocarditis) are no longer recommended routinely for patients with acquired valve disease.
Historical perspective22
Back to contentsThis often dramatic disease has been recognised for centuries. Baillou (1538-1616) realised that the arthritis was different to gout. Sydenham (1624-1668) famously described the chorea. The association of RF with sore throat was made in 1880 and the association with scarlet fever in the early 1900s. The arrival of antibiotics in the 1940s heralded the start of treatment and preventative strategies. The incidence in developed countries has declined since. Unfortunately, developing countries have not benefited very much from the progress made.
Further reading and references
- Saxena A, Kumar RK, Gera RP, et al; Consensus guidelines on pediatric acute rheumatic fever and rheumatic heart disease. Indian Pediatr. 2008 Jul;45(7):565-73.
- Ralph AP, Fittock M, Schultz R, et al; Improvement in rheumatic fever and rheumatic heart disease management and prevention using a health centre-based continuous quality improvement approach. BMC Health Serv Res. 2013 Dec 18;13(1):525. doi: 10.1186/1472-6963-13-525.
- Cunningham MW; Streptococcus and rheumatic fever. Curr Opin Rheumatol. 2012 Jul;24(4):408-16. doi: 10.1097/BOR.0b013e32835461d3.
- Cilliers AM; Rheumatic fever and its management. BMJ. 2006 Dec 2;333(7579):1153-6.
- Webb RH, Grant C, Harnden A; Acute rheumatic fever. BMJ. 2015 Jul 14;351:h3443. doi: 10.1136/bmj.h3443.
- Engel ME, Stander R, Vogel J, et al; Genetic susceptibility to acute rheumatic fever: a systematic review and meta-analysis of twin studies. PLoS One. 2011;6(9):e25326. doi: 10.1371/journal.pone.0025326. Epub 2011 Sep 30.
- Kumar RK, Tandon R; Rheumatic fever & rheumatic heart disease: the last 50 years. Indian J Med Res. 2013 Apr;137(4):643-58.
- Lahiri S, Sanyahumbi A; Acute Rheumatic Fever. Pediatr Rev. 2021 May;42(5):221-232. doi: 10.1542/pir.2019-0288.
- Zuhlke LJ, Steer AC; Estimates of the global burden of rheumatic heart disease. Glob Heart. 2013 Sep;8(3):189-95. doi: 10.1016/j.gheart.2013.08.008. Epub 2013 Sep 26.
- Carapetis JR.; Rheumatic heart disease in developing countries. N Engl J Med. 2007;357:439–441
- Scarlet fever; NICE CKS, April 2022 (UK access only)
- Baker MG, Gurney J, Oliver J, et al; Risk Factors for Acute Rheumatic Fever: Literature Review and Protocol for a Case-Control Study in New Zealand. Int J Environ Res Public Health. 2019 Nov 15;16(22). pii: ijerph16224515. doi: 10.3390/ijerph16224515.
- Szczygielska I, Hernik E, Kolodziejczyk B, et al; Rheumatic fever - new diagnostic criteria. Reumatologia. 2018;56(1):37-41. doi: 10.5114/reum.2018.74748. Epub 2018 Feb 28.
- No authors listed; Guidelines for the diagnosis of rheumatic fever. Jones Criteria, 1992 update. Special Writing Group of the Committee on Rheumatic Fever, Endocarditis, and Kawasaki Disease of the Council on Cardiovascular Disease in the Young of the American Heart Association. JAMA. 1992 Oct 21;268(15):2069-73.
- The Australian guideline for prevention, diagnosis and management of acute rheumatic fever and rheumatic heart disease (2nd edition); RHD Australia, 2012 - updated 2022.
- Steer AC, Vidmar S, Ritika R, et al; Normal ranges of streptococcal antibody titers are similar whether streptococci are endemic to the setting or not. Clin Vaccine Immunol. 2009 Feb;16(2):172-5. doi: 10.1128/CVI.00291-08. Epub 2008 Dec 3.
- Ploutz M, Lu JC, Scheel J, et al; Handheld echocardiographic screening for rheumatic heart disease by non-experts. Heart. 2016 Jan;102(1):35-9. doi: 10.1136/heartjnl-2015-308236. Epub 2015 Oct 5.
- Ralph AP, Noonan S, Boardman C, et al; Prescribing for people with acute rheumatic fever. Aust Prescr. 2017 Apr;40(2):70-75. doi: 10.18773/austprescr.2017.011. Epub 2017 Apr 3.
- Kumar RK, Antunes MJ, Beaton A, et al; Contemporary Diagnosis and Management of Rheumatic Heart Disease: Implications for Closing the Gap: A Scientific Statement From the American Heart Association. Circulation. 2020 Nov 17;142(20):e337-e357. doi: 10.1161/CIR.0000000000000921. Epub 2020 Oct 19.
- Hashkes PJ, Tauber T, Somekh E, et al; Naproxen as an alternative to aspirin for the treatment of arthritis of rheumatic fever: a randomized trial. J Pediatr. 2003 Sep;143(3):399-401.
- Dean SL, Singer HS; Treatment of Sydenham's Chorea: A Review of the Current Evidence. Tremor Other Hyperkinet Mov (N Y). 2017 Jun 1;7:456. doi: 10.7916/D8W95GJ2. eCollection 2017.
- Gerber MA, Baltimore RS, Eaton CB, et al; Prevention of rheumatic fever and diagnosis and treatment of acute Streptococcal pharyngitis: a scientific statement from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the Council on Cardiovascular Disease in the Young, the Interdisciplinary Council on Functional Genomics and Translational Biology, and the Interdisciplinary Council on Quality of Care and Outcomes Research: endorsed by the American Academy of Pediatrics. Circulation. 2009 Mar 24;119(11):1541-51. doi: 10.1161/CIRCULATIONAHA.109.191959. Epub 2009 Feb 26.
- Good MF, Batzloff MR, Pandey M; Strategies in the development of vaccines to prevent infections with group A streptococcus. Hum Vaccin Immunother. 2013 Jun 28;9(11).
- Kadri SM; Diagnosis of Rheumatic Fever, Indian Journal for the Practising Doctor, 2005
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 29 Sept 2027
30 Sept 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free