Scarlet fever
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 16 Jan 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Scarlet fever article more useful, or one of our other health articles.
In this article:
Synonyms: scarlatina, scarlatinella
This disease is notifiable in the UK - see NOIDs article for more detail.
Continue reading below
What is scarlet fever?
Scarlet fever is an exotoxin-mediated disease arising from a specific bacterial infection by an erythrogenic toxin-producing strain of Streptococcus pyogenes - Group A beta-haemolytic streptococci (GpA BHS). Scarlet fever can follow infection at other sites, including wounds, burns and postnatally (for example, surgical scarlet fever and puerperal scarlet fever).
Pathophysiology
Back to contentsGpA BHS are normally found in the nasopharynx but can cause disease - for example, pharyngitis, skin infections and pneumonia.1
In most cases scarlet fever evolves from a tonsillar or pharyngeal infection but the rash is uncommonly seen in 'strep throats'.2
GpA BHS secrete a variety of haemolysing enzymes and toxins including the erythrogenic toxins causing the characteristic rash of scarlet fever.3
Person-to-person spread is mainly by respiratory droplets. The incubation is typically 2-5 days but ranges from 1-7 days.4
Patients are contagious both during the acute illness and the initial subclinical stage. Advice on exclusion from school is variable (see 'Prevention', below).
Continue reading below
How common is scarlet fever? (Epidemiology)5
Back to contentsEpidemics were common throughout Europe and the USA in the 18th and 19th centuries. Although scarlet fever nearly disappeared during the 20th century, several countries, including the UK, have recently experienced a re-emergence. However, the reason for these new outbreaks remains unclear.6 Scarlet fever is still one of the top ten causes of infectious deaths worldwide causing approximately 500,000 deaths annually.7
In the 1800s there were serious epidemics of scarlet fever. The death rate from scarlet fever then was as high as 150/100,000. Complications, case mortality and incidence have fallen dramatically because of antibiotics, enhanced immunity and improved socio-economic conditions.8 There are still sporadic outbreaks.9
The age profile has remained unchanged - 87% being children aged under 10 years, with a median age of 4 years.10 Scarlet fever is unusual under the age of 2 years because of maternal antibodies to the exotoxin and lack of prior sensitisation.
The infection rate increases with overcrowding and close contact. School populations have a higher incidence.11
Incidence decreases in adults as immunity develops.
Incidence is seasonal, most cases in the UK occurring in the winter and spring months.
In the last reported season (from 12 September 2022 to 7 May 2023), there were 55,872 notifications of scarlet fever in the UK. In the last comparable high season (from September 2017 to September 2018), there were 30,768 scarlet fever notifications overall across the year.12
Scarlet fever symptoms (presentation)5
Back to contentsIncubation is 2-4 days (range 1-7 days). Onset of the illness is usually sudden with fever. The rash follows 12-48 hours after the fever.
Often prodrome of sore throat, fever, headache, vomiting, abdominal pain, and myalgia. Tachycardia accompanies the fever.
Scarlatiniform rash appears on the second day of illness. The rash has the following characteristics:13
Appears typically on the neck first and also chest and scapular regions. It then affects the trunk and legs later.
The rash has a coarse texture like sandpaper. It is punctate on a diffuse erythematous base (that is, pin-point dark red spots on a general reddening of the skin).
Circumoral pallor is evident. The area around the mouth is unusually pale against the surrounding flushed face. This effect is more prominent than in other fevers.
The rash lasts for several days but after a few days of becoming generalised it may appear more prominent in skin creases, with confluent petechiae or lines (capillary fragility). This sign, seen particularly in the axillae and groin, is Pastia's sign and the lines are known as 'Pastia's lines'.
The skin may start to peel (desquamation) even during the febrile stage. This peeling, which often produces flakes of skin on the face, continues for several weeks. It also affects the tips of the fingers, the toes, axilla, groin and ears. It is a valuable sign if the patient has not been seen during the febrile phase.
Child with scarlet fever
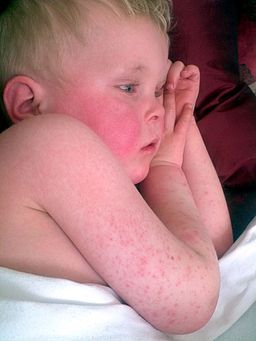
© By www.badobadop.co.uk (Own work) via Wikimedia Commons
The throat may have some of the typical features described:
There may be small haemorrhagic spots on the palate.
The tonsils are often red and oedematous.
The tonsils may be covered with pale exudate.
Accompanying tender cervical lymphadenopathy is typical.
The tongue has a characteristic appearance which develops during the illness:
Initially, during the first two days of the illness, patients may have a 'white strawberry tongue'. The tongue is covered by prominent red papillae seen through a white 'fur'.
After about two days the 'fur' is lost (desquamation). The tongue appears to look more raw and red but still has prominent papillae. This is called the 'raspberry tongue' or 'red strawberry tongue'.
Strawberry tongue
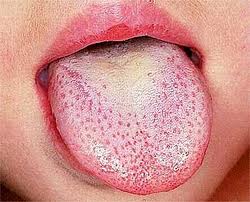
© By Afag Azizova (Own work) via Wikimedia Commons
Continue reading below
Differential diagnosis5
Back to contentsOther viral exanthema:
Other nonspecific viruses.
Exfoliative dermatitis.
Drug rashes.
Severe sunburn.
Plant allergies.
Investigations5
Back to contentsThe diagnosis is usually made clinically. However, investigations may be required in cases of diagnostic difficulty. These may include:
Throat swab and culture:4
This has 90% sensitivity for presence of GpA BHS. However, it is less specific, as there is a 10-15% carrier rate in healthy subjects.
It is important to take throat swabs correctly, avoiding the lips, tongue and buccal mucosa.
Swab tonsils, posterior pharynx and any exudate under good illumination.
Antigen detection kits:
Various kits are available for near patient testing. Rapid antigen tests (RATs) and 'strep tests' use latex agglutination. Enzyme-linked immunosorbent assays (ELISAs) are more expensive.
These are promoted to allow quick diagnosis and hence more appropriate administration of antibiotics. However, the cost and variable sensitivity and specificity are amongst some of the reasons that use is limited.
Streptococcal antibody tests:
Prove recent infection but are of no value in acute infection.
Have a value in patients with complications such as acute glomerulonephritis.
FBC:
A polymorphonuclear lymphocytosis is typical.
During the second week an eosinophilia may develop.
Scarlet fever treatment
Back to contentsThe aims of treatment are to:
Shorten the illness.
Prevent suppurative complications (such as peritonsillar abscess formation, mastoiditis, cellulitis and ethmoiditis).
Reduce the risk of spread to others.
Prevent progression to other complications. Unfortunately, however, although early use of penicillin may reduce rheumatic fever it does not prevent post-streptococcal glomerulonephritis.
Medical treatment 5
Antibiotics. Penicillin, or azithromycin (if penicillin-allergic) are the treatments of choice, given for a full 10 days. There are no documented penicillin-resistant GpA BHS infections. Amoxicillin can be used in children if compliance with penicillin is a problem.14
If there is high fever with marked systemic toxicity, the dose of antibiotic can be doubled or a second-line antibiotic (eg, a cephalosporin) used but in such circumstances specialist advice should be sought.
Rest and adequate fluids should be encouraged.
Ibuprofen or paracetamol should be offered to relieve symptoms.
Aspirin should be avoided in patients younger than 16 years.
Referral and other treatment
Recurrent infection would be an indication for ENT referral.
Difficulty swallowing may necessitate hospitalisation for intravenous fluids and antibiotics.
Management of complications may require hospitalisation.
The UK Health Security Agency recommends children can return to school after 24 hours of antibiotics.15 If antibiotic treatment is declined the patient should remain excluded until the symptoms have resolved.
Complications13
Back to contentsSigns of complications developing may be indicated by a persistent fever, increased throat pain or swelling.
Local spread:
Cervical lymphadenopathy.
Distant spread:4
Brain abscess.
Myocarditis (toxin-mediated).
Toxic shock-like syndrome (toxin-mediated).
Rare but feared, late complications include rheumatic fever (0.3%) or acute kidney injury (post-streptococcal glomerulonephritis). 16
Children who have recently had chickenpox are more likely to get a more serious infection during an outbreak of scarlet fever. Parents should be warned to watch out for cellulitis, high fever and arthritis.14
Minor late sequelae:
Beau's lines on nails.17
Telogen hair loss.
Prognosis5
Back to contentsScarlet fever follows a benign course in the vast majority of cases with rash and infection resolving in about a week. Any morbidity is likely to arise from suppurative complications, most often in untreated patients.
Historical
Back to contentsSecond in the historical order of classic exanthems identified:
Rubeola (measles).
Scarlet fever.
Rubella (German measles).
Dukes' disease (Coxsackievirus or echovirus) - no longer considered as a separate entity.
Fifth disease, or erythema infectosum (parvovirus B19).
Exanthem subitum or roseola infantum (human herpesvirus 6 (HHV-6)).
A disease previously confused with measles, the credit for a definitive, distinctive name must go to Thomas Sydenham (1624-1689), the English Hippocrates and the father of English medicine.18
Further reading and references
- Hurst JR, Brouwer S, Walker MJ, et al; Streptococcal superantigens and the return of scarlet fever. PLoS Pathog. 2021 Dec 30;17(12):e1010097. doi: 10.1371/journal.ppat.1010097. eCollection 2021 Dec.
- Alotaibi A, Binsaqr MA, Mutlaq MR, et al; Atypical Presentation of Scarlet Fever. Cureus. 2022 Dec 30;14(12):e33142. doi: 10.7759/cureus.33142. eCollection 2022 Dec.
- Smith A, Li A, Tolomeo O, et al; Mass antibiotic treatment for group A streptococcus outbreaks in two long-term care facilities. Emerg Infect Dis. 2003 Oct;9(10):1260-5.
- Choby BA; Diagnosis and treatment of streptococcal pharyngitis. Am Fam Physician. 2009 Mar 1;79(5):383-90.
- Todar K; Streptococcus pyogenes and Streptococcal Disease, Online Textbook of Bacteriology
- Scarlet fever: guidance and data; Public Health England
- Scarlet fever; NICE CKS, July 2023 (UK access only)
- No authors listed; Managing scarlet fever. Drug Ther Bull. 2017 Sep;55(9):102. doi: 10.1136/dtb.2017.8.0529.
- Brouwer S, Lacey JA, You Y, et al; Scarlet fever changes its spots. Lancet Infect Dis. 2019 Nov;19(11):1154-1155. doi: 10.1016/S1473-3099(19)30494-3. Epub 2019 Sep 10.
- Radikas R, Connolly C; Young patients in a young nation: scarlet fever in early nineteenth century rural New England. Pediatr Nurs. 2007 Jan-Feb;33(1):53-5.
- Feeney KT, Dowse GK, Keil AD, et al; Epidemiological features and control of an outbreak of scarlet fever in a Perth primary school. Commun Dis Intell. 2005;29(4):386-90.
- Group A streptococcal infections: update on seasonal activity, 2013/14; Health Protection Report, News Archives
- Wong S et al; Emerging Microbes and Infections, Nature.com, 2012
- UKHSA update on scarlet fever and invasive group A strep; Latest data from the UK Health Security Agency (UKHSA) on scarlet fever and invasive group A streptococcus cases. May 2023
- Basetti S, Hodgson J, Rawson TM, et al; Scarlet fever: a guide for general practitioners. London J Prim Care (Abingdon). 2017 Aug 11;9(5):77-79. doi: 10.1080/17571472.2017.1365677. eCollection 2017 Sep.
- Interim guidelines for the public health management of scarlet fever outbreaks in schools, nurseries and other childcare settings; Public Health England, 2014 (archived content)
- Guidelines for the public health management of scarlet fever outbreaks in schools, nurseries and other childcare settings; UK Health Security Agency (January 2023)
- Pardo S, Perera TB; Scarlet Fever.
- Zhou HY, Lu QH, Zhang LL, et al; Nail changes after scarlet fever. Pediatr Neonatol. 2023 Nov;64(6):692. doi: 10.1016/j.pedneo.2023.05.003. Epub 2023 Jun 26.
- Thomas Sydenham (1624-1689).; Thomas Sydenham (1624-1689). Can Med Assoc J. 1924 Oct;14(10):983-4.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Jan 2029
16 Jan 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free