Subconjunctival haemorrhage
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Suchita Shah, MRCGPLast updated 24 Jun 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Subconjunctival haemorrhage article more useful, or one of our other health articles.
In this article:
Continue reading below
What is a subconjunctival haemorrhage?
Subconjunctival haemorrhage results from bleeding of the conjunctival or episcleral blood vessels into the subconjunctival space. Causes may be traumatic or non-traumatic. Non-traumatic causes may be idiopathic or associated with other medical conditions.
Subconjunctival haemorrhage epidemiology1
Back to contentsIt is a common presentation.
The incidence of non-traumatic versus traumatic subconjunctival haemorrhage depends on the characteristics of the population.
One Taiwanese study reported a mean annual incidence of non-traumatic subconjunctival haemorrhage to be about 0.6%.2
It can occur at all ages but is more common with increasing age, probably as a result of increasing frequency of risk factors.3
There is little robust evidence about gender differences. One study reported that non-traumatic subconjunctival haemorrhage is more common in women than men.2 Another study reported that traumatic subconjunctival haemorrhage is more common in young men.4
It is common in the newborn.
Continue reading below
Subconjunctival haemorrhage causes (aetiology)1
Back to contentsThe cause of a subconjunctival haemorrhage is usually idiopathic.
Other causes include:
Valsalva manoeuvre (eg, coughing, sneezing, vomiting or straining; weight lifting; it has also been reported as a complication of bronchoscopy and endoscopy.5 )
Trauma - surgical or accidental (isolated or associated with retrobulbar haemorrhage or ruptured globe). This can include minor trauma, such as rubbing the eye, which the patient may not recall.
Contact lenses.6
Hypertension.
Bleeding disorders.
Diabetes mellitus.
Hyperlipidaemia.
Coronary heart disease.
Drugs - eg, warfarin, aspirin and other non-steroidal anti-inflammatory drugs (NSAIDs), steroids.
Normal sequelae of ocular surgery even if there is no conjunctival incision.
Febrile systemic infections.
Diseases which can present with subconjunctival haemorrhage include:7
Stevens-Johnson syndrome.
Haemochromatosis.
Pyogenic granuloma.
Telangiectasias.
Haemangiomas.
Subconjunctival haemorrhage symptoms
Back to contentsRed eye, usually unilateral.
It is usually asymptomatic, but there may be mild irritation of the eye.
The patient may not be aware of its presence but it has been reported to them by family or friends, who can find its appearance quite alarming.
Signs
The most common appearance is a flat, bright red patch anywhere in the conjunctiva with sharply defined edges and relatively normal conjunctiva surrounding it.
Overall, subconjunctival haemorrhages are most commonly found in the inferior conjunctiva, but traumatic subconjunctival haemorrhages are more common in the temporal area and tend to be more localised.8
The haemorrhage may spread and become green or yellow, like a bruise. Usually it disappears within two weeks.
Examination of the eye, including pupil responses and visual acuity, is otherwise normal.
It is worth noting that a haemorrhage without a posterior margin (ie extends posteriorly so that the whole extent of the haemorrhage cannot be seen) may be associated with an intracranial bleed or an orbital roof fracture (associated with a black eye) - the history should guide you as to whether to consider this or not.
Subconjunctival haemorrhage: "Red eye"
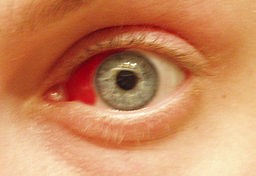
© Standardissue at en.wikipedia,CC BY-SA 3.0, via Wikimedia Commons
Continue reading below
Differential diagnosis
Back to contentsOther causes of acute red eye, including:
If it is a persistent haemorrhage (as opposed to the conjunctival injection seen in a red eye), consider rarer causes such as:
Other conjunctival neoplasms.
Investigations
Back to contentsCheck blood pressure.
No laboratory studies are indicated if it is an isolated problem.
If there is history of trauma, the patient may need referral to rule out more extensive eye injury.
In recurrent cases, investigation for an underlying bleeding disorder may be indicated.9
Subconjunctival haemorrhage treatment
Back to contentsMedical care is not required, unless there is an underlying disorder.
Artificial tears can be used four times per day for mild eye irritation.
Discourage elective use of aspirin products or NSAIDs.
Simultaneous bilateral haemorrhages, and persistent or unexplained recurrence, warrant a referral to the ophthalmologist.
Consider non-accidental injury in infants with bilateral isolated subconjunctival haemorrhages, especially if associated with facial petechiae.
Prognosis
Back to contentsSubconjunctival haemorrhage is a benign, self-limiting condition when not associated with systemic illness.
The prognosis is excellent.
There may be a small increased risk of stroke in the three years following a subconjunctival haemorrhage.10
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Tarlan B, Kiratli H; Subconjunctival hemorrhage: risk factors and potential indicators. Clin Ophthalmol. 2013;7:1163-70. doi: 10.2147/OPTH.S35062. Epub 2013 Jun 12.
- Hu DN, Mou CH, Chao SC, et al; Incidence of Non-Traumatic Subconjunctival Hemorrhage in a Nationwide Study in Taiwan from 2000 to 2011. PLoS One. 2015 Jul 16;10(7):e0132762. doi: 10.1371/journal.pone.0132762. eCollection 2015.
- Mimura T, Usui T, Yamagami S, et al; Recent causes of subconjunctival hemorrhage. Ophthalmologica. 2010;224(3):133-7. doi: 10.1159/000236038. Epub 2009 Sep 9.
- Sahinoglu-Keskek N, Cevher S, Ergin A; Analysis of subconjunctival hemorrhage. Pak J Med Sci. 2013 Jan;29(1):132-4. doi: 10.12669/pjms.291.2802.
- Lim HY, Puah SH, Ang LJ, et al; Subconjunctival haemorrhage from bronchoscopy: A case report. Respir Med Case Rep. 2015 Sep 3;16:97-100. doi: 10.1016/j.rmcr.2015.08.008. eCollection 2015.
- Mimura T, Yamagami S, Mori M, et al; Contact lens-induced subconjunctival hemorrhage. Am J Ophthalmol. 2010 Nov;150(5):656-665.e1. doi: 10.1016/j.ajo.2010.05.028. Epub 2010 Aug 14.
- Doshi R, Noohani T; Subconjunctival Hemorrhage. StatPearls, Jan 2023.
- Mimura T, Yamagami S, Usui T, et al; Location and extent of subconjunctival hemorrhage. Ophthalmologica. 2010;224(2):90-5. doi: 10.1159/000235798. Epub 2009 Aug 28.
- Cronau H, Kankanala RR, Mauger T; Diagnosis and management of red eye in primary care. Am Fam Physician. 2010 Jan 15;81(2):137-44.
- Wang TJ, Keller JJ, Sheu JJ, et al; A 3-year follow-up study on the risk of stroke among patients with conjunctival haemorrhage. Acta Ophthalmol. 2013 May;91(3):226-30. doi: 10.1111/j.1755-3768.2011.02359.x. Epub 2012 Mar 9.
Continue reading below
About the authorView full bio

Dr Suchita Shah, MRCGP
General Practitioner and Public Health Specialist
MRCGP, MPH, MA (Cantab), MPhil, BMBch (Oxon), DCH, DFSRH, DRCOG
Dr Suchita Shah is a GP, Population & Global Health specialist, writer, editor, and medical educator.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 2 Jun 2027
24 Jun 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free