Tinea capitis
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 23 Mar 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Fungal scalp infection article more useful, or one of our other health articles.
In this article:
Continue reading below
What is tinea capitis?
Tinea capitis, or scalp ringworm, is an exogenous infection caused by the dermatophytes Microsporum spp. and Trichophyton spp. These originate from a number of possible sources including other children or adults (anthropophilic), animals (zoophilic) or soil (geophilic).
See also the separate related Dermatophytosis (Tinea Infections) article.
How common is tinea capitis? (Epidemiology)1
Back to contentsThe reported prevalence in Europe is about 1.5% of the population.
Tinea capitis predominantly affects prepubertal children aged 6 months to 10-12 years.
The incidence in adults is low, but infection may be seen in people who are immunosuppressed.
It occurs most commonly in Afro-Caribbean children living in urban areas.
Risk factors1 2
Little is known about the risk factors for anthropophilic infection. Those cited include:
Age (most common in pre-pubescent children).
Overcrowding (households or schools).
Hairdressing salons.
Use of shared combs.
Ethnicity.
Continue reading below
Presentation of tinea capitis1 3
Back to contentsClinical diagnosis alone is unreliable. There is a wide range of clinical presentations and it can, particularly in mild cases, be very difficult to detect. Infection in the hair and scalp skin is associated with symptoms and signs of inflammation and hair loss (mainly in prepubertal children).
The main signs are scaling and hair loss but acute inflammation with erythema and pustule formation can occur.
There may be a 'black dot' appearance of the scalp, caused by broken-off, swollen hair stubs within the follicles, which is typically caused by Trichophyton tonsurans infection.
Tinea capitis
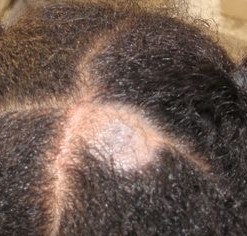
© Myself, CC BY-SA 4.0, via Wikimedia Commons
Laboratory methods should be used wherever possible to confirm the diagnosis.
The dermatophytes that cause tinea capitis can affect nails and skin in other parts of the body (only very rarely the feet or groins).
Children or adults who have neither signs nor symptoms of infection but from whose scalps causative fungi can be grown, are described as 'carriers'.
A kerion is an abscess caused by fungal infection, most often occurring on the scalp as a result of tinea capitis). It presents as a boggy pus-filled lump, often several centimetres in diameter, with marked inflammation and localised alopecia. There may be enlargement of the regional lymph nodes, and some people become systemically unwell with fevers and malaise. It may be followed by a widespread itchy eczema-like rash.4
Kerion on a child's scalp
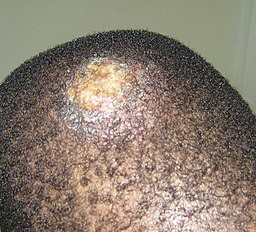
© Grook Da Oger, CC BY-SA 4.0, via Wikimedia Commons
Differential diagnosis3
Back to contentsId reaction (autoeczematisation).
Psoriasis (including plaque and pustular varieties).
Syphilis (including secondary syphilis).
Continue reading below
Investigations1 5
Back to contentsDefinitive diagnosis depends on an adequate amount of clinical material submitted for examination by direct microscopy and culture:
Scalp scrapings - including hairs and hair fragments - should, wherever possible, be used as the primary method of detection. At least 5 mm2 of skin flakes and hair should be obtained wherever possible.
This may be difficult (some children may not tolerate the plucking) and the second-line approach is to use sterile brushes (such as disposable toothbrushes).
Any treatment cream should be wiped off before sampling.
Do not refrigerate samples: keep at room temperature.
Cultures should be repeated after therapy.
Microscopy and culture:
Routine direct microscopy takes 24 hours (depending on the laboratory). Microscopic examination of the infected hairs may provide immediate confirmation of the diagnosis of ringworm and establishes whether the fungus is small-spore or large-spore, etc.
Culture may take several weeks. Culture provides precise identification of the species (for epidemiological purposes).
Conventional sampling of a kerion (pus-filled boggy mass which looks like a bacterial abscess) can be difficult. Negative results are not uncommon in these cases.
Include any treatment, animal contact and overseas travel in the details on the request form.
Scrape material directly on to special black cards provided by the laboratory.
Send samples for microscopy (results available within 24 hours) and culture (takes 2-3 weeks).
Management of tinea capitis1 5
Back to contentsIf suspected kerion, arrange urgent referral to a dermatology specialist.
Treatment of tinea capitis can otherwise be carried out in primary care and, for most cases, it is not necessary to refer children to a dermatologist.
Self-care management
Soften any surface crusts by applying moistened dressings to the affected areas.
Do not share towels, and ensure they are washed frequently.
Parents or carers should inspect the scalps of other children and household contacts regularly for clinical signs of infection.
If a household pet is suspected of being source of infection, it should be assessed and treated by a vet.
Adults
Offer treatment with an oral antifungal agent if there is:
A positive skin and hair sample microscopy or culture result.
A negative mycology result, but clinical features are very suggestive of infection.
A strong clinical suspicion of fungal scalp infection before mycology results are back, depending on clinical judgement.
Children
Offer treatment with an oral antifungal agent in primary care.
Oral antifungal agent if the diagnosis is certain. Once appropriate treatment is started, children should attend school or nursery as normal.
Oral antifungal treatment in primary care
Either oral griseofulvin (licensed) or oral terbinafine (off-label) empirically until culture results are available.
If in an urban area, start treatment with terbinafine for four weeks.
If in a rural area, start treatment with griseofulvin for 4-8 weeks.
When the culture results are available:
If Trichophyton tonsurans, continue or switch to terbinafine.
If a Microsporum species, continue or switch to griseofulvin.
Consider itraconazole (off-label) for four weeks if griseofulvin is not tolerated or is contra-indicated.
Consider additional topical antifungal agent during initial oral antifungal treatment, to reduce the risk of transmission to other people, with either:
Selenium sulfide or ketoconazole shampoo for at least twice weekly for 2-4 weeks; or
An imidazole cream (in children less than 5 years of age) to be used daily for one week.
In persistent positive cases (often T. tonsurans and Microsporum spp.) - that is, when fungi can still be isolated at the completion of treatment but clinical signs have improved - the recommendation is to continue the treatment for another month.
Carriers
Do not generally need oral antifungals.
They are given a topical preparation such as selenium sulfide shampoo at least twice-weekly.
However, if there is heavy growth of dermatophytes from scalp brushes taken from children with clinically normal scalps, they should be treated with oral therapy as for infected cases.
Children in contact with tinea capitis
Should be examined very carefully for signs of infection (may be just a few visible broken hairs).
If infected hairs are seen and confirmed by mycological examination, the children should receive oral therapy.
Complications of tinea capitis1
Back to contentsSecondary bacterial infection.
Scarring alopecia.
Skin pigmentation changes.
Dermatophytid (id) reaction: reaction to the dermatophyte causing a disseminated itchy, papular or vesicular eruption, often affecting around the outer helix of the ear, but may also affect the trunk or limbs. May accompany the start of oral antifungal treatment, and may be mistaken for a widespread fungal infection.
Erythema nodosum may rarely be associated with fungal scalp infection.
Kerion.
Psychological impact (ridicule, bullying, isolation, emotional disturbance, family disruption).
Prognosis1
Back to contentsThere is only very limited evidence for any detailed account for the prognosis of fungal scalp infection.
Continuous shedding of fungal spores may last several months even with active treatment. Keeping patients with tinea capitis out of school is impractical.
The treatments are very effective. However, treatment failure can occur because of:
Re-infection.
Relative insensitivity of the organism.
Poor absorption of the medication.
Poor compliance (the long courses of treatment).
Prevention
Back to contentsAsymptomatic carriers should be detected and treated. Increased surveillance in schools would be helpful.6 Spread should be prevented (avoid sharing of toys or other personal objects, such as combs and hairbrushes, with siblings and playmates of patients).
Further reading and references
- Kovitwanichkanont T, Chong AH; Superficial fungal infections. Aust J Gen Pract. 2019 Oct;48(10):706-711. doi: 10.31128/AJGP-05-19-4930.
- Hay RJ; Tinea Capitis: Current Status. Mycopathologia. 2017 Feb;182(1-2):87-93. doi: 10.1007/s11046-016-0058-8. Epub 2016 Sep 6.
- Fungal skin infection - scalp; NICE CKS, July 2022 (UK access only)
- Michaels BD, Del Rosso JQ; Tinea capitis in infants: recognition, evaluation, and management suggestions. J Clin Aesthet Dermatol. 2012 Feb;5(2):49-59.
- Guidelines for the management of tinea capitis 2014; British Association of Dermatologists (Sept 2014)
- Kerion; DermNet.
- Fungal Skin and Nail Infections: Diagnosis and Laboratory Investigation - Quick Reference Guide for Primary Care; GOV.UK, 2017
- Ginter-Hanselmayer G, Weger W, Ilkit M, et al; Epidemiology of tinea capitis in Europe: current state and changing patterns. Mycoses. 2007;50 Suppl 2:6-13.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 21 Mar 2028
23 Mar 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free