Ménière's disease
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 17 Nov 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:TinnitusAcoustic neuroma
Ménière's disease typically causes attacks of dizziness with a spinning sensation (vertigo), hearing loss and noises in the ear (tinnitus). The attacks can vary in severity and in how often they occur. You may develop permanent hearing loss and/or permanent tinnitus in some cases.
There is no cure but treatment can help to ease and prevent symptoms. If you are a driver, you must stop driving if Ménière's disease is diagnosed. The Driver and Vehicle Licensing Agency (DVLA) will permit driving again if there is good control of symptoms.
In this article:
Video picks for Hearing problems
Continue reading below
What is Ménière's disease?
Ménière's disease is a condition of the inner ear. It causes problems with balance and hearing. Ménière's disease is named after a French doctor called Prosper Ménière who first described the disease in the 1860s.
About 1 in a 1,000 people develop Ménière's disease. It can affect anyone at any age but it most commonly begins between the ages of 40 and 60. Generally, this condition starts in one ear only. The other ear is also affected at some stage in about 4 in 10 cases.
Ménière's diseases symptoms
Back to contentsShort-term symptoms
Ménière's disease typically comes in attacks (episodes) of the following symptoms:
Dulled hearing in the affected ear(s). The degree of hearing loss varies.
Vertigo. This is dizziness with a spinning sensation. It can be quite severe and make you feel sick or be sick (vomit). Vertigo can develop with little or no warning. You may feel very dizzy and ill. You may need to go to bed until it passes.
Tinnitus. This is a noise such as a ringing, roaring or buzzing which you can hear from inside the affected ear.
Ear pressure. You may have a sense of fullness or pressure inside the ear.
Loud noises may seem unpleasant and distorted.
How long does an attack last?
An attack of Ménière's disease may last from 20 minutes to several hours. The average is 2-4 hours. Many people feel quite sleepy after an attack. Slight unsteadiness may last a day or so after an attack - sometimes longer.
The symptoms can vary from person to person and from time to time in the same person. A typical attack is of vertigo, hearing loss and tinnitus, which lasts a few hours. However, some people only have the vertigo without the hearing loss. Attacks of hearing loss without vertigo are uncommon. Some people just have slight vertigo during an attack. Others are severely affected and vomit for several hours.
Attacks may be frequent, or occur only every few months or longer. Sometimes they come in clusters of several attacks in quick succession. For example, attacks may occur every couple of days for a week or so. Some attacks may be so close together that it may seem that one attack lasts for several days. On average, there may be 6-11 clusters a year.
At the start, symptoms may occur on one side only but as the years go by some people have symptoms on both sides.
An uncommon symptom is to have sudden unexplained falls (drop attacks). These are falls without losing consciousness. Drop attacks last just a short time with little associated vertigo. They occur in about 1 in 25 people with Ménière's disease. So, although uncommon, drop attacks can be alarming and potentially dangerous if, for example, the person is climbing up a ladder or driving when one occurs.
There may be long periods of time (months or years) between attacks (or clusters of attacks) when there are no symptoms. In about 7 in 10 people with Ménière's disease, the attacks stop altogether within 5-10 years of starting.
Long-term symptoms
If permanent symptoms develop, they usually take months or years to develop.
Hearing loss. During each attack the hearing loss is temporary at first. In the early stages of the disease the hearing usually reverts back to normal when an attack is over. In time, some permanent hearing loss may develop. In some people this becomes worse and leads to deafness in the affected ear.
Tinnitus. Like hearing loss, tinnitus is often temporary at first during each attack. Again, like hearing loss, it eventually becomes permanent in some cases.
Some people report fatigue and a sense of imbalance following an attack of vertigo, which can last some time. Some people have reported that these symptoms have become permanent. However, whether these symptoms are an actual feature of Ménière's disease is debatable.
Continue reading below
What causes Ménière's disease?
Back to contentsIt is thought to be caused by slight changes and damage within the inner ear.
The inner ear includes the cochlea and semicircular canals. These are small shell-like structures in which there is a system of narrow fluid-filled channels called the labyrinth. The semicircular canals sense movement of the head and help to control balance and posture.
The cochlea is concerned with hearing. Messages of balance and sound are sent down nerves (the vestibular nerve and the cochlear nerve) to the brain.
Inner ear diagram
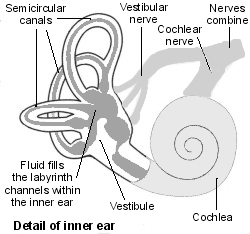
Cross-section of the ear
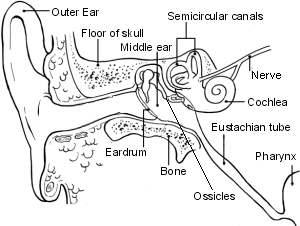
It is thought that a build-up of fluid (called endolymph) in the labyrinth from time to time causes the symptoms. The build-up of fluid may increase the pressure and cause swelling of the labyrinth. Also, fluid may leak between different parts of the labyrinth. These effects may cause the inner ear to send abnormal messages to the brain, which causes the dizziness and being sick (vomiting).
An increased pressure of fluid on the hearing cells (called 'hair cells') which line the labyrinth is probably why they do not work so well; this leads to dulled hearing. As the pressure eases, the cells work better again, and hearing returns to normal. However, repeated bouts of increased pressure may eventually damage the hearing cells. This is why hearing loss may become permanent.
What causes fluid to build up in the labyrinth?
It is not clear why a build-up of fluid occurs in the labyrinth. There may be some fault where the amount of fluid made is more than the amount drained. A variety of factors may cause this. For example, slight abnormalities of the bones around the middle ear may be a factor.
Inheritance may play some part. (About 8 in 100 close relatives of affected people develop Ménière's disease compared with 1 in 1,000 of the general population.) Other theories include viral infections of the ear, salt imbalance in the labyrinth fluid, diet and a faulty immune system.
Note: side-effects from some medicines can cause symptoms similar to Ménière's disease, or make symptoms of Ménière's disease worse. For example, some anticonvulsants, antidepressants, antihistamines, antipsychotics and sedatives. Tell your doctor if you think that a medicine that you are taking may be causing symptoms, or making them worse.
How is Ménière's disease diagnosed?
Back to contentsAlthough the diagnosis is usually based on the typical symptoms, a hearing test (audiometry) is often performed. Typically, it shows low frequency loss in one ear. Ideally, it is best performed during an attack. However, this is often impractical as attacks usually come out of the blue and can make you feel ill.
The diagnosis may only become clear over time as the typical pattern of recurring attacks develops.
Continue reading below
Conditions similar to Ménière's disease
Back to contentsOther conditions can cause similar symptoms; such as tinnitus, dizziness and vertigo, to Ménière's disease. For example:
Injury to the ear.
Tumours in the inner ear.
Nerve damage.
However, Ménière's disease is the likely cause if the symptoms are intermittent (that is, they come and go as attacks). Ear tests and scans may be advised in some cases to rule out other conditions. In particular, a scan will normally be needed if you have persistent symptoms of vertigo and/or hearing loss.
Ménière's disease treatment
Back to contentsThere is no cure for Ménière's disease but symptoms can be helped. Understanding the cause of the symptoms is often helpful in itself.
Treating attacks of vertigo
A short course of a medicine such as prochlorperazine or cinnarizine may ease dizziness and being sick (vomiting) when attacks of these symptoms occur. These medicines work by calming the nerve messages which are sent from the ear to the brain.
Many people have a warning feeling (an aura) just before an attack begins. If possible, medicine should be taken at this stage to prevent the attack from becoming worse or to lessen its severity. The medicine should be stopped when the attack of symptoms has gone.
Tablets may not be absorbed from the gut so well if there is vomiting. The absorption may be helped by:
Using a medicine which is absorbed from within the mouth and gums straight into the bloodstream; or
Using a medicine in suppository form; or
Using a soluble form of medicine which may be absorbed quickly into the bloodstream.
The aim is to get the medicine into the body as soon as possible after symptoms begin. If one type of medicine does not help, see a doctor, as another type may be more suitable.
Sometimes an injection is needed to help stop severe dizziness and vomiting. A short course of steroids may be given as a last resort if the attack does not settle.
Preventing attacks of vertigo
If you have mild or infrequent attacks then you may not need or want any treatment to prevent the attacks. You may just prefer to treat each attack, as it arises, with one of the medicines mentioned above.
If needed, treatments which can help to prevent attacks include the following:
Betahistine is a medicine that is thought to increase the blood flow around the inner ear. This may reduce the amount of fluid inside the labyrinth and prevent symptoms from developing.
Other medicines. These are sometimes tried on the advice of a specialist. For example, thiazide diuretics or beta-blockers may help in some cases.
Intratympanic gentamicin. This treatment involves injecting a drug called gentamicin through your eardrum into the middle ear. This gives a very high concentration of the drug next to the affected inner ear. This drug works by damaging the nerve endings that send signals of balance down the vestibular nerve. It is only considered if you are greatly troubled with vertigo and other treatments have not helped. It works quite well but occasionally it can cause deafness and is less likely than surgery to relieve vertigo.
Pressure pulse treatment (Meniett® device). This is a machine which generates a pulse of pressurised air into the ear canal and may be offered to you if your main problem is severe vertigo. The scientific evidence supporting this device is small, and further research is needed.
Surgery to the inner ear. There are various operations. Surgery may be suggested if you have severe or frequently recurring attacks of vertigo that have not been helped by other treatments. Operations that may be considered include:
Micropressure therapy. This is the treatment that involves the least amount of surgery. A small tube (a grommet) is inserted through your eardrum into the middle ear and air is blown at low pressure into the inner ear. This reduces the pressure in the ear. The effectiveness of this treatment is still being researched.
Saccus decompression. This is an operation to reduce the pressure of the fluid in the labyrinth. This is another form of treatment that is still being studied to see how well it works.
Vestibular nerve section. This means that the nerve of balance is cut - which stops the abnormal signals of balance being sent to the brain.
Labyrinthectomy. This means totally destroying the inner ear. The big disadvantage of this is that the hearing part of your ear is destroyed in addition to the balance part. So, you will be totally deaf in the operated ear.
Diet and lifestyle
There is little research evidence to prove that diet and lifestyle can help. However, some people claim their symptoms improve by one or more of the following:
A low-salt diet. This may help to reduce the fluid build-up in the inner ear.
Regular exercise and methods to combat stress.
Stopping smoking.
Food triggers. There seems to be a link between migraine and Ménière's disease. Food triggers are known to cause migraine attacks in some people. A similar trigger may contribute to some attacks of Ménière's disease. For example, cutting out alcohol and also avoiding caffeine (found in tea, coffee, cola and chocolate) may be worth trying.
Other treatments
For example:
If you develop permanent hearing loss, you may benefit from a hearing aid.
If loud sounds become distressing then an audiologist or hearing therapist can provide you with advice on compression hearing aids which may help to ease this symptom.
If you develop permanent noises in the ear (tinnitus) then various strategies may be advised. For example, an audiologist or hearing therapist may advise on sound therapy. This is often a CD or on an MP3 player which plays soothing and relaxing sounds, helping to distract you from the sound of tinnitus.
Some people have found coping strategies, relaxation training, counselling and other such techniques useful, particularly to combat tinnitus. See the separate leaflet called Tinnitus.
A physiotherapist may be involved if your balance becomes permanently affected (in severe cases). They might offer a programme of vestibular rehabilitation, which can help to make vertigo and balance better, although initially the symptoms can get worse.
Important safety points
Back to contentsIf you are prone to sudden attacks of dizziness with a spinning sensation (vertigo) with little or no warning then:
It is sensible always to carry some medication in case it is needed.
Avoid heights, ladders, etc. Do not go swimming alone.
Make your home safe in case you fall whilst dizzy. In particular, if you have vertigo you are likely to go to bed until it eases. The trip to the bathroom may pass open stairs. It may be sensible to block the top of the stairs in case you fall.
Driving and Ménière's disease
If you are a driver, you must stop driving if Ménière's disease is diagnosed and you must tell the Driver and Vehicle Licensing Agency (DVLA). This is because you may have sudden attacks of vertigo, or even drop attacks, with little warning.
The DVLA will permit driving again if there is good control of symptoms. See the DVLA guide for details (the link is in Further reading below).
What is the outlook (prognosis)?
Back to contentsThe way Ménière's disease affects people can vary greatly. At the outset of the disease, it is not possible to predict how badly it will affect an individual in the coming years. In many cases, months or years go by between attacks. In some cases the attacks are more frequent.
Some attacks are minor and don't last long. Some attacks can be very distressing with severe sickness (vomiting) and dizziness. However, treatments that can ease symptoms have improved in recent years.
There is a good chance that after a while (typically after 5-10 years) the attacks stop occurring altogether. However, some permanent hearing loss or permanent noises in the ear (tinnitus) may have developed in the affected ear or ears by this time. This may be only a minor degree of hearing loss but some people become deaf in the affected ear or ears.
Patient picks for Hearing problems

Ear, nose and throat
Perforated eardrum
A burst (perforated) eardrum is usually not serious and often heals in a few weeks on its own. Complications sometimes occur, such as hearing loss and infection in the middle ear. A small procedure to repair the eardrum may be an option if it does not heal by itself, especially if the perforation causes hearing loss.
by Dr Surangi Mendis, MRCGP

Ear, nose and throat
Cholesteatoma
Cholesteatoma is the name given to a collection of skin cells that form a pearly-white greasy-looking lump deep in the ear, usually at the top of the area behind the eardrum.
by Dr Doug McKechnie, MRCGP
Further reading and references
- Micropressure therapy for refractory Ménière's disease; NICE Interventional Procedure Guideline, April 2012
- Assessing fitness to drive: guide for medical professionals; Driver and Vehicle Licensing Agency
- Pullens B, Verschuur HP, van Benthem PP; Surgery for Meniere's disease. Cochrane Database Syst Rev. 2013 Feb 28;(2):CD005395. doi: 10.1002/14651858.CD005395.pub3.
- Wright T; Meniere's disease. BMJ Clin Evid. 2015 Nov 5;2015. pii: 0505.
- Meniere's disease; NICE CKS, March 2023 (UK access only)
- Tinnitus: assessment and management; NICE Guidance (March 2020)
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 16 Nov 2027
17 Nov 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.