Achalasia
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 20 Nov 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Achalasia is an uncommon condition that affects the muscles of the gullet (oesophagus). It usually causes difficulty in swallowing both food and fluids. There are different treatments available which can improve symptoms.
In this article:
Video picks for Swallowing difficulty
Continue reading below
What is achalasia?
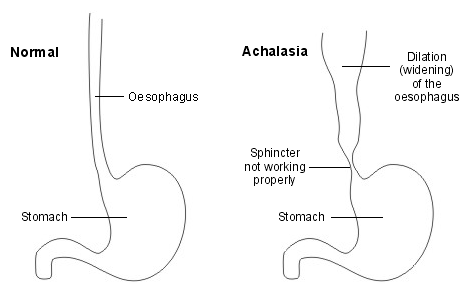
Achalasia affects both the muscles and the nerves of the oesophagus, especially initially the nerves that cause the sphincter between the oesophagus and stomach to relax.
The muscles do not contract properly so the rhythmic contraction of muscles, which allows food to pass down the oesophagus (peristalsis), does not occur correctly.
In addition, the sphincter does not relax properly so food cannot pass through into the stomach easily. This makes it difficult to swallow food properly.
The main part of the oesophagus then becomes enlarged and widened (dilated) with time.
How common is achalasia?
Back to contentsAchalasia is a very uncommon condition. Less than 1 in 100,000 people in the UK are diagnosed with it each year. It mainly affects adults aged between 20-40 years.
In most cases, no underlying cause can be found and the reason why the nerves and muscles in the gullet (oesophagus) do not work so well is not clear.
It is more common in people with Chagas' disease (an infectious disease more common in South America), Parkinson's disease and stomach cancer. However, the majority of people with these conditions do not have achalasia.
achalasia
Continue reading below
What are the symptoms of achalasia?
Back to contentsThe most common symptom is difficulty in swallowing (dysphagia) both food and liquids. It may feel as though some food is sticking in your chest after eating.
Other symptoms include:
Weigh loss.
Chest pains.
A heavy sensation on the chest.
A cough, which is sometimes worse at night.
Heartburn.
Regurgitation.
How is achalasia diagnosed?
Back to contentsMost people will have had achalasia for a length of time, even for years, before the diagnosis is made. Various tests may be advised if your doctor thinks you may have achalasia. These usually include one or more of the following:
Barium swallow
This is a specialised X-ray test. In this test, X-rays of your gullet (oesophagus) are taken after you swallow a liquid called barium, which shows up as white on the X-ray.
This test will show if your oesophagus has widened (dilated). It will also show if the barium stays in your oesophagus for longer than normal. See separate leaflet called Barium Swallow/Meal/Follow Through for more details.
Manometry
In this test, the pressure that is generated within your oesophagus when you swallow is monitored. During this test, a thin tube is placed through your nose, down the back of your throat and into your oesophagus. This test can often detect earlier changes than a barium swallow can.
Gastroscopy - sometimes called endoscopy
A gastroscope (endoscope) is a thin, flexible telescope. It is passed through the mouth, into the oesophagus and down towards the stomach and the first section of the intestine (the duodenum).
The endoscope contains fibre-optic channels which allow light to shine down so the doctor or nurse can see inside your oesophagus, stomach and duodenum. See separate leaflet called Gastroscopy (Endoscopy) for more details.
Continue reading below
What are the treatment options for achalasia?
Back to contentsThere are different treatments available. These include:
Medication
Various medicines can help to relax the sphincter at the lower end of the gullet (oesophagus). Examples include calcium-channel blockers (such as nifedipine) and nitrates (such as isosorbide dinitrate).
These work best when achalasia is first diagnosed. However, they usually only work in the short term and are most often prescribed for people who cannot have other forms of treatment.
Dilatation
This is a procedure in which the sphincter is made wider (dilated). This is done by using a balloon which is inflated to stretch the sphincter. This is done with the use of a gastroscope, to ensure the balloon is in the correct position.
Surgery
In some cases, the muscle fibres in the sphincter are divided (cut) during an operation. This is often done by keyhole surgery. This is usually very successful at easing the symptom of difficulty swallowing.
However, it may cause complications such as gastro-oesophageal reflux disease. This is a condition where the acid from the stomach comes up into the oesophagus. This can cause heartburn.
Botulinum toxin
This is another method of treating achalasia. Botulinum toxin acts as a muscle relaxant and is injected into the sphincter to weaken the muscle.
This is usually a safe treatment. However, it only works for a few months, so further injections are often necessary. It may be more suitable for people who are unable to have surgery.
Complications of achalasia
Back to contentsThe main complication of achalasia is weight loss. Another possible complication is that if food is brought up again (regurgitated), there is a risk that some food can enter the lungs. This can then lead to an infection in the lungs.
This type of infection is known as aspiration pneumonia. It is usually treated with antibiotic medicines but it can be more difficult to treat than other types of pneumonia.
There is also an increased risk of developing some inflammation of the lining of the gullet (oesophagus), due to the food and fluid which collect in the gullet and cause irritation. This is called oesophagitis.
There are also possible complications of some of the treatments. For example, widening (dilatation) of the sphincter can sometimes lead to a puncture (perforation) of the oesophagus. If this occurs, it will need an emergency operation to repair it.
There is a slightly increased risk of developing cancer of the oesophagus if it contains a large amount of food which does not pass into the stomach in the normal way. Your doctor will be able to discuss this with you in more detail.
What is the oesophagus?
Back to contentsThe gullet (oesophagus) contains muscles. These muscles contract in a rhythmic way to allow food to pass down the oesophagus. This is known as peristalsis.
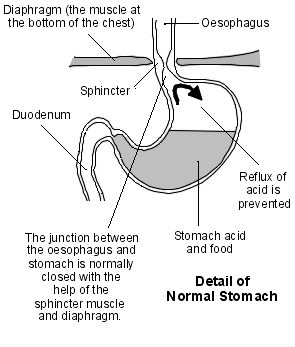
At the lower end of the oesophagus there is a ring of muscle called a sphincter. This sphincter relaxes to allow food to pass from the oesophagus into the stomach.
But, the sphincter contracts when no food is passing down, to stop food passing back up (refluxing) into the oesophagus.
Diagram of upper gut and nearby organs
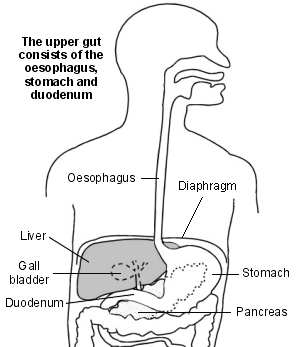
Diagram of normal stomach
Patient picks for Swallowing difficulty

Oral and dental care
Dysphagia
There are various causes of dysphagia (difficulty swallowing). See your doctor as soon as possible if you develop dysphagia. This is because a serious condition such as cancer of the gullet (oesophagus) can be the cause. As a general rule, the earlier a serious problem is diagnosed, the better the chance that treatment may improve the outlook (prognosis). This leaflet discusses the main causes of dysphagia.
by Dr Rachel Hudson, MRCGP

Oral and dental care
Globus sensation
Globus sensation is the feeling of having a lump in the throat when in fact there is nothing there. The sensation can come and go and does not interfere with eating and drinking. The exact cause of globus sensation is uncertain. Examination and investigations may be carried out to exclude any other underlying problem. Reassurance that there is no serious underlying problem may be all that is needed in terms of treatment.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Vaezi MF, Pandolfino JE, Yadlapati RH, et al; ACG Clinical Guidelines: Diagnosis and Management of Achalasia. Am J Gastroenterol. 2020 Sep;115(9):1393-1411. doi: 10.14309/ajg.0000000000000731.
- Oude Nijhuis RAB, Zaninotto G, Roman S, et al; European guidelines on achalasia: United European Gastroenterology and European Society of Neurogastroenterology and Motility recommendations. United European Gastroenterol J. 2020 Feb;8(1):13-33. doi: 10.1177/2050640620903213.
- Costantini M, Salvador R, Costantini A; Esophageal Achalasia: Pros and Cons of the Treatment Options. World J Surg. 2022 Jul;46(7):1554-1560. doi: 10.1007/s00268-022-06495-z. Epub 2022 Mar 3.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 18 Nov 2028
20 Nov 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.