Discoid eczema
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 16 Apr 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
In this series:Atopic eczemaEczema triggers and irritantsEmollients and eczema creamsTopical steroids for eczemaPompholyxEczema herpeticum
Eczema (dermatitis) is a term used to describe conditions where there is inflammation of skin. There are several types of eczema. Discoid eczema is one type which causes round or oval red patches of inflamed skin. The cause is uncertain. Treatment includes regular use of emollients to moisturise your skin, steroid creams to reduce inflammation and treatment of any infection of the affected skin.
In this article:
Video picks for Eczema
Continue reading below
What is discoid eczema?
Discoid eczema is a type of eczema that causes round- or oval-shaped red patches on the skin. Eczema is also called dermatitis. Dermatitis is a general term which means inflammation of the skin. Discoid refers to the disc shape of the eczema patches. Discoid eczema is sometimes called nummular eczema. Nummular literally means coin-shaped, another way of describing the shape of the patches of eczema.
Discoid eczema symptoms
Back to contentsThe most common symptom of discoid eczema is a patch of coin-shaped eczematous lesions on the body. These are:
Pinky-red, dry and scaly patches of skin.
Itchy patches of skin that are often worse at night.
Skin patches that burn or sting.
The skin between the discoid eczema patches looks normal except that, in general, many people with discoid eczema have dry skin.
Discoid eczema often starts on the legs. Some people will only have one or two patches of discoid eczema but others may develop many patches. Discoid eczema can occur anywhere on the body but it is relatively common for it to only be on the legs. It is uncommon on the face and scalp. It tends to become worse in the winter months in cold, dry climates. Sun tends to improve the symptoms in most people. Because of this discoid eczema can sometimes be mistaken for psoriasis.
Sometimes the skin patches can clear in the centre, just leaving a ring of eczema . If this happens, discoid eczema can sometimes be mistaken for ringworm. It is possible for patches of discoid eczema to become infected with germs (bacteria). Signs of infection include:
Increased redness.
Weeping or blistering of the skin patch.
Continue reading below
Discoid eczema image
Back to contentsDiscoid eczema (also called nummular eczema)
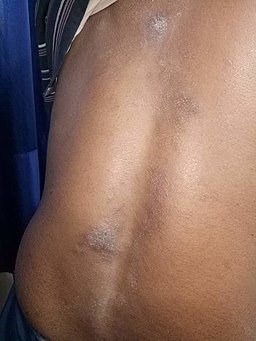
© Mohammad2018, CC BY-SA 4.0, via Wikimedia Commons
Discoid eczema causes
Back to contentsThe exact cause of discoid eczema is uncertain. However, most people with discoid eczema have generally dry skin. One theory is that the dry skin upsets the normal fatty layer within the outer layer of the skin (the epidermis) which usually helps to protect the skin. Because this protection is lost, special proteins that can cause allergy (allergens) can penetrate through the skin. This can lead to an allergic or irritant response in the skin, so leading to the patches of eczema. In fact, some doctors consider discoid eczema as a form of adult-onset atopic (allergic) dermatitis.
Sometimes certain medicines can trigger discoid eczema in some people. For example, medicines used to treat hepatitis C infection (called interferon and ribavirin). Insect bites or a minor skin injury can also trigger an outbreak of discoid eczema in some people.
Because the fatty, protective layer within the skin is lost, it is thought that some people with discoid eczema may also have an increased risk of developing contact dermatitis. Contact dermatitis is eczema that is caused by your skin reacting to a substance it has come into contact with. Such substances can include nickel in jewellery or belt buckles, cosmetics, preservatives in creams and ointments, additives to leather, etc. See the separate leaflet called Contact Dermatitis for more details.
Continue reading below
How common is discoid eczema?
Back to contentsDiscoid eczema is quite common and probably affects about 2 in 1,000 people. It seems to be more common in men than in women. Discoid eczema can affect men and women of any age but it most commonly affects people aged between 50 and 65 and women between the ages of 15 and 25. It is rare in children.
Discoid eczema diagnosis
Back to contentsIt is diagnosed by the typical skin appearance. If a doctor is uncertain about the diagnosis then they may need to exclude a fungal skin infection. For example, if there has been clearing of the skin rash in the centre (as described above), they may suggest scraping a few skin cells off a skin patch which can then be sent off to the laboratory to look for a fungal infection.
If your doctor feels that this may have contact dermatitis, they may suggest skin patch testing. In this procedure, tiny amounts of up to 25 or more substances are applied as small patches to the skin, usually on your upper back. They are fixed on with non-allergic tape. Some days later, the patches are removed by a dermatology specialist and the skin is examined to see if there is a reaction to any of the tested substances. See the separate leaflet called Patch Testing for Contact Dermatitis for more details.
Discoid eczema treatment
Back to contentsTreatment is aimed at:
Restoring fluid to your skin (called rehydration).
Treating the skin inflammation.
Also treating any infection that may be present.
Medicines are available to help relieve the symptoms and keep the condition under control.
Treatments include:
Skin rehydration treatment
This is done by using emollients. Emollients are often called moisturisers. They are lotions, creams, ointments and bath/shower additives that are applied to the skin to stop it becoming dry. Emollients should be used as soap substitutes when washing as regular soap tends to dry out the skin. After bathing/showering, emollients should be applied to the skin.
Regular use of emollients is the most important part of the day-to-day treatment for people with eczema, including discoid eczema. Emollients prevent skin from becoming dry and help to protect the skin from irritants. They should be used on all skin and not just the areas affected by discoid eczema. It is particularly important to carry on with daily moisturising of the skin even after a flare-up of discoid eczema has healed. This is to help reduce the chance of a further flare-up.
There are many types and brands of emollients, ranging from runny lotions to thick ointments. The difference between lotions, creams and ointments is the proportion of oil (lipid) to water. The lipid content is lowest in lotions, intermediate in creams and highest in ointments. The higher the lipid content, the greasier and stickier it feels and the shinier it looks on the skin. As a general rule, the higher the lipid content (the more greasy and thick the emollient), the better and longer it works but the messier it is to use. See the separate leaflet called Emollients and Eczema Creams for more details.
The use of petroleum jelly is sometimes recommended to keep the skin hydrated.
Topical steroids to reduce inflammation
A topical steroid is a steroid cream or ointment that is applied to the skin. In discoid eczema, topical steroids are applied to the skin patches to reduce inflammation. Ointments tend to be better than creams because they tend to hold water in the skin better and form a better protective barrier for the skin.
Steroid cream or ointment should not be used on normal skin and should only be used when there is a flare-up of the discoid eczema. This is because long-term steroid cream use can have some negative effects on skin, including thinning of your skin. See the separate leaflet called Topical Steroids for Eczema for more details.
Sometimes wet wrap treatments are used with a topical steroid to treat discoid eczema. The skin is made wet first with lukewarm water so that it is well hydrated. Then, a steroid ointment is applied to the affected areas of skin. Next, damp pyjamas or bandaging are used to seal in the steroid ointment for around one hour. These treatments would normally be recommended by a dermatologist if needed.
Very rarely, in severe cases, steroid tablets taken by mouth or given by injection may be needed to treat discoid eczema.
Note: when using both an emollient and a topical steroid, the emollient should be applied first. After applying an emollient, 10-15 minutes should be left before applying a topical steroid. That is, the emollient should be allowed to absorb before a steroid is applied. (The skin should be moist or slightly tacky but not slippery, when applying the steroid.)
Treatment of infection
Antibiotic medication might be needed if there is bacterial infection of discoid eczema patches. This may be in a cream or tablet form depending on the severity of the infection.
Treatment to reduce itching
Antihistamine tablets may help to reduce itching and may be particularly useful at night when trying to sleep. However, some antihistamines can cause drowsiness (even the next day), needing caution with driving or operating machinery.
Other treatments
Tar preparations may be helpful, especially in areas of skin that have been thickened and scaly for a long time.
Tacrolimus and pimecrolimus are other creams that may be used to help reduce inflammation in some people with discoid eczema. They may be considered in some people if steroid treatment is not working.
Because discoid eczema tends to improve in the sun, ultraviolet (UV) light treatment (phototherapy) can sometimes be helpful as a treatment. The UV radiation helps to reduce the inflammation in the skin. However, care should be taken, as exposure to UV radiation does carry its own risks of skin damage. This includes an increased risk of skin cancers. So, the risks of this type of treatment need to be weighed against the benefits. This type of treatment is usually used if discoid eczema is severe or other treatments have not worked.
Medicines that suppress the immune system may occasionally be needed to treat discoid eczema. They include medicines such as ciclosporin. Again, they are usually only used in severe cases of discoid eczema that are very difficult to treat and have not responded to other treatments.
Discoid eczema complications
Back to contentsAs mentioned above, bacterial infection of a patch of discoid eczema can occur and needs to be treated with antibiotics. Also, care should be taken to avoid scratching the itchy patches where possible as scarring can sometimes occur.
After a discoid eczema skin patch has healed, in many people there will be no residual signs. However, in some people there can be some permanent brown discolouration of the skin in the affected area. In others, the affected area of skin can become paler than the surrounding skin.
Outlook for discoid eczema
Back to contentsOnce discoid eczema has been successfully treated, a flare-up can occur again in the future. Therefore, it is important to keep the skin well hydrated with emollients to reduce the chance of future flare-ups.
Where possible, it is best to try to avoid anything that may have triggered the eczema, such as hot baths or irritating clothing. A humidifier in the room may help to reduce flare-ups. If flare-ups do occur, they often affect the same areas of skin as before.
Patient picks for Eczema

Skin, nail and hair health
Atopic eczema
Eczema is sometimes called dermatitis which means inflammation of the skin. There are different types of eczema, but most are chronic conditions. The most common type is atopic eczema. In this type of eczema there is a typical pattern of skin inflammation which causes the symptoms. Moisturisers (emollients) and steroid creams or ointments are the common treatments. About 2 in 3 children with atopic eczema grow out of it by their mid-teens.
by Dr Doug McKechnie, MRCGP

Skin, nail and hair health
Eczema triggers and irritants
In atopic eczema, avoiding certain causes (triggers) and irritants may help to prevent flare-ups of symptoms.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Fleming C, Parry E, Forsyth A, et al; Patch testing in discoid eczema. Contact Dermatitis. 1997 May;36(5):261-4.
- Leung AKC, Lam JM, Leong KF, et al; Nummular Eczema: An Updated Review. Recent Pat Inflamm Allergy Drug Discov. 2020;14(2):146-155. doi: 10.2174/1872213X14666200810152246.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Apr 2028
16 Apr 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.