Ringworm
Tinea corporis
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 19 May 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Fungal infectionsAntifungal medicationThrush in menAthlete's footYeast infectionFungal groin infection
Ringworm is a skin infection caused by a fungus. Treatment with an antifungal cream usually works well.
In this article:
Video picks for Skin infections
Continue reading below
What is ringworm?
Ringworm is a fungal skin infection caused by parasites that live on dead skin tissue. (It is not due to a worm as its name implies!) There are many types of fungal germs (fungi) and some can infect the skin, nails, and hair.
Fungal infections are also known as 'jock itch', 'tinea', 'tinea infections', 'dermatophyte infections' or 'dermatophytosis'. This leaflet just deals with ringworm of the skin (sometimes called tinea corporis).
See also the separate leaflets called Fungal Scalp Infection (Scalp Ringworm), Athlete's Foot (Tinea Pedis), Fungal Groin Infection (Tinea Cruris) and Fungal Nail Infections (Tinea Unguium).
How do you get ringworm?
Back to contentsGenerally speaking, ringworm and other fungal skin infections are contagious, but not especially so. It is possible to touch someone's skin if they've got ringworm or some other fungal infection and, as long as hands are washed afterwards, it's unlikely that it will be passed on.
Occasionally ringworm can be caught by the following means:
From person to person by touching a person who has the infection.
From touching items which have been in contact with an infected person, for example, towels, clothes, bed linen or chairs which have been used by somebody who has ringworm.
From animals. Some animals, such as dogs, cats, guinea pigs and cattle, have fungal infections on their skin. They can pass on the infection, especially to children. (Animals can be treated too. If it is suspected that a pet is the cause, advice should be sought from a vet.) Farm animals can also be a source. Touching a farm gate where infected animals pass through may be enough to infect skin.
From soil. Rarely, fungi can be present in soil and the infection can be caught from contact with the soil.
Continue reading below
What does ringworm look like?
Back to contentsTinea corporis
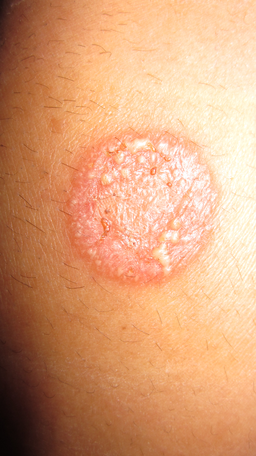
© Corina G., Public domain, via Wikimedia Commons
Ringworm symptoms
Back to contentsThe most common symptom of ringworm is the emergence of a small area of infected skin that tends to spread outwards. In most cases, ringworm develops into a rounded, red, inflamed patch of skin.
The outer edge is more inflamed and scaly than the paler centre. So, it often looks like a ring that becomes gradually larger - hence the name ringworm. Sometimes only one patch of infection occurs. Sometimes several patches of ringworm occur over different parts of the body.
The rash may be irritating, itchy and inflamed. If it's not itchy and annoying, it's very unlikely the ringworm is fungal.
Sometimes fungal skin infections and symptoms of ringworm look similar to other skin rashes, such as psoriasis, discoid eczema or granuloma annulare.
Continue reading below
Ringworm treatment
Back to contentsAntifungal creams for ringworm
An antifungal cream can be bought from pharmacies over the counter (OTC) or prescribed. There are various types and brands, which include terbinafine, clotrimazole, econazole, ketoconazole and miconazole. These are good at clearing fungal skin infections such as ringworm. There is no evidence that any one cream is better than any other one.
The cream should be applied to the affected areas for as long as advised. This varies between the different creams, so the instructions should be read carefully. Typically:
Clotrimazole: apply 2-3 times a day for at least four weeks.
Miconazole: apply twice a day and continue for 10 days after the skin is back to normal.
Econazole: apply twice a day until the skin is back to normal.
Ketoconazole: apply once or twice a day and continue for a few days after the skin is back to normal. Cannot be used for children.
Terbinafine: apply once or twice a day for one to two weeks. Cannot be used for children.
Antifungal steroid cream
For ringworm skin that is particularly inflamed, a doctor may prescribe an antifungal cream combined with a mild steroid cream. This would normally be used for no more than seven days and an antifungal cream might need to be used alone for a time afterwards.
The steroid reduces inflammation and may ease itch and redness quickly. However, the steroid does not kill the fungus and so a steroid cream alone should not be used; in fact, it will probably make the fungal infection worse.
Antifungal tablets for ringworm
An antifungal medicine taken by mouth is sometimes prescribed if the ringworm infection is widespread or severe. These include terbinafine, griseofulvin, or itraconazole tablets.
Not all ringworm treatments are suitable for everyone. People who may not be able take antifungal tablets include:
Women who are pregnant or breastfeeding.
People with certain liver diseases.
People at risk of heart failure.
People with long-standing lung disease.
Elderly people.
People taking other medication which may interact with antifungal tablets.
Children.
Risk factors
Back to contentsClose contact with an infected person or animal is the biggest risk factor. Ringworm is also more common in people living in a warm climate.
General advice and tips for ringworm
Keep the affected area clean and dry.
Do not share clothes or towels. Wash towels, sheets and clothes frequently. Clean the shower or bath well after use. Try not to scratch the rash, as this may spread the fungus to other areas of the body.
There is no need to stay off work or school once ringworm treatment has started.
Is is necessary to contact a doctor for ringworm?
Generally, no. A pharmacist can diagnose ringworm, so they should be consulted first and they will tell you whether or not GP advice is needed.
Advice from a GP should be sought if the ringworm has not improved after using the antifungal medicine prescribed by the pharmacist or in someone with a weakened immune system from other medications or treatments.
How to prevent ringworm
Back to contentsAvoid contact with infected people or animals. Avoid sharing towels, flannels or bedding.
Patient picks for Skin infections

Infections
Measles
Measles is an infection that mainly affects children but can occur at any age. It is rare in the UK, due to immunisation. The illness is unpleasant but most children fully recover. However, some children develop serious complications.
by Dr Toni Hazell, MRCGP

Infections
Eczema herpeticum
Eczema herpeticum is a rare and serious skin infection caused by one of the herpes viruses. It causes a blistery, painful skin rash. It most often affects children who have eczema. It is often confused with other skin infections. It should be treated as soon as possible to avoid complications. It can become very serious if not treated quickly enough. Treatment with an antiviral medicine usually works very well.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Andrews MD, Burns M; Common tinea infections in children. Am Fam Physician. 2008 May 15;77(10):1415-20.
- Rotta I, Ziegelmann PK, Otuki MF, et al; Efficacy of topical antifungals in the treatment of dermatophytosis: a mixed-treatment comparison meta-analysis involving 14 treatments. JAMA Dermatol. 2013 Mar;149(3):341-9. doi: 10.1001/jamadermatol.2013.1721.
- Malhotra S, Malhotra SK, Aggarwal Y; Tinea faciei caused by Trichophyton mentagrophytes in a 20-day-old neonate. Indian Dermatol Online J. 2015 Dec;6(Suppl 1):S43-6. doi: 10.4103/2229-5178.171045.
- Fungal skin infection - body and groin; NICE CKS, July 2022 (UK access only)
- Tinea Corporis: DermNetNZ
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
19 May 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.