Athlete's foot
Tinea pedis
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Caroline Wiggins, MRCGP Last updated 17 May 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Fungal infectionsAntifungal medicationThrush in menYeast infectionFungal groin infectionRingworm
Athlete's foot is a common skin infection caused by a fungus. The medical name for athlete's foot is "tinea pedis". Treatment with an antifungal cream usually works well. The tips given below may help to prevent athlete's foot coming back after it has been treated.
In this article:
Video picks for Fungal infections
What is athletes foot?
Continue reading below
What is athlete's foot?
Athlete's foot is a common fungal infection of the skin on the feet. Up to one in four people have athlete's foot at some point in their lives.
Fungal germs (fungi) often occur in small numbers on human skin where they usually do no harm. However, if conditions are right they can invade the skin, multiply and cause infection. The conditions fungi like best are warm, moist and airless areas of skin, such as between the toes.
What does athlete's foot look like?
Back to contentsTineas pedis - between toes
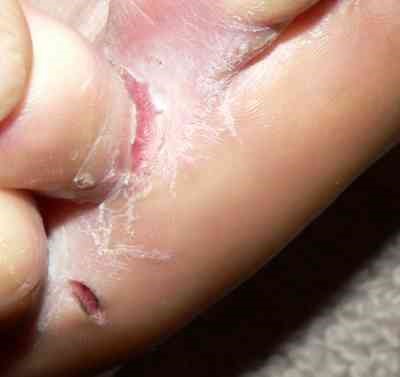
© User Falloonb on en.wikipedia, Public domain, via Wikimedia Commons
Continue reading below
Athlete's foot symptoms
Back to contentsCommon symptoms include:
Itchy, white or scaly rash between the toes or on the feet.
Cracked, sore skin between the toes or on the feet.
Painful splits (fissures) in between the toes.
Infected skin becoming flaky and falling off.
The rash may spread gradually along the toes if the athlete's foot is left untreated. In some cases it spreads to the soles or the nails.
What causes athlete's foot?
Back to contentsAthelete's foot is caused by a fungal infection. Anyone can get athlete's foot. It is more common in people who sweat more, or who wear shoes and socks which make their feet more sweaty. People with weakened immune systems are more likely to develop infections, including fungal infections. Athlete's foot can also be passed on from person to person.
Continue reading below
Is athlete's foot contagious?
Back to contentsYes, the fungus can spread from person to person. For example, infected flakes of skin can be shed and then come into contact with another person's skin. Sometimes the infection spreads to the skin on other parts of the body. These are usually the moist and airless parts of the skin such as the groin. The infection can also affect nails if the skin near the nail is infected. This can be treated. However, it takes several weeks of antifungal tablets to clear the infection from a nail. See the separate leaflet called Fungal Nail Infections (Tinea Unguium).
Fungi do not usually spread deeper than the skin. However, other germs (bacteria) may enter through the cracked skin of untreated athlete's foot. This can occasionally cause more serious infections.
How is athlete's foot diagnosed?
Back to contentsOften the infection is diagnosed by a doctor, nurse or pharmacist examining the skin and asking questions, without the need for any tests. If they are uncertain, the doctor or nurse may scrape a small sample of the flaking skin and send it to a laboratory to look for the fungus.
How to get rid of athlete's foot
Back to contentsAntifungal medication
You can buy topical antifungal medications from pharmacies, or get one on prescription. Topical means it is applied directly to the affected area, ie the skin of the feet.
There are various types and brands of antifungal cream - for example, terbinafine, clotrimazole, econazole, ketoconazole and miconazole. They are usually creams but can also be sprays, liquids or powders that will help in treating athlete's foot.
These treatments are all good at clearing fungal skin infections. There is no evidence that one is better than another. For children clotrimazole, econazole or miconazole should be used. Other options are undecenoic acid or tolnaftate, which are available over the counter.
Apply for as long as advised. This varies between the different treatments, so read the instructions carefully. Although the athlete's foot rash may seem to go quite quickly, you may need to apply the treatment for 1-2 weeks after the rash has gone. This is to clear the fungi completely from the skin, which will prevent the athlete's foot rash from returning.
Creams that have steroids in them, like hydrocortisone are not usually necessary - however, the hydrocortisone can help with the itching or any inflammation around the skin. These creams should not be used for more than 7 days.
If the problem does not get better after using the creams for the advised length of time it is sensible to consult your pharmacist or medical centre.
Antifungal tablets
An antifungal tablet is sometimes prescribed for adults with athlete's foot if the infection does not clear with a cream, or if the infection is severe. Tablets are also sometimes needed if the infection is in many places on the skin in addition to the toes. Tablets used include terbinafine, griseofulvin, or itraconazole. They are generally taken once a day but a course of eight weeks might be necessary.
See the separate leaflet called Antifungal Medicines.
Not all treatments are suitable for everyone. Women who are pregnant or breastfeeding and people with liver disease who suffer with athlete's foot may not be able to use antifungal tablets. Some people may be on other medication which interacts with antifungal tablets. Children are not usually prescribed antifungal tablets.
Management
You do not need to stay away from work, school or sports if you have athlete's foot. However, in communal areas, try to keep your feet covered until the rash is gone. Also, try not to touch the affected skin, as this may spread infection to other sites.
How to prevent athlete's foot
Back to contentsWash and dry your feet daily. Dry well between your toes and ensure your feet are completely dry before putting on socks or shoes.
Avoid sharing towels.
Do not wear the same shoes on consecutive days, in order to allow the shoes to dry out fully after wearing them. This reduces the chance of the fungus affecting your shoes.
Change your socks daily. Fungi may multiply in flakes of skin in unwashed socks. Cotton socks and leather footwear are probably better than nylon socks and plastic footwear, which increase sweating. Wearing sandals or flip flops to air your feet may help.
Ideally, not being barefooted in communal areas. This prevents the soles of your feet coming into contact with the ground, which may contain flakes of skin from other people.
Ideally, when at home, leave your shoes and socks off as much as possible to let the air get to your feet. However, this may not be practical for some people.
ash your feet daily, and dry the skin between your toes thoroughly after washing. This is perhaps the most important point. It is tempting to put socks on when your feet are not quite dry. The soggy skin between the toes is then ideal for fungi to grow.
Patient picks for Fungal infections

Infections
Fungal lung infections
A fungus is a tiny type of germ that usually doesn't cause any problems. They are all around us: you can only see them with a microscope. But in some situations, particularly if you have other serious illnesses, fungi (the plural of fungus) can infect your lungs. This can be very serious and requires specialist care.
by Dr Colin Tidy, MRCGP

Infections
Fungal infections
Fungi are a type of germ - they are all around us and don't usually cause any problems. Sometimes they can cause infections in the skin, hair and nails, which are treated with creams or tablets. Occasionally fungi (which is the plural of fungus) can cause more serious infections, particularly if you are already ill. This can happen if you are taking medicines that cause you to have a weakened immune system, such as chemotherapy or some medications used to treat inflammatory conditions - this will put you at a higher risk of a fungal infection.
by Dr Toni Hazell, MRCGP
Further reading and references
- Athletes foot; DermNet NZ
- Fungal skin infection - foot; NICE CKS, July 2022 (UK access only)
Continue reading below
About the author

Dr Caroline Wiggins, MRCGP
General Practitioner, Medical Author
MBBS Honours (with Distinction), MRCGP (2016), MSc.SEM (with Distinction), BSc (Hons)
Dr Caroline Wiggins is a GP locum currently in the South-West of England.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
17 May 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.