Hepatitis B
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni HazellLast updated 18 Dec 2023
Meets Patient’s editorial guidelines
In this series:HepatitisHepatitis AHepatitis CAutoimmune hepatitis
The hepatitis B germ (virus) can cause a short-term (acute) infection, which may or may not cause symptoms. Following an acute infection, a minority of infected adults develop a persistent infection called chronic hepatitis B.
Many people with chronic hepatitis B remain well, but can still pass on the virus to others. Some develop serious liver problems. The virus is mainly passed on by sexual contact, by sharing needles to inject drugs, and from mother to baby.
In this article:
Continue reading below
What is hepatitis B?
Hepatitis means inflammation of the liver. There are many causes of hepatitis. For example, drinking too much alcohol can cause hepatitis and it can also be caused by an autoimmune process, where the body's immune system acts against itself. As well as this, various drugs and chemicals can cause hepatitis. Finally, you can catch a virus that causes hepatitis.
One virus that causes hepatitis is called the hepatitis B virus. This leaflet is only about hepatitis B. Hepatitis A and Hepatitis C are caused by different viruses.
Hepatitis B is a virus which is carried in the bloodstream to the liver. It can then affect and damage your liver.
What does the liver do?
Human abdomen anatomy
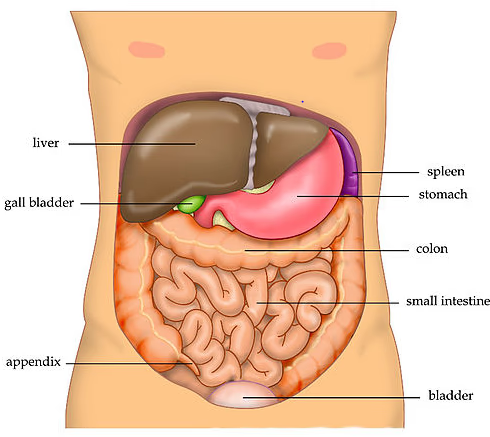
By Tvanbr - Ties van Brussel (Own work), via Wikimedia Commons
The liver is in the upper right part of the tummy (abdomen). It has many functions which include:
Storing fuel made from sugars (called glycogen) for the body. When required, glycogen is broken down into glucose which is released into the bloodstream.
Helping to process fats and proteins from digested food.
Making proteins that are essential for blood to clot (clotting factors).
Processing many medicines which you may take.
Helping to remove or process alcohol, poisons and toxins from the body.
Making bile which passes from the liver to the gut down the bile duct. Bile breaks down the fats in food so that they can be taken in (absorbed) from the bowel.
How common is hepatitis B?
The exact number of people infected is not known. In the UK, around 0.3% of people (3 people per 1000) are thought to have chronic persistent (chronic) hepatitis B infection and around 380 people catch it each year.
Worldwide, it is much more common and hepatitis B is the most common cause of hepatitis. For example, in parts of Asia and Africa nearly 1 person in 10 has chronic hepatitis B infection.
Continue reading below
How can you get hepatitis B?
Hepatitis B is a very infectious disease.
From mother to baby (sometimes called vertical transmission)
Worldwide, the most common way the germ (virus) is passed on is from an infected mother to her baby. This usually occurs during childbirth.
This is very common in some parts of the world where many people are infected with this virus (but is rare in the UK). All women in the UK are now tested for hepatitis B when they are pregnant.
From person to person (sometimes called horizontal transmission)
Blood and other bodily fluids, such as semen and vaginal secretions, contain the virus in infected people. The main ways in which people in the UK become infected include the following:
Having unprotected sex with an infected person. Even having oral sex can transmit hepatitis B. (Note: many people with hepatitis B do not realise that they are infected and can pass on the virus during sex.)
From infected blood. You only need a tiny amount of infected blood to come into contact with a cut or wound on your body to allow the virus to enter your bloodstream, multiply and cause infection. For example:
Sharing needles and/or any injecting equipment (for example, spoons, filters, water for injection) to inject drugs. Even a tiny amount of blood left on a needle from an infected person is enough to cause spread to others.
Some people who had a blood transfusion or another blood product several years ago were infected with hepatitis B. Now, all blood donated in the UK is checked for the hepatitis B virus (and for certain other infections). So, the risk of getting hepatitis B from a blood transfusion in the UK is now very small.
From 'needlestick' accidents where the needle was used on an infected person.
There is a small risk of contracting the virus from sharing toothbrushes, razors and other such items which may be contaminated with blood. The virus can actually live outside the body for more than one week.
From using equipment which is not sterile for dental work, medical procedures, tattooing, body piercing, etc.
A bite from an infected person, or if their blood spills on to a wound on your skin, or on to your eyes or into your mouth.
The virus is not passed on during normal social contact such as holding hands, hugging, kissing or sharing cups or crockery.
What are the symptoms and how does hepatitis B progress?
It is helpful to think of two phases of infection with the hepatitis B germ (virus).
A short-term (acute) phase when you are first infected
A persistent (chronic) phase when the virus remains long-term in some cases.
Acute hepatitis B infection
Symptoms of acute hepatitis may develop shortly after you first become infected with the virus (within 1-6 months, which is the incubation period).
Symptoms include:
Feeling sick (nausea).
Being sick (vomiting).
Tummy (abdominal) pains
Feeling generally unwell.
You may look yellow (become jaundiced).
Jaundice is due to a build-up of the chemical bilirubin which is made in the liver and spills into the blood in some liver conditions. With jaundice due to hepatitis your urine goes dark and your stools (faeces) may go pale.
Symptoms of acute hepatitis B infection usually go after a few weeks, as the immune system either clears the virus or brings it under control. Rarely, an acute severe (fulminant) hepatitis develops which is life-threatening.
However, in about half of cases, no symptoms, or only mild flu-like symptoms, develop in the acute phase. You may not even be aware that you have been infected with hepatitis B. In particular, babies who are infected from their mothers during childbirth usually have no symptoms at first.
Following the initial acute phase:
In more than 9 in 10 cases in adults, the virus is cleared from the body by the immune system within 3-6 months. In this situation you are no longer infectious and you are immune to further infection.
In around 4% of otherwise healthy adults, the virus remains long-term (chronic hepatitis B infection). This may occur whether or not you have symptoms in the acute phase. This number is higher if the adult has a problem with their immune system (is immunocompromised), if they have HIV or if they have kidney (renal) failure.
In up to 90% of babies infected from their mothers, who are not offered vaccination immediately after birth, the virus remains long-term.
So, in other words, there is a good chance of full recovery and clearing the virus for adults who become infected with hepatitis B. However, this is less likely for newborn babies who become infected.
Chronic hepatitis B infection
Of those people who develop chronic hepatitis B infection:
Up to 2 in 3 people remain well. You can have the virus in your body but develop no damage or problems to the liver or other organs. This is called being a carrier and is sometimes called chronic inactive hepatitis B. You may not know that you are infected and are a carrier. However, even if you have no symptoms, you can still pass on the virus to others. About 1 in 5 carriers eventually clear the virus from their body naturally, but this may be after several years.
Some people develop persistent liver inflammation (sometimes called chronic active hepatitis B). Symptoms include muscle aches, tiredness, feeling sick, lack of appetite, intolerance of alcohol, pains over the liver, jaundice and depression. Symptoms vary in severity and some people have liver inflammation without having any symptoms.
Some people develop cirrhosis. Cirrhosis is like a scarring of the liver, which can cause serious problems and liver failure when it is severe. Cirrhosis usually takes many years to develop after a person has been infected with hepatitis B. See the separate leaflet called Cirrhosis for more details.
A small number of people who develop cirrhosis then develop liver cancer after a further period of time.
Continue reading below
How is hepatitis B diagnosed?
A simple blood test can detect if you are infected with the hepatitis B germ (virus). This test detects a protein on the surface of the virus called hepatitis B surface antigen (HbsAg).
If you are found to be infected (if you are HBsAg-positive) then other tests may be advised to check on the severity of infection, liver inflammation and damage to the liver.
For example:
A blood test can detect various parts of the virus. This can assess how active the virus is (if it is multiplying rapidly which indicates that it is more likely to cause liver damage).
Blood tests called liver function tests. These measure the activity of chemicals (enzymes) and other substances made in the liver. This gives a general guide as to whether the liver is inflamed, and how well it is working.
A small sample (biopsy) of the liver may be taken to look at under the microscope. This can show the extent of any inflammation and scarring of the liver (cirrhosis).
A blood test can also be performed to show if you have immunity to hepatitis B.
Other tests may be done if cirrhosis or other complications develop.
There are other specialised blood tests being developed which assess the development and severity of cirrhosis.
What is the treatment for hepatitis B?
Treatment for the short-term (acute) phase
No treatment can clear the germ (virus) from the body. If you develop symptoms when first infected, treatment aims to help ease symptoms until they go - for example, drinking plenty of water to avoid lack of fluid in the body (dehydration).
Rarely, a severe hepatitis develops which may need hospital care. No treatment can prevent acute hepatitis B from becoming persistent (chronic).
Treatment for chronic infection
Treatment for hepatitis B does not cure hepatitis B but works to delay or even to prevent complications from developing, like liver damage and 'scarring' of the liver (cirrhosis).
People with chronic hepatitis B usually need treatment to stop or to reduce the activity of the virus, so limiting liver damage. A liver specialist will usually advise on when treatment may be beneficial. There are two types of treatment currently given:
Interferon. This medicine is similar to a substance produced in your body, which is also called interferon. It works to fight infections by boosting your immune system. Interferon is usually given as an injection each week.
Antiviral medicines. These work by stopping the hepatitis B virus from multiplying in the body. They include lamivudine, adefovir, tenofovir, and entecavir. Your doctor will discuss these in more detail with you, as the medicine used can vary between people. A combination of antiviral medicines is sometimes used.
Treatment with medicines is usually continued for many years.
Possible side-effects from hepatitis B medicines
Side-effects with these medicines can occur. You will be monitored regularly while you are taking treatment, which includes blood tests. Some people need to change their medicines, or take a lower strength, if they have troublesome side-effects.
Also, in some people, resistance can develop to their treatment medicine, which means that it does not work so well. If this happens then it is likely you will have to change the medicine you take.
The treatment of hepatitis B is a developing area of medicine. New medicines continue to be developed and the information above is very general.
There are some newer medicines that have been introduced in the last few years that show promise to improve the outlook. The specialist who knows your case can give more accurate information about the outlook for your particular situation.
Liver transplant
For some people with advanced 'scarring' of the liver (cirrhosis), liver transplantation may be an option. Although this is a major operation, the outlook following a liver transplant can be very good. However, the new liver may also eventually become damaged by the persisting (chronic) hepatitis B infection.
Diet and alcohol
Most people with persistent (chronic) hepatitis B will be advised to eat a normal healthy balanced diet. Ideally, anybody with inflammation of the liver should not drink alcohol. If you already have liver inflammation, alcohol increases the risk and speed of developing 'scarring' of the liver (cirrhosis).
Can hepatitis B be prevented?
Immunisation
A vaccine is available to protect against hepatitis B. This should be offered to anyone who is at increased risk of being infected with the hepatitis B germ (virus).
For example, sexual and household contacts of someone infected with hepatitis B. See the separate leaflet called Hepatitis B Immunisation for more details.
Post-exposure prevention
If you are not immunised and have been exposed to the virus, you should see a doctor immediately. (For example, if you are a healthcare worker and you have a 'needlestick' injury.)
You can be given an injection of antibodies called immunoglobulin as well as starting a course of immunisation. This may prevent infection from developing.
Preventing infection in newborn babies at risk
All pregnant women in the UK are offered a hepatitis B blood test. If the mother is infected, her baby is immunised straight after birth - if the mother's blood test shows that her baby is at particularly high risk of catching hepatitis B from her, then the baby may also be given an injection of immunoglobulins (antibodies) against hepatitis B.
With this treatment there is a good chance of preventing infection developing in the baby.
If I am infected, how can I prevent passing on the virus to others?
If you have a current hepatitis B infection you should:
Avoid having sex with anyone (especially any sex without using a condom) until they have been fully immunised and checked with a blood test to see that the immunisation has worked.
Not share any injecting equipment such as needles, syringes, etc.
Not donate blood or semen or carry a donor card.
Not share razors, toothbrushes, etc, that may be contaminated with blood.
Cover any cuts or wounds with a dressing.
Make sure that, if any of your blood spills on to the floor or other surfaces following an accident, it is cleaned away with bleach.
Further reading and references
- EASL Clinical Practice Guidelines: Management of chronic hepatitis B virus infection; European Association for the Study of the Liver (EASL), 2018
- 2017 interim update of the 2015 BASHH National Guidelines for the Management of the Viral Hepatitides; British Association of Sexual Health and HIV, 2017.
- Hepatitis B; NICE CKS, February 2023 (UK access only)
- ; EASL 2017 Clinical Practice Guidelines on the management of hepatitis B virus infection. J Hepatol. 2017 Aug;67(2):370-398. doi: 10.1016/j.jhep.2017.03.021. Epub 2017 Apr 18.
Article History
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 16 Dec 2028
18 Dec 2023 | Latest version

Feeling unwell?
Assess your symptoms online for free