Nephrotic syndrome
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Surangi Mendis, MRCGPLast updated 11 Sept 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:GlomerulonephritisIgA nephropathyDMSA scanKidney biopsy
Nephrotic syndrome is a condition where the 'filters' in the kidney become 'leaky' and large amounts of protein leak from the blood into the urine. The main symptom is fluid retention (oedema) which is mainly due to the low protein level in the blood. Various diseases can cause nephrotic syndrome, some more serious than others. Treatment and outcome (prognosis) vary, depending on the cause. The most common cause in children, minimal change disease, usually responds very well to treatment.
At a glance
Nephrotic syndrome is a group of symptoms caused by leaky kidney filters.
It can result in a lot of protein leaking into the urine.
This leads to low protein levels in the blood and fluid retention, often causing swelling.
It can cause tiredness, frothy urine, and increase the risk of infections or blood clots.
Treatment involves managing symptoms like swelling and addressing the underlying cause.
In this article:
Video picks for Kidney problems
Continue reading below
What is nephrotic syndrome?
Nephrotic syndrome is not a single disease - it is a syndrome. A syndrome is a set of symptoms and signs that tend to occur together and which can be caused by one or more different diseases. Nephrotic syndrome can be caused by many different diseases, some more serious than others.
Cross-section diagram of the urinary tract
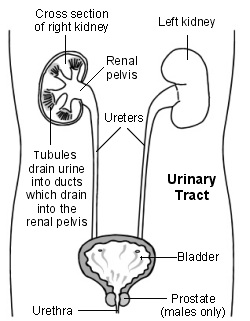
The main feature of nephrotic syndrome is that the kidneys leak a lot of protein. Normally, urine contains virtually no protein. In nephrotic syndrome the urine contains large amounts of protein. Filters in the kidneys (the glomeruli) become 'leaky' and protein, instead of remaining in the blood, leaks out into the urine. Protein in the urine is called proteinuria.
The other key features of nephrotic syndrome are:
A low level of protein in the blood as a result of protein loss in the urine. Although there is a drop in many of the proteins normally found in the bloodstream, the main protein that leaks from the blood into the urine is called albumin. A low blood level of albumin is a main feature of nephrotic syndrome.
Fluid retention (oedema). This is a consequence of the low level of albumin in the bloodstream. Fluid becomes trapped in body tissues. Parts of the body, particularly the feet and ankles, appear puffy and swollen.
A high blood level of cholesterol and other fats (lipids). This is due to the change in the balance of various protein levels in the blood due to protein leakage.
Normal kidney function, at least initially. This means that the 'waste clearing' function of the kidneys is not affected - at least not at first. However, some of the conditions that cause nephrotic syndrome can progress to cause kidney disease.
Other typical symptoms and signs of nephrotic syndrome are discussed later.
What are the causes of nephrotic syndrome?
Back to contentsVarious diseases can affect the glomeruli and cause nephrotic syndrome. The following gives a brief description of the main ones:
Minimal change disease
'Minimal change' means there is virtually no change detectable in the glomeruli if a sample of kidney is looked at under a microscope. Although the glomeruli appear normal, there seems to be some minor change in the glomeruli that allows leakage of protein.
The cause of minimal change disease is not clear. It probably has something to do with a slight change in the immune system, or perhaps a reaction of parts of the immune system to some unidentified factor.
Minimal change disease causes about 9 in 10 cases of nephrotic syndrome in children under the age of 5 years. It causes about 1 in 5 cases of nephrotic syndrome in adults. It usually responds well to treatment with steroid medication taken by mouth and does not cause kidney failure in most cases.
Membranous nephropathy
This is sometimes called membranous nephritis or membranous glomerulonephritis. It is a common cause of nephrotic syndrome in adults. It is an uncommon cause in children.
In this condition there is some thickening of the membrane in the glomeruli (the 'filter' of the glomeruli) which makes the glomeruli 'leaky' to protein. The thickening can be seen under a microscope if a sample of kidney is taken for testing.
In many cases, the cause or reason for this change to occur in the glomeruli is not known. However, there are various conditions that can cause membranous nephropathy to develop. For example, an abnormal reaction of the immune system to some infections or medicines can cause this disease.
Focal segmental glomerulosclerosis (FSGS)
This is a condition where small scars (sclerosis) develop on some glomeruli. The cause is unknown in most cases. However, a reaction of the immune system to something, or to various different things, is thought to be the cause. FSGS accounts for up to 1 in 10 cases of nephrotic syndrome in children but a higher percentage of cases in adults.
Congenital nephrotic syndrome
This is a rare cause of nephrotic syndrome which affects children. 'Congenital' means it is present from birth. It is genetic (inherited due to a faulty gene) in most cases. Babies with this form of nephrotic syndrome usually develop symptoms within the first three months of life. It is usually hard to treat and most children eventually require dialysis (diversion of blood, often to a machine, to remove waste products) or a kidney transplant (replacement of a faulty kidney with a healthy one).
Other disorders of the glomeruli
There are various other uncommon kidney disorders, which primarily affect the glomeruli, that can result in nephrotic syndrome. For example, membranoproliferative glomerulonephritis, mesangial proliferative glomerulonephritis, fibrillary glomerulosclerosis, diffuse mesangial sclerosis, IgM mesangial nephropathy.
The cause of some of these conditions is not clear. However, some are probably caused by reactions of the immune system that cause damage to the glomeruli or nearby cells.
Other general conditions
A complication of some other more generalised conditions can cause damage to glomeruli, resulting in nephrotic syndrome. For example, nephrotic syndrome is a possible complication of diabetes, systemic lupus erythematosus (SLE), rheumatoid arthritis, polyarteritis nodosa, Henoch-Schönlein purpura, various infections, some cancers and amyloidosis. It can also occur as a side-effect of certain medicines and as a consequence of various poisons or toxins.
Continue reading below
What are the symptoms of nephrotic syndrome?
Back to contentsFluid retention (oedema) is a main symptom
Fluid retention occurs when fluid leaks out of blood vessels into the body tissues. This causes swelling and puffiness. The swelling is usually painless but the swollen tissues may feel tight. With children, the face is often affected first and the face becomes puffy. With adults, the ankles often become swollen at first (as gravity helps fluid to pool in the lower legs). As fluid retention becomes worse, the calves and then the thighs may become swollen.
In severe cases, the fluid retention can become extensive. Fluid may accumulate in the lower back, the arms, in the tummy (abdominal) cavity (where it is called ascites), genitals, or in the chest between the lungs and the chest wall (pleural effusion). Ascites can cause tummy pain and discomfort due to swelling of the abdomen. Pleural effusions may cause chest pain and breathlessness.
The main reason why fluid leaks out from the blood vessels and into the body's tissues with nephrotic syndrome is because of a low level of protein in the blood. As protein is lost from the body in the urine, the body makes more protein in the liver which passes into the bloodstream.
However, the amount made by the liver cannot keep up with the amount lost by the leaky kidneys and so the blood level of protein goes down. If the blood level of protein is low, then fluid tends to leak out of the blood vessels into the body tissues. Protein and other chemicals in the blood create an osmotic pressure which tends to pull fluid into the blood vessels. If the concentration of protein reduces, the osmotic pressure reduces and fluid leaks out.
Note: nephrotic syndrome is just one cause of fluid retention. There are other causes of fluid retention. For example, heart failure is the most common cause of fluid retention, especially in older people.
Other symptoms
The following symptoms may also develop due to nephrotic syndrome:
Urine that looks frothy.
Tiredness and a poor appetite.
Diarrhoea and/or being sick (vomiting) - especially in children.
If the nephrotic syndrome persists for a long time then wasting of the muscles may develop and the nails may look like they have white bands on them (called Muehrcke's lines).
Depending on the cause of the nephrotic syndrome, there may also be other symptoms. For example, if nephrotic syndrome has arisen as a complication of rheumatoid arthritis there may be a range of other symptoms caused by the arthritis. Some conditions of the kidney can cause high blood pressure (hypertension) and/or chronic kidney disease.
Tests of kidney function
Back to contentsDoctors can assess how well (or poorly) the kidneys are working with blood and urine tests.
'U&Es' is the abbreviation medical professionals use for urea and electrolytes. These are a group of blood tests to measure the levels of salts (such as sodium and potassium) in the blood, as well as the urea and creatinine levels, which show the kidney function as they are waste products.
The eGFR is a term doctors use. It stands for estimated glomerular filtration rate and is another measure of kidney function. The levels of protein and albumin (a type of protein) can also be measured with blood tests.
Urine can be tested for blood and protein with a 'dipstick' in clinic, or an exact measurement can be calculated by the laboratory. Other chemicals in urine can be measured and the urine is often examined under the microscope to see if it contains any abnormal cells or sediment.
Sometimes doctors refer to CKD. This stands for chronic kidney disease, which itself is a general term and can be caused by many different diseases or processes. The term 'chronic' mean the illness is persistent or long-lasting, and does not relate to how severe it is.
Continue reading below
What are the possible complications of nephrotic syndrome?
Back to contentsPossible complications from nephrotic syndrome itself
Complications can be caused by nephrotic syndrome itself due to the loss of normal proteins from the blood. These include:
An increased risk of developing infections. This is because antibodies can be lost in the urine. Antibodies are proteins that help to defend the body from infection. Any signs of infection (sore throat, high temperature (fever), etc) should be taken seriously and reported promptly to a doctor.
An increased risk of developing blood clots in the blood vessels (thrombosis). For example, a deep vein thrombosis (DVT) in a leg. This can cause pain, swelling and other complications. The reason for this is because there can be a change in the balance of proteins in the blood that protect against blood clots forming.
A high cholesterol level. If this persists long-term it is a risk factor for developing heart disease.
Increased risk of vitamin D deficiency which may lead to bone problems. This is due to loss of vitamin D-binding protein from the bloodstream.
Anaemia. This is due to loss of proteins that help to carry iron around in the bloodstream. Iron is needed to make red blood cells and to prevent anaemia.
Acute kidney injury. This may rarely occur from the nephrotic syndrome itself, or more commonly due to complications such as infections, or as an unintended result of treatment.
Depending on the duration and severity of the nephrotic syndrome, treatment may be advised to help prevent or reduce the risk of these possible complications.
Possible complications from the cause of the nephrotic syndrome
Various complications can arise from the underlying condition which has caused the nephrotic syndrome. For example:
One of the most common complications of kidney disorders is high blood pressure (hypertension).
Some kidney disorders lead to chronic kidney disease.
Some disorders (for example, diabetes, rheumatoid arthritis, etc) that cause nephrotic syndrome can have various other symptoms and complications.
Possible complications from treatment
Often, the treatment of nephrotic syndrome requires a course of steroid medicines or other medicines to suppress the immune system (see below). Some people develop side-effects and complications from these treatments, especially if the treatment requires high doses, or is needed for long periods.
Do I need any tests for nephrotic syndrome?
Back to contentsTo confirm nephrotic syndrome
A simple 'dipstick' test of the urine can confirm that it contains a lot of protein. Protein in the urine is not always due to nephrotic syndrome but is often a cause of underlying kidney disease. There are exceptions, such as protein in the urine caused by a urinary tract infection, exercise, or dehydration. The amount of protein lost can be measured by more detailed urine and blood tests.
An early morning urine sample is usually requested. A low blood level of albumin combined with a lot of protein found in the urine usually confirms that nephrotic syndrome is present.
Blood tests are also performed to check the function of the kidneys.
To find the cause of the nephrotic syndrome
A range of blood tests may be done to try to identify the cause of the nephrotic syndrome. A kidney biopsy may also be done. A kidney biopsy is a procedure which involves taking a small sample of tissue from a kidney. The sample is looked at under a microscope, or tested in other ways.
This is often the most important test to clarify the cause of the nephrotic syndrome in adults. However, in children a biopsy is usually only done in specific situations. This is because most cases in young children are due to minimal change disease. A trial of treatment is usually advised first and a biopsy done only if treatment does not work, although there are some exceptions to this general rule.
How is nephrotic syndrome treated?
Back to contentsTreatment of fluid retention (oedema)
'Water tablets' (diuretics) help to clear the body of excess fluid. Diuretics work by acting on the cells in the kidney tubules to make them pass out more water rather than reabsorbing water back into the bloodstream, so more urine is passed out. The excess fluid in the body's tissues then passes back into the bloodstream to keep the blood volume up to normal.
Limiting the amount of salt in the diet may also be advised to try to limit fluid retention. One way of trying to measure whether fluid is being retained (or to see if the diuretics are helping) is to weigh yourself regularly.
Treatment of high blood pressure (hypertension)
Many people with kidney disorders have high blood pressure. This is because the kidney makes chemicals involved in the control of blood pressure. If high blood pressure develops then treatment is usually advised to bring the blood pressure down. A medicine called an angiotensin-converting enzyme (ACE) inhibitor or an angiotensin-II receptor antagonist (AIIRA) - sometimes called an angiotensin receptor blocker (ARB) - is commonly used for this.
These medicines seem to have a protective effect on the kidneys and can reduce the amount of protein leaking. However, these medicines might not be suitable for everyone.
Treatment of the underlying cause
The exact treatment offered will depend on the underlying cause. For example, a course of steroid medication usually works well to stop the leak of protein from the kidneys in minimal change disease. In some cases, this is a one-off treatment and the disease does not return. In other cases of minimal change disease, the disease comes back (recurs) from time to time which needs repeated courses of steroid medication.
Steroids or other medicines called immunosuppressants may be used to reduce inflammation and abnormal immune responses in various diseases that cause nephrotic syndrome. In a small number of cases, steroids or immunosuppressant medications do not work or they stop working after a period of time. Dialysis or a kidney transplant may be required. The treatment options available for each situation are usually discussed on a case-by-case basis.
Can nephrotic syndrome be cured?
Back to contentsThere is no cure for nephrotic syndrome at present. The treatments described above are used to prevent the damage to the kidneys from getting worse and to manage symptoms.
Depending on the underlying cause, a course of steroid medication, or other therapy, may cause remission. Remission means that the signs and symptoms of the condition have gone, but there is still a chance it could return in the future. Remission is different from the term cure, which means that the condition will never occur again. However some people may recover from their first episode and never have another relapse. 25 - 30% of children with minimal change disease go into complete remission after the first episode. So they are considered to be 'cured' once they have been relapse-free for several years.
What is the outlook (prognosis)?
Back to contentsThe outlook depends on the cause. As mentioned, the most common cause of nephrotic syndrome in children (minimal change disease) usually responds well to treatment and generally has a good outlook. The outlook is less good with some other conditions. Those affected by nephrotic syndrome can discuss the outlook for their particular cause with their doctor.
Cross-section diagram of the urinary tract
The kidneys clear waste materials from the body and maintain a normal balance of fluids and chemicals in the body.
Patient picks for Kidney problems

Kidney and urinary tract
Kidney stones
Kidney stones are hard stones that can cause severe pain in your side along with blood in your urine, and nausea and vomiting. You are more likely to develop kidney stones if you eat a Western diet, don't drink enough fluids or are overweight. Once you have had one episode they are likely to recur but there are several kidney stone treatment options available.
by Dr Colin Tidy, MRCGP
Kidney and urinary tract
Glomerulonephritis
Glomerulonephritis is the name given to a range of conditions that can affect the kidney, specifically the glomeruli of the kidney. The glomeruli become damaged, commonly because of a problem with the body's immune system. Many people with glomerulonephritis may not notice any symptoms initially. However, salt and excess fluid can build up in the body if the glomeruli and kidneys are not working normally. This can lead to complications such as high blood pressure and, in some cases, chronic kidney disease, which may lead to end-stage kidney disease. Treatment will depend on the underlying cause as well as the severity of symptoms.
by Dr Toni Hazell, MRCGP
Frequently asked questions
What is the difference between nephrotic syndrome and kidney disease?
Nephrotic syndrome is a set of symptoms and signs where the kidneys leak a lot of protein. It is not a single disease itself. Kidney disease is a more general term for various conditions that affect the kidneys. Some causes of nephrotic syndrome can lead to chronic kidney disease over time, but initial kidney function in nephrotic syndrome is often normal, meaning the kidneys' 'waste clearing' function is not immediately affected.
My urine looks frothy. Does this mean I have nephrotic syndrome?
Frothy urine can be a symptom of nephrotic syndrome, as it indicates protein leaking into the urine. However, it's just one of several possible symptoms. Other key features of nephrotic syndrome include fluid retention (oedema), low protein levels in the blood, and high cholesterol. A doctor would need to perform urine and blood tests to confirm if nephrotic syndrome is present.
If I have nephrotic syndrome, what is the impact on my iron levels?
Nephrotic syndrome can lead to anaemia. This is because proteins that help carry iron around in the bloodstream are lost. Iron is essential for making red blood cells and preventing anaemia.
What does it mean if my nephrotic syndrome goes into remission?
Remission means that the symptoms and signs of nephrotic syndrome have disappeared. While this is a positive outcome, it doesn't mean you are completely cured, as there is still a chance the condition could return in the future. In some cases, especially in children with minimal change disease, sustained remission for several years can lead to being considered 'cured'.
Are there specific dietary changes I should make if I have fluid retention?
If you are experiencing fluid retention (oedema) due to nephrotic syndrome, limiting the amount of salt in your diet may be advised. This measure aims to help reduce the amount of fluid your body retains. Regular weighing of yourself can also help to monitor fluid retention and the effectiveness of treatments like 'water tablets' (diuretics).
Can taking medication for other conditions cause nephrotic syndrome?
Yes, nephrotic syndrome can sometimes occur as a side-effect of certain medicines. It can also be a consequence of various poisons or toxins. Additionally, some infections and other general conditions like diabetes or rheumatoid arthritis can also cause damage to the glomeruli, leading to nephrotic syndrome.
Further reading and references
- KDIGO Clinical Practice Guideline for Glomerulonephritis; International Society of Nephrology (2021).
- Kodner C; Diagnosis and Management of Nephrotic Syndrome in Adults. Am Fam Physician. 2016 Mar 15;93(6):479-85.
- Hahn D, Samuel SM, Willis NS, et al; Corticosteroid therapy for nephrotic syndrome in children. Cochrane Database Syst Rev. 2020 Aug 31;(8):CD001533. doi: 10.1002/14651858.CD001533.pub6.
- Sinha A, Bagga A; Clinical practice guidelines for nephrotic syndrome: consensus is emerging. Pediatr Nephrol. 2022 Dec;37(12):2975-2984. doi: 10.1007/s00467-022-05639-6. Epub 2022 Jun 28.
- Tamura H; Trends in pediatric nephrotic syndrome. World J Nephrol. 2021 Sep 25;10(5):88-100. doi: 10.5527/wjn.v10.i5.88.
- Trautmann A, Vivarelli M, Samuel S, et al; IPNA clinical practice recommendations for the diagnosis and management of children with steroid-resistant nephrotic syndrome. Pediatr Nephrol. 2020 Aug;35(8):1529-1561. doi: 10.1007/s00467-020-04519-1. Epub 2020 May 7.
- Tapia C, Bashir K; Nephrotic Syndrome.
Continue reading below
About the authorView full bio

Dr Surangi Mendis, MRCGP
Consultant and Medical Author
MBBS, BSc (1st), MRCGP (2014), DFSRH, PGcert otology and audiology
Surangi Mendis is a consultant in Audiovestibular Medicine and Neuro-otology at The Royal National ENT and Eastman Dental Hospitals, UCLH.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 9 Sept 2028
11 Sept 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.