Voiding cystourethrogram
Micturating cystourethrogram
Peer reviewed by Dr John Cox, MRCGPLast updated by Dr Laurence KnottLast updated 27 Jul 2016
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
This page has been archived.
It has not been reviewed recently and is not up to date. External links and references may no longer work.
A micturating/voiding cystourethrogram (MCUG/VCUG) produces X-ray images of the bladder and urinary tract.
Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
In this article:
Video picks for Urine and bladder tests
Continue reading below
What is a micturating/voiding cystourethrogram (MCUG/VCUG)?
A cystourethrogram produces specialised X-ray pictures. These help assess the structure and function of the lower urinary tract, in particular the bladder ('cysto') and the urethra (a tube which takes urine to the outside of your body). Images are also taken while the patient passes urine. Passing urine can be called micturating or voiding, hence the name. This is done to see whether urine flows away correctly from the bladder.
Note: for the rest of this leaflet we will use the short form of 'micturating/voiding cystourethrogram': MCUG/VCUG.
How does the urinary tract work?
Back to contentsUrinary Tract
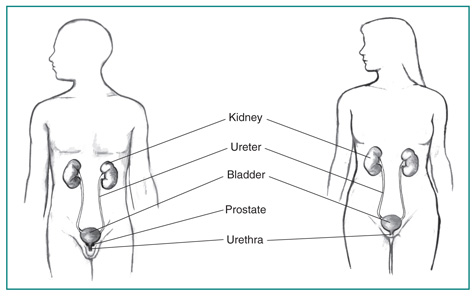
There are two kidneys, one on each side of the tummy (abdomen). They make urine which drains down tubes called ureters into the bladder. Urine is stored in the bladder and is passed out through the urethra from time to time when we go to the toilet.
The ureter passes through the wall of the bladder at an angle. So, when the bladder contracts to pass urine, the wall of the bladder squeezes the end of the ureter to prevent urine being passed back up the ureter. In effect, this action works like a valve to stop backflow (reflux) of urine up the ureters. Normally, urine should only flow in one direction.
Muscles under the bladder (called the pelvic floor) create the valve which allows urine to flow out when we go to the toilet. When working correctly, they should stop the urine coming out until we want it to.
Continue reading below
What is an MCUG/VCUG used for?
Back to contentsAn MCUG/VCUG is most commonly used in children who have repeated urinary tract infections. In some children, a problem with the junction of the ureters and bladder allows urine to flow backwards towards the kidneys instead of away from them. This condition is called vesicoureteric reflux. Usually this valve problem does not cause the urine infections. However, in children who get them, it is important that it is picked up. This is so that action can be taken to protect the kidneys from infected urine, and so prevent kidney damage. This is most often why an MCUG/VCUG is done.
Other reasons an MCUG/VCUG is done:
To find the cause of urinary incontinence.
To look for a cause of repeated urinary tract infections.
To check for structural problems of the bladder and the urethra.
To look for enlargement (hypertrophy) of the prostate or narrowing of the urethra in men (urethral stricture).
To look for injuries to the bladder or urethra.
How does an MCUG/VCUG work?
Back to contentsNormally, soft, hollow structures such as the bladder and ureters don't show up on X-ray images. In an MCUG/VCUG a special dye called a contrast agent is inserted into the bladder. The contrast agent blocks X-rays so that the areas it fills show up bright white in colour. This shows up the structures being examined by making them stand out against the black background on the X-ray picture.
An MCUG/VCUG also uses fluoroscopy. This is a technique which produces moving live video X-ray pictures on a screen. This allows the doctor to watch as the contrast agent fills the bladder and to observe any problems or defects. Urine should not flow backwards from the bladder so if the images show the contrast agent entering the ureters, this suggests vesicoureteric reflux. Your doctor may be able to assess how much of a problem this is by looking at the X-ray images.
Continue reading below
What happens during an MCUG/VCUG?
Back to contentsThe test takes about 30 minutes.
For a child
You will be able to stay with your child throughout the scan, unless you are pregnant. If you are pregnant, X-ray exposure during this procedure could harm the unborn child. It will therefore be necessary to arrange for another adult the child knows well to be with them for reassurance. Anyone staying with the child in the X-ray room will be given a lead apron to wear to protect them from X-ray exposure.
You will help your child to put on a hospital gown. They will lie down on the table. It might help distract them if you bring a favourite toy they can play with during the procedure. A very small child may need to be strapped in to stop them moving while the X-ray pictures are being taken.
Your child's genital area will be gently cleaned with an antiseptic solution by the nurse. Then a small, flexible tube (a catheter) will be gently pushed into the urethra and up into the bladder. Once this is in place, the dye (contrast agent) will be injected into the bladder through the catheter. The doctor will watch the pictures on the screen to see where the contrast agent goes. Your child may have to move into different positions so the contrast agent reaches all the relevant places. Finally your child will be asked to pass urine, whilst still on the table, into a jug or pan. The images on screen will show what is happening inside.
After this, your child will be able to get dressed and go home.
For an adult
The procedure is the same. You will be asked to take off your clothes and wear a hospital gown. You will be asked to lie on the table.
Your genital area will be cleansed and the catheter will be inserted in the same way. You may find this uncomfortable and it may feel uncomfortable as the contrast agent fills the bladder. You may be asked to change positions during the test to obtain different views of the bladder and urinary tract.
Finally, the doctor will take some pictures as you empty your bladder by urinating. You may feel embarrassed about having to urinate in front of other people. However, this is a routine test and the staff will want you to feel as relaxed as possible. You may feel a strong urge to urinate at other times during the test.
What should I do to prepare for an MCUG/VCUG?
Back to contentsYour hospital should give you information on how to prepare for this test. There is usually very little preparation needed. You/your child may be asked to take antibiotic medication before and/or after the test.
The test would not be done if the person having it has a urinary tract infection, so let the hospital know if you/your child have any of the signs of an infection (see below for a list).
Pregnant women should not have the test. So, let your hospital know if you are, or may be, pregnant. You should also advise the hospital if you are breast-feeding. They will let you know whether any special precautions need to be taken.
What can I expect after an MCUG/VCUG?
Back to contentsYou/your child may feel a burning sensation when you urinate and/or need to go to the toilet more often than usual for a short time. It is normal for urine to have a pinkish tinge for a couple of days after the test.
Are there any side-effects or complications from an MCUG/VCUG?
Back to contentsMost people have an MCUG/VCUG without any complications. Rarely, a person may have an allergic reaction to the dye (contrast agent) used. It is also possible, although uncommon, that damage to the bladder or urinary tract could be caused during injection of the contrast agent. The most common complication is a urinary tract infection.
You should contact your doctor if you/your child have any of the following problems:
Blood in the urine after two days.
Pain in the lower part of the tummy (abdomen).
Signs of a urinary tract infection. These signs include:
Pain or burning upon urination.
An urge to urinate frequently but usually passing only small amounts of urine.
Dribbling or leaking of urine.
Urine that is reddish or pinkish, foul-smelling, or cloudy.
Pain in the back just below the rib cage on one side of the body (flank pain).
High temperature (fever) or chills.
Feeling sick (nausea) or being sick (vomiting).
Patient picks for Urine and bladder tests

Tests and investigations
Cystoscopy
A cystoscopy is a procedure which looks into the bladder with a special telescope called a cystoscope. Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
by Dr Philippa Vincent, MRCGP
Tests and investigations
Midstream specimen of urine
A midstream specimen of urine (MSU or MSSU) is usually tested to look for infection, although in some cases, illness other than infection might be diagnosed based partly on what is seen in an MSU.
by Dr Rachel Hudson, MRCGP
Further reading and references
- Urinary tract infection in children: diagnosis, treatment and long-term management; NICE Clinical Guideline (August 2007)
- Hua L, Linke RJ, Boucaut HA, et al; Micturating cystourethrogram as a tool for investigating UTI in children - An institutional audit. J Pediatr Urol. 2016 Apr 16. pii: S1477-5131(16)30015-8. doi: 10.1016/j.jpurol.2016.03.009.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
27 Jul 2016 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.