Urethral stricture
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 22 May 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Prostate problemsEnlarged prostateUrinary retentionPSA testChronic prostatitisLower urinary tract symptoms in men
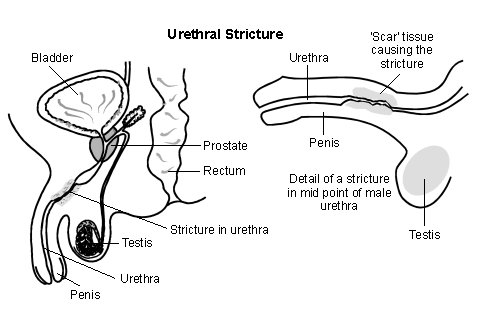
A stricture occurs when a part of your urethra (the tube that carries urine) becomes narrowed. Any section of your urethra may be affected, from the bladder to the tip of the penis. There is usually some scar tissue around the affected part of your urethra that causes the narrowing.
The length of strictures vary from less than 1 cm to the full length of the urethra. The diagram below illustrates a fairly long and severe stricture. However, many are shorter than this. Urethral stricture is uncommon in men and rare in women.
At a glance
A urethral stricture is a narrowing of the tube that carries urine out of the body.
Symptoms often include reduced urine flow, spraying urine, or dribbling after urinating.
Causes can include injury, infection, or, rarely, being born with it or cancer.
Diagnosis involves urine flow tests, looking into the urethra, and special X-rays.
Treatments include widening the stricture, surgery, urethroplasty, or antibiotics.
Untreated strictures can lead to bladder, prostate, and kidney infections.
In this article:
Video picks for Other men's health problems
Urethral stricture
Continue reading below
Urethral stricture symptoms
There may not be any symptoms initially. However, the following symptoms of urethral stricture - which are likely to worsen with time - may occur:
Reduced urine flow is the usual first symptom. Straining to pass urine is common but a complete blockage of urine flow is rare.
Spraying of urine or a double stream may occur.
Dribbling of urine for a while after going to the toilet to pass urine.
Frequency sometimes occurs (needing to pass urine more often than normal).
You may have a reduced force of ejaculation.
Sometimes, pain on passing urine.
Urethral stricture causes
Back to contentsInjury or damage to the urethra can heal with scar tissue that may cause a stricture. There are various types of injury that can damage the urethra. For example: an injury may occur during medical procedures to look into your bladder via your urethra; radiotherapy treatment may damage your urethra; a fall astride on to the frame of a bike can cause damage, or any trauma which is severe enough to cause a pelvic fracture.
Infection of your urethra is another cause - for example:
Sexually transmitted infections such as gonorrhoea or chlamydia.
Infection as a complication of long-term use of a tube (catheter) to drain your bladder.
Infection may cause inflammation in the tissues in and around your urethra.
These infections usually clear with treatment but may leave some scar tissue at the site of the inflammation, which can cause a stricture. Note that most urethral infections do not cause a stricture. A stricture is just one possible complication from a urethral infection.
Some babies are born with a urethral stricture.
Cancer - very rarely, a cancer of the urethra can be the cause of a stricture.
Continue reading below
Complications of urethral stricture
Back to contentsMore pressure is needed from the bladder muscle to pass urine out through a stricture (it acts like a bottleneck). Not all urine in the bladder may be passed when you go to the toilet. Some urine may pool in the bladder. This residual pool of urine is more likely to become infected.
This makes you more prone to bladder, prostate and kidney infections. A ball of infection (an abscess) above the stricture may also develop. This can cause further damage to the urethra and tissues below the bladder. Cancer of the urethra is an extremely rare complication of a long-standing stricture.
Urethral stricture diagnosis
Back to contentsAre tests needed?
As with all medical conditions, your doctor will start by asking you what your symptoms are (taking a history) and will then move on to a physical examination.
Tests to determine the flow rate of urine are usually advised if a urethral stricture is suspected. These are generally done by hospital consultants, after referral by a GP.
This involves:
Passing urine and measuring how much is passed per second. The flow rate is much reduced if you have a stricture.
A look into the urethra by a special thin telescope called a cystoscope will be needed to assess the stricture.
Special X-rays may be taken whilst you pass urine, which can show the site and severity of a stricture. This is called a retrograde urethrogram and involves having a contrast dye put into the bladder via a catheter, and x-rays are then taken to look at the flow of the dye out of the bladder, through the urethra.
Treatment for urethral stricture include:
Widening of the stricture.
Urethrotomy.
Surgery.
Antibiotics.
Treatment is usually advised to improve the flow rate of urine, to ease symptoms and to prevent possible complications. A specialist surgeon called a urologist advises on treatment. (A urologist treats problems of the urinary tract - such as conditions affecting the prostate, bladder, kidney and penis.) The one advised by your specialist will depend on factors such as the site and length of your stricture and also your age and general well-being.
Widening (dilatation) of the stricture
This is usually done by passing a thin plastic rod (boogie) into the urethra. This procedure may be done either under a local or a general anaesthetic. Rods of increasing thickness are gently inserted to gradually dilate the narrowed stricture. The aim is to stretch and widen the stricture without causing additional scarring.
However, a stricture often tends gradually to narrow again after each dilation. Therefore, a repeat dilation is commonly needed every so often when symptoms recur. (Some people are given a self-lubricating tube (catheter) which they insert themselves regularly to keep a stricture dilated.)
As a rule, the shorter the stricture, the greater the chance of a cure with dilation. It is a relatively easy procedure to do and so may be tried first.
Urethrotomy
In this procedure, a thin telescope is passed into the urethra to see exactly where the stricture is. This is done during a general anaesthetic. A tiny knife is then passed down the telescope to cut along the stricture. This widens the narrowed stricture.
You will get relief of symptoms from this procedure. About half of people are cured for good by this procedure. However, like dilation, the stricture may re-form and the procedure may have to be repeated from time to time in some cases.
Generally, the shorter the stricture, the greater the chance of a cure with this procedure.
Surgery
A corrective operation which is called a urethroplasty is performed if the above procedures do not work. Various techniques are used. For example, a short stricture can be cut out and the two ends of the healthy urethra stitched together.
If the stricture is longer then one kind of operation is similar to skin grafting the inside lining of the urethra. A graft is usually used from the inside of your cheek to form the new section of your urethra.
Techniques continue to improve and your specialist will advise if an operation is likely to be successful and which operation is best for the length and site of your stricture. As a rule, there is a high success rate in curing symptoms with these operations.
Antibiotics
A long course of antibiotics may be advised to prevent urine infections until a stricture has been widened.
Continue reading below
Urethral stricture prevention
Back to contentsIt may not always be possible to prevent a stricture, but the list of causes gives us some obvious ways to reduce the chance of getting one. Using condoms whenever you have sex will reduce the risk of getting a sexually transmitted infection, which is a risk factor for urethral stricture. Taking sensible safety precautions to avoid pelvic trauma could also reduce the risk.
Outlook
Back to contentsThe outlook will vary depending on the cause and the severity of the stricture - your urologist will be able to give you a better idea of your own personal outlook (prognosis) if you have a urethral stricture.
Frequently asked questions
Can I prevent urethral strictures, or for how long do I need to worry about one forming?
Preventing a urethral stricture isn't always possible, but reducing risk factors can help. For example, using condoms during sex can lower your chance of getting a sexually transmitted infection, which is a cause of strictures. Also, taking sensible safety precautions to avoid pelvic trauma can reduce the risk. Regarding how long to worry, the article doesn't specify a timeframe for when strictures typically develop after an injury or infection, but it does say symptoms are likely to worsen over time.
What is the typical recovery time after a procedure to widen a urethral stricture?
The article describes several procedures for urethral stricture, but it does not specify typical recovery times for any of them. It mentions that widening (dilatation) can be done under local or general anaesthetic. Urethrotomy is done under general anaesthetic. For surgery (urethroplasty), success rates in curing symptoms are high, but the recovery isn't detailed.
How do doctors choose which treatment option for urethral stricture is best for me?
A specialist surgeon called a urologist will advise on your treatment. The specific treatment recommended will depend on several factors, including the site and length of your stricture, as well as your age and overall health. Widening (dilatation) may be tried first as it's a relatively easy procedure, especially for shorter strictures. If that doesn't work, urethrotomy or surgery (urethroplasty) may be considered.
Is it normal for urethral stricture symptoms to come and go?
The article states that symptoms of urethral stricture are likely to worsen with time. While it doesn't explicitly say symptoms come and go, it does mention that after widening (dilatation) or urethrotomy, a stricture often tends to narrow again, and symptoms can recur. This might mean periods where symptoms improve after treatment, only to return later.
If I have an infection causing my stricture, how long will I need to take antibiotics?
If an infection is present or if you're prone to infections due to the stricture, a long course of antibiotics may be advised. The purpose of these antibiotics is to prevent urine infections until the stricture has been widened. The exact duration of this 'long course' is not specified in the article and would likely be determined by your doctor.
What does a 'urethrogram' involve, and will it be painful?
A retrograde urethrogram is a special X-ray procedure used to show the site and severity of a stricture. It involves having a contrast dye inserted into your bladder via a catheter. X-rays are then taken to observe how the dye flows out of your bladder and through your urethra. The article does not describe the procedure as painful, but it does involve the insertion of a catheter and dye.
Further reading and references
- Lumen N, Hoebeke P, Willemsen P, et al; Etiology of Urethral Stricture Disease in the 21st Century. J Urol. 2009 Jul 17.
- Jackson MJ, Veeratterapillay R, Harding CK, et al; Intermittent self-dilatation for urethral stricture disease in males. Cochrane Database Syst Rev. 2014 Dec 19;12:CD010258. doi: 10.1002/14651858.CD010258.pub2.
- Lee YJ, Kim SW; Current management of urethral stricture. Korean J Urol. 2013 Sep;54(9):561-9. doi: 10.4111/kju.2013.54.9.561. Epub 2013 Sep 10.
- Hampson LA, McAninch JW, Breyer BN; Male urethral strictures and their management. Nat Rev Urol. 2014 Jan;11(1):43-50. doi: 10.1038/nrurol.2013.275. Epub 2013 Dec 17.
- Tritschler S, Roosen A, Fullhase C, et al; Urethral stricture: etiology, investigation and treatments. Dtsch Arztebl Int. 2013 Mar;110(13):220-6. doi: 10.3238/arztebl.2013.0220. Epub 2013 Mar 29.
Continue reading below
About the authorView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
22 May 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
