Chronic prostatitis
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 24 May 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Prostate problemsEnlarged prostateUrinary retentionPSA testUrethral strictureLower urinary tract symptoms in men
Prostatitis means that you have inflammation of your prostate gland. There are two main types of prostatitis: short-lived (acute) or persistent (chronic). It can also be caused by an infection (infective) or be non-infective. Less than 1 in 10 cases of prostatitis are due to bacterial infection.
For the diagnosis of chronic prostatitis, symptoms need to have been present for at least three months. In acute prostatitis, symptoms usually come on and go away much more quickly.
About 9 in 10 men with chronic prostatitis have chronic prostatitis/chronic pelvic pain syndrome (CPPS). About 1 in 10 men with chronic prostatitis have chronic bacterial prostatitis.
At a glance
Chronic prostatitis involves pain around the penis, anus, lower tummy, or lower back.
You might have urinary issues like painful or frequent urination, and sexual problems.
Chronic bacterial prostatitis symptoms can flare up and then ease with treatment.
Diagnosis involves a prostate exam, urine tests, and sometimes further specific tests.
Treatment can include painkillers, antibiotics, or medicines like alpha-blockers.
Symptoms often improve over time, with many seeing improvement within months.
Chronic prostatitis may affect sperm quality and reduce fertility.
In this article:
Video picks for Prostate problems
Continue reading below
Chronic prostatitis symptoms
The symptoms of chronic prostatitis/chronic pelvic pain syndrome include:
Pain
This is usually around the base of the penis, around the anus, in the lower tummy (abdomen) and in the lower back. Sometimes the pain spreads down to the tip of the penis and/or into the testicles (testes). Pain is the main symptom in chronic prostatitis. The pain may vary in severity from day to day.
Urinary symptoms
These may include mild pain when you pass urine, an urgent desire to pass urine at times, some hesitancy when trying to pass urine or a poor urinary stream.
Sexual problems
You may experience difficulty in getting an erection (impotence), ejaculation may sometimes be painful, or be premature, and some men have worse pain (as described above) after having sex.
Other symptoms
You may feel tired and have general aches and pains. You may feel anxious, stressed or depressed and your quality of life may feel worse.
Men with chronic bacterial prostatitis tend to have symptoms that wax and wane:
During a flare-up, you can have pain and discomfort. You feel this mainly at the base of your penis, around your anus, just above your pubic bone and/or in your lower back. Pain may spread to your penis and testicles (testes). Passing stools (faeces) can be painful.
You may also have symptoms from a urine infection, such as pain when you pass urine, passing urine frequently or an urgent desire to pass urine.
These symptoms are similar to the symptoms of acute bacterial prostatitis. However, men with a flare-up of chronic bacterial prostatitis tend to be less ill than those with acute prostatitis. For example, a high temperature (fever) is less likely and you are less likely to have general aches and pains.
If you have chronic bacterial prostatitis, your symptoms will generally ease when treated with antibiotics. However, unless the antibiotics completely clear the infection from the prostate gland, you are at risk of the infection coming back (flaring up) again.
In between flare-ups, you may have some mild residual pain and some mild urinary symptoms (such as passing urine frequently or an urgent desire to pass urine).
How common is chronic prostatitis?
Back to contentsUp to 8% of men will be affected by symptoms of prostatitis at some point in their lives, however it is difficult to know how many truly have chronic prostatitis as the symptoms may sometimes be due to another condition. The risk of having chronic prostatitis goes up with age, being three times more common in men aged 50 - 59 than in those aged 20 - 39.
Continue reading below
How do you get chronic prostatitis?
Back to contentsThe exact cause is often unknown and there may be several different causes or types of prostatitis. Chronic bacterial prostatitis is one possibility - caused by a persistent (chronic) infection with a germ (a bacterial infection). A man with chronic bacterial prostatitis will usually have had recurring urine infections. Chronic bacterial prostatitis is more common in men who have an immune system that doesn't work properly (are immunocompromised) - this may be due to a disease, such as untreated HIV, or because they have a condition such as arthritis which needs to be treated with drugs that suppress the immune system.
Chronic bacterial prostatitis is usually caused by the same type of germs (bacteria) that causes the urine infections. The prostate gland can harbour infection and therefore recurring infections can occur. Chronic bacterial prostatitis is not a sexually transmitted infection, but it can sometimes be caused by sexually transmitted bacteria.
What causes chronic pelvic pain syndrome (CPPS)?
CPPS is a type of chronic prostatitis that causes discomfort or pain in your lower pelvic region - mainly at the base of your penis and around your anus. It is usually diagnosed if you have had pain for at least three months within the previous six months. The cause of this type of chronic prostatitis is not fully understood.
How is chronic prostatitis diagnosed?
Back to contentsExamination of your prostate gland
Your doctor may examine your prostate gland. The doctor inserts a gloved finger in your back passage (rectum). Your prostate gland may be tender on examination in chronic prostatitis. However, this is not so in every case.
A urine sample
A urine sample is usually taken to rule out urine infection. This is especially important for chronic bacterial prostatitis although, in between flare-ups, there may be no signs of infection.
Further tests of your kidneys and urinary tract
If your doctor suspects that you have chronic bacterial prostatitis, they may suggest that you have further tests to rule out any problem with your urinary tract that may have contributed to (or caused) the infection. For example, an ultrasound scan of your kidneys to look for any abnormalities.
Tests to exclude other causes for your symptoms
This includes:
Fluid sample from the prostate.
Swab or urine tests are done to exclude a sexually transmitted infection (STI) which can produce similar symptoms to chronic prostatitis.
Sometimes your doctor may suggest a blood test to exclude other problems with your prostate gland. These are done to rule out other conditions of your prostate or nearby organs if your symptoms are not typical.
If you are referred to a urologist, a sample of fluid ('secretions') from the prostate may be collected to rule out infection in your prostate. This is sometimes done in cases of chronic prostatitis.
To do this, a doctor can gently massage your prostate, with a gloved finger in your rectum. By doing this, fluid from the prostate is pushed out into the urethra and comes out from the penis to be collected and tested for germs (bacteria). If you have CPPS, no bacteria are found in the prostate fluid or urine.
Continue reading below
What is the prostate gland?
Back to contentsCross-section diagram of the prostate and nearby organs
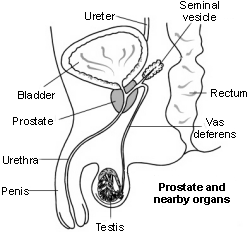
The prostate gland is only found in men and is part of the male reproductive system. It lies just beneath the bladder. It is normally about the size of a chestnut.
The urethra is the tube that passes urine from the bladder and it runs through the middle of the prostate. The prostate helps to make semen and seminal fluid but most semen is made by another gland (the seminal vesicle).
Chronic prostatitis treatment
Back to contentsThe treatment of chronic prostatitis can be difficult. However, in most people, symptoms improve over months or years.
If your GP suspects that you have chronic prostatitis, as mentioned above, they will usually refer you to a specialist for further assessment. In the meantime, your GP may suggest one or more of the following whilst you are waiting for your appointment with a specialist:
Painkillers such as paracetamol or ibuprofen may ease the pain.
Laxatives may be helpful if it is painful or difficult to pass stools.
Antibiotics are recommended if your doctor thinks you have chronic bacterial prostatitis. The antibiotic course should last for 2-4 weeks. Antibiotics are usually advised if you have had a urinary tract infection or an episode of acute prostatitis within the previous year. This is to be absolutely sure that no infection is present.
Treatments that a specialist may suggest
Various treatments have been tried for chronic prostatitis. They may benefit some people but so far there are few research studies to confirm whether they help in most cases. They are not 'standard' or routine treatments but a specialist may advise that you try one.
Possible treatments for chronic bacterial prostatitis include the following:
A longer course of antibiotics. If the specialist suspects that you have chronic bacterial prostatitis and your symptoms have not cleared after a four-week course of antibiotics, they may suggest a longer course. Sometimes a course of up to three months is used.
Removal of the prostate (prostatectomy) may very occasionally be considered if you have small stones (calculi) in the prostate. It is not clear how much this may help but it has been suggested that these small stones may be a reason why some people have recurrent infections in chronic bacterial prostatitis. However, this is not a common type of treatment and is not suitable in everyone. Your specialist will advise.
For chronic prostatitis/CPPS, possible treatments may include the following:
Antibiotics - these may be tried initially, although the evidence for their effectiveness is limited. It may be that some antibiotics have anti-inflammatory properties as well or that they may clear some germs (bacteria) that are difficult to find when your urine is tested.
Alpha-blockers - are medicines that are used to treat prostate gland enlargement. They relax the muscle tissue of the prostate and the outlet of the bladder. There are several different brands. There is some evidence that they help in CPPS and one may be worth a try.
Other medicines - for example, bioflavonoids (such as quercetin) and finasteride (a medicine which may 'shrink' the prostate).
Stress management - this and other pain-relieving techniques are sometimes tried to help cope with the persistent pain.
What is the outlook?
Back to contentsIt is difficult to give an outlook (prognosis). Your symptoms may last a long time, although they may 'come and go' or vary in severity. Painkillers can keep discomfort to a minimum.
Some people worry that they may have a serious disease such as prostate cancer. However, worry and anxiety can make symptoms of chronic prostatitis worse so seeking a formal diagnosis is advised.
Most men diagnosed with chronic prostatitis/CPPS tend to have an improvement in their symptoms over the following six months. In one study, about a third of men had no further symptoms one year later. In another large study, one third of men showed moderate to marked improvement over two years.
Can chronic prostatitis cause infertility?
It is though that chronic prostatitis may reduce the amount and quality of sperm, which may have an effect on fertility.
Patient picks for Prostate problems

Men's health
Enlarged prostate
The prostate gland commonly becomes larger in older men. Women do not have a prostate gland. This prostate gland enlargement is also called benign prostatic hypertrophy (or hyperplasia). It can cause problems with passing urine. Symptoms are often mild. Without treatment, symptoms do not always become worse and may even improve over time. If symptoms become troublesome or distressing they can be improved by medicines or surgery.
by Dr Toni Hazell, MRCGP

Men's health
Acute prostatitis
When the prostate gland becomes infected with a germ (a bacterial infection), the condition is known as acute prostatitis. 'itis' means inflammation, so prostatitis is inflammation of the prostate - not all forms of prostatitis are bacterial, but this leaflet will mainly cover bacterial prostatitis. Symptoms include pain, mainly at the base of the penis and around the anus. A bladder infection commonly occurs at the same time. Treatment includes a four-week course of antibiotic medication.
by Dr Toni Hazell, MRCGP
Frequently asked questions
Can chronic prostatitis be a sexually transmitted infection?
Chronic bacterial prostatitis is generally not considered a sexually transmitted infection (STI). However, in some cases, it can be caused by bacteria that are typically spread through sexual contact.
If I have chronic bacterial prostatitis, how long might I need to take antibiotics?
If your GP suspects chronic bacterial prostatitis, an initial course of antibiotics might last for 2-4 weeks. If symptoms persist and a specialist confirms bacterial prostatitis, they might suggest a longer course, sometimes up to three months. This extended treatment aims to ensure the infection is completely cleared from the prostate gland.
What is the difference between chronic bacterial prostatitis and chronic pelvic pain syndrome (CPPS)?
Chronic bacterial prostatitis is caused by a persistent bacterial infection in the prostate gland, often linked to recurring urine infections. Chronic pelvic pain syndrome (CPPS) also causes pain in the lower pelvic region, but its cause is not fully understood, and unlike bacterial prostatitis, tests for CPPS typically do not find bacteria in the prostate fluid or urine.
Are there any non-medicinal ways to help manage the symptoms of chronic prostatitis?
Yes, some approaches can help manage symptoms. Painkillers like paracetamol or ibuprofen can help with pain. Laxatives might be useful if passing stools is painful or difficult. Additionally, stress management techniques can be tried to help cope with persistent pain, as anxiety can sometimes worsen symptoms.
What is the purpose of the doctor massaging the prostate during diagnosis?
To diagnose chronic prostatitis, a doctor may gently massage your prostate through your back passage. This action pushes fluid from the prostate into the urethra and out of the penis, allowing it to be collected and tested for bacteria. This test helps to determine if an infection is present, particularly in cases where chronic bacterial prostatitis is suspected.
How quickly do symptoms of chronic prostatitis usually improve?
The improvement of symptoms can vary. While symptoms may last a long time and fluctuate in severity, many men with chronic prostatitis/CPPS experience an improvement over several months. Studies have shown that about a third of men might have no further symptoms after a year, and a significant number show moderate to marked improvement over two years.
Can chronic prostatitis lead to more serious conditions like prostate cancer?
The article states that some people worry about serious diseases like prostate cancer. However, it also clarifies that worry and anxiety can make symptoms worse and advises seeking a formal diagnosis for reassurance. It does not indicate that chronic prostatitis directly leads to prostate cancer; instead, diagnostic tests are sometimes performed to rule out other prostate issues if symptoms are unusual.
Further reading and references
- Bowen DK, Dielubanza E, Schaeffer AJ; Chronic bacterial prostatitis and chronic pelvic pain syndrome. BMJ Clin Evid. 2015 Aug 27;2015. pii: 1802.
- Holt JD, Garrett WA, McCurry TK, et al; Common Questions About Chronic Prostatitis. Am Fam Physician. 2016 Feb 15;93(4):290-6.
- Urological infections; European Association of Urology (2022 -updated 2024)
- Prostatitis - chronic; NICE CKS, June 2024 (UK access only)
Continue reading below
About the authorView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
24 May 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.