Developmental dysplasia of the hip
Peer reviewed by Dr Adrian Bonsall, MBBSLast updated by Dr Jacqueline Payne, FRCGPLast updated 23 Sept 2016
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Newborn screening testNewborn physical examinationsNewborn hearing testNewborn bloodspot testUndescended testiclesTreating newborn health problems
This page has been archived.
It has not been reviewed recently and is not up to date. External links and references may no longer work.
Developmental dysplasia of the hip is a problem with the way that the hip joint develops. It is usually present from birth although may develop later. It is more common in girls. When developmental dysplasia of the hip is diagnosed and treated early in a young baby, the outcome is usually excellent. If treatment is delayed, the treatment is more complex and has less chance of being successful.
In this article:
Video picks for Development
Continue reading below
Understanding the hip joint
Pelvis and Hips

The place where the rounded top of the thigh bone (head of the femur) meets the pelvis is called the hip joint. Within the pelvis, the acetabulum is a rounded cup-like structure in which the rounded top of the thigh bone sits. It is called a 'ball and socket' joint. The ball is the head of the femur and the socket is the acetabulum.
The diagram on the right shows the normal structures.
What is developmental dysplasia of the hip?
Back to contentsDevelopmental dysplasia of the hip (DDH) is an abnormality in the hip joint, usually present from birth.
DDH was previously known as congenital dislocation of the hip (CDH). It was renamed as there are different degrees of abnormality (not just dislocated hips) and it isn't always there from birth but can develop later.
In a normal hip, the head of the femur is a smooth rounded ball and the acetabulum is a smooth cup-like shape. The head of the femur and the acetabulum are in close contact, a little bit like an egg in an egg cup.
Subluxed and dislocated hip
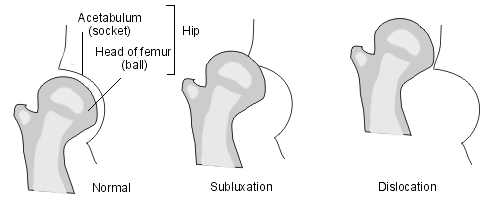
In DDH, there is an abnormality either in the shape of the head of the femur, the shape of the acetabulum, or the supporting structures around them. As a result, the acetabulum and femur are not in close contact. It may be a mild abnormality where there is some contact between them. This is called subluxation. It may be a severe abnormality where there is no contact between them and this is called dislocation.
Continue reading below
What causes developmental dysplasia of the hip?
Back to contentsThe cause of developmental dysplasia of the hip (DDH) is not clear. However, there are factors that are known to contribute to the chance of a baby being born with DDH. Only 1 in 75 babies with a risk factor have DDH. Risk factors include:
Family history. If there is a parent, brother or sister with DDH then this makes it five times more likely than normal for a child to have DDH.
Gender. About 8 in 10 cases of DDH are female. This may be due to the effects of a chemical (hormone) called relaxin that is made during pregnancy but from which male babies have some protection. Relaxin makes the ligaments stretchier and means that the bones are more likely to move out of position.
Pregnancy conditions. If there is only a small amount of fluid in the womb (uterus) this is called oligohydramnios. This can increase the risk of developing DDH because the baby is not able to move about within the uterus as much.
Breech position. If an unborn baby is in the breech position (bottom down position in the womb), this can put the legs in a position which increases the risk of DDH. Most breech babies are born by caesarean section. These babies have a risk of DDH seven times higher than normal. (The risk of DDH for a breech baby delivered vaginally is 17 times higher than normal.)
Firstborn baby. About 6 in 10 cases of DDH occur in firstborn children. This may be because the womb is tighter and less elastic than in future pregnancies so that the baby has less room to move.
Other abnormalities. If the baby has cerebral palsy, spinal cord problems or other nerve and muscle disorders, this increases the risk of developing DDH. DDH is also more common in premature babies or babies born weighing more than 5 kg.
Culture. The risk of a child having DDH is much greater in certain cultures. For example, DDH was much more common in American Navajo infants and infants in Turkey and Japan but much less common in African American infants. This was due to the way that Navajo, Japanese and Turkish babies use to be swaddled, although this has changed in recent times.
How common is developmental dysplasia of the hip?
Back to contentsDevelopmental dysplasia of the hip (DDH) occurs in about 1 to 3 out of every 100 babies. It is more common in the left hip. This is thought to be due to the fact that most unborn babies lie against the mother's spine on their left side. This position may put more pressure on the left hip and cause it to develop abnormally more often than the right one. In about 2 in 10 cases, DDH affects both hips.
Continue reading below
What are the symptoms and signs of developmental dysplasia of the hip?
Back to contentsA newborn baby with developmental dysplasia of the hip (DDH) is not distressed or in pain. Soon after birth, most babies are examined by a midwife and/or a hospital doctor. One of the problems they are looking for is DDH. They will bend your baby's knees and turn their thighs outwards, a bit like opening a book. Whilst doing this, they are feeling for a clunk, which feels similar to when a light switch is turned on. If they feel this then it may indicate that there is a problem with the hip.
Two other signs of hip problems are:
The thigh bone may look shorter on one side. Your doctor or midwife can do an examination to check for this. In about one in four normal babies there are unequal skin folds, so it is not such an important finding.
The skin folds between the legs and the body may not be equal on both sides.
Examining babies' hips is difficult. The baby needs to be out of its nappy and relaxed, not crying. Ideally, babies should be examined within 24 hours of birth, at the six-week check, between 6-9 months of age and again at walking age. This is because a normal examination at a younger age doesn't mean that DDH won't be present later.
In older children with DDH who are walking, they may have a limp in their walk. This should raise the suspicion of DDH. The child may also walk on its toes. However, it is not common for DDH to cause a delay in walking.
How is developmental dysplasia of the hip diagnosed?
Back to contentsWhen developmental dysplasia of the hip (DDH) is suspected in a newborn baby, you may simply be advised to return for a review examination in a few weeks. This is because the hip may be unstable at birth in many newborn babies because the tissues are soft and lax. In most babies, the hip will become stable by itself by two months, as the soft tissues tighten. Sometimes, just by examining a newborn baby's hips, a dislocated or subluxed hip can be relocated into the correct position and be made stable.
If the instability persists on review then, for a baby up to 4-6 months old, an ultrasound scan may be done. This gives a good picture of whether there is a problem with the hip joint or not. (An ultrasound scan is a painless test that uses sound waves to detect structures in the body. It is the same type of scan that is done routinely on pregnant women early in their pregnancy.) If your baby was bottom down (breech) inside your womb they will have an ultrasound scan of their hips when they are about 2 weeks old. This is because they have a high risk of having DDH due to their position in the womb.
In children aged over 4-6 months, an X-ray is more helpful. Various measurements are taken on the X-ray picture of the pelvis and femur to determine whether a child has DDH.
What is the treatment for developmental dysplasia of the hip?
Back to contentsTreatment for developmental dysplasia of the hip (DDH) is needed because if the head of the thigh bone is left in an abnormal position then the hip joint doesn't develop normally. The earlier treatment is started after birth, the greater the likely success of treatment and the lower rate of long-term complications.
The goal of treatment is to get the head of the thigh bone to go back into the hip joint. This then allows the structures of the rapidly developing hip joint (femur, acetabulum, supporting ligaments, etc) to become established normally. The treatment goal can be achieved through a variety of methods, depending on the age of your child. The success rate of simple non-surgical treatments reduces significantly after 7 weeks of age. Commonly used treatments are as follows:
Pavlik® harness
This is a device that is used to hold the hips in the correct position. It is often the first treatment used in children under 6 months old. It usually needs to be worn full-time for at least six weeks and then part-time for six weeks in young babies. Older babies may need to wear it for longer. During this time, ultrasound scans are usually done to check that the hip is in the correct position. This harness keeps the legs bent and turned outwards but allows certain movements. It does not allow your child to straighten their legs or turn them inwards. The harness is adjusted as the child grows and as the hip stabilises.
For mild DDH (subluxation) this harness works in more than 9 in 10 children if used at this young age. In severe DDH (dislocation) the harness is effective in about 8 in 10 children. The main possible complication of the harness is called avascular necrosis. This is uncommon (about 2 in 100 babies treated with the harness) but sometimes occurs if the hip is not held in the correct position. (Avascular necrosis means that the bone tissue at the head of the thigh bone dies due to undue pressure on the blood supply to the bone.)
Closed reduction and hip spica
This method is used in children over 6 months of age, or if the Pavlik® harness is not effective. This involves your child being given an anaesthetic. While they are anaesthetised, the doctor positions the hip the correct way and then applies a special cast or plaster to keep the hip in the right position. The position of the hip is confirmed as correct by an MRI or CT scan done after the procedure. This cast is kept on for at least 12 weeks.
Open reduction
If the above options fail or your child is much older when DDH is diagnosed, then an operation is needed. The operation involves loosening the tendons around the hip and removing anything that is stopping the hip from moving freely. Once the bones are in a good position, the joint is strengthened.
Other types of surgery
If DDH has not resolved by 18 months, more complicated surgery is required. This involves removing some parts of the bone and joint so that the hip can be kept in the right position.
What if developmental dysplasia of the hip is not treated?
Back to contentsIf your child's developmental dysplasia of the hip (DDH) is not diagnosed and treated early, they may develop early arthritis of the hip joint. This causes pain and reduced movement. The treatment of DDH becomes more complex and with less chance of success once your child's bones have fully developed. Even at this stage, however, treatment may still provide a better long-term outcome but this depends on the severity of the DDH.
What is the outlook (prognosis)?
Back to contentsMost children who are diagnosed early and treated before the age of 6 months have an excellent outcome. However, they will usually need to be reviewed with X-ray pictures taken throughout childhood until their bones have fully developed. The outlook is less good if the diagnosis or treatment is delayed, especially if the child has begun to walk before developmental dysplasia of the hip (DDH) is diagnosed. About 3 in 10 hip replacement operations done in people under the age of 60 years are because of DDH (either untreated, unsuccessfully treated, or delayed in treatment).
Can developmental dysplasia of the hip be prevented?
Back to contentsMany of the factors that are linked to the cause of developmental dysplasia of the hip (DDH), cannot be changed, such as being a baby girl or having a relative with DDH. However, if you carry your baby in front or behind you, with their hips wide open across your body, this makes DDH less likely.
If you are going to swaddle your baby it is important that you do so safely, so that you don't increase the chance of your baby having DDH:
Make sure your baby's hips are drawn up towards the tummy and slightly open, like a book, 'frog' style.
Your baby's knees should also be slightly bent.
It may also help if your baby's hips can move freely up and outwards.
Making sure that your baby's hips aren't held straight and together allows the hips to develop properly.
Patient picks for Development

Children's health
Restricted growth
Dwarfism is a medical or genetic condition which causes people to have restricted growth so that they are shorter than average. Specifically, people with dwarfism grow no higher than 4 ft 10 ins (147 cm). It can be due to literally hundreds of different causes, so the term actually includes many different medical conditions. The cause and type of dwarfism will therefore affect the outlook and problems that may be associated with it. The most common condition causing dwarfism is achondroplasia.
by Dr Hayley Willacy, FRCGP

Children's health
Surviving adolescence
This leaflet is adapted from a leaflet provided by the Royal College of Psychiatrists, the professional body responsible for education, training, setting and raising standards in psychiatry. Adolescence is the transitional stage from childhood to adulthood that occurs between ages 13 and 19 years. Therefore adolescence more or less means the teenage years. The teenage years can be a very difficult emotional time for both adolescents and their parents. A gulf can grow between parents and their children during adolescence. The rapid physical development and deep emotional changes are exciting, but can also be confusing and difficult to deal with.
by Dr Colin Tidy, MRCGP
Further reading and references
- Sewell MD, Rosendahl K, Eastwood DM; Developmental dysplasia of the hip. BMJ. 2009 Nov 24;339:b4454. doi: 10.1136/bmj.b4454.
- Shorter D, Hong T, Osborn DA; Cochrane Review: Screening programmes for developmental dysplasia of the hip in newborn infants. Evid Based Child Health. 2013 Jan;8(1):11-54. doi: 10.1002/ebch.1891.
- Schwend RM, Shaw BA, Segal LS; Evaluation and treatment of developmental hip dysplasia in the newborn and infant. Pediatr Clin North Am. 2014 Dec;61(6):1095-107. doi: 10.1016/j.pcl.2014.08.008. Epub 2014 Sep 18.
Continue reading below
About the author

Dr Jacqueline Payne, FRCGP
General Practitioner, Medical Author
MB, BS, DFFP, DRCOG, FRCGP
Jacqueline was a GP in Kendal, Cumbria for 25 years, where she trained young GPs for the RCGP and was an Instructing Doctor for the FSRH.
About the reviewerView full bio

Dr Adrian Bonsall, MBBS
Medical Author
MA (Chemistry), MBBS (Hons), DCH
Since 2000 Adrian has been employed in emergency and critical care paediatrics based in Sydney, with particular interests in toxicology, trauma and resuscitation.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
23 Sept 2016 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.