Actinic keratosis
Solar Keratosis
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 20 Jan 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
An actinic keratosis (also known as a solar keratosis) is the most common skin condition caused by sun damage. It is the result of skin being damaged by the sun over many years. Actinic keratoses are usually rough, scaly patches on sun-exposed areas such as the head and face.
Actinic keratoses are common, especially in older people, many of whom have more than one. Usually they are harmless but there is a small risk that they may eventually turn into skin cancer and therefore treatment may be advised.
In this article:
Video picks for Skin rashes
Continue reading below
What is an actinic keratosis?
An actinic keratosis (AK) is a small, thickened, scaly skin growth which develops on the skin. It is the most common skin condition caused by sun damage. It is caused by excessive exposure to ultraviolet (UV) rays from the sun over many years.
What does an actinic keratosis look like?
Back to contentsThe below pictures show actinic keratoses on a forehead.
Forehead actinic keratoses
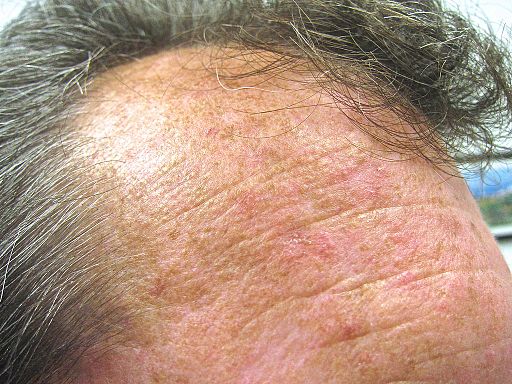
© Future FamDoc (own work), via Wikimedia Commons
Close view of actinic keratosis
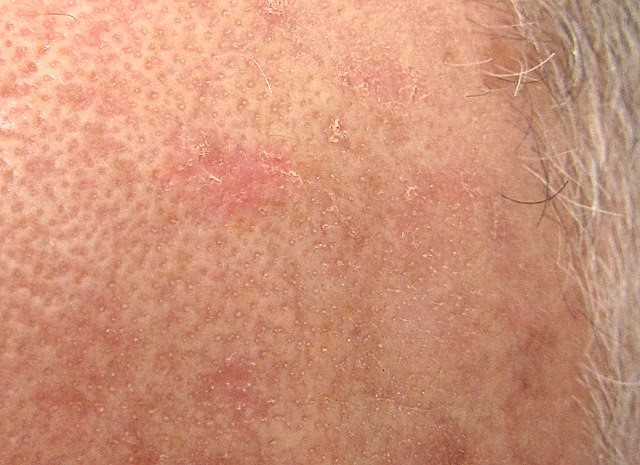
© Future FamDoc, CC BY-SA 4.0, via Wikimedia Commons
Continue reading below
Symptoms of an actinic keratosis
Back to contentsEach actinic keratosis can range from the size of a pinhead to 1-3 cm across. They may also:
Be light, dark, pink, red, or the same colour as the underlying skin, or a combination of these.
Have a yellow-white, scaly crust on the top of them.
Have redness around the surrounding skin.
Feel rough and dry.
Be slightly raised from the surface of the skin. (Often it is easier to feel rather than see them).
Be hard and warty. Sometimes hard skin grows out of an actinic keratosis like a horn (called a cutaneous horn).
Several actinic keratoses may develop at about the same time, often in the same area of skin. Sometimes they can join together and form a large, flat-ish, rough area of skin.
Actinic keratoses usually develop on areas of skin which have received a lot of sun exposure. Skin on the following areas is commonly affected:
Face.
Neck.
Ears.
Bald patches on the scalp.
The backs of the hands.
They may also appear in other areas (such as the back, chest and legs) in people who do a lot of sunbathing. There are usually no other symptoms. Rarely, there may be an itchy or prickling sensation from affected areas of skin.
What causes an actinic keratosis?
Back to contentsAn actinic keratosis is caused by damage to the skin by UV light which is part of sunlight. The skin is normally good at repairing any minor damage. However, over the years, some areas of skin are unable to cope with the repeated exposure to sun and an actinic keratosis can form.
Continue reading below
Who gets actinic keratoses?
Back to contentsAnyone can get actinic keratoses; however, it most commonly affects:
People with fair skin who do not tan easily - especially those with blue/green eyes and blonde/red hair.
Those over the age of 50.
People who work outdoors (such as construction workers, farmers, etc).
Those who sunbathe a lot or use tanning beds.
Actinic keratoses can occur in people with darker skin but they are almost unheard of in black-skinned people.
As it usually takes years of sun exposure to develop an actinic keratosis, older people tend to be most commonly affected.
How common are actinic keratoses?
Back to contentsIn the UK, about 1 in 4 or 5 people over the age of 60 years have (or have had) actinic keratoses. It is much more common in places where the climate is sunnier, for example in Australia. They are more common in men, mainly because men are traditionally more likely to have had outdoor occupations.
Actinic keratoses are also more common in people who have a suppressed immune system, such as:
People who have had organ transplants (because they take long-term anti-rejection medication).
People who have had chemotherapy to treat cancer.
People who take medicines which suppress the immune system for other conditions such as rheumatoid arthritis or systemic sclerosis.
People with HIV infection.
However, even in such people, they do not occur without some exposure of the skin to the sun.
What happens to an actinic keratosis?
Back to contentsThree things can happen to each actinic keratosis. This is important when considering treatment of an actinic keratosis:
The actinic keratosis may regress. This means it clears away on its own without treatment.
An actinic keratosis may persist. So it remains stable, not changing but not disappearing either.
It might progress into a skin cancer (see below).
Is an actinic keratosis dangerous?
Back to contentsIn themselves, actinic keratoses are not cancerous (non-malignant) and do no harm. However, they can sometimes be unsightly.
In people who have between seven and eight actinic keratoses on their skin, there is about a 1 in 10 chance that one will turn into a form of skin cancer called squamous cell carcinoma (SCC) over a 10-year period.
This is not the most serious form of skin cancer (melanoma). It is often a fairly slow-growing cancer and can usually be easily cured if treated early enough. This means that actinic keratosis can be seen as a possible precursor to cancer. See the separate leaflets called Types of Cancer and Non-melanoma Skin Cancer for more details.
The reason that actinic keratoses can become cancerous is because the UV exposure from the sun's rays causes changes (mutations) to the genes in the DNA of skin cells. This causes the skin cells to divide and grow abnormally instead of just repairing damage. The abnormal cells tend to multiply in an out of control way - this causes a lump (tumour).
Actinic cheilitis is a lesion like an actinic keratosis that develops on the lip. If this progresses to a squamous cell carcinoma it is more dangerous than squamous cell carcinomas presenting on other parts of the skin - therefore actinic cheilitis should be referred to a dermatologist sooner rather than later.
How are actinic keratoses diagnosed?
Back to contentsA GP may be able to diagnose an actinic keratosis by its typical appearance alone or using a dermatoscope. This is a magnifier with a light that helps to distinguish between harmless (benign) skin lesions and cancerous (malignant) ones. Sometimes this is difficult and, if doubt exists, a referral may be made to a skin specialist (dermatologist).
Sometimes it is necessary to take a biopsy of the skin lesion. This means that a small sample of skin (a biopsy) is taken and examined under the microscope in a laboratory. A biopsy means that the cells in the skin can be seen and an accurate diagnosis can be confirmed.
What is the treatment for an actinic keratosis?
Back to contentsNo treatment
Without treatment, some actinic keratoses will disappear on their own. However, they can come back (recur) or new ones may develop. It is sometimes advised to leave them alone without treatment, particularly if there are only one or two.
Medical advice should be sought again if there are any changes to the appearance or if it becomes tender. A moisturising (emollient) cream might be advised to help soften the skin around the actinic keratosis.
High sun protection factor (SPF) sunscreen should always be used. High-factor sunscreens also moisturise but - more importantly - they will prevent further sun damage to the skin (and hopefully prevent the development of further actinic keratoses).
If treatment is advised, there are several options. The method advised will depend on factors such as:
The number of actinic keratoses.
Where they are.
How big or thick they are.
How big an area of skin is affected.
Freezing an actinic keratosis with liquid nitrogen
Liquid nitrogen is a common treatment in people who have small numbers of actinic keratoses. It is also called cryotherapy or cryosurgery. Liquid nitrogen is so cold that it destroys tissue. This is sometimes used by dermatology clinics.
An actinic keratosis can be easily sprayed with liquid nitrogen. It is destroyed and then falls off a few days later. A small scab is left and is gradually replaced by fresh healthy skin. Liquid nitrogen often causes the surrounding skin to blister for a few days. Sometimes this form of treatment can leave a white spot on the skin after treatment.
A cream or gel
Topical treatments (meaning they are applied directly to the skin) are useful where there are a lot of small actinic keratoses which would otherwise need repeated freezing to get rid of them all. Creams, gels (water-based) and ointments (greasier) are available.
One type of gel contains an anti-inflammatory medicine called diclofenac. Usually at least three months of treatment is needed. Side-effects may include itching, redness and a rash.
Another cream which is sometimes used contains a medicine called fluorouracil. This kills the abnormal cells and fresh normal skin grows back. This cream is usually applied for 3-4 weeks but it can cause significant (but temporary) inflammation, soreness and blistering of surrounding skin. Fluorouracil cream is often used if someone has several actinic keratoses.
Imiquimod cream is an alternative. There are two strengths of imiquimod. One type (Aldara®) is applied three times per week for a month initially. After a four-week break, the response of the skin treated is reassessed. Sometimes it is necessary to repeat one further four-week course. The other type (Zyclara®) is applied once daily for two weeks, followed by a two-week break, and then once daily for a further two weeks. Imiquimod may also cause inflammation, irritation or redness of the skin where it is applied.
Salicylic acid ointment is another cream that is sometimes used. It may be used alone or in a combination cream with fluorouracil, called Actikerall®.
Photodynamic therapy
Photodynamic therapy is an alternative to topical treatments. It is used in conjunction with a cream called methyl-5-aminolevulinate (Metvix®). This cream is sensitive to light (photosensitive).
A particular light is focused on the area to be treated. The combination of the cream and the light helps to kill the abnormal cells. This form of treatment may be useful if there are a large number of actinic keratoses, or if the keratoses are around the eyes or where healing of the skin may be more difficult (such as the lower part of the leg). It may also be used if other treatments have not been successful.
Other treatments
An actinic keratosis may be cut or scraped off. This is usually done after numbing the skin with some local anaesthetic. Other treatments which are sometimes used can include laser surgery, chemical peels and dermabrasion (where skin surface is removed by abrasion).
Other risks if you have an actinic keratosis
Back to contentsIn people with one or more actinic keratoses it is a marker that they have had a lot of sun exposure. The most serious type of skin cancer, melanoma, usually occurs in people who have had a lot of sun exposure.
So, although an actinic keratosis does not progress into a melanoma, people with an actinic keratosis have an increased risk of developing a melanoma on some other part of their skin.
Medical advice should therefore be sought if there are other changes on the skin, such as new moles, small dark patches developing, or a change in an existing mole (for example, if it is getting bigger, has an irregular outline, or is bleeding or crusting.)
Can actinic keratoses be prevented?
Back to contentsSpending a lot of time in the sun increases the risk of developing actinic keratoses and skin cancer. It will also prematurely age the skin and cause wrinkles.
To reduce the risk of developing skin cancers, actinic keratoses and other conditions associated with sun-damaged skin, everyone should:
Stay out of strong sunlight. In particular, avoid sun between 11 am and 3 pm.
When out in the sun:
Seek natural shade in the form of trees or other shelter.
Wear clothes as a sunscreen, including T-shirts, long-sleeved shirts, and hats.
Use a broad-spectrum sunscreen with an SPF of 30 or higher to protect skin against UVB and UVA.
Reapply sunscreen regularly, particularly if swimming, sweating a lot, or after towelling dry.
Use plenty of sunscreen. At the very least, six full teaspoons are needed to cover the body of an average adult.
What is the outlook for people with actinic keratosis?
Back to contentsThe outlook for people with actinic keratosis is good. Most people with actinic keratosis do not develop skin cancer, and there are effective treatments to remove patches of actinic keratosis.
Actinic keratoses can come back, or develop in new areas, after treatment. If this happens, they can be treated again.
Actinic keratoses develop due to long-term sun exposure. Because people with actinic keratosis have had sustained sun damage to their skin, they have a higher risk of developing other types of skin cancers in their lifetime.
This means it's even more important to watch for any signs of skin cancer, and see a doctor as soon as possible if you notice them. Possible signs of skin cancer include:
New or unusual-looking moles.
Moles that have changed in size, shape, colour, or texture.
Moles that have an irregular shape, irregular borders, more than two colours.
Moles or other skin problems that are itchy, painful, sore, scabbing or bleeding.
Open sores on the skin that do not heal within a few weeks.
Growths on the skin.
Patient picks for Skin rashes

Skin, nail and hair health
Purpura
Because there are so many causes for purpura, diagnosing the reason why you have developed a purpuric rash takes a bit of detective work.
by Dr Hayley Willacy, FRCGP

Skin, nail and hair health
Bowen's disease
Bowen's disease is a very early form of skin cancer. It causes one or more small patches of scaly red skin. It occurs when skin cancer cells grow in the outer layer of the skin, but don't spread any deeper into the skin, or elsewhere in the body. Because these cancer cells stay in the outer layer of the skin, they don't cause serious problems in themselves. However, over time, there is a chance that these cells can develop into a different type of skin cancer, which can cause problems. So, Bowen's disease is generally treated to stop this happening. Close follow-up is needed after treatment to check for any return (recurrence) of Bowen's disease.
by Dr Doug McKechnie, MRCGP
Further reading and references
- Photodynamic therapy for non-melanoma skin tumours (including premalignant and primary non-metastatic skin lesions); NICE Interventional procedure guidance, February 2006
- Actinic keratosis; DermNet NZ
- Werner RN, Stockfleth E, Connolly SM, et al; Evidence- and consensus-based (S3) Guidelines for the Treatment of Actinic Keratosis - International League of Dermatological Societies in cooperation with the European Dermatology Forum - Short version. J Eur Acad Dermatol Venereol. 2015 Nov;29(11):2069-79. doi: 10.1111/jdv.13180. Epub 2015 Sep 14.
- Del Rosso JQ, Kircik L, Goldenberg G, et al; Comprehensive management of actinic keratoses: practical integration of available therapies with a review of a newer treatment approach. J Clin Aesthet Dermatol. 2014 Sep;7(9 Suppl S2-S12):S2-S12.
- British Association of Dermatologists guidelines for the care of patients with actinic keratosis 2017; British Association of Dermatologists (2017)
- Muse ME, Crane JS; Actinic Cheilitis.
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 19 Jan 2028
20 Jan 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.