Melanoma skin cancer
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 11 Aug 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Melanoma (also called malignant melanoma) is the most serious type of skin cancer. It affects young adults as well as older people. It can be caused by too much sun exposure, but sometimes even people who haven't had much sun get melanoma too.
The treatment for melanoma is mainly surgical but other treatments, including chemotherapy and radiotherapy, are increasingly used, especially if it is not possible to remove all the melanoma or if the melanoma is diagnosed at a relatively late stage.
At a glance
Melanoma is a type of skin cancer and is the 5th most common cancer in the UK.
About 6 out of 10 cases of melanoma are thought to be caused by sun exposure.
Risk factors include fair skin, a family history, and using sunbeds.
Look out for new moles that grow, or changes in existing moles, especially in size, border, or colour.
See a doctor if you have a skin lump or patch you are unsure about.
Diagnosis often involves a biopsy to remove the suspicious mole for examination.
Treatment can involve surgery, and sometimes radiotherapy, chemotherapy, or targeted therapies.
In this article:
Video picks for Skin cancer types
Continue reading below
How common is melanoma?
Melanoma skin cancer is the 5th most common cancer in the UK, accounting for about 4 in every 100 new cancer cases. There are around 16,700 new melanoma skin cancer cases in the UK every year. The number of cases has more than doubled over a period of 30 years or so, partly because it is being picked up more easily by dermatologists and family doctors.
About 3 in 10 of all melanomas occur in those aged over 75 years. However, melanoma can affect young adults too, even people in their 20s and 30s.
What causes melanoma?
Back to contentsMelanoma has a number of causes: some of which you can do something about, others which are beyond your control.
Sun or sunbed damage to skin
In general, sunlight is good for you: it boosts your vitamin D levels and is also good for your emotional well-being. However too much sun, particularly getting sunburnt, is bad for you. In melanoma it is thought that 'intermittent' sun exposure is important: for example, getting a lot of sun just a few times a year; on holiday, for example, but then staying indoors, working in an office perhaps, for the rest of the year. Surprisingly, people who are outside most of the time, like gardeners, do not seem to be at an increased risk of melanoma, although they may be at increased risk of other types of skin cancer.
About 6 out of 10 cases of melanoma are thought to be caused by sun exposure. However, the picture is not that clear: some studies have shown that people in cold countries like Sweden have higher rates of melanoma than warm countries like Greece. On the other hand, sunny countries like Australia and Israel have high rates of melanoma. Some of this might be down to how accurate countries are at recording melanoma.
People most at risk of sunlight skin damage are people with fair skin - in particular, those with skin which always burns and never tans, red or blond hair, green or blue eyes. Melanoma is uncommon in dark-skinned people, as they have more protective melanin in their skin.
Children's skin is most vulnerable to damage. Sun exposure in childhood is the most damaging. People who had a lot of freckling in childhood, or had frequent or severe sunburn in childhood, are most at risk of developing melanoma as adults. (The damage to the skin can occur many years before a cancer actually develops.)
Being fair-skinned, pale and getting sunburnt on holiday are certainly risk factors for getting melanoma.
However, some people get melanoma without having had much sun exposure in their lives. For these people, the melanoma has developed because of a genetic mutation: this is beyond their control and there is nothing that can be done to prevent it.
Other risk factors
Other factors which increase the risk of developing melanoma include the following:
A family history. If a close blood relative develops melanoma then your risk is approximately doubled. This increased risk may be due to a shared family lifestyle of frequent sun exposure and/or having fair skin. It may also be due to inherited faulty genes. Around one in ten people with melanoma will have a relative who has also had a melanoma. Further research aims to clarify the role of these and other genes which may be involved. Gene testing for melanoma is not yet possible. As a rule, if you have a family history of melanoma you should take extra care to protect your skin from sun damage. Also, check your skin regularly for early signs of melanoma (see below).
Using sunbeds or similar tanning machines which emit UV light. Damage caused by sunbeds seems to be worse in people with red hair and freckles and also in young people under the age of 20 years.
Having a weakened immune system (for example, due to untreated HIV infection, or if you are taking immunosuppressive medicines, perhaps after an organ transplant) increases the chance of getting a melanoma.
Continue reading below
What are the signs of melanoma?
Back to contentsMelanomas generally grow from fresh skin. They are a new mole that grows over a few months. Generally speaking if you've had a mole for years it is very unlikely to change into a melanoma. If a long-standing mole does change though, it's always best to get it checked by a doctor.
Melanomas can grow on skin that is very hard to see yourself: on the back of your shoulder blade, the sole of your foot, or in between your buttocks (what doctors call the 'natal cleft').
The features of a melanoma that are different from a benign mole include poorly defined edges, variations in colour and larger size.
Unfortunately not all melanomas are typical in appearance and it is sometimes hard to diagnose without being cut out.
Malignant melanoma on thigh
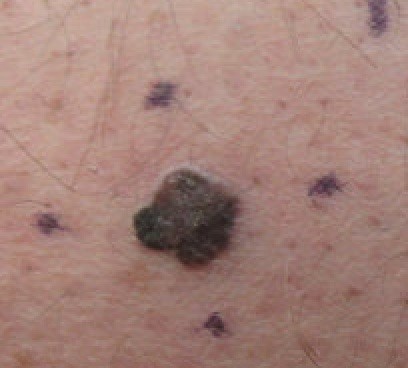
© Dermanonymous, CC BY-SA 4.0, via Wikimedia Commons
Some melanomas are not dark, some are nice and smooth to the naked eye, and a melanoma has to start somewhere, so at some point will have been small. Melanomas can be any size, although moles that are larger than 6 mm in size are more likely to be a melanoma.
The take home message is: see a doctor if you develop a lump or patch on the skin, which you are unsure about, or if a mole grows out of fresh skin and you are worried about it.
A melanoma can develop on any area of skin. The most common place for a melanoma to develop in a woman is on the legs; whereas for men it is on the chest or back. Rarely, a melanoma can develop in the iris or back of the eye: this might be noticed by an optician at a routine eye check, but will not cause any problems with your vision.
If some cells break off and spread (metastasise) to other parts of the body, various other symptoms can develop. A common early symptom of spread is for the nearby lymph glands (nodes) to swell.
The situation is complicated further by the fact that some melanomas can spread to the lymph nodes and then fade and disappear from the skin (what doctors call 'regression').
This is all in direct contrast to skin cancer that isn't melanoma: squamous cell carcinoma and basal cell carcinomas. For these, they are easier to diagnose and have a typical appearance that will be familiar to most family doctors. The role of sun exposure is also much more straightforward for basal cell carcinomas. You can read more about these more common skin cancers in the separate leaflet called Non-melanoma skin cancer.
How is a melanoma diagnosed?
Back to contentsDiagnosing melanoma with the naked eye is very hard and there are no particularly accurate ways to do it. Two scoring systems have been developed which can help guide patients and doctors as to whether a mole needs to be seen by a specialist:
The ABCDE rule:
Asymmetry of a mole (not being a circle, or an oval).
Border irregularity (instead of having a smooth outline).
Colour being uneven (instead of one colour all over).
Diameter more than 6 mm.
E stands for evolving (a mole that is changing or getting bigger) or expert: see an expert if you're worried.
The National Institute for Health and Care Excellence (NICE) recommends that the 7-point checklist is used to assess whether a pigmented skin lesion may be a melanoma:
The three major features of change in size; an irregular border; or an irregular colour.
And the four minor features of a size more than 7 mm; inflammation of a mole (where it gets red); oozing or crusting; and a change in sensation or itch.
However, some melanomas scores very low on these checklists and so you might be falsely reassured; on the other hand some completely harmless moles or bumps score very highly and don't need cutting out.
Most skin specialists, and some family doctors, use a handheld microscope called a dermatoscope to help diagnose melanoma. By looking closely at a mole through the dermatoscope a doctor can quite confidently 'rule out' melanoma and tell you the mole is harmless. If the dermatoscope shows a suspicious mole then most specialists will advise to have it cut out (excised).
If a melanoma is suspected then your doctor is likely to advise an excisional biopsy (where the mole and some surrounding skin will be cut out, with the skin numbed so it doesn't hurt).
Some family doctors (GPs) have the skills to do this, but in the UK generally a family doctor will refer you to a skin specialist (a dermatologist) or a plastic surgeon (who is an expert at cutting out skin problems).
In this procedure, the entire abnormal area of skin is removed by a minor operation. (Local anaesthetic is injected into the skin to make this painless.) This tissue is looked at under the microscope. This is to:
Confirm the diagnosis - abnormal melanoma cells can be seen.
Assess the melanoma's thickness (how deep it has spread into the skin). The thickness of the melanoma helps to guide treatment and the need for further assessment.
Some pharmacists and supermarkets offer you a 'skin check' using cameras to see if you have skin cancer. These are not accurate and may do more harm than good, by suggesting to you that you have skin cancer when you don't. They are best avoided. Instead, if you are worried about a mole, see your doctor.
Continue reading below
Melanoma initial treatment and assessment
Back to contentsThe excisional biopsy may be curative
When doing an excisional biopsy (described above) the doctor will remove a margin of normal skin around the melanoma. When the biopsy is looked at under the microscope, if the doctor is sure that all the melanoma cells have been removed and the melanoma cells are confined to the top layer of skin, no further treatment may be needed. Otherwise, a second operation called a wide local excision is usually advised.
Wide local excision may be needed
This aims to remove an area of normal skin around where the melanoma had been (before it was removed with excisional biopsy). This aims to make sure that any cells which may have grown in the local area of skin have been removed. The amount of normal-looking skin removed varies - depending on the thickness of the melanoma (how deep it has spread into the skin) as reported from the biopsy. It may be 1-2 cm around where the melanoma had been. This operation may be done under local or general anaesthetic. In some cases a skin graft may be needed to cover the wound.
Staging of melanoma
The aim of staging is to find out how much a cancer has grown and spread. Finding out the stage of the cancer helps doctors to advise on the best treatment options. It also gives a reasonable indication of outlook (prognosis). See the separate leaflet called Cancer for more details.
Most cases of melanoma are diagnosed at stage 1 when there is a very good chance that simply cutting out the melanoma fully will cure the condition. Other stages (2-4) are diagnosed if the tumour has spread. The stage diagnosed depends on how much and how far the original tumour has spread to other parts of the body.
How is melanoma assessed and staged?
If the initial biopsy and the tissue taken from the wide local excision show that the melanoma is just in the very top layer of skin then no further tests are usually needed. It is highly unlikely that it will have spread. This is an early stage 1 melanoma.
A doctor will examine you to see if you have any swollen lymph glands (nodes) near to the melanoma. If you have, the melanoma may have spread to these local lymph nodes.
It is possible that there may be some early spread without causing symptoms if the melanoma is thicker on the initial biopsy. In particular, there may be spread of some cells to the nearest lymph node without it yet causing it to swell. Therefore, a test called sentinel lymph node biopsy, and sometimes other tests, may be advised.
Sentinel lymph node biopsy
This is a procedure in which the lymph node nearest to the melanoma is removed. For example, if you have melanoma on your leg, the surgeon will take out a lymph node up in your groin. The idea is to see if the melanoma has spread up to the lymph nodes; this can give an idea of the prognosis. Removing the lymph node doesn't make the survival rates any better.
Further tests
Cancer specialists (oncologists) will organise detailed scans if you have been diagnosed with melanoma. These scans can see if the melanoma has spread elsewhere in your body.
What is the treatment for melanoma?
Back to contentsCutting out the melanoma may be all that is needed if it hasn't spread yet. This is very good news and all that is required afterwards is for a skin specialist to keep a close eye on you in the future.
If the melanoma has spread to the lymph nodes or to other organs inside the body (like the liver) then things are more complicated.
Until recently, there was no recommended additional treatment for melanoma that has been completely cut out and that hasn't spread. However, as with other cancers, even if a cancer has been completely cut out, it is possible that microscopic tumour cells have been missed.
Traditional treatments for cancer, like radiotherapy and chemotherapy, are now increasingly used to treat melanoma. Studies have looked at 'adjuvant' treatment. This is medication given after a main treatment to destroy any microscopic cancer cells and cut the chance of the cancer coming back.
There are also several 'targeted' treatments and immunotherapy treatments, which are newer drugs and may be suitable for some people with melanoma.
NICE now recommends various medicines that can be used for some people with melanoma, particularly for people with more advanced stages of melanoma.
You can read more about these treatments in the articles in Further Reading, below.
What is the outlook for melanoma?
Back to contentsThe outlook (prognosis) for people with malignant melanomas has been improving over a period of 25 years and people with melanomas. Almost 9 in 10 people diagnosed with melanoma skin cancer in England survive their disease for ten years or more.
The outlook depends on the stage. Most cases of stage 1 melanoma are cured with a minor surgical operation to remove the tumour (described above). For people with deeper melanomas then there is still a chance of cure. People with advanced melanoma that has spread to other parts of the body are not likely to be cured. However, treatment can often slow down the progression of the cancer.
The treatment of cancer is a developing area of medicine. New treatments continue to be developed and the information on outlook above is very general. The specialist who knows your case can give more accurate information about your particular outlook and how well your type and stage of cancer are likely to respond to treatment.
Can melanoma be prevented?
Back to contentsNo one can prevent melanoma entirely: sometimes it happens because of a genetic mutation, which is beyond your control. However, some melanomas are related to sunlight and here are some tips to help prevent it:
You should never use tanning beds or artificial tanning machines: they expose your skin to very strong UV light and have been linked to skin cancer.
Staying indoors or in the shade as much as possible between 11 am and 3 pm.
Try not to get sunburnt at all.
Covering up with clothes and a wide-brimmed hat when out in the sunshine.
Applying sunscreen with a sun protection factor (SPF) of 15 (SPF 30 for children or people with pale skin) which also has high ultraviolet A (UVA) protection.
These tips are particularly relevant to children and teenagers - particularly teenagers who might be tempted to use sun tanning booths: don't do it.
However, avoiding all sunlight is generally not a good idea and, even if you have a family history of melanoma, probably won't reduce your risk to zero. Insufficient sunlight may particularly reduce the level of vitamin D in your body and cause vitamin D deficiency.
You can read more about preventing skin cancer in the separate leaflet called Preventing skin cancer.
Patient picks for Skin cancer types

Cancer
Skin cancer types
This leaflet gives a general overview about skin cancer and the different skin cancer types - melanoma and non-melanoma.
by Dr Toni Hazell, MRCGP

Cancer
Preventing skin cancer
Some skin cancers can be partly prevented by protecting yourself from the sun, not smoking, and generally taking care of your health. Some kinds of skin cancer can't be prevented however, because they are caused by something going wrong in your genes: this is beyond your control.
by Dr Oliver Starr, MRCGP
Frequently asked questions
Does melanoma only affect older people, or can young adults get it too?
While about 3 in 10 melanomas occur in those aged over 75 years, it can also affect young adults. This includes people in their 20s and 30s.
Can I get melanoma if I don't spend much time in the sun?
Yes, some people develop melanoma without having had much sun exposure. In these cases, it is thought to be caused by a genetic mutation that is beyond their control.
How can I tell if a mole or new patch on my skin is a melanoma?
Melanomas usually grow as a new mole over a few months. Key features that differentiate a melanoma from a benign mole include asymmetry, irregular borders, uneven colour, and a diameter larger than 6 mm. A mole that is changing or getting bigger, or any new lump or patch that you are unsure about, should be checked by a doctor.
Are there specific areas on the body where melanoma is more likely to develop?
Melanoma can develop anywhere on the skin. In women, the legs are the most common site, while in men, it's typically the chest or back. They can also appear in hard-to-see areas like the back of the shoulder blade, the sole of the foot, or between the buttocks. Rarely, melanoma can develop in the iris or back of the eye.
What happens after a doctor suspects a mole might be melanoma?
If melanoma is suspected, your doctor will likely advise an excisional biopsy, where the mole and some surrounding skin are removed under local anaesthetic. This tissue is then examined under a microscope to confirm the diagnosis and assess the melanoma's thickness, which helps guide further treatment.
Are 'skin check' services using cameras, offered by some pharmacies or supermarkets, reliable for detecting melanoma?
No, these 'skin check' services using cameras are not considered accurate and may be misleading. It is best to avoid them. If you are concerned about a mole, you should see your doctor directly.
What is the general outlook for someone diagnosed with melanoma?
The outlook for people with melanoma has been improving, with almost 9 in 10 people diagnosed in England surviving their disease for ten years or more. Most early stage 1 melanomas are cured with surgery. While deeper melanomas still have a chance of cure, advanced melanoma that has spread to other parts of the body is less likely to be cured, though treatment can often slow its progression.
Further reading and references
- Vemurafenib for treating locally advanced or metastatic BRAF V600 mutation‑positive malignant melanoma; NICE Technology appraisal guidance, December 2012 - last updated January 2015
- Ipilimumab for previously treated advanced (unresectable or metastatic) melanoma; NICE Technology appraisal guidance, December 2012
- Electrochemotherapy for metastases in the skin from tumours of non-skin origin; NICE Interventional procedure guidance, March 2013
- Dabrafenib for treating unresectable or metastatic BRAF V600 mutation‑positive melanoma; NICE Technology Appraisal Guidance, October 2014
- Suspected cancer: recognition and referral; NICE guideline (2015 - last updated April 2026)
- Melanoma: assessment and management; NICE Guidance (July 2015 - last updated July 2022)
- Melanoma; DermNet NZ
- Pembrolizumab for advanced melanoma not previously treated with ipilimumab; NICE Technology appraisal guidance, November 2015
- Nivolumab for treating advanced (unresectable or metastatic) melanoma; NICE Technology appraisal guidance, February 2016
- Trametinib in combination with dabrafenib for treating unresectable or metastatic melanoma; NICE Technology appraisal guidance, June 2016
- Talimogene laherparepvec for treating unresectable metastatic melanoma; NICE Technology Appraisal Guidance, September 2016
- Cutaneous melanoma; Scottish Intercollegiate Guidelines Network (January 2017)
- Melanoma; NICE CKS, July 2022 (UK access only)
- Dabrafenib with trametinib for adjuvant treatment of resected BRAF V600 mutation-positive melanoma; NICE Technology appraisal guidance, October 2018
- Nivolumab for adjuvant treatment of completely resected melanoma with lymph node involvement or metastatic disease; NICE Technology appraisal guidance, March 2021
- Nivolumab in combination with ipilimumab for treating advanced melanoma; NICE Technology appraisal guidance, July 2016
- Encorafenib with binimetinib for unresectable or metastatic BRAF V600 mutation-positive melanoma; NICE Technology appraisal guidance, February 2019
Continue reading below
About the authorView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 10 Aug 2028
11 Aug 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.