Mediastinoscopy
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Laurence KnottLast updated 17 Feb 2019
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
This page has been archived.
It has not been reviewed recently and is not up to date. External links and references may no longer work.
Mediastinoscopy is a type of 'keyhole' surgery that allows doctors to look inside the chest. It can be used to take samples of body tissue for further testing.
Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
In this article:
Video picks for Imaging
Continue reading below
What is mediastinoscopy?
Mediastinoscopy involves a small operation to look at an area of the body, called the mediastinum. The mediastinum is part of the chest and contains the heart, gullet (oesophagus), windpipe (trachea) and various nerves. It is the area shown in purple in the image below.
Mediastinum
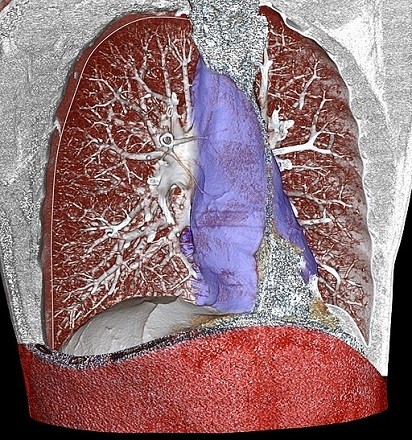
© By Mikael Häggström (Own work), via Wikimedia Commons
The mediastinum also contains lymph nodes and the thymus. Both of these are part of the immune system and help in fighting infection.
Mediastinoscopy is a type of 'keyhole' surgery where only very small cuts (incisions) are made to the body. It uses a special instrument called a mediastinoscope. This is a thin, tube-like instrument which has a camera built into the end. The 'scope' is inserted into a small incision in the upper chest. This is then linked up to a monitor, allowing the surgeon to see pictures of the chest.
While looking at these pictures, the surgeon may see something which they feel needs investigating further. Using the mediastinoscope they can take very small samples from within the chest. These can then be looked at further under a microscope.
What is mediastinoscopy used for?
Back to contentsThe most common reason for mediastinoscopy is as a staging procedure in the diagnosis of non-small cell lung carcinoma. The results obtained from the procedure are very important in tailoring care for the patient.
Other indications for mediastinoscopy include:
The diagnosis and removal of mediastinal masses and enlarged lymph nodes.
Lymphoma, both Hodgkins and non-Hodgkins, can be diagnosed via mediastinoscopy along with sarcoidosis which has similar appearances on imaging.
A mediastinal mass, such as a thymoma, may be removed using mediastinoscopy, depending on its size.
A sampling of lymph nodes may diagnose infectious processes such as tuberculosis and fungal infections.
Benign (non-cancerous) mediastinal cysts can be taken out using mediastinoscopy.
Mediastinoscopy is used in the diagnosis and treatment of mesothelioma.
Continue reading below
How does mediastinoscopy work?
Back to contentsBefore the operation, a small needle will be placed into a vein (usually on the back of the hand) to give you fluids and medication.
Mediastinoscopy is generally done under general anaesthetic, meaning that you will be asleep for the procedure. After you are asleep, a tube (an endotracheal tube - also called an ET tube) will be placed in your throat to help you breathe during the procedure. Your neck and chest will be washed with an antiseptic soap and covered with a sterile drape.
The surgeon may make two or three small cuts (incisions) in the chest wall above the breastbone (sternum). These holes are known as 'ports' and are usually about an inch long. The mediastinoscope is inserted through one hole. The camera in the mediastinoscope feeds video images to a computer screen, allowing the surgeon to see inside the chest.
Your doctor will also insert special surgical instruments through the other ports. He or she will examine the space in your chest between your lungs and heart. Lymph nodes or abnormal tissue samples will be collected and sent to the laboratory for further tests. After the 'scope' is removed from your chest, all these incisions will be closed with a few stitches and covered with a bandage.The entire procedure usually takes about an hour.
What should I do to prepare for mediastinoscopy?
Back to contentsYour doctor should discuss any specific preparation necessary with you before the procedure. Usually there is not much preparation necessary.
Note: if you take 'blood-thinning' medicines such as warfarin or aspirin, your doctor may ask you to stop taking these for a few days before your operation.
You will also be asked not to eat or drink for a certain length of time before the procedure. Your local hospital will give you information on this.
Continue reading below
What can I expect after mediastinoscopy?
Back to contentsSome people may go home after the procedure if the general anaesthesia wears off and they are able to swallow fluids without gagging or choking. Other people may need to stay in hospital for one or two days. If your stitches are not the dissolving type, you will need to return to your doctor to have them removed.
You may have a slightly sore throat - this is normal and usually due to the tube used to help you breathe during the operation. The sites where the cuts (incisions) were made may be sore for a few days after the procedure.
Are there complications after mediastinoscopy?
Back to contentsMost people who have a mediastinoscopy do not develop any complications.
Sometimes the mediastinoscope can temporarily injure a nerve, which may cause hoarseness. This can occasionally be permanent.
In rare cases, bleeding complications might require a transfusion or larger chest surgery. Air leaks from the lung can also occur and occasionally require additional treatment. Usually this involves putting in a drainage tube between your ribs for a few days.
Rarely mediastinoscopy may cause a collapsed lung (pneumothorax) or damage to the gullet (oesophagus).
You should contact your doctor if you become unwell after a mediastinoscopy. In particular, if you have any of the following problems:
Bleeding from your stitches.
A high temperature (fever).
Severe chest pain.
Swelling in the neck.
Shortness of breath.
Difficulty swallowing.
Hoarseness of your voice that lasts more than a few days or continues to worsen.
Advances in X-ray technology and surgical techniques mean that it may be possible to offer you options which cause less discomfort than mediastinoscopy.
Patient picks for Imaging

Tests and investigations
Cerebral angiography
Cerebral angiography is a test that uses X-rays and a special dye to create pictures of the blood vessels that supply the brain. Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
by Dr Mary Harding, MRCGP

Tests and investigations
CT scan
Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
by Dr Rachel Hudson, MRCGP
Further reading and references
- McNally PA, Arthur ME; Mediastinoscopy. StatPearls Publishing. 2018.
- Onat S, Ates G, Avci A, et al; The role of mediastinoscopy in the diagnosis of non-lung cancer diseases. Ther Clin Risk Manag. 2017 Jul 27;13:939-943. doi: 10.2147/TCRM.S144393. eCollection 2017.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
17 Feb 2019 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.