Bartholin's cyst and abscess
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Rachel Hudson, MRCGPLast updated 9 Oct 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Vulval problemsItchy vulvaLichen sclerosusVulvitis
Bartholin's glands are small glands that are just next to the lower part of the entrance to the vagina, one on each side. Each gland is about the size of a pea. Unless swollen or infected, you cannot normally see or feel these glands. They are within the soft tissues (labia) next to the vaginal opening.
Each gland makes a small amount of mucus-like fluid. The fluid from each gland drains down a short tube (duct) called the Bartholin's gland duct. Each duct is about 2 cm long and comes out towards the lower part of the opening of the vagina. The fluid helps to keep the entrance to the vagina moist.
At a glance
A Bartholin's cyst is a fluid-filled sac in one of the Bartholin's glands near the vaginal opening.
A cyst forms when the gland's fluid drainage tube becomes blocked, but the cause is often unclear.
Symptoms can include a painless lump, or discomfort if the cyst is larger.
If a cyst gets infected, it can become a very painful abscess, needing antibiotics.
See your GP for any lumps on your vulva or vagina to get a diagnosis.
Small cysts might not need treatment, but an abscess will likely need antibiotics.
Surgical procedures like marsupialisation can treat persistent cysts or abscesses.
In this article:
Video picks for Vaginal and vulval problems
Continue reading below
What is a Bartholin's cyst?
A Bartholin's cyst is a fluid-filled sac that develops in one of the Bartholin's glands. This fluid-filled swelling usually develops because the tube (duct) that drains the fluid has become blocked. The size of a cyst can vary from small and pea-like to the size of a golf ball - or even bigger in some cases. The cyst may remain the same size or may slowly become bigger. The reason why a Bartholin's duct may become blocked and lead to a cyst is not clear.
A Bartholin's cyst or abscess typically only develops on one of the two glands.
Symptoms of a Bartholin's cyst include:
A small lump to one side at the lower end of the entrance to the vagina (just inside the labia minora) may be felt, which may cause no problems.
A larger cyst may cause some pain and discomfort - particularly when walking, sitting or having sex.
Cysts that remain small and do not become infected may cause no symptoms at all.
With a Bartholin's abscess:
A lump develops and quickly becomes bigger, typically over a few hours or days.
It is likely to become very painful.
There may be a build-up of white or yellow pus in the gland.
There may be other symptoms of feeling generally unwell and have a high temperature; the skin over the abscess tends to become red, hot and very tender.
The tender swelling makes it painful to sit down, to walk or to have sex.
Some women may also have some vaginal discharge.
Bartholins cyst
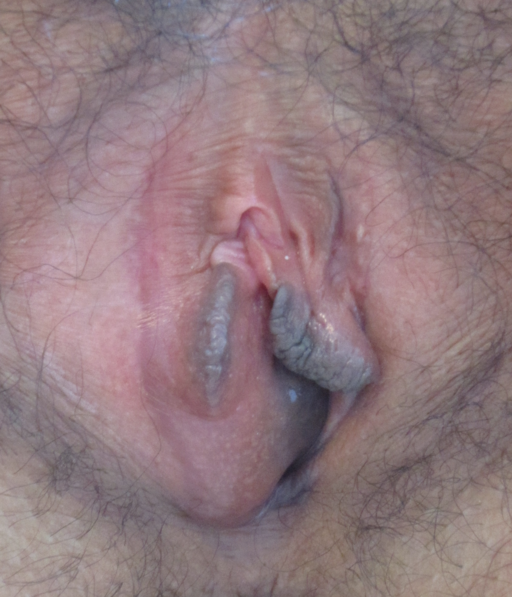
© Medimage, CC BY-SA 3.0, via Wikimedia Commons
What is a Bartholin's cyst?
Complications of a Bartholin's cyst
Back to contentsBartholin's abscess
If a Bartholin's cyst becomes infected then an abscess (known as a Bartholin's abscess) can develop. An abscess is a collection of pus that can occur with an infection. Sometimes the gland itself becomes infected and forms into an abscess. Within a few days, the abscess can become the size of a hen's egg and is usually very painful.
Many types of germs (bacteria) can infect a Bartholin's cyst or gland to cause an abscess. Most are the common germs that cause skin or urine infections, such as Staphylococcus (which lives on the skin normally) and Escherichia coli (which lives in the gut normally). Some cases are due to sexually transmitted infections (STI's) such as gonorrhoea or chlamydia.
Bartholin's gland cancer
This is a very rare cancer and is very unlikely in women aged under 40. However, if there is any doubt about the cause of the swelling, a small sample of tissue (biopsy) can be checked.
Continue reading below
How common are Bartholin's cysts and abscesses?
Back to contentsAbout three in 100 women will develop a fluid-filled swelling (Bartholin's cyst) or a collection of pus (Bartholin's abscess) at some point in their lives. Most cases occur without warning in women aged between 20 and 30. However, they can also occur in older or younger women.
How is a Bartholin's cyst caused?
What does a Bartholin's cyst look like?
How are Bartholin's cysts or abscesses diagnosed?
Back to contentsIf you find a lump on your vulva or vagina you should contact your GP surgery. An examination by a clinician in general practice can usually diagnose the problem. A Bartholin's cyst and abscess have a typical appearance. No test is usually needed to make the diagnosis.
Occasionally, a sample of the pus inside an abscess may be taken (a swab). This is sent to the laboratory to find out which germs are causing the infection. This helps the doctors choose the right antibiotics if these are needed.
Continue reading below
Bartholin's cyst treatment
Back to contentsTreatment is not always required for a Bartholin's cyst, but an abscess will often require antibiotics, and sometimes a surgical procedure.
How do you treat a Bartholin's cyst?
A small Bartholin's cyst that causes no symptoms is ideally left alone. However, new lumps in the vagina or vulva should usually be examined by a nurse or doctor to check that there is not another cause.
If the cyst is big enough to cause symptoms then a referral can be made to a gynaecology specialist and it can be operated on to remove the cyst and prevent its recurrence. This a procedure known as "marsupialisation".
A Bartholin's abscess will almost always need treatment with antibiotics as it can be very painful. If an abscess is left for long enough without treatment it is likely to burst and then may resolve without treatment; however this would not be recommended as it can be very painful and it is possible to become unwell due to the infection spreading.
Antibiotic medicines for an infection or abscess
A course of antibiotics may cure an abscess. However, the more pus that forms, the larger the abscess and the less chance that antibiotics alone will be sufficient to clear the abscess. In large abscesses, it may be necessary to drain the pus. Where this is done, antibiotics may or may not also be needed.
Marsupialisation
A small operation called marsupialisation is the traditional treatment used to treat a Bartholin's cyst or abscess. It is usually done under general anaesthetic but can also be done under local anaesthetic when the overlying skin is numbed with an injection of local anaesthetic.
A small cut (incision) is made into the cyst or abscess just inside the entrance to the vagina. Any fluid or pus drains out. The cut is widened to about 1 cm. A few stitches are then used to stitch the inside lining of the cyst to the overlying skin. This then creates a small new permanent opening for fluid to drain out of the gland.
Initially, the opening that is left is like a pouch - hence the name of the operation. However, the opening gradually becomes smaller and soon the opening becomes tiny and not noticeable. This new opening becomes a new tube (duct) which allows any fluid that is made by the gland to drain.
A course of antibiotics may be prescribed if pus is drained from an abscess. However, antibiotics are not always needed once the pus has been drained.
Marsupialisation is usually successful and it is rare for the problem to recur if this procedure is done. If a simple cut is made to drain the fluid or pus without then doing a marsupialisation, there is a higher chance that the problem will come back at some point.
As with all operations there is a small chance of problems. For example, infection of the wound can occur in a small number of cases following marsupialisation.
Other types of operation
In recent years, various other procedures have been introduced which are sometimes used instead of marsupialisation. For example:
Insertion of a Word catheter. This is a small, thin rubber tube. The head of the catheter is inserted through a small cut made into the cyst or abscess. The tip of the catheter has a tiny balloon which is blown up to keep the catheter in place for 2-6 weeks. Whilst the catheter is in place it is possible to continue activities as normal. The aim is to keep the opening from closing up. As the tissues heal, it allows the cells to form a new tube (duct) over the catheter.
Insertion of a Jacobi ring. This too is a thin catheter that is passed into the cyst or abscess through one small cut and out from a separate cut. The two ends of the catheter are tied together with a silk thread that goes through the middle of the catheter. As with a Word catheter, this is left in place for a few weeks to allow a new duct to form.
The operation chosen depends on factors such as the size of the cyst or abscess and the preference and expertise of the surgeon. They all usually work well, with a low rate of recurrence. Evidence suggests that there is no benefit of one particular procedure over the others.
Other techniques
With a Bartholin's cyst that is uncomfortable or painful, sitting in a few inches of warm water (easiest in a bath), for 10-15 minutes, three or four times a day, may encourage the cyst to burst naturally. It is not clear how well this may work. A sitz bath can be used in the same way (a bath where someone can sit in warm water which reaches to the hips).
Will it happen again?
Back to contentsIn most cases, a Bartholin's fluid-filled swelling (cyst) or collection of pus (abscess) does not happen again after treatment with one of the operations described above. If antibiotics alone cured the problem, or if the abscess is simply drained, there is a chance of it happening again at some point. Treatment may need to be repeated or another type of treatment used.
Cases due to sexually transmitted infections
Back to contentsWith a Bartholin's abscess, a swab (a small ball of cotton wool on the end of a thin stick, used to take a sample) of the area or a sample of pus is sometimes sent to the laboratory. This is to identify which germ (bacterium) caused the infection. If a sexually transmitted infection is found to be the cause then further screening for other sexually transmitted infections will usually be advised.
Can Bartholin's cysts or abscesses be prevented?
Back to contentsBartholin's cysts and abscesses cannot usually be prevented. Most occur 'out of the blue' for no apparent reason. It is important to keep the area clean via good hygiene; however many abscesses occur even where hygiene is very good. Some Bartholin's abscesses are due to sexually transmitted infections and so using a condom when having sex may prevent some cases.
Patient picks for Vaginal and vulval problems

Women's health
Vulvitis
Vulvitis is an inflammation of your vulva. It is not a disease or an actual condition. It is very common and can occur in women of all ages. It has many different causes, as listed below. It is sometimes difficult to determine the cause of the vulvitis.
by Dr Rachel Hudson, MRCGP

Women's health
Vulval intraepithelial neoplasia
Vulval intraepithelial neoplasia (VIN) is a skin condition of the vulva. It is not a cancer, but it can turn into cancer if not treated.
by Dr Colin Tidy, MRCGP
Frequently asked questions
Can a Bartholin's cyst go away on its own without any medical treatment?
A small Bartholin's cyst that doesn't cause any symptoms is often left alone. If an abscess is left untreated for long enough, it might burst and resolve on its own, but this is not recommended as it can be very painful and the infection could spread. Sitting in warm water for 10-15 minutes, three or four times a day, might encourage an uncomfortable or painful cyst to burst naturally.
What should I do if I find a new lump in my vaginal or vulvar area?
If you notice a new lump on your vulva or vagina, you should contact your GP surgery. All new lumps should be examined by a nurse or doctor to ensure there isn't another underlying cause.
Are there any specific activities I should avoid if I have a Bartholin's cyst or abscess?
A larger cyst or an abscess can cause pain and discomfort when walking, sitting, or having sex. Therefore, it might be advisable to avoid these activities if they cause increased pain. If you have a Word catheter in place, you can usually continue normal activities as it aims to keep the opening from closing up.
How long does the recovery typically take after a marsupialisation procedure?
The article mentions that after marsupialisation, the opening initially looks like a pouch but gradually becomes smaller and unnoticeable. It doesn't specify a exact recovery time, but it implies a healing process over time as the opening forms a new duct.
Are there any alternative treatments to surgery for a Bartholin's cyst or abscess?
For an uncomfortable or painful Bartholin's cyst, sitting in warm water (sitz bath) for 10-15 minutes, three to four times a day, may encourage the cyst to burst. For an abscess, a course of antibiotics may cure it, especially if it's not too large. However, if there's a lot of pus, antibiotics alone might not be enough, and drainage may be needed.
Further reading and references
- Illingworth B, Stocking K, Showell M, et al; Evaluation of treatments for Bartholin's cyst or abscess: a systematic review. BJOG. 2020 May;127(6):671-678. doi: 10.1111/1471-0528.16079. Epub 2020 Feb 4.
Continue reading below
About the authorView full bio

Dr Rachel Hudson, MRCGP
General Practitioner and Medical Author
MBChB, MRCGP (2008), BSc (Medical Science), DFSRH, DRCOG, DCH
Dr Rachel Hudson, is an NHS GP working in the North West of England.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 8 Oct 2027
9 Oct 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.