Alopecia
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Philippa Vincent, MRCGPLast updated 12 Aug 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Alopecia areata article more useful, or one of our other health articles.
In this article:
What is alopecia?
Alopecia describes loss of hair from areas where hair normally grows. It comes in a variety of patterns with a variety of causes. The most common form is male pattern baldness, or androgenetic alopecia.
In all forms of acquired baldness, skin that has previously been protected may be subjected to strong sunlight. Hats should be worn to prevent burning and possibly later malignant change.
Alopecia areata bald spot
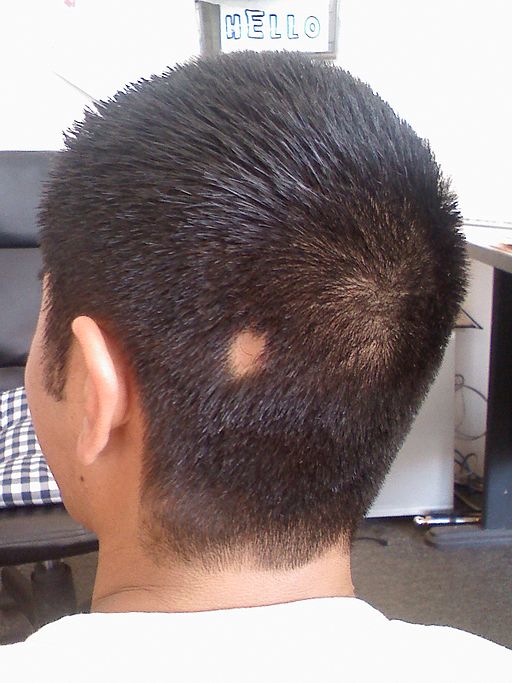
© Kevlaraz, CC0, via Wikimedia Commons
Kevlaraz, CC0, via Wikimedia Commons
Normal hair cycle1
Back to contentsEach follicle produces a number of hairs during a lifetime. There are three phases:
Anagen or growth phase on the scalp lasts between three and five years and the hair grows at approximately 1 cm a month. The duration of the anagen phase varies from person to person and it determines how long hair will grow if not cut. Usually about 85% is in anagen phase.
Catagen phase follows the anagen phase and is an involutional stage that lasts around two weeks.
Telogen, or dormant, phase lasts about three months. The hair remains in the follicle but does not grow.
At the end of the telogen phase the follicle starts production of new anagen hair.
Continue reading below
Causes of alopecia (aetiology)
Back to contentsThere are a number of types and patterns of alopecia. Aetiology, epidemiology and management will vary between them. Some of the more common forms of alopecia (further discussed below) are:
Male pattern baldness, or androgenetic alopecia (male).
Female pattern baldness, or androgenetic alopecia (female).
Alopecia areata.
Telogen effluvium (TE).
Anagen effluvium.
Trichotillomania.
Alopecia related to or caused by skin conditions or systemic illness, including:
Seborrhoeic dermatitis.
Lichen planus and discoid lupus erythematosus.
Tinea capitis.
Impetigo.
Secondary syphilis.
Thyroid disease.
Iron deficiency.
Determining the cause will guide management and prognosis.
Androgenetic alopecia - male pattern
Back to contentsThis is a characteristic pattern of balding in men, which becomes more common with age. There may be bitemporal recession and/or a central recession to produce a characteristic horseshoe shape of remaining hair.
Aetiology
Genetic predisposition via a number of different genes.
A number of mechanisms play a part. Hair follicles become smaller over time. Terminal hairs are gradually replaced by thinner hairs with less pigmentation. Hairs are in the anagen phase for less time and fewer hairs are in this growing phase. The end result is shorter hairs which do not reach the skin surface. Telogen hairs are more loosely attached and fall out more easily. Finally, there is increased time between telogen phase shedding and anagen phase regrowth.
Believed to be androgen-dependent; however, androgen levels in affected men are usually normal. The condition is a matter of end-organ sensitivity to androgens and men who are deficient on their head may have an abundance of hair over the rest of their bodies. Dermal cells convert testosterone into dihydrotestosterone. For reasons that are not clear, affected hair follicles become more sensitive to dihydrotestosterone, which then causes the hair follicles to shrink.
Epidemiology
Increasingly common with age.
Initial signs seen in teenage years.
Half of men are affected by the age of 50.
Rate of progression and severity of end result are extremely variable.
Significant ethnic variations - white men are affected four times more than those of Afro-Caribbean origin. Alopecia tends to occur later and more slowly in Asian men.
Management23
Doing nothing is likely to be the best treatment option. For many men, there is no effective affordable treatment; therefore, acceptance is the ideal management strategy. Counselling or support groups may be useful.
Aesthetic treatment options include wigs and hairpieces and surgical transplantation. The latter is expensive and not available on the NHS, although newer techniques result in improved results.
There are two pharmacological options approved for this condition. Neither is available on the NHS. There is a high rate of discontinuation of treatment due to lack of satisfaction with the results.
Minoxidil. Topical application of minoxidil twice daily, in either 2% or 5% form may be used. It is available over-the-counter or by private prescription. The stronger formulation may be more effective; it may, however, cause more irritation. Minoxidil is more likely to be effective in the early stages of balding than once it is established. It should be used for at least six months to establish efficacy and then used indefinitely in order to maintain any effect.
Finasteride. Oral finasteride in a dose of 1 mg daily may be effective. It is only available by private prescription. A trial of at least six months is needed and, if effective, treatment needs to be continued indefinitely. Side effects include gynaecomastia, testicular atrophy. There is a small but significant risk of adverse sexual side-effects (both erectile dysfunction and reduced libido). This may persist even after stopping the medication so very good counselling is required. There is also a risk of psychiatric side effects, including depression, self-harm and attempted suicide. It is also highly teratogenic, such that partners of men using this should not handle the medication if they are not using contraception and should not attempt to conceive. There is evidence of moderate efficacy.
Other options which have been used include dutasteride and low-level laser light therapy.45 Evidence is not yet sufficient for these, or for other miscellaneous options, as mainstream treatments.6
Continue reading below
Androgenetic alopecia - female pattern
Back to contentsThis is a characteristic pattern of hair loss in genetically predisposed women. There is a more diffuse hair loss than in men, particularly affecting the top of the scalp.
Aetiology
Terminal hairs are gradually replaced by smaller hairs with less pigmentation. Fewer hairs are in the anagen phase. Telogen hairs are more loosely attached and fall out more easily.
The genetic basis and the role of androgens are less well established than in male pattern hair loss.
There may be distinct early-onset and late-onset forms.
Epidemiology
Reported prevalence rates vary widely.
It increases after the menopause.
It affects around one third of white women over the age of 70.
There is ethnic variation with it being less common in women of Oriental origin.
Rate of progression is variable but women rarely go completely bald.
Management
Address fears of baldness.
Reassurance - total baldness is unlikely.
Note that terms such as "hair thinning" are more acceptable than "balding".
Encourage cosmetic improvements through hair styling, colouring and products.
Support groups or counselling may be of benefit.
Doing nothing is likely to be the best treatment option.
Aesthetic options include hair pieces, wigs and surgical transplantation. Surgery is expensive and not available on the NHS.
Topical 2% minoxidil is the only licensed pharmaceutical agent. It has to be applied twice-daily indefinitely. Response is modest and there may be side-effects (such as unwanted facial hair growth).
Finasteride should not be used in women.
Evidence is not sufficient to use anti-androgenic agents such as spironolactone, drospirenone and cyproterone.6
Alopecia areata78
Back to contentsAlopecia areata is a chronic inflammatory disease, which affects hair follicles and sometimes nails. The typical clinical presentation is with well-circumscribed bald patches on the scalp or beard area. There is no scarring or scaling on the skin. Exclamation mark hairs (short broken hairs tapering towards the proximal end) may be found around the margins and are said to be pathognomonic but not invariable. The more severe forms of alopecia areata are:
Alopecia totalis - total loss of scalp hair.
Alopecia universalis - total loss of all body hair.
Aetiology
This condition is of unknown aetiology, although there is much support for an autoimmune component. It is more common in acquired thyroid disease, vitiligo, diabetes and collagen diseases.
Stress is sometimes given as a factor but it may be that the disease is the cause rather than the result of stress. There is a tendency for it to run in families (especially the more severe cases) and it is linked to a variety of genes and gene complexes. Around 20% have a positive family history.
Epidemiology and natural disease course
Estimated prevalence in the UK is 15 per 10,000 of the population.
It can affect any age but onset is most common in childhood and adolescence. Incidence peaks between the ages of 15 and 29. 50-60% develop a first bald patch before the age of 21.
Males and females are affected equally.
There is nail involvement in 10-15%.
Spontaneous remission occurs in up to 80%, although recurrence is the norm.
14-25% progress to alopecia totalis or alopecia universalis.
Severity at presentation is the best indicator of long-term outcome.
As well as severe disease, factors associated with a poorer prognosis include nail abnormalities, onset at a young age, extensive alopecia, involvement of the scalp margin, atopy and associated autoimmune disease.
Management
Assessment
Extent: over 50% hair loss is considered extensive and should prompt specialist referral.
Investigate further if there is suggestion of other autoimmune disease.
Explanation and education are important. Stress the high levels of spontaneous remission when considering treatment in milder cases.
No treatment option should be discussed and is appropriate if:
There is evidence of hair regrowth.
Treatment is not wanted.
There is less than 50% hair loss (unless the person affected wishes for treatment).
Primary care treatment options
For non-pregnant adults only.
Not for use on the face.
Trial of potent topical steroid - eg, betamethasone valerate 0.1%, fluocinolone acetonide 0.025% or hydrocortisone butyrate 0.1%.
Off-licence use of a very potent topical steroid - eg, clobetasol propionate 0.05% scalp application.
Warn of high failure rate of treatment and also that it may take at least three months to take effect.
Warn that if hair growth occurs, it initially may be fine and depigmented. It can be dyed with a non-peroxide-based dye while awaiting return to its usual colour.
Consider counselling and psychological support.
Specialist treatment options
Although a number of treatments have been shown to result in hair regrowth, none alter the long-term outcome. Response rates are generally poor. Options dermatologists may consider include:
Intralesional corticosteroids.
Topical corticosteroids.
Topical immunotherapy.
Topical minoxidil.
Topical dithranol
Topical or systemic psoralen plus ultraviolet A (PUVA) light therapy.
Oral ciclosporin.
Ritlecitinib. In May 2024, the National Institute for Clinical Effectiveness recommended
ritlecitinib as an option for treating severe alopecia areata in people 12 years and over. Evidence from clinical trials shows that it is more effective than placebo for improving hair regrowth for up to 24 weeks.9Dermatography (tattooing). Particularly effective for eyebrow loss.
Wigs. (Certain wigs can be prescribed on the NHS by a specialist. Human hair wigs are better but more expensive and only available on the NHS if there is a contra-indication to acrylic hair.)
Telogen effluvium1011
Back to contentsTelogen effluvium (TE) occurs when physiological or hormonal stress triggers many hairs to move into telogen phase. When new hairs appear in anagen phase they push out the telogen hairs; this is between one and six months (on average three months) after the initial insult. People with TE notice they are shedding more hair than usual and often present with handfuls of hair found on the pillow, on a brush or in the plughole.
This can be an acute or chronic condition but the chronic condition may go unnoticed. The acute condition may be precipitated by a variety of factors:
Childbirth. TE is estimated to affect one third to one half of women following childbirth. It is also called telogen gravidarum.
Crash dieting, anorexia nervosa or low protein intake.
Sudden weight loss or dietary restriction following bariatric surgery.
Iron deficiency.
Acute febrile illness or severe infection.
Major surgery and severe trauma.
Heavy metal poisoning, including selenium, arsenic and thallium.
Medication changes - eg, contraceptives, antidepressants.
Chronic diffuse telogen hair loss may be idiopathic (affecting women only) or may be secondary to an organic cause. Possible causes include:
Thyroid disease.
Iron-deficiency anaemia.
Chronic illness such as malignancy, particularly lymphoproliferative malignancy and any chronic debilitating illness, such as systemic lupus erythematosus, end-stage chronic kidney disease or liver failure.
Zinc deficiency.
Chronic starvation, malabsorption or hypoproteinaemia.
Medication, including beta-blockers, anticoagulants, retinoids, lithium, carbamazepine and immunisations.
Management is the correction of any matters that require attention (such as poor diet) and reassurance that hair will return in a matter of months. Minoxidil is occasionally prescribed for this condition.
Anagen effluvium12
Back to contentsAnagen effluvium occurs when hair production is arrested in the anagen phase. This mainly happens when cancer chemotherapy, immunosuppression or radiotherapy causes rapid hair loss. Doxorubicin and cyclophosphamide are especially notorious but most antimitotics can have this effect.
Rarely, anagen effluvium can be a feature of pemphigus vulgaris, or be caused by trauma, pressure or exposure to chemicals such as thallium, boron and arsenic.
Within a few months of stopping chemotherapy the hair will usually return. It can be very psychologically damaging for people in a vulnerable situation. Scarves, hairpieces and wigs may be useful. Patients undergoing cancer chemotherapy are entitled to free NHS wigs. If the treatment includes hormonal manipulation that may induce hot flushes, a wig may be very uncomfortable to wear. Minoxidil shortens the alopecia by about 50 days. Local cooling of the scalp may also be helpful.
Trichotillomania1314
Back to contentsTrichotillomania, or hair-pulling disorder, is a behavioural disorder which may have links with obsessive-compulsive disorder. It may be associated with other conditions, particularly mood and anxiety disorders. It can occur at any age, but starts most often in adolescence. Hair loss is asymmetrical and has an unusual shape, with broken hairs across the bald patch which are not easily removed. Single or multiple areas can be affected, including eyebrows, eyelashes and pubic hair. There is minimal or no inflammation.
Genetic and environmental factors have been implicated. It may be possible to see that the individual wraps the hair around a finger and pulls on it, perhaps when concentrating on something such as when studying. Most individuals report pleasurable feelings during or after pulling out hairs. There may be boredom, tension or anxiety before pulling episodes and a significant reduction in such negative emotions following pulling. Management involves behavioural modification.
This is classified as a psychiatric disorder but results in a form of traumatic alopecia. Traction alopecia can also occur with hairstyles that pull tightly on the hair and it may lead to frontal recession.
Trichobezoar (swallowing hair which forms a ball in the intestines) can be a complication.
Psychotherapy (specifically habit-reversal therapy) and cognitive behavioural therapy are usually first-line treatments with some evidence base. Unlicensed medications occasionally found to be helpful and which have been studied include:
Antidepressants of all classes.
Antipsychotics, particularly olanzapine.
N-acetylcysteine.
Opioids.
Anticonvulsants.
A Cochrane review found moderate evidence for efficacy of clomipramine, olanzapine and N-acetylcysteine but warned that results should be interpreted with caution due to the small number of studies and small size of those studies.
Other causes of alopecia
Back to contentsThere are a number of other conditions that can lead to loss of hair. These include:
Scalp conditions:
Infection - impetigo, boils, abscesses, tinea capitis (especially animal ringworm).
Psoriasis.
Seborrhoeic dermatitis - produces large amounts of dandruff and is often associated with thinning of hair.
Atopic dermatitis.
Trauma:
Traction alopecia can be caused by tight hairstyles and hair grooming devices such as curling irons and straighteners.
Scarring alopecia. Conditions causing alopecia that are associated with scarring of the skin are known collectively as cicatricial alopecia. These are rare and include:
Certain infections such as folliculitis, boils or tinea capitis.
Scleroderma.
Discoid lupus erythematosus.
Lichen planopilaris.
Secondary syphilis:
Causes a typical "moth-eaten" pattern of hair loss.15
Further reading and references
- Hair loss; DermNet NZ
- Qiao J, Fang H; Moth-eaten alopecia: a sign of secondary syphilis. CMAJ. 2013 Jan 8;185(1):61. doi: 10.1503/cmaj.120229. Epub 2012 Jul 3.
- Kimura-Ueki M, Oda Y, Oki J, et al; Hair Cycle Resting Phase Is Regulated by Cyclic Epithelial FGF18 Signaling. J Invest Dermatol. 2012 May;132(5):1338-45. doi: 10.1038/jid.2011.490. Epub 2012
- Evidence-based (S3) guideline for the treatment of androgenetic alopecia in women and in men – short version; European Academy of Dermatology and Venereology, 2017
- Adil A, Godwin M; The effectiveness of treatments for androgenetic alopecia: A systematic review and meta-analysis. J Am Acad Dermatol. 2017 Jul;77(1):136-141.e5. doi: 10.1016/j.jaad.2017.02.054. Epub 2017 Apr 7.
- Gubelin Harcha W, Barboza Martinez J, Tsai TF, et al; A randomized, active- and placebo-controlled study of the efficacy and safety of different doses of dutasteride versus placebo and finasteride in the treatment of male subjects with androgenetic alopecia. J Am Acad Dermatol. 2014 Mar;70(3):489-498.e3. doi: 10.1016/j.jaad.2013.10.049. Epub 2014 Jan 9.
- Avci P, Gupta GK, Clark J, et al; Low-level laser (light) therapy (LLLT) for treatment of hair loss. Lasers Surg Med. 2014 Feb;46(2):144-51. doi: 10.1002/lsm.22170. Epub 2013 Aug 23.
- Blumeyer A, Tosti A, Messenger A, et al; Evidence-based (S3) guideline for the treatment of androgenetic alopecia in women and in men. J Dtsch Dermatol Ges. 2011 Oct;9 Suppl 6:S1-57. doi: 10.1111/j.1610-0379.2011.07802.x.
- Guidelines for the management of alopecia areata; British Association of Dermatologists (2012)
- Alopecia areata; NICE CKS, March 2023 (UK access only)
- Ritlecitinib for treating severe alopecia areata in people 12 years and over; NICE Technology appraisal guidance, March 2024
- Grover C, Khurana A; Telogen effluvium. Indian J Dermatol Venereol Leprol. 2013 Sep-Oct;79(5):591-603. doi: 10.4103/0378-6323.116731.
- Werner B, Mulinari-Brenner F; Clinical and histological challenge in the differential diagnosis of diffuse alopecia: female androgenetic alopecia, telogen effluvium and alopecia areata--part II. An Bras Dermatol. 2012 Nov-Dec;87(6):884-90.
- Kanwar AJ, Narang T; Anagen effluvium. Indian J Dermatol Venereol Leprol. 2013 Sep-Oct;79(5):604-12. doi: 10.4103/0378-6323.116728.
- Rothbart R, Amos T, Siegfried N, et al; Pharmacotherapy for trichotillomania. Cochrane Database Syst Rev. 2013 Nov 8;11:CD007662. doi: 10.1002/14651858.CD007662.pub2.
- Snorrason I, Berlin GS, Lee HJ; Optimizing psychological interventions for trichotillomania (hair-pulling disorder): an update on current empirical status. Psychol Res Behav Manag. 2015 Apr 7;8:105-13. doi: 10.2147/PRBM.S53977. eCollection 2015.
- Qiao J, Fang H; Moth-eaten alopecia: a sign of secondary syphilis. CMAJ. 2013 Jan 8;185(1):61. doi: 10.1503/cmaj.120229. Epub 2012 Jul 3.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 11 Aug 2027
12 Aug 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free