Alopecia areata
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 13 Jul 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Alopecia areata is a condition where patches of hair loss develop, usually on the head. In some cases, total baldness develops. Usually the hair regrows after several months. In some cases, the hair loss is permanent. Treatments to promote hair regrowth work in some cases, but often the hair regrows of its own accord.
At a glance
Alopecia areata is a type of hair loss where bald patches appear, typically on the scalp.
It is an autoimmune condition where the body's immune system attacks hair follicles.
Hair often regrows by itself within a few months to a year, especially in mild cases.
Treatment options include steroid injections, topical creams, and, in some hospitals, immunotherapy.
Wigs and counselling can also be helpful for managing the condition.
In this article:
Video picks for Hair and scalp problems
Continue reading below
What is alopecia areata?
Alopecia means loss of hair or baldness. There are a few different types.
The most common type is alopecia areata where small patches of hair loss, often in circles, appear on the scalp.
There are other types, like alopecia universalis, where all the hair on the body (including the eyebrows, groin area and under the arms) disappears, or alopecia totalis, where all the hair on the head is lost. These are rarer than alopecia areata.
Diffuse alopecia is a condition where there is hair loss on the scalp which do not cause total hair loss as in alopecia totalis but also do not occur in patches. The hair loss is more widespread than in typical alopecia areata and is generalised but not complete. Diffuse alopecia areata is either caused by excessive hair shedding (telogen effluvium) or hair thinning (androgenic alopecia - male pattern baldness).
How common is alopecia areata?
Back to contentsIn the UK, alopecia areata is estimated to affect about 15 in 10,000 people.
Alopecia areata can occur at any age but about half of all cases occur in childhood and eight in ten cases start before the age of 40 years. Men and women are equally affected. The condition tends to be milder if it comes on at an older age.
A relative, friend or hairdresser may be the first person to notice the bald patch or patches.
Continue reading below
Alopecia areata symptoms
Back to contentsThe typical pattern is for one or more bald patches to appear on the scalp. These tend to be round in shape and about the size of a large coin. They develop quite quickly. Often the person with it hasn't noticed it at all, particularly if they have long hair which is covering the bald patch.
This photo shows a typical patch of alopecia areata on the back of a young man's head:
Alopecia areata on the back of the head
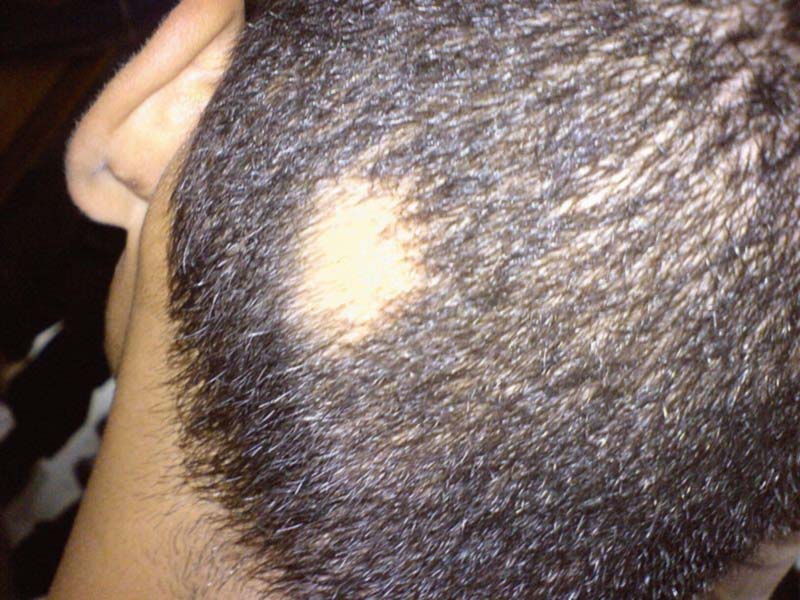
© By Abbassyma at English Wikipedia via Wikimedia Commons
This photo shows a patch of hair loss on a woman's head:
Alopecia areata on a woman's head
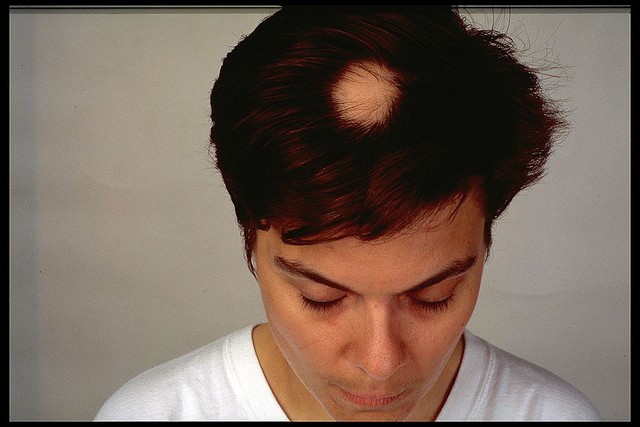
© By Carolyn P Speranza, CC BY 2.0, via Wikimedia Commons
When a bald patch first develops, it is difficult to predict what will happen. The following are the main ways it may progress:
Quite often the bald patch or patches regrow hair within a few months. If hair grows back, it may not have its usual colour at first and look grey or white for a while. The usual colour eventually returns after several months.
Sometimes one or more bald patches develop a few weeks after the first one. Sometimes the first bald patch is regrowing hair whilst a new bald patch is developing. It can then appear as if small bald patches rotate around different areas of the scalp over time.
Sometimes several small bald patches develop and merge into a larger bald area.
Patches of body hair, beard, eyebrows or eyelashes may be affected in some cases, but this is unusual.
Large bald patches develop in some people. Some people lose all their scalp hair. This is called alopecia totalis. This is rare.
In a small number of cases, all scalp hair, body hair, beard, eyebrows and eyelashes are lost. This is called alopecia universalis. Again, this is very rare.
The nails are affected in about 1 in 10 cases and can become pitted or ridged.
Is alopecia areata itchy?
Occasionally, there is some mild redness, mild scaling, mild burning or a slightly itchy feeling on the bald patches, but usually the person doesn't feel anything. Apart from the patch, the scalp usually looks healthy and there is no scarring.
Below shows a beard hair loss patch: this is quite common and usually grows back by itself.
Alopecia areata in the beard area
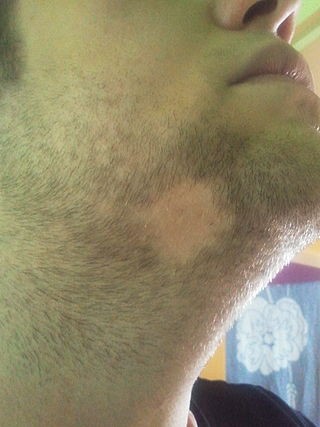
© By XxRoxettexX (Own work) via Wikimedia Commons
Understandably most people with alopecia areata become self-conscious or distressed by the appearance of the hair loss. However, the hair regrows by itself in almost all cases.
What causes alopecia areata?
Back to contentsAlopecia areata is an 'autoimmune disease'. This is one of those conditions where the body's immune system, which usually fights off germs, accidentally attacks itself.
Tiny cells in the immune system, called T cells, gather around the base of a hair follicle and try to kill it. This causes the hair to fall out. But at some point the immune attack usually comes to an end and the hair grows back.
Alopecia areata can be triggered by a recent illness, like a viral infection, or by taking certain medications for other medical conditions. Some people can link the onset of their alopecia to a stressful life event but many can't. Sometimes it seems to run in families and it has been known to come on in twins at the same time. More often than not, no cause is found at all.
People with alopecia areata have a slightly higher-than-average chance of developing other autoimmune diseases such as thyroid disease, pernicious anaemia and vitiligo. These will sometimes be tested for if there are any symptoms of them alongside the hair loss.
Continue reading below
Do I need any tests?
Back to contentsUsually no tests are needed. The diagnosis is usually based on the typical appearance of the bald patches. If there is doubt about the cause of the hair loss, sometimes some blood tests or a skin scraping from a bald patch may be done to rule out other causes (such as a fungal infection). A small sample of skin (skin biopsy) is sometimes taken to look at under the microscope.
Occasionally tests might be advised to check for other autoimmune diseases. For example, if there are certain other symptoms, blood tests might be used to check blood count and thyroid function. Usually blood tests come back entirely normal with alopecia areata.
What is the outlook for people with alopecia areata?
Back to contentsThankfully, mild cases of alopecia areata often get better without treatment within a few months to a year.
In some cases, patchy baldness may come and go over many months or years. The size of the bald patch or patches and how long they last are quite variable.
If less than half of the scalp is affected and no treatment is started, there is about an 80% chance of full hair regrowth within one year.
With more extensive hair loss, it is less likely that hair will regrow.
However, even if the hair grows back fully after an episode of alopecia areata, it is common to have one or more recurrences of the condition throughout life. A few people who develop alopecia areata will progress to total scalp baldness (alopecia totalis). A very few people will lose all scalp and body hair (alopecia universalis). Progression to these more extensive types of hair loss is more common if:
The bald patches start in childhood.
The initial bout of hair loss affects more than half of the scalp.
There is also atopic eczema.
There is eyelash and/or eyebrow hair loss.
There is a family history of alopecia areata.
There is hair loss around the scalp margin.
There are nail changes.
There is another autoimmune disease.
Treatment can promote hair regrowth in some cases.
Alopecia areata treatment
Back to contentsUnderstandably, hair loss is upsetting - particularly in young women - and there are plenty of private clinics out there who promise 'instant hair regrowth'. Be careful: a lot of treatments for alopecia are unproven, often don't work and can quickly become very expensive.
Not treating is a common option
In many cases, bald patches regrow by themselves without treatment. In particular, if there are just one or two small bald patches then many doctors would advise that it can be left alone at first.
A change in hairstyle may perhaps conceal one or two small bald patches. If the hair loss becomes more extensive then the decision on whether to treat can be reconsidered. But even with extensive hair loss, there is still a chance that hair will regrow without treatment.
Note: alopecia areata itself won't damage your general health and so not treating will not lead to any general health problems. When considering any treatment choices, you should take into account the possible side-effects that some of the treatments may have. Also, treatments promote hair to regrow and do not affect or cure the underlying cause of the condition.
Steroid injections
Injections of steroid into the bald patches of the scalp can in theory suppress the local immune reaction that occurs in alopecia areata. This can then allow the hair follicles to function normally again for hair to regrow. This treatment may be an option for one or more small- to medium-sized bald patches. Steroid injections are thought to be the most effective treatment for patches of alopecia areata that are not too big. However, they do not work in every case.
This treatment is usually only done by a skin specialist and referral to hospital will usually be needed. Several injections (about 1 cm apart) are usually given at each session of treatment but the number is often limited by pain. Therefore, large bald areas are not suitable for steroid injections. It takes 1-2 months for the hair to start to regrow. Injections are repeated every 4-6 weeks.
Note: there is no guarantee that any hair regrown during treatment will persist once the treatment is finished.
Topical steroids
Rub-on (topical) steroid creams or gels may help hair regrowth but do not work as well as steroid injections. It may be worth a try if there are bald patches that are not suitable for steroid injections or whilst waiting to see a specialist to have steroid injections. If regrowth occurs, it takes 3-6 months. There is no point continuing with this treatment if there has been no regrowth after 3-6 months.
Topical minoxidil solution
This is rubbed into the bald patches and has been shown to promote hair regrowth in some cases. This is the same treatment that is used for the common male pattern baldness. It is not known how it works. The success rate is not high but may be considered , particularly for more extensive bald patches that are not suitable for steroid injections.
Minoxidil is not available on the NHS and it is expensive. It is normally available through private hair clinics or pharmacies. Some people with certain medical conditions may not be able to use it.
Minoxidil is not licensed for alopecia areata. It is licensed for other types of alopecia, such as male pattern baldness (although, again, only privately). If it works, it usually takes two to three months of treatment for an initial response and one year for a maximum response. There is no point continuing with this treatment if there is no improvement after one year.
See also Minoxidil scalp preparations for women and Minoxidil scalp preparations for men.
Topical immunotherapy
It is thought that topical immunotherapy is the most effective option for people with extensive alopecia areata. This is a very specialised treatment that is only available in some hospitals. A substance is put on affected skin to make the skin react like an allergy.
A commonly used substance is diphencyprone (DPCP). Increasing strengths of this substance are placed on the affected skin once a week over several weeks until the skin looks like it has mild dermatitis (eczema). The skin reaction seems to affect the process involved in causing alopecia areata in some way to allow hair to regrow.
Side-effects can be troublesome. For example, some people develop severe skin reactions.
Once regrowth occurs, treatment can be stopped but, in many cases, the hair loss then recurs. Therefore, regular maintenance treatment is often needed to keep the hair loss from returning.
Wigs
Wigs are a common treatment choice in patients with alopecia areata. You can get some wigs on the NHS in the UK. However, this needs a referral to hospital as only a specialist can sanction the prescription of a wig on the NHS.
Other treatments
Various other treatments may be used or advised. These include the following:
A plant substance called psoralen combined with ultraviolet A (PUVA) light therapy or phototherapy has been used with some limited success. This treatment requires many light therapy sessions in a hospital outpatient department.
Tattooing (dermatography) can be used to create the look of eyebrows that have fallen out.
Counselling is sometimes helpful for people who find it difficult to cope with hair loss.
Complementary therapies. There is not enough evidence to say how effective complementary treatments are in treating alopecia areata (for example, acupuncture, aromatherapy, etc).
It is very important to remember to use sunblock or a hat to protect bald patches when out in the sun.
Can alopecia areata be cured?
Back to contentsAs can be seen from the section above, there are various treatment options. It is hard to predict from the outset whether a particular treatment will benefit a particular person. One of the difficulties is that hair grows back without any treatment in many cases. Therefore, it is difficult to research the effect of treatments, as hair usually regrows naturally.
Patient picks for Hair and scalp problems

Skin, nail and hair health
Seborrhoeic dermatitis
Seborrhoeic dermatitis causes bad dandruff and sometimes a rash, commonly on the face and upper body. An anti-yeast (antifungal) shampoo and/or an antifungal cream will usually clear the dandruff and rash. The condition tends to come back (recur). If it recurs frequently, regular use of an antifungal shampoo and/or cream can help to keep it away.
by Dr Toni Hazell, MRCGP

Skin, nail and hair health
Fungal scalp infection
Ringworm is a skin infection caused by a fungus (not a worm). Ringworm on the scalp mainly affects children, particularly of African or Caribbean origin. Treatment is with antifungal medication which is needed for several weeks. An antifungal shampoo is not usually effective alone but may be advised in addition to medication.
by Dr Philippa Vincent, MRCGP
Frequently asked questions
If my patches of hair loss aren't perfectly round, is it still alopecia areata?
Alopecia areata typically presents as one or more bald patches on the scalp that are round in shape and about the size of a large coin. However, sometimes several small bald patches can develop and merge into a larger bald area, which might not be perfectly round.
What is the likelihood of my hair changing colour when it regrows after alopecia areata?
When hair regrows after an episode of alopecia areata, it may not have its usual colour at first and might look grey or white for a period. The usual colour then typically returns after several months.
Can alopecia areata affect hair on other parts of my body, besides just my scalp?
While it's unusual, patches of body hair, beard, eyebrows or eyelashes can be affected in some cases of alopecia areata. In very rare instances, all hair on the head and body, including eyebrows, groin area, and under the arms, can be lost (alopecia universalis).
What should I do if I notice nail changes along with my hair loss?
Nails are affected in about 1 in 10 cases of alopecia areata and can become pitted or ridged. If you notice nail changes, this is one of the factors that can make progression to more extensive hair loss (like alopecia totalis or universalis) more common.
If I only have small patches of hair loss, is it necessary to seek treatment?
In many cases, bald patches regrow by themselves without treatment, especially if there are just one or two small patches. Many doctors would advise leaving it alone at first. A change in hairstyle might conceal small patches. Not treating alopecia areata itself will not cause general health problems.
Are there any over-the-counter options I can try for alopecia areata?
Topical minoxidil solution can be rubbed into bald patches and has shown to promote hair regrowth in some cases, although the success rate is not high. It is the same treatment used for male pattern baldness and is normally available through private hair clinics or pharmacies. It is not available on the NHS and is not licensed specifically for alopecia areata.
How long do I need to use minoxidil before I know if it's working?
If minoxidil works, it usually takes two to three months of treatment for an initial response, and up to one year for a maximum response. If there's no improvement after one year, it's not worth continuing the treatment.
Further reading and references
- Guidelines for the management of alopecia areata; British Association of Dermatologists (2012)
- Darwin E, Hirt PA, Fertig R, et al; Alopecia Areata: Review of Epidemiology, Clinical Features, Pathogenesis, and New Treatment Options. Int J Trichology. 2018 Mar-Apr;10(2):51-60. doi: 10.4103/ijt.ijt_99_17.
- Hordinsky MK; Alopecia Areata: The Clinical Situation. J Investig Dermatol Symp Proc. 2018 Jan;19(1):S9-S11. doi: 10.1016/j.jisp.2017.10.015.
- Alopecia areata; NICE CKS, March 2023 (UK access only)
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 11 Jul 2028
13 Jul 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.