Underactive thyroid gland
Hypothyroidism
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 30 Jun 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
If you have an underactive thyroid gland, the condition is called hypothyroidism. In hypothyroidism, there is a reduced level of thyroid hormone in the body. This can cause various symptoms, the most common being tiredness, weight gain, constipation, aches, dry skin, lifeless hair and feeling cold.
Treatment usually involves taking a daily tablet of thyroid hormone to replace the missing thyroxine. Treatment works very well for most people with hypothyroidism but is required for life.
At a glance
Hypothyroidism means your thyroid gland does not make enough thyroid hormones.
Common symptoms include tiredness, weight gain, constipation, aches, and feeling cold.
A blood test is used to diagnose hypothyroidism, checking levels of TSH and thyroxine (T4).
Treatment involves taking levothyroxine tablets daily, usually for life.
If you have hypothyroidism, you are entitled to free prescriptions in the UK.
In this article:
Video picks for Thyroid problems
Continue reading below
What is hypothyroidism?
Neck cross-section showing the thyroid gland
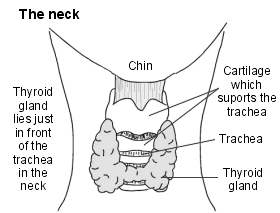
The thyroid gland is located in the neck and produces thyroid hormones. These are called thyroxine (T4) and tri-iodothyronine (T3) and are carried round the body in the bloodstream. They help to keep the body's functions (the metabolism) working at the correct pace.
Many cells and tissues in the body need thyroxine to keep them going correctly. Thyroid hormones are released when the thyroid gland is stimulated by thyroid stimulating hormone (TSH). This is a hormone released by another gland, in the brain. See the separate leaflet called Thyroid and parathyroid problems for further information about the thyroid gland.
Underactive thyroid gland (hypothyroidism) results from the thyroid gland being unable to make enough thyroid hormones, so that many of the body's functions slow down. Thyroid hormone levels are lower than normal. So some people call it having a 'low thyroid'. Hypothyroidism may also occur if there is not enough thyroid gland left to make thyroxine - for example, after surgical removal or injury.
Hypo- means not enough and hyper- means too much. If you have hyperthyroidism, you make too much thyroxine. This causes many of the body's functions to speed up. See the separate leaflet called Overactive thyroid gland (Hyperthyroidism) for more information.
Hypothyroidism symptoms
Back to contentsMany symptoms of having an underactive thyroid gland (hypothyroidism) can be caused by a low level of thyroxine. Basically, many body functions slow down. Not all symptoms develop in all cases.
Symptoms and signs that commonly occur include:
Tiredness.
Weight gain.
Constipation.
Aches.
Feeling cold.
Dry skin.
Dull or coarse hair.
Fluid retention.
Mental slowing.
Less common symptoms include:
A hoarse voice.
Irregular or heavy menstrual periods in women.
Infertility.
Loss of sex drive.
Carpal tunnel syndrome (which causes pains and numbness in the hand).
Memory loss or confusion in the elderly.
However, all these symptoms can be caused by other conditions and sometimes the diagnosis is not obvious. Symptoms usually develop slowly and gradually become worse over months or years as the level of thyroxine in the body gradually falls.
Continue reading below
What are the possible complications of hypothyroidism?
Back to contentsIf you have an untreated underactive thyroid gland (hypothyroidism):
You may feel generally unwell due to the symptoms above.
You have an increased risk of developing heart disease. This is because a low thyroxine level causes the blood fats (lipids) - cholesterol, etc - to rise. You may have a higher risk of coronary heart disease and of heart failure.
If you are pregnant, you have an increased risk of developing some pregnancy complications - for example:
Low birth weight.
Stillbirth.
Abnormalities in the baby.
Serious bleeding after the birth.
Hypothyroid coma (myxoedema coma) is a very rare complication.
However, with treatment, the outlook is excellent. With treatment, symptoms usually go and you are very unlikely to develop any complications.
Who develops hypothyroidism?
Back to contentsHaving an underactive thyroid gland (hypothyroidism) is ten times more common in women than it is in men. In the UK, around 1-2 in 100 people have hypothyroidism. It most commonly develops in adult women and becomes more common with increasing age. However, it can occur at any age and can affect anyone.
Continue reading below
What causes hypothyroidism?
Back to contentsAutoimmune thyroiditis - the most common cause in the UK
The most common cause of having an underactive thyroid gland (hypothyroidism) is an autoimmune disease called autoimmune thyroiditis. The immune system normally makes antibodies to attack bacteria, viruses and other germs. If you have an autoimmune disease, the immune system makes antibodies against certain tissues of your body.
If you have autoimmune thyroiditis, you make antibodies that attach to your own thyroid gland, which affect the gland's function. The thyroid gland is then not able to make enough thyroxine and hypothyroidism gradually develops. It is thought that something triggers the immune system to make antibodies against the thyroid. The trigger is not known.
Autoimmune thyroiditis is more common than usual in people with:
A family history of hypothyroidism caused by autoimmune thyroiditis.
Down's syndrome. Hypothyroidism develops in 1 in 3 people with Down's syndrome before the age of 25 years. Symptoms of hypothyroidism may be missed more easily in people with Down's syndrome. Therefore, some doctors recommend that all people with Down's syndrome should have an annual blood test to screen for hypothyroidism.
Turner syndrome. Again, an annual blood test to screen for hypothyroidism is usually advised for people with this condition.
A past history of Graves' disease or thyroiditis following childbirth.
A personal or family history of other autoimmune disorders - for example:
Some people with autoimmune thyroiditis also develop a swollen thyroid gland (goitre). Autoimmune thyroiditis with a goitre is called Hashimoto's disease. Also, people with autoimmune thyroiditis have a small increased risk of developing other autoimmune conditions such as vitiligo, pernicious anaemia, etc.
Surgery or radioactive treatment to the thyroid gland
If the thyroid gland has been damaged or destroyed by treatment (for another thyroid disorder, or for other problems in the neck), it may not produce enough thyroid hormone.
Other causes
Other causes of hypothyroidism include:
Worldwide, iodine deficiency is the most common cause of hypothyroidism. (Your body needs iodine to make thyroxine.) This affects some countries more commonly than others, depending on the level of iodine in the diet.
A side-effect to some medicines - for example, amiodarone and lithium. Also some people who have been treated for high thyroid levels with medicines such as propylthiouracil or carbimazole go on to develop hypothyroidism in later years.
Other types of thyroid inflammation (thyroiditis) caused by various rare conditions.
A pituitary gland problem is a rare cause. The pituitary gland that lies just under the brain makes a hormone called thyroid-stimulating hormone (TSH). This stimulates the thyroid gland to make thyroxine. If the pituitary does not make TSH then the thyroid cannot make enough thyroxine. This is called secondary hypothyroidism.
Some children are born with an underactive thyroid gland (congenital hypothyroidism). Babies in the UK are screened for this with a blood test at birth.
How is hypothyroidism diagnosed?
Back to contentsA blood test diagnoses an underactive thyroid gland (hypothyroidism). A normal blood test will also rule it out if symptoms suggest that it may be a possible diagnosis. One or both of the following may be measured:
Thyroid-stimulating hormone (TSH). This hormone is made in the pituitary gland. It is released into the bloodstream. It stimulates the thyroid gland to make thyroxine. If the level of thyroxine in the blood is low, then the pituitary releases more TSH to try to stimulate the thyroid gland to make more thyroxine. Therefore, a raised level of TSH means the thyroid gland is underactive and is not making enough thyroxine.
Thyroxine (T4). A low level of thyroxine confirms hypothyroidism. Test results might be described as having 'low thyroid levels' or a 'low thyroid'.
A test for thyroid antibodies may be done to confirm the diagnosis if the cause is thought to be autoimmune. Other tests are not usually necessary unless a rare cause of hypothyroidism is suspected.
For example, tests of the pituitary gland may be done if both the TSH and thyroxine levels are low. If you have a swollen thyroid gland when the doctor examines you (a goitre), you would usually have an ultrasound scan.
Subclinical hypothyroidism
Some people have a raised TSH level but have a normal T4 level. This means that you are making enough thyroxine but the thyroid gland is needing extra stimulation from TSH to make the required amount of thyroxine. In this situation you have an increased risk of developing hypothyroidism in the future.
Your doctor may advise a repeat blood test to see if you do eventually develop hypothyroidism. In many people, the blood test returns to normal on its own without treatment. So usually the test is repeated in three months rather than starting treatment straightaway. See the next section on hypothyroidism treatment for recommendations on treatment.
Hypothyroidism treatment
Back to contentsThe treatment of underactive thyroid gland (hypothyroidism) is to take levothyroxine (thyroxine) tablets each day. This replaces the thyroxine which your thyroid gland is not making. Most people feel much better soon after starting treatment.
Ideally, take the tablet on an empty stomach (at least half an hour before breakfast). This is because some foods rich in calcium or iron may interfere with the absorption of levothyroxine from the gut. (For the same reason, don't take levothyroxine tablets at the same time of day as calcium or iron tablets.)
Caffeine can also interfere with absorption of levothyroxine so avoid tea and coffee for half an hour after taking the tablet also.
Some other medicines can also affect thyroxine levels so ideally do not take levothyroxine with any other tablets. Check with your pharmacist if you do need to take another tablet at the same time.
What is the dose of levothyroxine?
Most adults need between 100 and 200 micrograms daily. A low dose is prescribed at first, especially in those aged over 60 or with heart problems. The dose is then gradually increased over a period of time. Blood tests are usually taken regularly and the dose may be adjusted accordingly. It may take a few months for you to start to feel better.
The blood test measures TSH (see above). Once the blood TSH level is normal it usually means you are taking the correct amount of levothyroxine. It is then common practice to check the TSH blood level once a year.
Women who are planning a pregnancy may need to adjust their dose of levothyroxine; as soon as pregnancy is confirmed, they should increase their levothyroxine dose by 25-30%. Speak to your doctor if you have an underactive thyroid and are planning a pregnancy.
Also, as you get into late middle age and older, you may need a reduced dose of levothyroxine.
Missed a tablet?
Everyone forgets to take their tablets from time to time. Don't worry as it is not dangerous to miss the odd forgotten levothyroxine tablet. If you forget to take a dose, take it as soon as you remember if this is within two or three hours of your usual time.
If you do not remember until after this time, skip the forgotten dose and take the next dose at the usual time. Do not take two doses together to make up for a missed dose. However, you should try to take levothyroxine regularly each morning for maximum benefit.
Other dosing routines have been studied. However these have only been explored in small studies and are not routinely recommended. It may be that levels will not be as steady if the medicine is not taken in a daily dose.
The best advice based on currently available evidence is to take the tablet once a day regularly. If you are having problems with this, discuss it with your doctor or pharmacist.
How long is the treatment for?
For most people, treatment is for life. Occasionally, the disease process reverses. This is uncommon, apart from the following:
Children. Sometimes hypothyroidism is a temporary condition in older children. (This is not so for children who are born with an underactive thyroid gland.)
Pregnancy. Some women develop thyroid imbalance after having a baby. If it occurs, it typically happens about three to six months after the birth. Often this lasts just a few months and corrects itself. Treatment is needed only in a small number of cases. However, afterwards it is wise to have a yearly blood test, as there is an increased risk of developing autoimmune thyroiditis and long-term hypothyroidism in the future.
What if it doesn't work?
Most people feel better once their blood tests have returned to normal with levothyroxine. In a small percentage of people, however, the blood tests go back to normal but they don't feel any better. If this is the case, you would normally be referred to a specialist (an endocrinologist).
The specialist doctor may do some more tests to check your symptoms are definitely due to hypothyroidism rather than something else. They will also check there is nothing interfering with your levothyroxine (such as other medication).
What is liothyronine?
Liothyronine is a manufactured form of triiodothyronine (T3).
UK guidelines recommend that T3 and combinations of T4 and T3 should not routinely be prescribed. The Royal College of Physicians does not recommend that T3 should ever be prescribed.
It says there is not enough evidence that it helps patients and not enough evidence to be sure it is not harmful. Clinical practice guidelines worldwide do not recommend or support the routine use of combination (LT4 and LT3) therapy.
The NHS recommends that:
Treatment with liothyronine should never be started in primary care (by a GP).
Patients who are currently taking liothyronine should be reviewed by a consultant NHS endocrinologist with a view to switching to levothyroxine if appropriate.
The British Thyroid Association states that a small number of patients have symptoms which do not improve on levothyroxine. For these, a consultant NHS endocrinologist may recommend a carefully monitored trial of liothyronine.
You can find out more from the further reading links to CKS hypothyroidism and NHS England guidance.
Treatment for subclinical hypothyroidism
National Institute for Health and Care Excellence (NICE) 2019 guidelines recommend giving levothyroxine replacement therapy even if your T4 level is normal, as long as your TSH level is raised over 10 mIU/L on two separate occasions three months apart. This blood result picture - normal T4 but raised TSH - is called 'subclinical hypothyroidism'.
These guidelines also suggest that a six-month trial of levothyroxine for adults aged under 65 with subclinical hypothyroidism should be considered, if you have a TSH lower than 10 mlU/L on two occasions three months apart, and also have some symptoms of hypothyroidism.
Treatment for hypothyroidism in pregnancy
Pregnant women taking levothyroxine should be monitored by a specialist (endocrinologist). Pregnancy can affect the amount of medication needed, and it is very important that levels do not get either too high or too low.
Are there any side-effects or problems from treatment?
Back to contentsLevothyroxine tablets replace the body's natural hormone, so side-effects are uncommon. However, if you have angina, you may find that your angina pains become worse when you first start levothyroxine. Tell a doctor if this happens.
If you take too much levothyroxine it can lead to symptoms and problems of an overactive thyroid gland (hyperthyroidism) - for example:
The sensation of a 'thumping heart' (palpitations).
Diarrhoea.
Irritability.
Sweating.
An increased risk of developing 'thinning' of the bones (osteoporosis).
This is why you need blood tests to check that you are taking the correct dose.
Other medicines may interfere with the action of levothyroxine - for example, carbamazepine, iron tablets, phenytoin, and rifampicin. If you start any of these medicines, or change the dose, you may need to alter the dose of the levothyroxine. Your doctor will advise. Also, if you take warfarin, the dose may need to be altered if you have a change in your dose of levothyroxine.
Free prescriptions
Back to contentsIn the UK, if you have hypothyroidism, you are entitled to free prescriptions. This is for all your medicines, whether related to the hypothyroidism or not. Ask at your GP surgery for a form to fill in (form FP92A) to claim this benefit.
What is the outcome (prognosis)?
Back to contentsMost people get better on levothyroxine treatment, although they usually have to stay on it for ever. If you are treated for hypothyroidism, a blood test each year is needed to make sure you are still on the right dose. As above, about 5 or 10 in 100 people will not feel any better on levothyroxine, even though their blood tests go back to normal. This may be more difficult to treat (as discussed above).
People who have subclinical hypothyroidism may or may not need treatment. In nearly 4 out of 10 people with subclinical hypothyroidism, the blood tests go back to normal on their own, without treatment ever being needed.
Very rarely, people who have not had their hypothyroidism treated develop a serious complication called myxoedema coma. This is rare but is very serious and can cause death.
In summary
Back to contentsHaving an underactive thyroid gland (hypothyroidism) is common.
Symptoms develop gradually. They may be confused with other conditions.
Treatment with levothyroxine tablets is usually easy and effective.
Treatment is usually for life.
Have a blood test once a year if you take levothyroxine tablets, once your dose has become stabilised. Blood tests are needed more often when you first start treatment.
Patient picks for Thyroid problems
Hormones
Overactive thyroid gland
Hyperthyroidism is an uncommon condition where your thyroid gland (which is in your neck) goes into 'overdrive'. It produces too much of a chemical called thyroxine. We all have a certain amount of thyroxine in our bodies to keep us working at just the right 'energy level'. If too much thyroxine is made, you can become very ill with tiredness, a fast heartbeat and weight loss. Initially the symptoms can mimic lots of other conditions. However, the diagnosis is usually made with a simple blood test. A number of treatments are available which makes hyperthyroidism fairly easy to treat: tablets are the mainstay of treatment, followed by radiotherapy. Occasionally surgery is needed.
by Dr Colin Tidy, MRCGP

Hormones
Iodine deficiency
Iodine is essential for the body to make thyroid hormone. Low levels of iodine may cause an underactive thyroid gland and symptoms of hypothyroidism (eg, tiredness, constipation and weight gain). Iodine deficiency in pregnant women may cause problems for the baby, including learning disability. There has been a worldwide campaign to prevent iodine deficiency by using salt containing added iodine. However, iodine deficiency is still a widespread problem in many countries. Mild iodine deficiency may still affect some people in the UK.
by Dr Rosalyn Adleman, MRCGP
Frequently asked questions
How will I know if my hypothyroidism symptoms are improving after starting treatment?
Most people feel much better soon after starting levothyroxine treatment. Blood tests are taken regularly to monitor your thyroid-stimulating hormone (TSH) level. Once your TSH level is normal, it usually indicates you are taking the correct amount of levothyroxine, and your symptoms should subside. It can take a few months to feel the full effects of the treatment.
If I am pregnant or planning to become pregnant, how does this affect my levothyroxine dose?
If you are pregnant, or planning a pregnancy, it is important to speak with your doctor. Women planning a pregnancy may need to adjust their levothyroxine dose, and as soon as pregnancy is confirmed, they should increase their dose by 25-30%. Throughout pregnancy, you will be monitored by a specialist to ensure your hormone levels remain appropriate, as pregnancy can affect the amount of medication needed.
What should I do if I forget to take my levothyroxine tablet?
It's not dangerous to miss an occasional levothyroxine tablet. If you remember within two or three hours of your usual time, take it as soon as you remember. If it's later than that, simply skip the missed dose and take your next dose at the usual time. Do not take two doses together to compensate for a forgotten one. For maximum benefit, try to take your tablet regularly each morning.
Are there any specific concerns for elderly people taking levothyroxine?
Yes, if you are over 60 years old, or as you get into late middle age and older, you may be prescribed a lower initial dose of levothyroxine. Your doctor will gradually increase the dose. Also, as you age, you may eventually need a reduced dose of levothyroxine.
Can taking other medications affect my levothyroxine treatment?
Yes, some medicines can interfere with the absorption of levothyroxine or affect its action. For example, foods rich in calcium or iron should not be taken at the same time as levothyroxine. Caffeine can also interfere with absorption, so avoid tea and coffee for half an hour after taking your tablet. Other medicines like carbamazepine, iron tablets, phenytoin, rifampicin, and warfarin may also require adjustments to your levothyroxine dose. Always check with your pharmacist or doctor if you need to take other tablets or start new medications.
How often will I need blood tests once my levothyroxine dose is stable?
Once your levothyroxine dose has stabilised and your blood TSH level is normal, it is common practice to have your TSH blood level checked once a year. When you first start treatment, blood tests are needed more frequently to find the correct dose.
Further reading and references
- Thyroid disease: assessment and management; NICE guidance (November 2019 - last updated October 2023)
- Hypothyroidism; NICE CKS, May 2021 (UK access only)
- Hughes K, Eastman C; Thyroid disease: Long-term management of hyperthyroidism and hypothyroidism. Aust J Gen Pract. 2021 Jan-Feb;50(1-2):36-42. doi: 10.31128/AJGP-09-20-5653.
- van Trotsenburg P, Stoupa A, Leger J, et al; Congenital Hypothyroidism: A 2020-2021 Consensus Guidelines Update-An ENDO-European Reference Network Initiative Endorsed by the European Society for Pediatric Endocrinology and the European Society for Endocrinology. Thyroid. 2021 Mar;31(3):387-419. doi: 10.1089/thy.2020.0333.
- British National Formulary (BNF); NICE Evidence Services (UK access only)
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 29 Jun 2027
30 Jun 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.