Addison's disease
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 13 Nov 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:TirednessChronic fatigue syndromeFibromyalgiaSleep apnoeaMuscle weaknessSleep debt calculator
Addison's disease is a condition in which your adrenal glands are not working as well as they should. In Addison's disease the adrenal glands do not produce as much of the steroid hormones (such as cortisol) as they normally do. These hormones are vital for your body and if you do not have enough of them, you can become very unwell. If the level of these hormones becomes very low, it can be life-threatening. Treatment is with replacement hormone tablets which you need to take every day.
At a glance
Addison's disease means your adrenal glands don't produce enough hormones like cortisol.
Symptoms often develop gradually and include tiredness, darkened skin patches, and low blood pressure.
An Addison's crisis is a medical emergency with severe vomiting, pain, and collapse.
Treatment involves daily steroid medication to replace missing hormones, which must be taken for life.
Always tell doctors you have Addison's disease, especially if you are unwell or need surgery.
Carry an emergency injection kit and know how to use it, along with carers or family.
In this article:
Video picks for Adrenal problems
Continue reading below
What is Addison's disease?
Addison's disease, also known as primary adrenal insufficiency, is a condition in which your adrenal glands do not make enough of certain hormones. The condition is named after Dr Thomas Addison, who first described it in 1855. Addison's disease is rare. Just over 8,000 people in the UK have Addison's disease at any one time. Most cases first develop in people aged between 30 and 50. However, it can occur at any age.
Addison's disease is also known as primary adrenal insufficiency. Adrenal insufficiency (reduced hormone production by the adrenal glands) has other causes as well (see below).
Adrenal glands and their function
You have two small adrenal glands that lie just above each kidney. Each adrenal gland has an outer part (adrenal cortex) and an inner part (adrenal medulla). Cells in the adrenal glands make various hormones. A hormone is a chemical which is made in one part of the body but passes into the bloodstream and has effects on other parts of the body.
Pituitary and adrenal glands
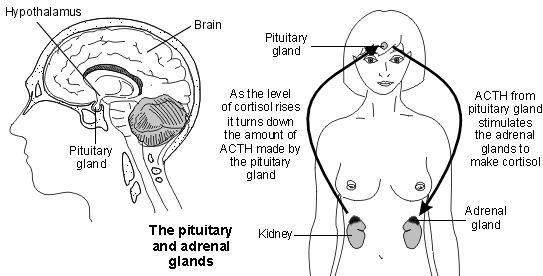
Cells in the outer layer of the adrenal gland (adrenal cortex) make the hormones cortisol, aldosterone, and androgens. The amount of cortisol that is made is controlled by another hormone called adrenocorticotrophic hormone (ACTH). ACTH is made in a small gland that lies just under the brain (the pituitary gland). This in turn is stimulated by another hormone which is produced by another part of the brain, called the hypothalamus. ACTH passes into the bloodstream, is carried to the adrenal glands and stimulates the adrenal glands to make cortisol.
Cortisol is a hormone that is vital for health. It has many functions which include:
Helping to regulate blood pressure.
Helping to regulate the immune system.
Helping to balance the effect of insulin in regulating the blood sugar level.
Helping the body respond to stress.
Aldosterone helps to regulate salts in the blood and helps to control blood pressure.
Androgens include hormones such as testosterone and oestrogen. Androgens produced in the adrenals are weaker, but are often converted into more potent forms (testosterone or oestrogen) in other parts of the body. Androgens have important functions in both men and women.
Cells in the inner part of the adrenals (adrenal medulla) make the hormones adrenaline (epinephrine) and noradrenaline (norepinephrine). These have various actions throughout the body.
Addison's disease symptoms
Back to contentsIn many cases the symptoms develop gradually over weeks or months. As the level of cortisol gradually falls you may develop one or more of the following:
General weakness and becoming easily tired.
Darkened areas of skin (pigmentation). This happens in Addison's disease (but not other types of adrenal insufficiency), because when the pituitary gland produces higher levels of the hormone ACTH, to try to get the adrenal glands to work harder, it also produces a different hormone that causes skin darkening. Pigment changes mainly occur on:
Sun-exposed areas of skin.
Armpits.
Nipples.
The creases of the hands.
Gums and inside the mouth.
Recent (rather than old) scars.
Pressure points such as the elbows.
In people with darker skin tones (including black or brown skin), it can sometimes be difficult to detect darkening of the skin tone. Changes can still be seen inside the mouth and of recent scars.
Blood pressure which is low and falls further when you stand, which can make you dizzy.
Being off your food.
Weight loss, or faltering growth in children.
Feeling sick and being sick (vomiting) from time to time.
Tummy (abdominal) pains which may come and go.
Diarrhoea or constipation which may come and go.
Cramps and pains in muscles.
Craving for salt or for salty foods and drinks.
Menstrual periods in women may become irregular or stop.
The symptoms can be vague at first. For example, you may feel tired and not right, but it is difficult to say why. Also, most of the symptoms can be caused by other problems, and Addison's disease is rare. So, the condition may not be recognised for weeks or months after symptoms first begin.
Continue reading below
Addison's crisis
Back to contentsIf the level of cortisol falls to become very low you can become very ill in a short time. This is called an Addison's crisis, or Addisonian crisis. In this situation symptoms include:
Severe vomiting and diarrhoea.
Pains in the back and abdomen.
Lack of fluid in the body (dehydration).
Low blood pressure.
Collapse.
You may become severely ill and may die if the cause of the symptoms is not diagnosed and treated quickly.
An Addisonian crisis may suddenly develop after a period of less severe symptoms (described above). The crisis is often triggered by another illness such as an infection or a stress such as a surgical operation. During these times your body needs extra cortisol. But, if you have Addison's disease you cannot make extra cortisol, and you may then quickly develop these crisis symptoms.
Increasing your daily steroid dose during times of stress (see below) helps to compensate for this, and can prevent an adrenal crisis from happening.
In some cases an Addisonian crisis develops when there have not been any previous symptoms.
Addison's disease treatment
Back to contentsThe main treatment for Addison's disease is daily steroid medication (usually tablets) to replace the adrenal hormones that are missing.
These steroid hormones are essential for life. People with Addison's disease need to take daily hormone medication for life.
Cortisol replacement
You need steroid medication to replace the cortisol which you no longer make. This is usually with a medicine called hydrocortisone which is very similar to cortisol.
The amount is usually about 15-30 mg each day. Some people need more than this and others less. The daily amount is broken up into two or three doses each day with a higher dose taken in the morning than in the evening. For example, you may be advised to take 15 mg in the morning and 10 mg early in the evening.
Some people say they feel better taking the daily amount divided into three doses over the daytime. This dosing aims to mimic the normal pattern of cortisol levels in the body which are normally higher in the morning than in the evening. The last dose should be taken no less than four hours before bedtime. Your doctor will explain the exact dosing plan. There is a newer once-a-day option available, which may be suitable for some people.
The exact dose needed depends on factors such as your height, weight, sex and level of activity. You will be advised of the doses by your doctor. It may take a while to adjust the doses to the correct ones for you.
You will need to increase the amount of hydrocortisone you need per day in certain situations - see below.
You should never miss taking your medication. These medications are essential for life, and stopping them is life-threatening.
People with Addison's disease should also have emergency management kits, which contain injectable hydrocortisone, to use if they might be having an adrenal crisis - see below.
Replacing aldosterone
Fludrocortisone is a substitute medicine for aldosterone. This helps to regulate blood pressure and blood salt level.
Replacing androgens
The adrenal glands also make androgen hormones. Androgens are also produced by the testicles in men, and the ovaries in women. Some people with Addison's take DHEA (a type of androgen hormone) to treat tiredness and low sex drive. It's not prescribable on the NHS, as it's classed as a food supplement.
Emergency
If you have an Addisonian crisis
This is a medical emergency.
If you, or someone you know, may be having an Addisonian crisis, use an emergency injection kit to give an injection of hydrocortisone as soon as possible.
An emergency injection kit can be used by anyone who knows how to use it, including carers and first-aiders. It does not need to be given by a healthcare professional.
Then call 999, and tell them you are having an Addisonian crisis, or an adrenal crisis.
If you think you are having an Addisonian crisis, and don't have access to an emergency injection kit, call 999 straight away.
In hospital, people with an Addisonian crisis are given hydrocortisone injections, and a drip of fluid to bring up blood pressure; they may need intensive care until the crisis is over. They will then need to continue taking hydrocortisone medication as detailed above.
It can be difficult for healthcare professionals to recognise an Addisonian crisis, as Addison's is a rare condition, and symptoms and signs can be very similar to other serious illnesses.
If you're unwell, tell the clinician looking after you that you have Addison's disease.
Consider wearing a medical alert bracelet, necklace or similar, or carrying a steroid card (see 'Other points to consider', below).
Cortisol replacement - special circumstances
If you have Addison's disease, it is vital that you take the right amount of cortisol replacement (hydrocortisone) every day. Without this replacement medicine you can become very ill. So, some things to bear in mind:
If you are ill or need an operation
If you have an illness such as an infection, or an accident, or anything else causing major stress, such as an operation, you need extra hydrocortisone. Your doctor should advise you on some general 'sick day rules' to follow. For example, this may include:
If you have a moderate-severity illness, double your normal dose of hydrocortisone until you have recovered. Examples of moderately severe illnesses include:
Having a temperature (fever) of 38°C or more.
Having to stay in bed for all or most of the day to recover.
Having to take antibiotics.
If you have any serious injury - take 20 mg hydrocortisone immediately (in addition to your normal doses for the day).
If you have diarrhoea, double your normal dose until it has settled.
If you have been sick (vomited) once - take 20 mg hydrocortisone immediately after you vomit. Also, make sure you have plenty to drink to make sure you do not become lacking in fluid in the body (dehydrated).
If you vomit twice or more - use an emergency injection of hydrocortisone (described below) and call a doctor for advice. Make sure that any doctor knows you have Addison's disease and this, in addition to the cause of the illness, needs attention.
If you are about to have any operation, dental procedure, or medical procedure such as an endoscopy - you must make sure that the doctor, dentist or anaesthetist knows that you have Addison's disease. You will need extra doses of hydrocortisone.
Basically, for any significant physical stress - illness, injury or operation - you need extra hydrocortisone. This can be taken as tablets but an emergency injection of hydrocortisone might be appropriate as an alternative, especially for situations such as a serious injury. And when you are ill, if you become dizzy or faint, this is a good indication that you might need a drip of fluid. Call a doctor immediately if this occurs and state that you have Addison's disease.
The Addison's Disease Self-help Group website (details below in Further reading) has a wealth of information about how to handle various situations. If you know what to do in different situations involving stress, trauma or illness, you can avoid an adrenal crisis.
If you are under emotional stress
Emotional or psychological stress also increases your cortisol requirements, and can sometimes be a trigger for an Addisonian crisis.
Whether or not to take extra hydrocortisone depends on the exact situation; everyone deals with things differently, and situations that can be very stressful to one person might be manageable to another person.
In general, though, you should consider increasing your steroid dose for a short time if you are dealing with a major stressful event, such as the death of a loved one, an important exam, or a significant life event like getting married or divorced.
Your repeat prescription - including stand-by emergency injections
Make sure you obtain your medication well in advance so that you never run out. In the UK, people with Addison's disease are entitled to free prescriptions. See your pharmacist for details.
You should also be prescribed two or three emergency injection kits to use if you think you are developing an Addisonian crisis. Keep these easily-accessible.
You, and anyone you spend a lot of time with, should learn how to use the emergency injection kit (it doesn't take very long).
Anyone can give an emergency injection of hydrocortisone to treat a suspected Addisonian crisis - it doesn't have to be given by a healthcare professional.
If you go on holiday
Take ample supplies of your medication and emergency hydrocortisone injections. Make sure you have extra hydrocortisone, in case you need to double it for any reason. Consider taking a letter about your condition (see below).
If you take part in strenuous sport or exercise
You will need extra hydrocortisone and fluids (for example, if you do a marathon). The amount can vary so take advice from your doctor.
If you work shifts or at night
The dosage of the hydrocortisone aims to replicate the normal variation in cortisol levels. This fluctuates with shift workers. Take advice from your doctor as to how to adjust the dose to suit your work schedule.
Other points to consider
Consider wearing a bracelet and carrying a letter. You are strongly advised to wear a medical emergency identification bracelet or similar. This can alert people that you need hydrocortisone in case of emergencies. For example, if you are knocked out in a car crash and are not able to tell the doctor that you have Addison's disease. Apart from any other treatment, you will always need your hydrocortisone (or similar steroid replacement for cortisol). Also, consider carrying a letter or card with details of your usual and emergency treatment to show to any doctor you may see who is unfamiliar with Addison's disease. The Addison's Disease Self-help Group (see Further reading below) has multilingual cards that can be used for this purpose.
Tell a doctor if you are prescribed other medication. Some medicines used to treat other conditions can interfere with the medicines used to treat Addison's disease. For example, the combined oral contraceptive pill and hormone replacement therapy (HRT) used in the treatment of menopausal symptoms both interact with cortisone. The dose, therefore, may need adjusting. Always tell a doctor that you are being treated for Addison's disease if you are prescribed any other medicine.
Osteoporosis prevention. 'Thinning' of the bones (osteoporosis) may be more common in people with Addison's disease compared to the general population. Osteoporosis mainly affects older people, in particular women who are past the menopause. There is much that can be done throughout your life to help prevent the development of osteoporosis or to minimise its severity if it develops when you are older. For example, regular exercise, a good diet and not smoking will all help. Where necessary, medication may be advised if bone 'thinning' is detected. A special type of scan that measures bone density is used to detect osteoporosis. See the separate leaflet called Osteoporosis for more details.
Other diseases
As mentioned above, if you have autoimmune Addison's disease, you have a higher-than-average chance of other autoimmune diseases developing. For example, thyroid problems, vitiligo, and pernicious anaemia - the most common being thyroid disorders, which are treatable.
Therefore, tell your doctor if you develop any other unexplained symptoms. You will normally have regular blood tests to check you have not developed any of these conditions.
Continue reading below
Addison's disease causes
Back to contentsCauses of Addison's disease include:
Autoimmune Addison's disease
In Western Europe, more than 8 in 10 cases are due to an autoimmune disease. The immune system normally makes proteins called antibodies, which are sent into the bloodstream to attack bacteria, viruses, and other germs. In autoimmune diseases, the immune system makes antibodies against part or parts of your own body.
In autoimmune Addison's disease, you make antibodies which attach to cells in the adrenal cortex. These destroy the cells which make cortisol and aldosterone. The adrenal medulla is not affected, so you still make adrenaline (epinephrine) and noradrenaline (norepinephrine). It is thought that something triggers the immune system to make these antibodies. The trigger is not known.
If you have autoimmune Addison's disease you have a higher-than-average chance of other autoimmune diseases developing, such as thyroid problems, vitiligo, diabetes and pernicious anaemia.
Tuberculosis (TB)
TB is an infection which usually affects the lungs. In some cases the infection can spread to the adrenals, meaning that the adrenal glands are damaged and sometimes completely destroyed. In the past this was the most common cause of Addison's disease. In some parts of the world where TB is still common, it remains the most common cause.
Other causes
Other less common adrenal gland causes include:
Other infections which can sometimes affect both adrenals - eg, some bacterial infections (such as meningococcus or pneumococcus), or HIV.
Cancers of other parts of the body, which can spread and destroy the adrenals.
Rare hereditary conditions - for example, adrenoleukodystrophy (ALD) and congenital adrenal hyperplasia (CAH).
Being critically unwell - for example, after a heart attack (myocardial infarction).
Damage to the adrenal gland (for example, due to injury, surgery or radiotherapy).
Medicines which occasionally can have an effect on production of adrenal hormones, such as ketoconazole, fluconazole and phenytoin.
Secondary causes of a low cortisol level
As mentioned, the amount of cortisol that you make in the adrenal glands is controlled by another hormone called ACTH. This is made in the pituitary gland. If you have a low level of ACTH, your adrenals make too little cortisol. Strictly speaking, this is not a condition of the adrenals, and is not classed as Addison's disease. However, it causes similar symptoms and is called secondary hypoadrenalism, or secondary adrenal insufficiency.
Secondary adrenal insufficiency occurs when ACTH levels are too low. Causes of a low ACTH level include:
Some disorders of the pituitary gland, which can cause a lack of ACTH (along with other pituitary hormones). For example, tumours, injury, surgery, radiotherapy or infection.
Some disorders of the hypothalamus, which in turn produces the hormone which stimulates ACTH. For example, tumours, injury, surgery, radiotherapy, or infection involving the hypothalamus.
When the problem is in the hypothalamus and not the pituitary, it is known as tertiary adrenal insufficiency.
Long-term use of steroid medicines such as prednisolone. Steroid medicines are similar to cortisol. They are sometimes used to treat arthritis, cancer, and various other conditions. If you take a steroid medicine for several weeks or more, you stop making ACTH and cortisol, as the steroid medicine takes over the role of cortisol. If you suddenly stop taking the steroid medicine, it takes quite some time for the pituitary and adrenal glands to get back into the normal making of ACTH and cortisol. Therefore, if you stop the medicine suddenly, adrenal insufficiency occurs because you have low cortisol levels. You can then quickly develop low cortisol symptoms similar to an Addisonian crisis.
The rest of this leaflet deals only with autoimmune Addison's disease.
Addison's disease diagnosis
Back to contentsBlood tests
Blood tests may help point to Addison's disease. These include measurements of some of the salts in your body (sodium and potassium), sugar levels, calcium levels and morning cortisol levels. (Cortisol levels are normally highest first thing in the morning, so it's easiest to spot an unusually low cortisol if measured at that time.) A one-off measurement of blood cortisol, however, may not be enough to diagnose Addison's disease. It may be low from time to time in normal people. Therefore, if Addison's disease is suspected, a special stimulation test is usually needed to confirm the diagnosis.
The adrenal gland can be stimulated by an injection of a substance similar to ACTH. If the adrenals are normal, then blood samples taken shortly after this injection should show a rise in cortisol. If you have Addison's disease you do not have a rise in blood cortisol following the injection. The usual test performed in this way is called a Synacthen® test.
Once tests show you have a lack of adrenal hormones, there will be tests done to find out why. A blood test may detect antibodies which cause autoimmune Addison's disease. This is (as mentioned above) the most common cause. If this is found to be the case further tests will not be needed.
X-rays or scans
Other tests may be needed if it is thought that you have Addison's disease caused by other conditions such as TB, or a secondary cause of a low ACTH and cortisol level. This may involve further blood tests, X-rays or scans.
Patient picks for Adrenal problems

Hormones
Adrenal fatigue
Adrenal fatigue is a theory that the adrenal glands can become 'overworked' from chronic stress, leading to symptoms such as fatigue and low energy. However, there is no scientific evidence to support this claim. Adrenal fatigue is not recognised as a medical condition by professional medical societies, and the consensus amongst mainstream doctors is that it does not exist as a disease.
by Dr Doug McKechnie, MRCGP

Hormones
Cushing's syndrome
Cushing's syndrome is caused by too high a level of glucocorticoid in the body. This can be caused by taking steroid medication long-term (the common cause) or by the body making too much cortisol (the main glucocorticoid made by the body). Symptoms usually develop gradually and so the diagnosis (other than that caused by steroid medication) may not be clear for some time.
by Dr Rachel Hudson, MRCGP
Frequently asked questions
What is the difference between Addison's disease and other types of adrenal insufficiency?
Addison's disease is specifically primary adrenal insufficiency, meaning the problem lies directly with the adrenal glands not producing enough hormones. Other types of adrenal insufficiency, such as secondary or tertiary, are caused by issues with the pituitary gland or hypothalamus, which in turn affect the adrenal glands' ability to produce cortisol.
How important are regular blood tests if I have Addison's disease?
Regular blood tests are important for people with Addison's disease. Initially, they help to confirm the diagnosis by measuring salt levels, sugar levels, calcium, and morning cortisol. Once diagnosed, they are used to ensure hormone levels are well-managed and can also check for the development of other autoimmune diseases, which are more common in people with autoimmune Addison's disease.
Considering Addison's disease is rare, how can I ensure I get the right care in an emergency?
Because Addison's disease is rare and its symptoms can mimic other illnesses, it's crucial to inform any healthcare professional looking after you that you have the condition. Wearing a medical alert bracelet or carrying a steroid card that details your diagnosis and emergency treatment can be very helpful, especially if you are unable to communicate yourself.
Why is the dosage of hydrocortisone split throughout the day?
The daily dose of hydrocortisone is typically split into two or three doses, with a higher amount taken in the morning. This dosing schedule aims to mimic the body's natural pattern of cortisol production, which is normally higher in the morning and decreases towards the evening. The last dose should be taken at least four hours before bedtime.
Are there any long-term health concerns I should be aware of if I have Addison's disease?
People with Addison's disease may have a higher risk of developing 'thinning' of the bones, known as osteoporosis, especially as they get older. Maintaining a healthy lifestyle with regular exercise, a good diet, and not smoking can help prevent or minimise its severity. Your doctor may also recommend checks for bone density.
What should I do if I think my hydrocortisone dose needs adjusting due to non-physical stress?
Emotional or psychological stress can also increase your body's cortisol requirements, and in some cases, trigger an Addisonian crisis. You should consider increasing your steroid dose for a short period if you are experiencing a major stressful event, such as a significant life event or loss. It's best to discuss specific situations with your doctor, as individual responses to stress vary.
Further reading and references
- Addison's Disease Self-help Group
- Adrenal insufficiency: identification and management; NICE guideline (August 2024)
- Addison's disease; NICE CKS, September 2024 (UK access only)
Continue reading below
About the authorView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Krishna Vakharia, MRCGP
Chief Medical Officer for Health, Optum UK
MBChB, MRCGP(2013), BMedSci (hons), DFSRH, DRCOG, PGDipDerm (Distn)
Dr Krishna Vakharia is an NHS GP. She is also a regular examiner for the postgraduate Diploma in Practical Dermatology at Cardiff University as well as being the Chief Medical Officer for health at Optum UK.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 Nov 2027
13 Nov 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.