Premature ovarian insufficiency
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 16 Oct 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:MenopauseVaginal drynessHormone replacement therapy (HRT)Alternatives to HRT for menopause symptomsGreene Menopause Scale
Premature ovarian insufficiency is sometimes called premature ovarian failure. The condition occurs when your ovaries no longer work properly when you are under the age of 40 years.
Your ovaries no longer produce normal amounts of oestrogen and therefore may not produce eggs. This means that your periods stop (or become irregular) and you may experience symptoms of the menopause.
In the majority of women, this occurs around the age of 51 years and is called the menopause. The term early menopause is usually used if you go through the menopause when you are between 40 and 45 years of age.
With premature ovarian insufficiency your ovaries are not working properly and have stopped producing eggs early. In some women, however, this loss of function is temporary and their ovaries work and function again in the future. This means that you may find that your periods return at some stage in the future. Therefore premature ovarian insufficiency is not necessarily the same as premature menopause, which means the irreversible loss of ovarian function before the age of 40 years.
Around 4 in 100 women under the age of 40 years have premature ovarian insufficiency. About 4 in 100 women have premature menopause.
In this article:
Video picks for Ovarian problems
Uterus and ovaries
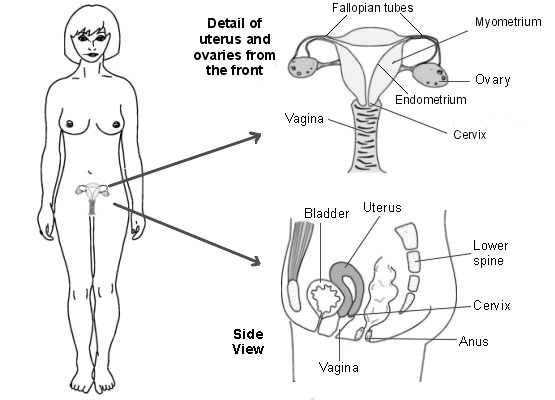
Continue reading below
Causes of premature ovarian insufficiency
There are many different causes of POI. However, for the majority of women there is no underlying cause found.
Some of the underlying causes include:
Surgery
When your ovaries are removed following an operation, you will no longer have oestrogen in your body. It is common to experience a sudden onset of symptoms soon after surgery.
Before your operation, it is important to discuss with your surgeon about receiving hormone replacement therapy (HRT) after your operation, as this will reduce the risk of having symptoms.
Cancer treatment
Some types of chemotherapy and radiotherapy can affect the function of your ovaries. For some women this may be a temporary effect but for others it may be permanent.
If you think you are at risk of developing POI in the future due to any cancer treatment, talk with your doctor. It is important to do so before starting treatment, so that you can discuss possible options for fertility preservation.
Autoimmune disease
In around 1 in 20 of women with POI, the condition is caused by an autoimmune disease. This means that your immune system (which normally protects your body from infections) mistakenly attacks itself. For example, diabetes, thyroid conditions or Addison's disease.
Genetic conditions
Genetic means that the condition is passed on through families through special codes inside cells called genes. Some women with POI have abnormalities with part of their genes.
The most common of these is Turner syndrome, in which one of the female sex chromosomes (the X chromosome) is missing.
Chromosomes are found in every cell in your body and contain genetic information. Genetic conditions causing POI are usually more common if you have other people in your family with POI or if you are very young (under 20 years) with POI.
Infections
Certain infections can very rarely be a cause of POI in some women. These include mumps, tuberculosis and malaria.
Symptoms of premature ovarian insufficiency
Back to contentsFor most women, the most common symptom is that their periods stop. For around 1 in 10 women with premature ovarian insufficiency (POI), their periods do not start and they present with POI at a very early age, usually under 20 years. Other women may notice that their periods become irregular.
Many women experience symptoms of the menopause. These include hot flushes, night sweats, reduced energy, mood disturbances, loss of energy and loss of sex drive. Some women notice that their hair becomes thinner and they have some joint pains. However, around 1 in 4 women do not have any of these symptoms.
It can be very common to feel anxious, be worried or even have feelings of hopelessness after a diagnosis of POI has been made. Some women find they feel very sad and even guilty, as having POI affects fertility.
When to see a doctor
If you've missed your period for three months or more, you should see a doctor to help find out the cause the cause. You can miss your period for a number of reasons, including pregnancy, stress, or a change in diet or exercise habits, but it's best to check with a doctor whenever your menstrual cycle changes.
Even if you don't mind not having periods, it's advisable to see a doctor to find out what's causing the change. Low oestrogen levels can lead to bone loss and an increased risk of heart disease.
Continue reading below
How is premature ovarian insufficiency diagnosed?
Back to contentsThe most common way of diagnosing this condition is by a blood test measuring the level of a hormone called follicle-stimulating hormone (FSH).
This level is usually very high as your body produces high levels to try to stimulate your ovaries to produce FSH. You will usually have two of these blood tests several weeks apart.
Other blood tests - for example, other hormone tests and genetic tests - may also be undertaken.
You may have a DXA bone scan. DXA (formerly DEXA) stands for dual-energy X-ray absorptiometry. It is a scan that uses special X-ray machines to check your bone density. A DXA scan can confirm 'thinning' of the bones (osteoporosis).
What effect may premature ovarian insufficiency have on my health?
Back to contentsThe low level of oestrogen in your body can lead to 'thinning' of the bones (osteoporosis) developing which can then lead to fractures developing in your bones.
There is also an increased risk of heart attacks at a young age. However, these increased risks are all reversed by taking hormone treatment.
See also the leaflet on Menopause for more information about the type of symptoms and complications that can occur with ovarian insufficiency.
Continue reading below
Premature ovarian insufficiency treatment
Back to contentsYou should receive treatment in the form of hormones to replace the hormones your body would be producing if you had not gone through POI.
This will either be in the form of hormone replacement therapy (HRT) or a combined (oestrogen and progestogen) hormonal contraceptive.
You should continue with treatment until you are at least 51 (the age of natural menopause), to give some protection from osteoporosis and other conditions that can develop after menopause.
The reported risks regarding HRT, such as an increased risk of breast cancer, are only relevant to those women who take HRT after the age of the natural menopause, which is around 51 years. These risks do not apply if you take HRT for POI.
If you are also needing contraception then your doctor may suggest that you take an oral contraceptive pill instead. The levels of hormones are different to those in HRT and HRT is not a contraceptive. However, HRT may be better for your blood pressure than the combined contraceptive pill.
There are many different types of hormone treatments. If one type does not suit you then it is important to talk with your doctor in order to be given an alternative treatment.
It is really important that you have a healthy lifestyle. This means that you should stop smoking if you smoke and you should eat a healthy, balanced diet.
Many experts also recommend that you have adequate calcium in your diet or take calcium supplements and also take vitamin D supplements.
If you are experiencing any mood changes (for example, feelings of anxiety, low mood or anger), it is very important that you seek help from your doctor. Some women find joining a support group and talking to other women with POI really helpful.
What is the outlook for women with premature ovarian insufficiency?
Back to contentsAround 1 in 10 women with POI which occurs without a known reason become pregnant. This is because their ovaries start working again.
IVF with egg donation is usually undertaken for those women who are keen to become pregnant. Your doctor will be able to describe this to you in more detail.
With hormone treatment, the risk of both 'thinning' of the bones (osteoporosis) reduces. Taking the correct dose and type of hormone treatment will also improve any symptoms you may be experiencing.
Patient picks for Ovarian problems

Women's health
Ovarian cyst
Ovarian cysts are fluid-filled pockets that grow on the ovaries. Almost all ovarian cysts are non-cancerous (benign), but some are cancerous (malignant), or may become cancerous over time. Many people with ovarian cysts don't have any symptoms or require any treatment, as many go away on their own. However, some ovarian cysts may need removal with an operation.
by Dr Toni Hazell, MRCGP

Women's health
Polycystic ovary syndrome
Polycystic ovary syndrome (PCOS) is a metabolic condition that affects how the ovaries work. It can cause symptoms such as weight gain, excess hair growth, period problems, and can impact fertility.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Menopause: diagnosis and management; NICE Guideline (November 2015 - last updated November 2024)
- Machura P, Grymowicz M, Rudnicka E, et al; Premature ovarian insufficiency - hormone replacement therapy and management of long-term consequences. Prz Menopauzalny. 2018 Sep;17(3):135-138. doi: 10.5114/pm.2018.78559. Epub 2018 Sep 30.
- Webber L, Anderson RA, Davies M, et al; HRT for women with premature ovarian insufficiency: a comprehensive review. Hum Reprod Open. 2017 Jul 12;2017(2):hox007. doi: 10.1093/hropen/hox007. eCollection 2017.
- Rudnicka E, Kruszewska J, Klicka K, et al; Premature ovarian insufficiency - aetiopathology, epidemiology, and diagnostic evaluation. Prz Menopauzalny. 2018 Sep;17(3):105-108. doi: 10.5114/pm.2018.78550. Epub 2018 Sep 30.
- Menopause; NICE CKS, November 2024 (UK access only)
Continue reading below
About the author

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Oct 2028
16 Oct 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.