Hiatus hernia
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 15 Aug 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Hiatus hernia article more useful, or one of our other health articles.
In this article:
Continue reading below
What is a hiatus hernia?
The term hiatus hernia refers to the herniation of a part of the abdominal viscera through the oesophageal aperture of the diaphragm. The vast majority of hiatus hernias involve only the herniation of a part of the gastric cardia through the muscular hiatal aperture of the diaphragm; however, rarely, hernias with a large defect can allow other organs to enter the thoracic cavity, such as the spleen and pancreas.
How common is hiatus hernia? (Epidemiology)1
Back to contentsThe precise incidence of hiatus hernia is not known, as most studies have looked only at individuals who presented with symptoms of dyspepsia. However, it is estimated that 55-60% of over 50s have a hiatus hernia but that only 9% are symptomatic.2
Over half of people with reflux oesophagitis diagnosed either endoscopically or radiologically are found to have a hiatus hernia.3 Estimates for the general population vary enormously - from 10-80% of the adult population in North America, for example. It is more common amongst men.4 The incidence increases with age and with obesity.
Risk factors
Obesity.5
Pregnancy.3
Ascites.6
Advanced age.4
Genetic predisposition.3
Conditions causing shortening of the oesophagus, such as chronic oesophagitis. Shortening is thought to occur by virtue of reflex contraction of oesophageal longitudinal muscle, evoked by intraluminal acid.3
Previous gastro-oesophageal surgery such as partial gastrectomy (para-oesophageal hernia).
Trauma to the chest and abdomen.
Skeletal deformities, such as scoliosis, kyphosis and pectus excavatum (predisposes to para-oesophageal hernia).
Continue reading below
Causes of hiatus hernia (aetiology)17
Back to contentsA hiatus hernia may be caused by one or more of three possible mechanisms:
Widening of the diaphragmatic hiatus.
Pulling up of the stomach, due to oesophageal shortening.
Pushing up of the stomach by increased intra-abdominal pressure.
The anti-reflux barrier is lost, and the larger the hernia, the more impaired the clearance of acid which has refluxed into the oesophagus. The hernia thereby exacerbates gastro-oesophageal reflux disease (GORD).
Classification
Hiatus hernias are broadly subdivided into two types:
Sliding hiatus hernia - the gastro-oesophageal junction slides up into the thoracic cavity (85-95% of cases).
Diagram of sliding hiatus hernia
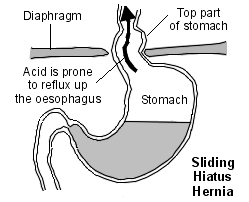
Para-oesophageal (rolling) hiatus hernia - the gastro-oesophageal junction remains in place but a part of the stomach (or colon, spleen, pancreas or small intestine) herniates into the chest next to the oesophagus (5-15% of cases). Many are mixed, with a sliding component also.
Diagram of rolling hiatus hernia
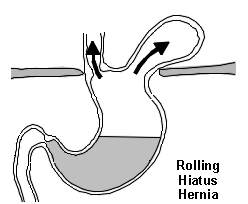
An alternative classification according to anatomical features is increasingly being used:8
Type I: sliding hiatal hernias, where the gastro-oesophageal junction migrates above the diaphragm. The stomach remains in its usual longitudinal alignment and the fundus remains below the gastro-oesophageal junction.
Type II: pure para-oesophageal hernias, where the gastro-oesophageal junction remains in its normal anatomical position but a portion of the fundus herniates through the diaphragmatic hiatus adjacent to the oesophagus.
Type III: a combination of types I and II, where both the gastro-oesophageal junction and the fundus herniate through the hiatus. The fundus lies superior to the gastro-oesophageal junction.
Type IV: structures other than stomach, such as the omentum, colon or small bowel, lie within the hernia sac.
Symptoms of hiatus hernia (presentation)
Back to contentsThe clinical significance of sliding hiatus hernias is their contribution to GORD; the concern with para-oesophageal hernias is the potential for obstruction, volvulus or ischaemia.
Many individuals with a sliding hiatus hernia will be totally asymptomatic; others may present with any of the following:
Retrosternal burning sensation or 'heartburn', especially on bending or lying.
Gastro-oesophageal reflux.
Difficulty in swallowing.
Para-oesophageal hernias may also be asymptomatic, or may present with chest pain, epigastric pain or fullness, or nausea - potentially symptoms of obstruction.
Examination is usually normal unless an underlying risk factor is present, or presentation is with complications of a para-oesophageal hernia such as obstruction.
Continue reading below
Diagnosing hiatus hernia (investigations)13
Back to contentsHiatus hernias are often intermittent, so investigation may be unreliable. Investigation is needed to rule out sinister causes of symptoms and to exclude complications.
The standard investigations are now endoscopy with or without manometry, although a hiatus hernia may be seen on chest X-ray or commonly incidentally on CT.
CXR. Hiatus hernias may be seen on plain X-rays as a soft tissue opacity with or without an air-fluid level. A retrocardiac air-fluid level on CXR is diagnostic of a para-oesophageal hiatus hernia.9
Barium studies may still be used for diagnosis of hiatus hernia but not for mucosal complications.
Endoscopy.
Oesophageal manometry (mostly used when surgery is being considered).
Associated diseases
Back to contentsBarrett's oesophagus - there is a strong link with hiatus hernia.10 Hiatus hernia is present in the vast majority of people with Barrett's oesophagus.3
Oesophageal adenocarcinoma - presence of a hiatus hernia is associated with at least twice the risk, which has been shown to increase to eight-fold if reflux is also present.3
Reflux laryngitis.11
Differential diagnosis
Back to contentsOther causes of reflux
Rumination syndrome - self-induced regurgitation from the stomach to the mouth, caused by a voluntary rise in intra-abdominal and intragastric pressure, leading to the reflux of the gastric content into the oesophagus.12
Other causes of chest pain.
More sinister causes or complications of GORD, such as Barrett's oesophagus and malignancy of the stomach or oesophagus.
Management of hiatus hernia13913
Back to contentsTreatment is not needed in the absence of symptoms, other than in para-oesophageal hiatus hernias where the potential risks are greater and surgery may be considered even in the absence of symptoms.
Lifestyle
Lifestyle measures to minimise symptoms are the same as those advocated to minimise GORD, although the evidence is weak:
People with hiatus hernia should be advised to avoid any factors likely to increase intra-abdominal pressure - eg, tight clothing, corsets.
Nocturnal symptoms may be helped by elevating the head of the bed to reduce postural reflux. Avoidance of eating late in the evening may also be helpful; advise eating at least three hours before going to bed.
Weight loss should be advised in obese patients; patients who smoke and/or drink alcohol should be encouraged to stop.
Smaller meals may be helpful, along with avoidance of foods which trigger symptoms.
Pharmacological
Symptomatic relief may be gained by the use of proton pump inhibitors (PPIs), although patients with hiatus hernia may require larger doses for symptom control. Long-term treatment is usually required. PPIs are more effective than antacids or H2-receptor antagonists, although these may be used as alternatives. The minimum dose needed to control symptoms should be used, and in some intermittent use may be sufficient.
Medical treatment is generally considered preferable to surgery.
Surgical
Asymptomatic patients with type 1 hernias do not need surgery. Indications for surgery in patients with severe GORD include:
People who are unable to comply with, or who are intolerant to, therapeutic regimes.
People who require high doses of medication, or in whom high doses are not working - eg, for intractable cough or oesophagitis due to reflux.
People who wish to avoid lifelong medical treatment.
People with respiratory complications of reflux, such as asthma.
People with symptomatic para-oesophageal hernia - elective surgery may be recommended due to the high incidence of strangulation. Asymptomatic para-oesophageal hernias do not necessarily need surgical repair. Age and any comorbidities should be taken into account.
People having bariatric surgery in whom a hiatus hernia is noted.
Currently the usual surgical procedure is a laparoscopic fundoplication. Open surgery may also be used. A laparoscopic approach is preferable, as it is equally effective and associated with reduced morbidity and mortality, especially in the case of large para-oesophageal hernias.14 The procedure involves mobilisation of the distal oesophagus, reduction of the associated hiatus hernia, and either complete (Nissen's) or partial (modified) wrapping of the fundus of the stomach around the oesophagus (fundoplication).
Risks include:
Side-effects of bloating and dysphagia.
1-2% risk of major complications or death.
High recurrence rate which increases with obesity and larger-sized hernias.
Gastropexy (suturing of the stomach to the abdominal wall) is sometimes used in addition to hiatus hernia repair or may be used as the sole procedure in high-risk patients.
In patients with proven GORD, laparoscopic fundoplication and magnetic sphincter augmentation are effective surgical options, and transoral incisionless fundoplication is an effective endoscopic option in carefully selected patients.15
Prognosis16
Back to contentsFurther reading and references
- Gastro-oesophageal reflux disease and dyspepsia in adults: investigation and management; NICE Clinical Guideline (Sept 2014 - last updated October 2019)
- Yadlapati R, Gyawali CP, Pandolfino JE; AGA Clinical Practice Update on the Personalized Approach to the Evaluation and Management of GERD: Expert Review. Clin Gastroenterol Hepatol. 2022 May;20(5):984-994.e1. doi: 10.1016/j.cgh.2022.01.025. Epub 2022 Feb 2.
- Garbarino S, Horton A, Patel A; The Utility of Esophageal Motility Testing in Gastroesophageal Reflux Disease (GERD). Curr Gastroenterol Rep. 2019 Jul 10;21(8):37. doi: 10.1007/s11894-019-0704-7.
- Omura N, Tsuboi K, Yano F; Minimally invasive surgery for large hiatal hernia. Ann Gastroenterol Surg. 2019 Jul 17;3(5):487-495. doi: 10.1002/ags3.12278. eCollection 2019 Sep.
- Roman S, Kahrilas PJ; The diagnosis and management of hiatus hernia. BMJ. 2014 Oct 23;349:g6154. doi: 10.1136/bmj.g6154.
- Smith RE, Shahjehan RD; Hiatal Hernia. StatPearls, Aug 2023.
- Hyun JJ, Bak YT; Clinical significance of hiatal hernia. Gut Liver. 2011 Sep;5(3):267-77. doi: 10.5009/gnl.2011.5.3.267. Epub 2011 Aug 18.
- Menon S, Trudgill N; Risk factors in the aetiology of hiatus hernia: a meta-analysis. Eur J Gastroenterol Hepatol. 2011 Feb;23(2):133-8.
- Che F, Nguyen B, Cohen A, et al; Prevalence of hiatal hernia in the morbidly obese. Surg Obes Relat Dis. 2013 Nov-Dec;9(6):920-4. doi: 10.1016/j.soard.2013.03.013. Epub 2013 Apr 19.
- Khouzam RN, Akhtar A, Minderman D, et al; Echocardiographic aspects of hiatal hernia: A review. J Clin Ultrasound. 2007 May;35(4):196-203.
- Weber C, Davis CS, Shankaran V, et al; Hiatal hernias: a review of the pathophysiologic theories and implication for research. Surg Endosc. 2011 Apr 29.
- Sfara A, Dumitrascu DL; The management of hiatal hernia: an update on diagnosis and treatment. Med Pharm Rep. 2019 Oct;92(4):321-325. doi: 10.15386/mpr-1323. Epub 2019 Oct 25.
- Guidelines for the Management of Hiatal Hernia; Society of American Gastrointestinal and Endoscopic Surgeons, 2013
- Lord RV, DeMeester SR, Peters JH, et al; Hiatal hernia, lower esophageal sphincter incompetence, and effectiveness of Nissen fundoplication in the spectrum of gastroesophageal reflux disease. J Gastrointest Surg. 2009 Apr;13(4):602-10. Epub 2008 Dec 3.
- Lien HC, Wang CC, Hsu JY, et al; Classical reflux symptoms, hiatus hernia and overweight independently predict pharyngeal acid exposure in patients with suspected reflux laryngitis. Aliment Pharmacol Ther. 2011 Jan;33(1):89-98. doi:
- Gourcerol G, Dechelotte P, Ducrotte P, et al; Rumination syndrome: When the lower oesophageal sphincter rises. Dig Liver Dis. 2011 Jul;43(7):571-4. Epub 2011 Feb 16.
- Sfara A, Dumitrascu DL; The management of hiatal hernia: an update on diagnosis and treatment. Med Pharm Rep. 2019 Oct;92(4):321-325. doi: 10.15386/mpr-1323. Epub 2019 Oct 25.
- Chan EG, Sarkaria IS, Luketich JD, et al; Laparoscopic Approach to Paraesophageal Hernia Repair. Thorac Surg Clin. 2019 Nov;29(4):395-403. doi: 10.1016/j.thorsurg.2019.07.002. Epub 2019 Sep 26.
- Yadlapati R, Gyawali CP, Pandolfino JE; AGA Clinical Practice Update on the Personalized Approach to the Evaluation and Management of GERD: Expert Review. Clin Gastroenterol Hepatol. 2022 May;20(5):984-994.e1. doi: 10.1016/j.cgh.2022.01.025. Epub 2022 Feb 2.
- Larusson HJ, Zingg U, Hahnloser D, et al; Predictive factors for morbidity and mortality in patients undergoing laparoscopic paraesophageal hernia repair: age, ASA score and operation type influence morbidity. World J Surg. 2009 May;33(5):980-5. doi: 10.1007/s00268-009-9958-9.
- Oor JE, Koetje JH, Roks DJ, et al; Laparoscopic Hiatal Hernia Repair in the Elderly Patient. World J Surg. 2016 Jun;40(6):1404-11. doi: 10.1007/s00268-016-3428-y.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Aug 2027
15 Aug 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free