The content on Patient is peer reviewed by our clinical content team, following the NHS Standard for Creating Health Content.

Thomas Andrew Porteus, MBCS
HealthTech
MBCS
Thomas writes to inform, inspire, and equip practice leaders and health professionals navigating change, drawing on two decades of hands-on work across the UK health system.
With over 20 years of experience at the intersection of healthcare and technology, Thomas is a trusted voice on practice operations, digital transformation, and patient engagement. A seasoned expert in supporting primary care and NHS practices, he brings deep insight into the real-world challenges—and opportunities—of delivering better care through smarter systems. Whether advising on workflow redesign, digital tools, or service innovation, Thomas combines strategic thinking with a practical understanding of what works on the ground.
Recently contributed to:
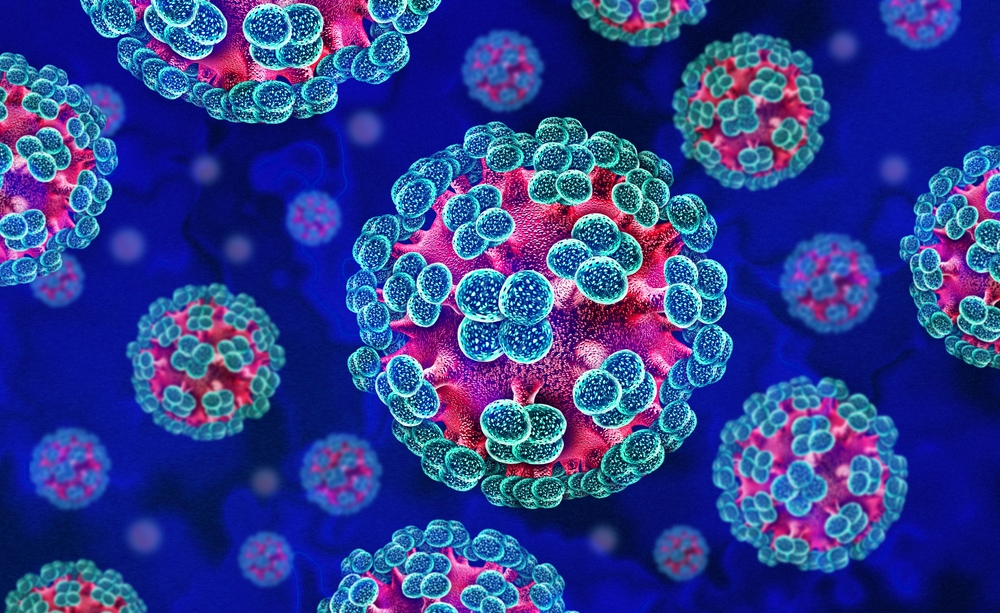
Hantavirus is making headlines again, after a cluster of serious illnesses linked to an expedition cruise ship prompted investigations by the World Health Organization. But what is Hantavirus - and is it something you need to worry about?
If you’ve booked a GP appointment or attended a hospital clinic recently, you may have found yourself sitting across from someone who introduces themselves as a 'physician associate'. For some patients, this is a familiar part of modern NHS care. For others, it can feel unexpected particularly if the assumption was that they would be seeing a doctor. Understanding what physician associates do, how they are trained, and what this means for your care can help you feel more confident navigating appointments and asking the right questions.

For years, one of the most common frustrations patients have shared is how fragmented healthcare can feel. You tell your story to one professional, then repeat it again somewhere else. You travel for appointments that feel like they could have happened closer to home. Too often, care only steps in once something has already gone wrong. The latest plans from NHS England are an attempt to change that pattern. They do not introduce a single new service or a quick fix. Instead, they outline a different way of organising care, one that is more local, more connected, and more focused on keeping you well.

Recent comments from Kanye West have once again pushed bipolar disorder into the centre of public conversation. When someone with a global platform speaks openly about their diagnosis, it can feel like a rare moment of visibility for a condition that is often misunderstood. But when that same diagnosis is linked to controversial or harmful behaviour, the tone shifts quickly. For many people living with bipolar disorder it has a real impact on how they are seen by others, how seriously they are taken, and whether they are met with empathy or suspicion. So it is worth stepping back from the noise and asking a calmer, more useful question - what does bipolar disorder actually mean in real life?

When doctors take part in strike action, it can feel disruptive and, at times, confusing. Headlines often focus on cancellations and delays, but understanding why this is happening can make it easier to navigate. At Patient we think it’s important to give a clearer, more balanced view - both of the reasons behind the strikes and what they mean in practice.
