Subarachnoid haemorrhage
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 13 Dec 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
A subarachnoid haemorrhage (SAH) is a form of stroke in which bleeding occurs into the fluid-filled space surrounding the brain (called the subarachnoid space). It is usually caused by the rupture of a small berry-like swelling (called a berry aneurysm) on one of the arteries in the brain.
SAH is a medical emergency. The risk of a further bleed is greatest during the first 24 hours from when the symptoms started.
At a glance
A subarachnoid haemorrhage (SAH) is bleeding around the brain.
It usually causes a sudden, severe headache, often described as the worst ever.
More than 8 in 10 cases are caused by a burst aneurysm.
SAH is very serious and can be life-threatening.
Seek medical advice immediately for any sudden, severe headache.
Smoking, excessive alcohol, and high blood pressure increase the risk of SAH.
In this article:
Video picks for Head injury
Continue reading below
What is a subarachnoid haemorrhage?
A subarachnoid haemorrhage (SAH) occurs when there is bleeding around the brain into the subarachnoid space. This is a space between two of the protective layers which surround the brain. These are the pia mater, which covers the brain directly, and the arachnoid mater, which is separated from the pia mater by a space filled with fluid. This fluid, the cerebrospinal fluid, is there to cushion and protect the brain from injury.
The bleeding usually comes from a burst (ruptured) berry aneurysm, most commonly at the back of the brain. Berry aneurysms are small berry-shaped swellings on the arteries which supply the brain, usually at a junction where an artery divides into two. These are relatively common in the general population, particularly in older patients, although most never rupture.
Brain and meninges
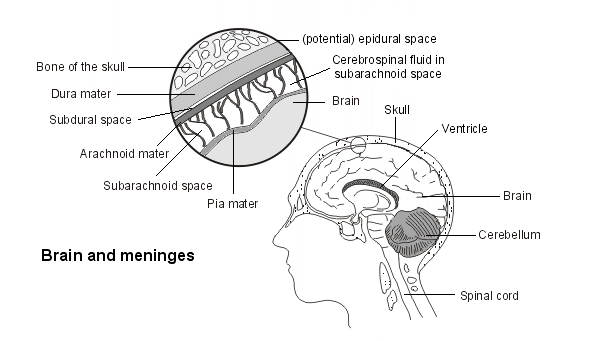
How serious is a subarachnoid haemorrhage?
Back to contentsSubarachnoid haemorrhage (SAH) is very serious. More than 1 in 4 people with a subarachnoid haemorrhage will die within the first six months after the subarachnoid haemorrhage. Of the survivors, about 1 in 3 are unable to live independently.
Continue reading below
Who is affected by subarachnoid haemorrhage?
Back to contentsSAH usually affects adults under the age of 60 years, with the average age of affected patients around 50 years. Children are not usually affected.
Women are affected slightly more often than men.
Patients of African descent are slightly more commonly affected than patients of white descent.
The condition is also more common in Finland and Japan, where the rates are around three times those in Europe.
Patients who smoke, use excessive alcohol or have high blood pressure are at greater risk.
First-degree relatives of people who have had an SAH are at greater risk.
How common is subarachnoid haemorrhage?
Back to contentsAround 8 people out of every 100,000 per year will have an SAH.
SAH causes around 6 out of 100 of all strokes.
Continue reading below
How does subarachnoid haemorrhage occur?
Back to contentsMore than 8 out of 10 cases of SAH are caused by the bursting (rupture) of berry aneurysms. About 1 in every 25 adults will have one or more berry aneurysms. However, an SAH rupturing is a relatively rare event.
Larger berry aneurysms (bigger than 7 mm) are more likely to rupture (smaller ones can grow larger over time). Rupture is more likely to occur if the elastic tissue in the walls of the berry aneurysm is weakened or strained by:
Uncontrolled high blood pressure.
High alcohol use.
Smoking.
Cocaine use.
Certain inherited conditions which cause weakening of the blood vessels. These include autosomal dominant polycystic kidney disease (ADPKD). These conditions cause only 1-2 in every 100 cases of SAH.
Other causes of SAH, accounting for fewer than 2 out of every 10 cases, include:
Head and neck trauma, when bleeding from injury to the brain or the structures around it can track into the subarachnoid space.
Abnormal blood vessels such as those that may be present in a brain tumour.
Brain infection such as encephalitis.
Vasculitis, when blood vessels inside the brain become swollen and inflamed. This can occur either due to infection or to conditions affecting the immune system.
Subarachnoid haemorrhage symptoms
Back to contentsHeadache
The most characteristic feature is a sudden explosive headache.
The headache is severe, often described as the most severe headache ever experienced. It is sometimes referred to as a thunderclap headache. However, the term thunderclap headache is more commonly used for some other types of sudden headache, including primary sexual headache.
Usually the headache lasts for a week or two. It is usually a dull, all-over headache. It may occasionally last only a few seconds or even less. The person may even look round and accuse someone of hitting him or her on the back of the head.
About 1 in 10 sudden explosive headaches are found to be due to SAH.
If you have an episode of sudden severe headache - coming on in minutes or less and being worse than headaches you have normally experienced - seek medical advice at once.
Being sick (vomiting)
Vomiting is very common in SAH. Vomiting also occurs with migraine and with other severe headaches. However, if you have an unusually severe sudden headache with vomiting you should seek medical advice.
Seizures and altered consciousness
A few people with SAH have a seizure due to irritation of the brain by the bleeding. Confusion or altered consciousness may also develop. If someone is unconscious they cannot tell you they have a headache. If someone complains of a severe headache then becomes unexpectedly drowsy, make sure that medical attendants are aware that the headache came first, as this suggests SAH.
Are there warning symptoms for subarachnoid haemorrhage?
Back to contentsSome people with SAH will have had some warning signs in the days or hours before the SAH occurs. The most common are:
Brief sudden headaches (the most common symptom).
Dizziness.
Eye pain.
Double vision or lost vision.
Loss of sensation or movement.
These symptoms may be caused by early small leaks of blood from the aneurysm as it starts to burst (rupture). However, they may not last long, and of course they may not be recognised as possibly serious by doctors or patients.
Subarachnoid haemorrhage CT scan
Back to contentsIf a subarachnoid haemorrhage is suspected then a computerised tomography (CT) scan should be performed as soon as possible. This will nearly always confirm the diagnosis.
Other investigations may include cerebral angiography. A lumbar puncture (spinal tap) may be needed if the CT scan is normal but a subarachnoid haemorrhage is still suspected.
Subarachnoid haemorrhage treatment
Back to contentsTreatment of SAH
Initial treatment is aimed at:
Stabilising the person.
Preventing further bleeding
Preventing further brain injury.
Medicines are used - for example, to:
Improve blood supply to damaged parts of the brain.
Prevent seizures which can worsen brain damage.
Surgery is used in some patients:
People with SAH are usually referred to a specialist neurosurgical unit.
Treatment usually consists of blocking off the aneurysm, either:
Through blocking it from the inside by using a special platinum coil (endovascular coiling); or
Through clipping it closed (neurosurgical clipping).
Patients need to be monitored for some time to avoid complications. These are fluid on the brain (hydrocephalus), further shortage of oxygen to the brain and low blood pressure.
Long-term management of SAH
This is aimed at:
Reducing risk of recurrence - treating high blood pressure, reducing alcohol intake and, if the person smokes, stopping smoking.
Specialist rehabilitation service for disabilities.
What is the outlook for patients with subarachnoid haemorrhage?
Back to contentsAbout 1 in 4 people die within the first six months after a subarachnoid haemorrhage. About 1 in 8 people die before reaching hospital. However more than 8 out of every 10 people admitted to a neurosurgical unit with a confirmed subarachnoid haemorrhage will survive.
Improvement will continue for about 18 months after the SAH.
Most affected people will have some impairment but some do well.
The things which increase the chance of doing better are:
A smaller bleed.
A younger age.
Remaining conscious at the time of the SAH.
About 1 in 2 people report changes with memory, mood or speech one year after a subarachnoid haemorrhage.
Can subarachnoid haemorrhage be prevented?
Back to contentsIt is not known why some people with berry aneurysms in the brain go on to develop SAH. However, it is known that certain avoidable risk factors make it more likely:
High blood pressure
Smoking
Excessive alcohol intake
Cocaine use
Avoiding these risk factors is the first way to reduce the risk of SAH.
The factors that affect the health of the walls of your brain's (cerebral) blood vessels are the same factors that affect your risk of heart disease (cardiovascular risk). Therefore, lifestyle measures which generally reduce cardiovascular risk will help prevent SAH. These include:
Healthy diet, following a five-a-day healthy eating plan.
Keeping a healthy body mass index (BMI), which will help prevent SAH.
What should I do if I know I have an aneurysm?
Back to contentsBerry aneurysms are common. They are present in around 4 in every 100 adults, being more common with greater age. They are probably the result of wear and tear on the cerebral arteries at their point of greatest weakness - the point where they divide into two.
Aneurysms less than 7 mm in diameter tend not to burst (rupture). If you have an aneurysm which is less than 7 mm in size, you may be advised that, as long as you keep your blood pressure well controlled and maintain a healthy lifestyle, your risk of SAH is no greater than that of the general population. The decision is more difficult if your aneurysm is larger than 7 mm, or you have several aneurysms. You might be offered repeat scanning, at intervals, to see if your aneurysm is growing, and to review the decision.
The alternative is to clip or block the aneurysm, even whilst it is small. The risks of surgery are significant, particularly if you are older. The risk of rupture also increases with age. These are not easy decisions.
Incidentally found aneurysms
Because they are common, berry aneurysms are often found incidentally. That is, you are found to have a berry aneurysm when having a CT scan for another reason. If this happens you will need specialist advice as to whether you need to consider operative treatment for your aneurysm. Many factors will be taken into account when advising you, including:
Your age.
The number of aneurysms you have.
Where the aneurysms are.
How large they are.
Any underlying conditions that might put you at greater risk.
People who have had an SAH and who have unruptured aneurysms
Those who have already had an SAH are usually offered treatment for other aneurysms, which is again an option between blocking the aneurysm from the inside using a platinum coil (endovascular coiling) or clipping it closed (neurosurgical clipping).
Screening for aneurysms
Back to contentsRoutine testing to check for aneurysms in relatives has not been shown to be of any benefit. Any testing is based on an assessment of each relative's own risk and is usually limited to people with at least two first-degree relatives (father, mother, sister or brother) who have had a subarachnoid haemorrhage.
Dr Mary Lowth is an author or the original author of this leaflet.
Patient picks for Head injury

Brain and nerves
Subdural haematoma
A subdural haematoma is a collection of clotting blood that forms in the subdural space. This is the space between two of the meninges, which form the protective lining that covers the brain. It usually occurs because of a head injury. It is a serious condition and emergency treatment may be needed. A CT scan can show a subdural haematoma. An operation to remove the haematoma may be needed. Many people with a small subdural haematoma can make a quick and full recovery.
by Dr Gurvinder Rull, MBBS

Brain and nerves
Concussion
Concussion is a mild traumatic brain injury that can happen after a blow to the head or a sudden, severe jolt.
by Dr Philippa Vincent, MRCGP
Frequently asked questions
What is the difference between the pia mater and the arachnoid mater around the brain?
The pia mater is one of the protective layers that directly covers the brain. The arachnoid mater is another protective layer, separated from the pia mater by a space called the subarachnoid space. This space contains cerebrospinal fluid, which helps cushion and protect the brain.
If an SAH is suspected, what kinds of tests can doctors perform to confirm it?
If a subarachnoid haemorrhage is suspected, a computerised tomography (CT) scan is usually performed first, as this almost always confirms the diagnosis. Other investigations might include a cerebral angiography. If the CT scan is normal but SAH is still suspected, a lumbar puncture (spinal tap) may be needed.
What are the main goals of treatment immediately after a subarachnoid haemorrhage?
Immediate treatment aims to stabilise the person, prevent further bleeding, and prevent further injury to the brain. Medicines may be used to improve blood supply to damaged areas of the brain and prevent seizures. Surgery, such as blocking the aneurysm with a coil or clipping it closed, is also commonly used.
Are there certain groups of people who are more likely to get a subarachnoid haemorrhage?
Yes, SAH usually affects adults under 60, with an average age of around 50. Women are slightly more affected than men, and people of African descent are slightly more commonly affected than those of white descent. It's also more common in Finland and Japan. Additionally, those who smoke, drink excessive alcohol, have high blood pressure, or have a first-degree relative who had an SAH are at greater risk.
If I have a berry aneurysm that hasn't ruptured yet, what factors might influence the decision to treat it?
Several factors are considered, including the aneurysm's size (aneurysms smaller than 7mm are less likely to rupture), your age, how many aneurysms you have, their location, and any underlying conditions that might increase your risk. For smaller aneurysms, you might be advised to control blood pressure and maintain a healthy lifestyle, with repeat scans to monitor its size. For larger or multiple aneurysms, the decision about whether to clip or coil it is more complex, weighing the risks of surgery against the risk of rupture.
Can an SAH be caused by something other than a berry aneurysm?
Yes, while over 80% of SAH cases are caused by ruptured berry aneurysms, other causes account for fewer than 2 out of 10 cases. These can include head and neck trauma, abnormal blood vessels (which might be due to a brain tumour), brain infections like encephalitis, or vasculitis, where blood vessels in the brain become inflamed.
Further reading and references
- Ziu E, Mesfin FB; Subarachnoid Hemorrhage. StatPearls, 2022.
- Etminan N, Chang HS, Hackenberg K, et al; Worldwide Incidence of Aneurysmal Subarachnoid Hemorrhage According to Region, Time Period, Blood Pressure, and Smoking Prevalence in the Population: A Systematic Review and Meta-analysis. JAMA Neurol. 2019 May 1;76(5):588-597. doi: 10.1001/jamaneurol.2019.0006.
- Stroke and TIA; NICE CKS, August 2020 (UK access only)
- Headache - assessment; NICE CKS, March 2022 (UK access only)
- Subarachnoid haemorrhage caused by a ruptured aneurysm: diagnosis and management; NICE guideline (November 2022)
Continue reading below
About the authorView full bio

Dr Mary Elisabeth Lowth, FRCGP
MA (Cantab), MB, BChir, DFFP, DRCOG, PG Cert, Med Ed, FRCGP, MA (London)
Dr Mary Lowth was a Suffolk GP for 20 years, specialising in paediatrics and child protection, and later in documentation of torture.
About the reviewerView full bio

Dr Krishna Vakharia, MRCGP
Chief Medical Officer for Health, Optum UK
MBChB, MRCGP(2013), BMedSci (hons), DFSRH, DRCOG, PGDipDerm (Distn)
Dr Krishna Vakharia is an NHS GP. She is also a regular examiner for the postgraduate Diploma in Practical Dermatology at Cardiff University as well as being the Chief Medical Officer for health at Optum UK.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 Dec 2027
13 Dec 2022 | Latest version
14 Jan 2015 | Originally published
Authored by:
Dr Mary Elisabeth Lowth, FRCGP

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.