Ascites
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Laurence KnottLast updated 10 Jan 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Cirrhosis article more useful, or one of our other health articles.
In this article:
Continue reading below
What is ascites?
Ascites is the excessive accumulation of fluid in the abdominal cavity. For ascites fluid to be detectable by clinical examination there has to be at least 1500 ml present (slightly less in a small, thin person, but significantly more in an obese person). Ultrasound can detect much smaller volumes (≤500 ml).
Ascites that is not infected and not associated with hepato-renal syndrome may be graded as follows:1
Grade 1 is mild ascites and is only detectable by ultrasound examination.
Grade 2 is moderate ascites causing moderate symmetrical distension of the abdomen.
Grade 3 is large ascites causing marked abdominal distension.
Refractory ascites can be divided into two groups:
Diuretic-resistant ascites is refractory to dietary sodium restriction and intensive diuretic treatment for at least one week.
Diuretic-intractable ascites is refractory to therapy due to the development of diuretic-induced complications that preclude the use of an effective dose of diuretic.
Causes of ascites1
Back to contentsCirrhosis:
Ascites is the most common manifestation in cirrhotic patients and is associated with a reduced survival rate.2
Approximately 55% of patients presenting with ascites have underlying alcohol-related cirrhosis.
Fluid retention (primarily ascites but also peripheral oedema and pleural effusions) is the most frequent complication of end-stage liver disease. It significantly impairs the quality of life of patients with cirrhosis and is associated with poor prognosis - one-year and five-year survival rates of 85% and 56% respectively.3
Beware the patient with a very long history of stable cirrhosis who then develops ascites - hepatocellular carcinoma must be excluded.
Malignancy accounts for around 30%. The usual causes are:
Malignancies of the gastrointestinal tract (carcinoma of stomach, colon, pancreas; primary hepatocellular carcinoma and metastatic liver cancer).
Carcinoma of ovary: Meigs' syndrome is a rare complication of ovarian cancer and produces ascites out of all proportion to the size of the tumour and pleural effusions, often unilateral.
Hodgkin's lymphoma and non-Hodgkin's lymphoma.
Metastatic carcinoma within the abdominal cavity.
Heart failure.
Nephrotic syndrome.
Protein-losing enteropathy.
Tuberculosis.
Pancreatitis.
Other rare causes, including hypothyroidism.
Iatrogenic - eg, ovarian hyperstimulation as a consequence of IVF procedures.
Continue reading below
Ascites symptoms (presentation)
Back to contentsAbdominal distension.
Weight gain as a result of water retention.
Discomfort: tense ascites is very uncomfortable but prior to this stage there is simply abdominal distension with only very mild discomfort. Malignancy-related ascites is frequently painful.
Nausea and appetite suppression: tense ascites presses on the stomach and bowel.
Increasing dyspnoea: due to limited venous return from the lower limbs (pressure on the inferior vena cava) and impaired expansion of the lungs (pressure on the diaphragm).
There may be other symptoms related to the cause of the ascites.
Consider risk factors for liver disease:
Alcohol consumption.
History of jaundice.
History of chronic hepatitis B or hepatitis C (or risk factors for these diseases).
Obesity, hypercholesterolaemia and type 2 diabetes mellitus are causes of non-alcoholic steatohepatitis, which can progress to cirrhosis.4
Examination
Perform a full abdominal examination.
Hepatic failure - ascites
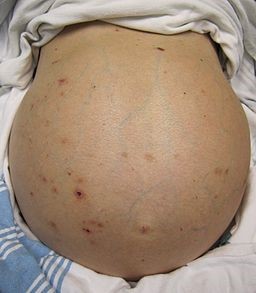
© James Heilman, MD, CC BY-SA 3.0, via Wikimedia Commons
Look at the patient, both with them lying down and standing up. The shape of the abdomen often suggests ascites fluid. On lying down, the flanks are full but on standing the ascites fluid accumulates in the lower abdomen.
The high intra-abdominal pressure may push out an umbilical hernia or even an inguinal hernia.
There may be stigmata of other diseases. Look for signs of liver disease and cirrhosis, including:
Jaundice.
Muscle wasting.
Gynaecomastia.
Spider naevi.
Palmar erythema.
Rarely, a firm nodule in the umbilicus (known as Sister Mary Joseph's nodule) is found and suggests peritoneal carcinomatosis originating from gastric, pancreatic, or hepatic primaries. A left-sided supraclavicular node, or Virchow's node, suggests the presence of upper abdominal malignancy.
Examination for ascites
Shifting dullness is used to detect ascites. One study found the absence of flank dullness to be the most accurate predictor against the presence of ascites - the probability of ascites without flank dullness was less than 10% :
Percuss from the level of the umbilicus and repeat moving laterally towards one side.
When the sound becomes dull, keep your fingers there to mark the spot and ask the patient to move on to the opposite side.
Wait briefly for the fluid to sink and then percuss again. If it is now resonant, that is a positive sign. Percuss down until dullness is reached again.
Repeat on the other side.
False positives do occur, probably from dilated coils of small intestine reacting to gravity.
At least 1500 ml of fluid must be present for a result. An ultrasound scan will detect much less fluid with greater certainty.
Large ascites can be detected by a 'fluid thrill'. This test requires two examiners. One person places the side of the palm of one hand firmly on the centre of the abdomen, with the fingers pointing towards the groin. The second person places the palm of one hand on one flank and then flicks the other flank. In large ascites, a palpable fluid thrill can be felt by the palm resting on the opposite flank.
Monitoring
Back to contentsSimple assessment of the progress of ascites may be made by:
Serial measurements of the abdominal girth - ensure the tape measure is placed in the same position each time.
Serial measurement of weight - rapid changes indicate fluid gain or loss which are much faster than gain or loss of fat or lean body mass.
Continue reading below
Differential diagnosis
Back to contentsThe differential diagnosis of ascites is with other causes of abdominal mass, especially large cysts, although sometimes plain obesity may seem like ascites. The essential feature is the fluidity and shifting with position.
Investigations1
Back to contentsThe cause of the ascites is often apparent after an adequate history and examination. The aims of investigation for ascites are:
Confirming the presence of ascites.
Finding the cause for the ascites.
Assessing any complication due to the ascites.
Blood tests
FBC.
Renal function tests.
LFTs.
Clotting screen.
TFTs.
If cirrhosis is confirmed, further tests will be required to elucidate the cause - eg, antibody tests for hepatitis B or hepatitis C.
Imaging studies
Abdominal ultrasound is a very sensitive way of assessing ascites and may also show the causative pathology such as carcinoma of ovary or metastatic liver disease.
CXR may show pleural effusion, evidence of pulmonary metastases or heart failure.
If ultrasound has failed to reveal a cause then CT scanning may be used.
Invasive procedures
A diagnostic paracentesis is recommended in all patients with new-onset ascites. See the separate Ascites tapping article.
Ascites treatment and management1
Back to contentsTreatment of any underlying cause.
Patients with cirrhosis and ascites should have a moderately salt-restricted diet with daily salt intake of no more than 5-6.5 g (87 mmol-113 mmol sodium). In reality, this means a no added salt diet with avoidance of precooked meals.
Drugs
The first line of management of ascites is sodium restriction and diuretic therapy, although diuretic therapy provides symptomatic treatment only:
Diuretics:
Spironolactone is the best initial choice in cirrhosis: it increases sodium excretion and potassium reabsorption in the distal tubules. 100 mg/day can gradually be increased to 400 mg as necessary. Serum potassium levels need monitoring, as hyperkalaemia frequently limits spironolactone's use.
Loop diuretics may be used as an adjunct to spironolactone, generally only when maximum doses of the latter have been reached. Start cautiously with, for example, furosemide 40 mg/day, although up to 160 mg/day may be used. High doses cause severe electrolyte disturbance, particularly hyponatraemia.
Amiloride may be used in patients intolerant of spironolactone but it is not as effective.
Midodrine:
Portal hypertension and splanchnic vasodilatation are major factors in the development of ascites. Vasopressors such as midodrine, an α-adrenergic agonist, have been used in non-azotemic patients with ascites. This results in significant increase in mean arterial pressure and urine sodium excretion and significant decreases in plasma renin and aldosterone.
Small randomised controlled trials show improvement in ascites control and reduction of girth and body weight. The British Society of Gastroenterology (BSG) guidelines suggest that it should be considered for patients with refractory ascites on a case-by-case basis. This is an off-licence use which will probably be more suitably prescribed in the secondary care sector.
Therapeutic paracentesis
Patients with large or refractory ascites generally benefit from therapeutic paracentesis.
This needs to be a sterile procedure.
Paracentesis of >5 litres of uncomplicated ascites should be followed by volume expansion using human albumin solution. Artificial plasma expanders may be cheaper but further evidence is needed regarding their effectiveness.
Surgical
A transjugular intrahepatic portosystemic shunt (TIPS) can be used in patients with refractory ascites needing frequent paracentesis (>3/month). It is a local anaesthetic procedure (with sedation) and has generally replaced surgically created portocaval shunts. Shunts block in about a quarter of cases. The effectiveness of TIPS has been improved by the inclusion of covered stents which improve long-term shunt patency.5
Trial results are often conflicting as to whether such a procedure offers improved survival as compared with repeated therapeutic paracentesis. The most recent Cochrane review on this subject concluded that TIPS significantly improved the survival of cirrhotic patients with refractory ascites who had not had a liver transplant, and decreased the risk of recurrent ascites and hepatorenal syndrome. There was however an increased risk of hepatic encephalopathy compared with paracentesis.6
The Model for End Stage Liver Disease (MELD) score can be calculated, which is helpful in determining when the risk:benefit ratio for TIPS is favourable.7 The calculation involved is quite complex and an online calculator is available to assist.8
Palliative care1
The only curative option for untreatable ascites is liver transplantation. If the patient is not suitable for liver transplantation, the focus is then on the control of symptoms. The most common palliative treatment is repeated ascitic drainage in hospital. Alternative treatments for untreatable ascites, such as long-term abdominal drains, need further research.
Ascites complications
Back to contentsHyponatraemia on diuretics.1
Spontaneous bacterial peritonitis (SBP) - see also the separate Intra-abdominal sepsis and abscesses article:
This occurs in 10-30% of patients with ascites and has a mortality rate of 20%.
It is frequently asymptomatic but most will have some symptom(s) such as fever, mild abdominal pain, vomiting or confusion.
Suspect SBP where patients present with hepatic encephalopathy, renal impairment or peripheral leukocytosis without any obvious precipitating factor.
A diagnostic paracentesis is mandatory in all patients with cirrhosis, requiring hospital admission to ensure that it will be detected.
Organisms are usually Escherichia coli, streptococci and enterococci.
Empirical antibiotics should be started if ascitic fluid contains >250 cells/mm3. Third-generation cephalosporins have become the standard treatment for SBP.9 However, there is no clear evidence favouring one particular antibiotic, and further research is needed.10
Prophylactic antibiotics for SBP should be given in certain patient populations.
All patients with SBP should be referred for consideration for liver transplantation.
Prognosis
Back to contentsPatients with cirrhosis who develop ascites have a one-year mortality rate of 15% and a five-year survival rate of 44%.12
For most patients with cirrhosis, therapeutic paracentesis and TIPS without transplantation may improve quality of life but are not thought to improve long-term survival significantly.
Malignancy ascites tends to suggest widespread disease and a poor prognosis.
Further reading and references
- Maruyama H, Kondo T, Sekimoto T, et al; Differential Clinical Impact of Ascites in Cirrhosis and Idiopathic Portal Hypertension. Medicine (Baltimore). 2015 Jul;94(26):e1056. doi: 10.1097/MD.0000000000001056.
- Sundaram V, Manne V, Al-Osaimi AM; Ascites and spontaneous bacterial peritonitis: recommendations from two United States centers. Saudi J Gastroenterol. 2014 Sep-Oct;20(5):279-87. doi: 10.4103/1319-3767.141686.
- Aithal GP, Palaniyappan N, China L, et al; Guidelines on the management of ascites in cirrhosis. Gut. 2021 Jan;70(1):9-29. doi: 10.1136/gutjnl-2020-321790. Epub 2020 Oct 16.
- Kuiper JJ, van Buuren HR, de Man RA; Ascites in cirrhosis: a review of management and complications. Neth J Med. 2007 Sep;65(8):283-8.
- Kashani A, Landaverde C, Medici V, et al; Fluid retention in cirrhosis: pathophysiology and management. QJM. 2008 Feb;101(2):71-85. Epub 2008 Jan 9.
- Vuppalanchi R, Chalasani N; Nonalcoholic fatty liver disease and nonalcoholic steatohepatitis: Selected practical issues in their evaluation and management. Hepatology. 2009 Jan;49(1):306-17.
- Fidelman N, Kwan SW, LaBerge JM, et al; The transjugular intrahepatic portosystemic shunt: an update. AJR Am J Roentgenol. 2012 Oct;199(4):746-55.
- Bai M, Qi XS, Yang ZP, et al; TIPS improves liver transplantation-free survival in cirrhotic patients with refractory ascites: an updated meta-analysis. World J Gastroenterol. 2014 Mar 14;20(10):2704-14. doi: 10.3748/wjg.v20.i10.2704.
- Casadaban LC, Parvinian A, Zivin SP, et al; MELD score for prediction of survival after emergent TIPS for acute variceal hemorrhage: derivation and validation in a 101-patient cohort. Ann Hepatol. 2015 May-Jun;14(3):380-8.
- MELD Score (Model For End-Stage Liver Disease) (12 and older); MDCalc, 2016
- Chavez-Tapia NC, Soares-Weiser K, Brezis M, et al; Antibiotics for spontaneous bacterial peritonitis in cirrhotic patients. Cochrane Database Syst Rev. 2009 Jan 21;(1):CD002232. doi: 10.1002/14651858.CD002232.pub2.
- Iogna Prat L, Wilson P, Freeman SC, et al; Antibiotic treatment for spontaneous bacterial peritonitis in people with decompensated liver cirrhosis: a network meta-analysis. Cochrane Database Syst Rev. 2019 Sep 16;9:CD013120. doi: 10.1002/14651858.CD013120.pub2.
- Lenz K, Buder R, Kapun L, et al; Treatment and management of ascites and hepatorenal syndrome: an update. Therap Adv Gastroenterol. 2015 Mar;8(2):83-100. doi: 10.1177/1756283X14564673.
- Biecker E; Diagnosis and therapy of ascites in liver cirrhosis. World J Gastroenterol. 2011 Mar 14;17(10):1237-48. doi: 10.3748/wjg.v17.i10.1237.
Continue reading below
About the author

Dr Laurence Knott
General Practitioner, Medical Author
BSc (Hons) Biochemistry, MBBS
Dr Laurence Knott qualified in 1973 and has had extensive experience as a General Practitioner.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 9 Dec 2026
10 Jan 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free