Chest deformity
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 23 Dec 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
This article deals with two of the three most common chest deformities: pectus excavatum (funnel chest) and pectus carinatum (pigeon chest). The third commonest chest deformity is due to scoliosis. See the separate Scoliosis and Kyphosis article.
Continue reading below
Pectus excavatum (funnel chest)
This is thought to be caused by an abnormality of connective tissue, which results in depression of the sternum. It is sometimes associated with Marfan's syndrome and Ehlers-Danlos syndrome. Most cases are recognised at birth or within the first two years of life.
Pectus excavatum
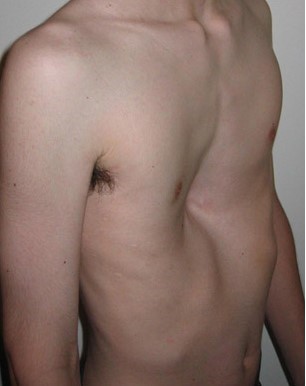
© ShareAlike 3.0 Unported(CC BY-SA 3.0), via Wikimedia Commons
Epidemiology1 2
Pectus excavatum is a congenital anomaly. It is the most common deformity of the anterior chest in children and is present in between 1 in 300-400 live births. There is a 4:1 male-to-female ratio. It is thought to be an inherited condition.
Investigations3
Radio-imaging with CXR is the first-line investigation.
Two clinical methods have also been developed here in assessing the severity of pectus excavatum:4
Chest cytometry involves measuring the circumference of the chest in the region of the distal third of the sternum or at the site of greatest deformity with the patient in the orthostatic position and inspiring deeply.
Calculation of the anthropomorphic index - this involves taking two measurements. Firstly, the maximum anteroposterior measurement in the region of greatest deformity or of the distal third of the sternum (A) is assessed. Secondly, the greatest depth of the defect is measured with the highest point of the anterior costal wall and the lowest point of the pre-sternal region at the site of greatest deformity being used as reference (B). The index is calculated as B/A.
Standardised cardiopulmonary function tests may be useful, particularly in assessing whether patients would benefit from surgery.
CT chest scanning may be indicated to assess the degree of sternal deformity, the severity of lung compression and the presence of mediastinal displacement.
An MRI technique has been developed due to concerns about the radiation dose obtained from CT scans.5
Echocardiography may be clinically indicated in patients with dyspnoea to evaluate cardiac compression. 20-60% of patients have mitral valve prolapse. Atrial compression and cardiac displacement are frequently seen.
Pulmonary function tests may be required to assess lung capacity.6
Management3
Mild cases may not require treatment, as the deformity can be hidden under clothing.
The treatment to correct functional disability was for many years the Ravitch operation in which the anterior chest wall is exposed, skin and muscle flaps are created, the affected cartilages are excised and sternal osteotomy is performed.
A newer minimally invasive procedure called the Nuss technique has been developed which involves the insertion of a retrosternal metal bar via two incisions, using a thorascope - this is now the standard treatment. The bar is removed 2-3 years later.7 2 It is mainly used in those aged 12-14 years but can be performed in younger children and in adults, in whom two bars may be required.8 The technique may lower the threshold for surgical treatment which was previously hampered by the high incidence of keloid formation of the anterior chest wall which bedevilled the Ravitch procedure. There appears to be little difference between the Nuss procedure vs the Ravitch procedure with respect to overall complications, length of hospital stay and time to ambulation. However, the rate of re-operation, postoperative haemothorax and pneumothorax after the Nuss procedure may be higher compared to the Ravitch procedure.9
Autologous fat transplantation has been reported, as has polyethylene implant for patients with mild deformity who required aesthetic improvement.10 11
A survey of patients who have had surgery showed considerable improvement in body image and function.12
NHS England does not routinely fund surgery for pectus excavatum.13
Pectus carinatum (pigeon chest)14
Back to contentsIn this condition, the sternum is raised (carina = keel). It used to be associated with rickets. Nowadays there is usually an associated history of severe asthma in childhood, sometimes with a ventricular septal defect (VSD). 20% of patients have an associated scoliosis. Pectus carinatum complicating surgical treatment for pectus excavatum has been reported.15
Pectus carinatum
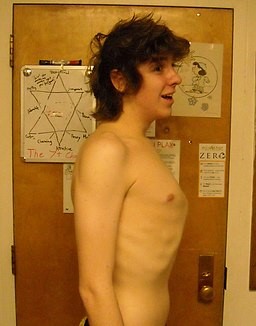
© Tolson411, CC BY-SA 3.0,via Wikimedia Commons
Two main types have been identified - chondrogladiolar (90%, keel chest, prominent middle and lower sternum) and chondromanubrial (pouter pigeon breast, prominent upper sternum). Some authorities also identify a lateral type.
The large forces needed for inspiration lead to an in-drawing of the lower portion of the ribs giving a Harrison's sulcus.
Most cases were thought to be asymptomatic. However, recent studies suggest that some patients develop a rigid chest wall resulting in reduced vital capacity and symptoms of dyspnoea, exertional tachypnoea and reduced endurance.
Epidemiology1
This is much less common than pectus excavatum. The prevalence in the USA has been assessed at 0.06% with one third of patients having a positive family history. Associated diseases are Marfan's syndrome and congenital heart disease. The patient or their parents will often be aware of the condition from early childhood but typically present to health professionals between the ages of 11-15.
Investigations
Pulmonary function tests should be performed if reduced lung capacity is suspected.
Electrocardiography and echocardiography may be needed to rule out cardiac abnormalities and assess cardiac function.
Chest radiography should be carried out; CT scanning may be helpful.
A scoliosis series should be arranged if this condition is suspected.
Management14
Many patients have a mild deformity with no associated morbidity requiring treatment.
Various physical methods of correcting the deformity have been tried, including casting, bracing and chest compressors.
Endoscopic resection of costal cartilage and sternal osteotomy is available for patients who require cosmetic correction but this procedure does nothing to correct any functional disability.
Rarely, if there is significant pulmonary and/or cardiac dysfunction, open surgical repair is performed. Various techniques have been tried.16 17
NHS England does not routinely fund surgery for pectus excavatum.13
Further reading and references
- Placement of pectus bar for pectus excavatum (also known as MIRPE or the Nuss procedure); NICE Interventional procedures guidance, August 2009
- Park SY, Park TH, Kim JH, et al; A case of right ventricular dysfunction caused by pectus excavatum. J Cardiovasc Ultrasound. 2010 Jun;18(2):62-5. Epub 2010 Jun 30.
- Weiss HR, Goodall D; Rate of complications in scoliosis surgery - a systematic review of the Pub Med literature. Scoliosis. 2008 Aug 5;3:9.
- Coelho Mde S, Guimaraes Pde S; Pectus carinatum. J Bras Pneumol. 2007 Aug;33(4):463-74.
- Cobben JM, Oostra RJ, van Dijk FS; Pectus excavatum and carinatum. Eur J Med Genet. 2014 Aug;57(8):414-7. doi: 10.1016/j.ejmg.2014.04.017. Epub 2014 May 10.
- Cardio-respiratory investigation & management of adolescents with pectus excavatum; NHS Greater Glasgow and Clyde, 2021
- Jaroszewski D, Notrica D, McMahon L, et al; Current management of pectus excavatum: a review and update of therapy and treatment recommendations. J Am Board Fam Med. 2010 Mar-Apr;23(2):230-9. doi: 10.3122/jabfm.2010.02.090234.
- Brigato RR, Campos JR, Jatene FB, et al; Pectus excavatum: evaluation of Nuss technique by objective methods. Interact Cardiovasc Thorac Surg. 2008 Dec;7(6):1084-8. Epub 2008 Sep 4.
- Marcovici PA, Losasso BE, Kruk P, et al; MRI for the evaluation of pectus excavatum. Pediatr Radiol. 2011 Jun;41(6):757-8. Epub 2011 Mar 8.
- Malek MH, Coburn JW; Strategies for cardiopulmonary exercise testing of pectus excavatum patients. Clinics. 2008 Apr;63(2):245-54.
- Nyboe C, Knudsen MR, Pilegaard HK; Elective pectus bar removal following Nuss procedure for pectus excavatum: a Eur J Cardiothorac Surg. 2011 Jun;39(6):1040-2. Epub 2010 Nov 13.
- Pilegaard HK, Licht PB; Routine use of minimally invasive surgery for pectus excavatum in adults. Ann Thorac Surg. 2008 Sep;86(3):952-6.
- Nasr A, Fecteau A, Wales PW; Comparison of the Nuss and the Ravitch procedure for pectus excavatum repair: a meta-analysis. J Pediatr Surg. 2010 May;45(5):880-6. doi: 10.1016/j.jpedsurg.2010.02.012.
- Pereira LH, Sterodimas A; Free fat transplantation for the aesthetic correction of mild pectus excavatum. Aesthetic Plast Surg. 2008 Mar;32(2):393-6.
- Grappolini S, Fanzio PM, D'Addetta PG, et al; Aesthetic treatment of pectus excavatum: a new endoscopic technique using a porous polyethylene implant. Aesthetic Plast Surg. 2008 Jan;32(1):105-10. Epub 2007 Sep 5.
- Kelly RE Jr, Cash TF, Shamberger RC, et al; Surgical repair of pectus excavatum markedly improves body image and perceived ability for physical activity: multicenter study. Pediatrics. 2008 Dec;122(6):1218-22.
- Clinical Commissioning Policy: Surgery for pectus deformity (all ages); NHS England, 2019
- Desmarais TJ, Keller MS; Pectus carinatum. Curr Opin Pediatr. 2013 Jun;25(3):375-81. doi: 10.1097/MOP.0b013e3283604088.
- Swanson JW, Colombani PM; Reactive pectus carinatum in patients treated for pectus excavatum. J Pediatr Surg. 2008 Aug;43(8):1468-73.
- Schaarschmidt K, Lempe-Sellin M, Schlesinger F, et al; New Berlin-Buch "Reversed Nuss," Endoscopic Pectus Carinatum Repair using eight-hole stabilizers, submuscular CO2, and presternal Nuss bar compression: first results in 35 patients. J Laparoendosc Adv Surg Tech A. 2011 Apr;21(3):283-6.
- Del Frari B, Schwabegger AH; Ten-year experience with the muscle split technique, bioabsorbable plates, and postoperative bracing for correction of pectus carinatum: the Innsbruck protocol. J Thorac Cardiovasc Surg. 2011 Mar 30.
Continue reading below
About the author

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 22 Dec 2027
23 Dec 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free