Polymorphic light eruption
Peer reviewed by Dr Jo SealeLast updated by Dr Toni Hazell, MRCGPLast updated 22 Nov 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Polymorphic light eruption article more useful, or one of our other health articles.
In this article:
Continue reading below
What is a polymorphic light eruption?
A polymorphic light eruption (PMLE) occurs in response to sunlight after a period of time in which the skin has been covered and scarcely exposed to the sun. It is caused by ultraviolet A (UVA) light or visible light.1 As such it may occur after sun exposure through a window, and rarely it can occur with exposure to fluorescent lighting. The term polymorphous indicates the variable nature of the rash but, for any individual, the rash tends to be fairly constant. It is described as idiopathic primary photodermatosis.
How common is polymorphic light eruption? (Epidemiology)
Back to contentsIt is a fairly common condition, perhaps affecting 15% of people in the UK.2
It is common in those with fair skin and tends to affect women two to three times more often than men.1 3
PMLE occurs commonly in people with pigmented skin, although its presentation may differ, being more likely to be the pinpoint papular and lichenoid variants of the rash.4
Age of onset is usually 20-40 years.
Incidence increases with distance from the equator.5 This is thought to be due to the greater proportion of UVA further from the equator, as UVB suppresses the immune response in the skin and UVA tends to provoke the rash.
Continue reading below
Aetiology
Back to contentsThe cause of PMLE is likely to be multifactorial. It is thought to be caused by an immunological reaction to a compound in the spring, but the precise nature is unknown.5 Findings are consistent with a type IV delayed hypersensitivity reaction.3
UV exposure causes a contact hypersensitivity response - this is normally suppressed by the release of immunosuppressive cytokines from keratinocytes. It has been suggested that 17β-estradiol somehow prevents this response, thus leading to PMLE. This theory would account for the increased prevalence of PMLE in adult women and its tendency to wane after the menopause.6
Polymorphic light eruption symptoms5
Back to contentsChest area polymorphic light eruption
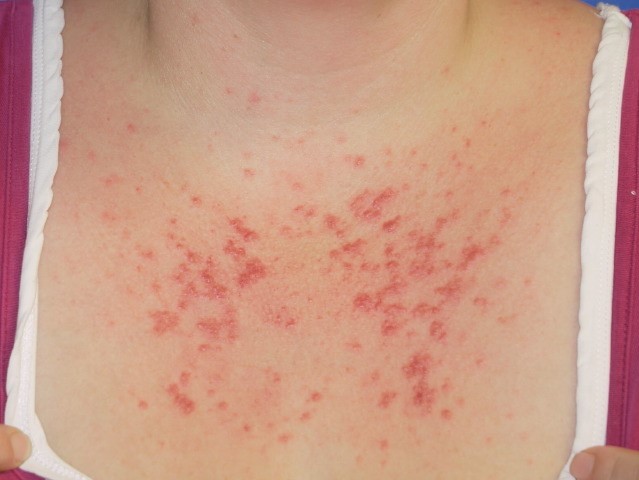
© DermNetNZ, CC BY 4.0, via Wikimedia Commons
PMLE usually presents in the spring or during travel to a sunny location. The rash varies (as its name suggests) but usually follows the same pattern in each individual:
The typical history is sudden onset of a rash 30 minutes to 24 hours after sun exposure at the start of the sunny season. The rash subsides over about a week (unless there is continuing exposure). Symptoms can recur, but reduce as summer and sun exposure progress.
The most common form of rash is crops of pink or red, raised spots of 2-5 mm on the arms, chest or lower legs. Usually the face is spared.
Other presentations include:
A dermatitis-like rash, ie vesicles followed by dry red patches.
Target lesions, resembling erythema multiforme.
In people with pigmented skin, there may be a rash with pinpoint papules on sun-exposed areas, sparing the face.
The rash is usually itchy or 'burning'.
There is occasionally a systemic flu-like illness.
The course of the rash also varies
In most, the rash settles in a few days to two weeks.
It may or may not recur next time the sun shines on the skin.
If the rash gets more sun exposure before it has cleared, the condition tends to worsen.
In most individuals there is a 'hardening' as the summer progresses and tolerance to sun increases. However, this does not always occur. Some people can develop PMLE even in the winter.
Is a polymorphic light eruption dangerous?
Most people are not severely affected and may not consult about their symptoms.
Continue reading below
Differential diagnosis1
Back to contentsPhotosensitivity drug reaction.
Chronic actinic dermatitis combines persistent light reaction, actinic reticuloid and photosensitive eczema. It is a condition of extreme photosensitivity with some overlap with PMLE.
Actinic prurigo is a variant form of PMLE which is strongly hereditary in Native Americans but also occurs sporadically in Northern Europeans. It occurs from childhood, can cause scarring and often requires treatment with immunosuppressants.
Investigations
Back to contentsUsually the diagnosis is clinical, based on a careful history.5
Investigations may be requested to exclude other diseases such as SLE or porphyria.
Photo-testing is sometimes used to aid diagnosis and to determine which type of light the skin is sensitive to. This involves repeatedly irradiating a patch of skin with UVA, UVB or visible light, repeated as necessary to produce a PMLE lesion. Photo-testing results do not correlate with the severity of PMLE.7
Skin biopsy is occasionally used.
Associated diseases5
Back to contentsPMLE may (rarely) precede the development of SLE.
There may be an association with autoimmune thyroid disease.8
Polymorphic light eruption treatment and management5 9
Back to contentsPrevention
Methods include:
Protection from sunlight - protective clothing and sunscreens (note that these may not filter out all sunlight).
Allow gradual exposure to sunlight, which may acclimatise the skin and prevent the rash.
Broad-spectrum sunscreens which are effective at blocking UVA are sometimes effective.
One small trial in 2004 suggested effective prevention using certain antioxidants combined with sunscreen but this idea does not seem to have progressed since then and does not appear in guidelines.10
The acute condition
This may be treated with:
Topical steroids or a short course of oral steroids.
Antihistamines, which may help pruritus (but note that phenothiazines can also cause photosensitivity).
Severe PMLE
This may be treated with:
Prophylactic light therapy (before sun exposure - eg, in early spring), which may help. This is known as 'photohardening' and aims to induce sunlight tolerance, using controlled exposure. This may use:UVB.UVA/UVB. Psoralen combined with UVA (PUVA) treatment.5
Recently, light-emitting diode (LED) treatment has also been suggested.11
Beta carotene and hydroxychloroquine can both improve tolerance to the sun.
Topical vitamin D analogues have been used with promising results.12 13
Immunomodulators (eg, azathioprine or thalidomide) have been used in the past to treat photodermatoses; however, the risk of adverse effects has meant that their use has declined as other treatments have become available.
Prognosis
Back to contentsMost patients can control their PMLE with simple treatments.9
The condition is likely to ease as the spring and summer advance; however, it will probably recur the following year unless precautions are taken.
Long-term prognosis - PMLE often improves over time (years) and may resolve in some patients.
A natural fall in oestrogens may account for the tendency to remit after the menopause.
Further reading and references
- Lehmann P, Schwarz T; Photodermatoses: diagnosis and treatment. Dtsch Arztebl Int. 2011 Mar;108(9):135-41. Epub 2011 Mar 4.
- Karthikeyan K, Aishwarya M; Polymorphous Light Eruption- An Indian Scenario. Indian Dermatol Online J. 2021 Mar 2;12(2):211-219. doi: 10.4103/idoj.IDOJ_434_20. eCollection 2021 Mar-Apr.
- Tutrone WD, Spann CT, Scheinfeld N, et al; Polymorphic light eruption. Dermatol Ther. 2003;16(1):28-39.
- Sharma VK, Sahni K, Wadhwani AR; Photodermatoses in pigmented skin. Photochem Photobiol Sci. 2013 Jan;12(1):65-77. doi: 10.1039/c2pp25182e.
- Polymorphic Light Eruption; DermNet NZ
- Aubin F; Why is polymorphous light eruption so common in young women? Arch Dermatol Res. 2004 Oct;296(5):240-1. Epub 2004 Sep 2.
- Schornagel IJ, Guikers KL, Van Weelden H, et al; The polymorphous light eruption-severity assessment score does not reliably predict the results of phototesting. J Eur Acad Dermatol Venereol. 2008 Jun;22(6):675-80. Epub 2008 Apr 2.
- Sharma L, Lamba S, Singh S; Thyroid function tests in cases of polymorphic light eruption: A case-control study. Indian Dermatol Online J. 2014 Jul;5(3):291-5. doi: 10.4103/2229-5178.137780.
- Fesq H, Ring J, Abeck D; Management of polymorphous light eruption : clinical course, pathogenesis, diagnosis and intervention. Am J Clin Dermatol. 2003;4(6):399-406.
- Hadshiew IM, Treder-Conrad C, v Bulow R, et al; Polymorphous light eruption (PLE) and a new potent antioxidant and UVA-protective formulation as prophylaxis. Photodermatol Photoimmunol Photomed. 2004 Aug;20(4):200-4.
- Barolet D, Boucher A; LED photoprevention: reduced MED response following multiple LED exposures. Lasers Surg Med. 2008 Feb;40(2):106-12.
- Wat H, Dytoc M; Off-label uses of topical vitamin D in dermatology: a systematic review. J Cutan Med Surg. 2014 Mar-Apr;18(2):91-108.
- Gruber-Wackernagel A, Bambach I, Legat FJ, et al; Randomized double-blinded placebo-controlled intra-individual trial on topical treatment with a 1,25-dihydroxyvitamin D(3) analogue in polymorphic light eruption. Br J Dermatol. 2011 Jul;165(1):152-63. doi: 10.1111/j.1365-2133.2011.10333.x. Epub 2011 May 30.
Continue reading below
About the author

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Jo Seale
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 21 Nov 2027
22 Nov 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free